For many people, dysfunction and pain in the pelvic region are uncomfortable to talk about, even with a doctor. For that reason, people often wait until mild discomfort and minor symptoms escalate into unbearable pain with embarrassing and unmanageable symptoms before seeking help.
Because of the complex anatomy of the pelvic region, many things can be at the root of pelvic pain and dysfunction, and until the cause is identified, the issue cannot be resolved. Treatment with internal manual therapy, drugs and steroid injections may dull the pain and mask the symptoms, but the condition often remains unresolved, relegating patients to a vicious cycle of pain and therapy.
or

Manual Physical Therapist

Acupuncture specialist
Most traditional approaches to pelvic pain fail to get at the root cause of pelvic floor dysfunction and correct it. Instead, we see an excessive amount of internal, intravaginal, intrarectal myofascial work, which does not address the true underlying cause of pelvic problems. Patients are subjected to years of “specialized” pelvic physical therapy and multiple injections, without making any significant progress.
Conventional methods merely treat the symptoms without fixing the problem, and fail to succeed in over 80% of patients with pelvic pain. In the course of treating pelvic pain patients for over 20 years, Dr.Kalika has found that manual internal trigger point release therapy should not be performed initially for the majority of patients with pelvic pain, as it tends to make the condition chronic, and makes patients dependent on the therapist without seeing any progress.
In some cases, people see a urologist for pelvic pain, even though most urologists are unfamiliar with pelvic pain and address it as a prostatitis, prescribing different antibiotics over the course of many months of treatment, only to tell the patient that the treatment failed and they will have to live with pelvic pain. Meanwhile, the patient’s gut health has been destroyed and the nerves become hypersensitized, resulting in chronic pain.
Dr.Kalika believes that pelvic pain and dysfunction are rarely caused by trigger points alone, and recent research has shown that, in the majority of pelvic patients, pelvic floor trigger points are secondary to the dysregulation of peripheral and autonomic nerves within the sacral plexus. The peripheral sensitization of sacral nerves causes dormant trigger points to become activated and resistant to myofascial therapies. Pudendal nerve compression is also rarely the problem, as it is rarely proven by MRI or ultrasound.
Given the failure of conventional pelvic therapy over the past 20 years, Dr. Kalika believes it is critical to identify the underlying cause prior to addressing the trigger point component of pelvic pain.
Pelvic pain is a multifactorial condition. When a patient’s chronic pain is caused by multiple factors, more than one treatment approach may be required. When we consider secondary causes, it is important to note that many of those factors also exist in people who never develop pelvic pain. Secondary factors should only be considered once dysregulation of the nervous system has been addressed. When exposed to stressful events, disease, surgery, or physical or emotional trauma, trigger points and myofascial pain may arise, but they should be considered secondary to sacral nerve dysregulation.
We believe that performing internal physical therapy when the patient is experiencing acute pain is counterproductive and merely leads to chronicity. This has been our experience with a large number of patients who have come to us after receiving unsuccessful internal physical therapy elsewhere.
Diagnosis begins with a medical history and physical exam of the pelvic floor, low back, hips and pelvis. Gait analysis may be performed as well. Your clinician will ask for detailed information about pregnancies and childbirth, and any difficulties or abnormalities you experienced associated with childbearing.
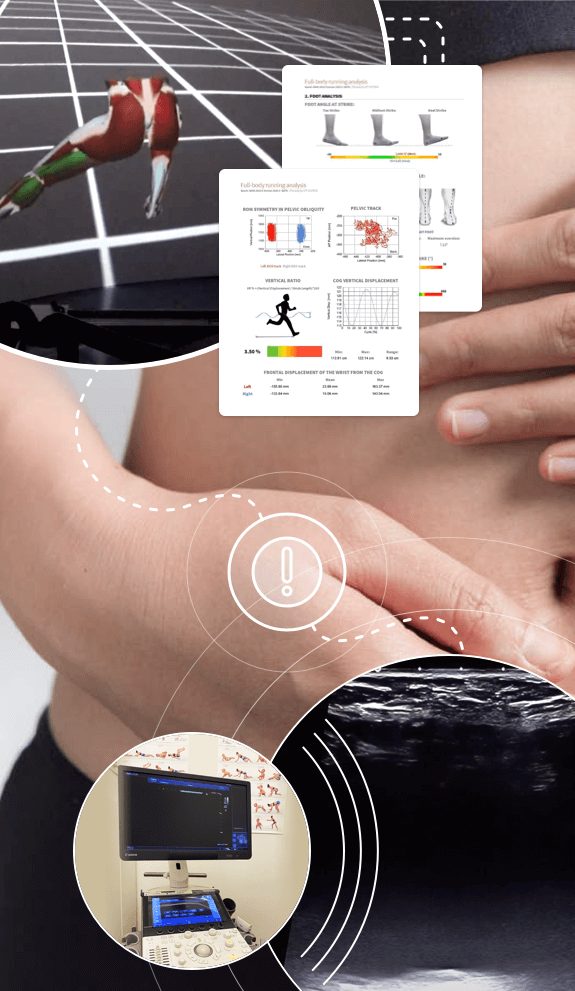
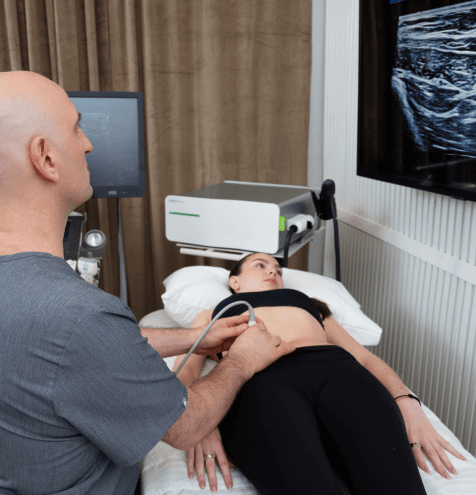
At NYDNRehab, we use high resolution dynamic ultrasound to visualize the structures of the pelvic floor with the patient in motion. Since the pelvic region is closely related to the low back and hips, we perform diagnostic and functional sonography to rule out hip and low back issues.
During a diagnostic ultrasound session, both patient and clinician can view the muscles of the pelvis and abdominal wall in motion, to assess for muscular deficits, excessive force production (pressure) and trigger points.
With real-time ultrasound imaging, we are able to diagnose and treat a number of issues related to pelvic dysfunction, including:
The superficial fascia of the pelvic floor is a thin fibrous layer of connective tissue embedded with adipocytes – specialized fat cells – along with a complex network of lymphatic and blood vessels. The pelvic fascia plays an important role in exteroception – sensory awareness of stimuli outside the body.
Fascia tissue has a high percentage of elastic fibers and a slippery coating of hyaluronan that facilitates the gliding of nerves and blood vessels. The pelvic fascia works together with the transversus abdominis, diaphragm and pelvic floor muscles to optimize abdominal pressure, providing spinal stability. Its autonomic innervation makes the pelvic fascia sensitive to stress and changes in temperature, and it is intricately connected to the genitalia.
Pelvic fascia manipulation is often the missing link in pelvic pain treatment. Pelvic pain is mostly generated from hyperactive nerves embedded in the deep fascia of the pelvis. These include peripheral nerves like the pudendal, gluteal and cluneal nerves that glide between the pelvic floor muscles and can be released from entrapment by manipulation of the endomysium and perimysium.
Other sensory nerves and their endings inhabit the superficial fascia, such as the ilioinguinal, iliohypogastric and genitofemoral nerves. When your parasympathetic nerves are entrapped in the superficial fascia they become hyperactivated, generating pelvic pain.
The intimate connection between the deep and superficial fascia layers has been largely overlooked in conventional treatment of pelvic pain. Most doctors and therapists focus on injections to block the pudendal nerve, and on manual release of trigger points.
According to evidence-based research, pelvic fascia manipulation therapy not only releases densified layers of superficial and deep fascia, but also calms hyperactivated nerves. Other therapies, such as ultrasound-guided electro acupuncture, are often used in conjunction with fascial manipulation for the neuromodulation of hyperactive pelvic nerves.
The human body has its own innate healing mechanisms, but it sometimes needs a nudge to accelerate the healing process. Regenerative technologies help to jump-start healing by stimulating tissue repair at the cellular level. Our outpatient regenerative therapies expedite recovery with minimal discomfort for the patient.

Focused Shockwave Therapy (ESWT)
Focused ESWT produces high frequency sound waves to stimulate the body’s own reparative mechanisms. In patients with chronic pelvic pain, ESWT works by interrupting hypersensitized nerve impulses, helping to reduce muscle spasms. It also reduces inflammation to free up entrapped nerves, allowing them to glide among other structures. We use ultrasound guidance to ensure that shockwaves reach the targeted nerves and tissues. Shockwave also helps to release myofascial trigger points and fascia adhesions that contribute to pelvic pain. ESWT is considered to be a top-tier, evidence-based treatment approach for pelvic pain.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Electromagnetic Transduction Therapy (EMTT)

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels. *It is important to note that the technology behind HEIT is identical to EMSELA (electromagnetic pelvic floor therapy). EMSELA is a rebranded version of HEIT, promoted by some clinics at more than double the price.

HIGH ENERGY INDUCTIVE THERAPY (HEIT)
Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.
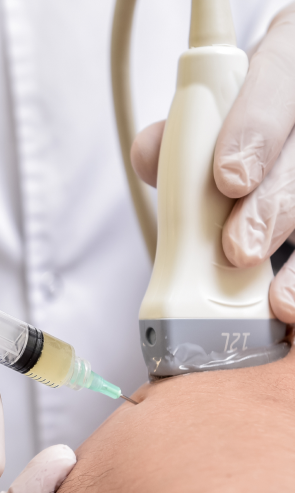

Sudden onset pelvic pain should not be ignored. It is essential to immediately rule out visceral pathology (organ dysfunction).
Treatments for acute pelvic pain include:
Ongoing or intermittent pelvic pain that lingers for weeks or months can often be eliminated with non-invasive conservative treatment.
Treatment options for chronic pelvic pain include:
Home treatment options for pain management and restoration include:
At NYDNRehab, we take a one-on-one approach to patient care. We understand that every patient has a unique anatomy, and that each condition has unique characteristics. We tailor our treatment plans to the individual, and never use cookie cutter approaches.
Our experience using innovative treatment methods and advanced technologies makes NYDNRehab the number one choice for pelvic floor physical therapy and rehabilitation in NYC.The muscles and connective tissues that make up your pelvic floor form a hammock that spans from your tailbone to your pubic bone, creating a wall of separation between your perineal region and your pelvic bowl. The pelvic floor provides support for your intestines, bladder and uterus, and its muscles govern bladder, bowel and sexual function.
Signs that your pelvic floor may not be doing its job often begin with bladder and bowel leakage, urinary hesitancy or urgency, or constipation.
High-impact sports like gymnastics, basketball and running create downward pressure on the pelvic floor muscles, putting athletes in those sports at risk for dysfunction. Pregnancy and childbirth may also lead to pelvic pain and dysfunction.
Pain that persists for six months or longer is categorized as chronic pelvic pain (CPP) which can seriously interfere with normal daily activities. CPP is common in women, accounting for about 10% of all visits to the gynecologist. It is also a common urologic complaint among men under age 50.
We strongly believe that the pelvic floor muscles are not the underlying cause of pain. Experience tells us that pelvic pain originates in walking gait deficits and imbalances in the hips and low back, interfering with the body’s ability to balance intrapelvic and intra abdominal pressure. While ESWT, EMTT, and USGDN are effective in relieving pain, restorative pelvic floor physical therapy provides the ultimate solution to pelvic pain and dysfunction.

Lifestyle factors play a key role in pelvic dysfunction. Eating whole organic foods and drinking plenty of plain filtered water can help you avoid urinary and bowel issues that lead to pelvic pain. Regular exercise that targets muscles throughout the entire body helps to strengthen the pelvic and core muscles and promote healthy function. Managing your weight, avoiding smoking, and stress management are all important lifestyle factors that help to prevent pelvic issues. Staying fit and active throughout your pregnancy can reduce your risk of developing pelvic floor issues.
In addition, you should rule out visceral pathologies by consulting your healthcare provider. If you suffer from hip or back pain, you should seek treatment, as untreated pain in those areas can affect the pelvic region. A 3D gait analysis can help to identify and correct asymmetrical gait patterns. Try to remain aware of your pelvic floor, and do not clench your pelvic muscles when stressed. Be sure to void your bladder and bowels when you feel the urge – do not hold your urine. Eating an organic whole foods diet and drinking plenty of purified water will help you avoid constipation.

Pelvic floor physical therapy helps your body heal itself, to eliminate pelvic floor dysfunction for good. However, not all physical therapy is effective. Conventional therapy uses manual intra vaginal or intrrectal release techniques to target the internal pelvic floor muscles. In our experience, this type of treatment only provides temporary relief with no significant progress, making patients dependent on ongoing therapy to relieve pain.
At NYDNRehab, we help our patients get long-term relief using a combination of extracorporeal shock wave therapy (ESWT), extracorporeal magnetic transduction therapy (EMTT) and ultrasound guided dry needling (UGDN). Our treatment approach goes beyond pain management, to actually regenerating damaged tissues and promoting healing. We are the top rated physical therapy clinic for pelvic pain in NYC.
These case studies reflect real clinical conditions evaluated at NYDNRehab using advanced diagnostic methods and individualized rehabilitation strategies. All cases are evaluated and managed by Dr. Lev Kalika and the NYDNRehab clinical team.
Independent peer-reviewed research relevant to this treatment approach.
Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.