Our patient is a 43 year-old female suffering from hand numbness and impingement of the right shoulder consequent to chemotherapy treatment for thymoma. The patient had previously sought medical attention at another clinic where her condition had been misdiagnosed, resulting in unsuccessful, costly and time-consuming treatment.
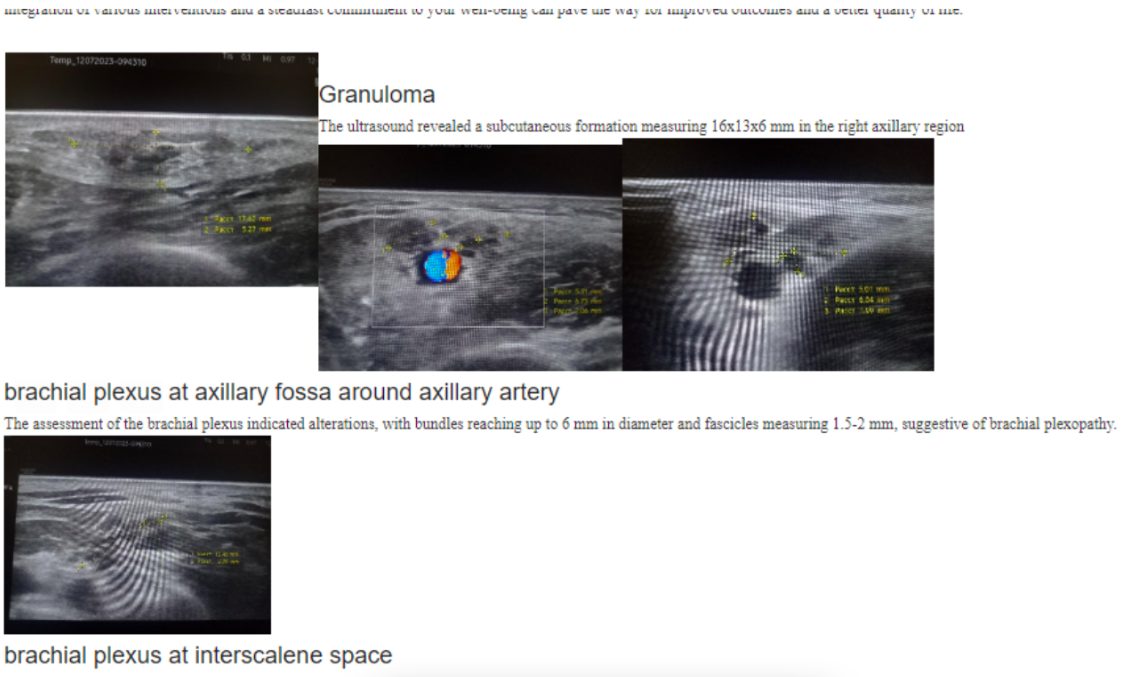
Our multidisciplinary team leveraged advanced ultrasound diagnostics to identify underlying factors contributing to the patient’s condition. We discovered the presence of axillary lymphadenopathy – an abnormality of the lymph node in the right armpit, marked by a granuloma of white blood cells. We also uncovered indicators of brachial plexopathy – a form of peripheral neuropathy affecting the nerves of the brachial plexus.
Given the patient’s previous misdiagnosis, our team wanted to ensure that our treatment plan provided both immediate relief and a strategy for long-term recovery. The following interdisciplinary measures were taken:
As a result of our multidisciplinary treatment approach, the patient’s symptoms significantly improved over time, and arm and shoulder functionality was significantly enhanced. Of particular benefit was ultrasound-guided dry needling (USGDN), which effectively addressed the brachial plexopathy and contributed to the patient’s overall recovery.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: