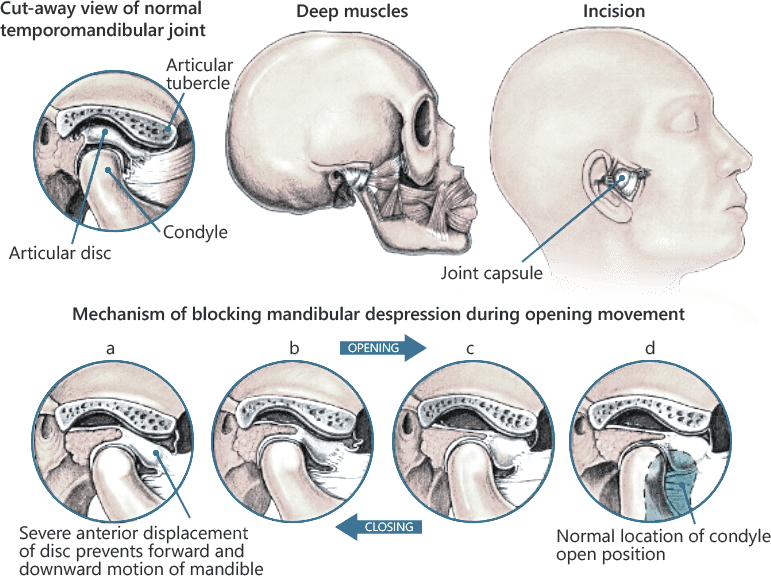
Your temporomandibular joints (TMJs) are the two hinge joints that connect your jawbone to your skull. The TMJs enable you to open and close your mouth, chew, talk, sing and smile. Disorders of the TMJ are not isolated to the jaw and teeth. They are complex systemic conditions that involve the central nervous system, with genetic and immunological components. Resolving TMJ disorders is a complex process that requires the intervention of an experienced jaw pain specialist.
or
Dr. Lev Kalika, clinical director at NYDNRehab, is a TMJ Specialist in NYC who has developed his own unique approach to treating TMJ disorders. Dr. Kalika has completed an internship in Chile under Mariano Rocabado, a world leader in the conservative treatment of TMJ disorders.
Dr. Kalika has pioneered a combined approach to TMJ that includes manual physical therapy, shockwave therapy and ultrasound guided dry needling. He often collaborates with some of the most experienced dental care specialists in the field.
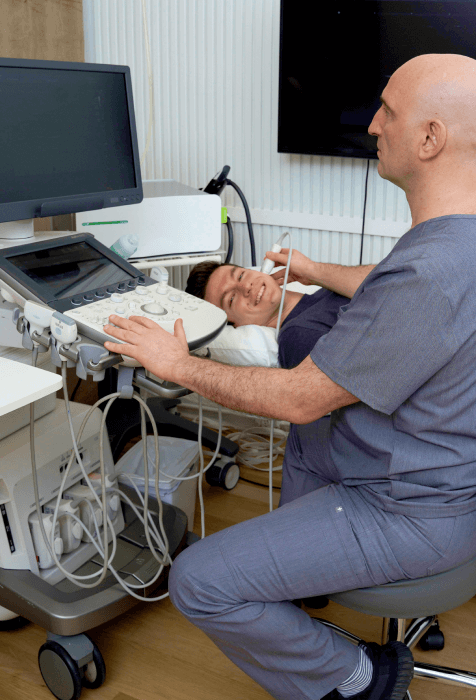
In addition to his expertise in treating TMJ, Dr. Kalika is an accomplished specialist in diagnostic ultrasonography, with multiple peer-reviewed research articles to his credit. Ultrasound imaging helps us to visualize the structures surrounding the jaw, and identify factors that may be contributing to TMJ symptoms.
Dr. Kalika has over 15 years of experience in treating TMJ disorders, and has published multiple research articles on the topic.
Physical therapy is a valuable and effective approach to resolving musculoskeletal pain and dysfunction, but in many cases, physical therapy does not provide a stand-alone solution. Prior to beginning physical therapy, patients often need to address underlying issues that contribute to their pain and disability.
Unfortunately, mainstream physical therapy clinics are often not adequately equipped or experienced to identify and treat complications that undermine the effectiveness of physical therapy. They often rely on one-size-fits-all treatment protocols that overlook the unique characteristics of the individual condition, opting to treat the symptoms and not the patient.
Identifying and treating underlying issues prior to beginning physical therapy is key to getting fast and effective results. Failure to do so can completely undermine your treatment protocol, and in some cases, your condition may even worsen.
At NYDNRehab, we use a broad range of advanced technologies and innovative therapeutic approaches to resolve issues that can potentially undermine the success of physical therapy.
Our talented staff is certified in a diverse array of treatment methodologies, rarely found in run-of-the-mill physical therapy clinics. Our one-on-one sessions are personalized, based on the patient’s unique diagnostic profile.
People suffering from TMJ symptoms often go from one practitioner to the next without completely resolving their TMJ disorder. The truth is that most TMJ “specialists” focus on symptoms and treat the locus of pain, without ever attempting to get to the underlying cause of TMJ.
At NYDNRehab, we believe that pain syndromes and movement disorders do not happen randomly. It is our goal to uncover the underlying factors that contribute to pain and dysfunction and correct them. In the case of TMJ, multiple factors may come into play. We don’t stop until your pain goes away and normal function is restored.
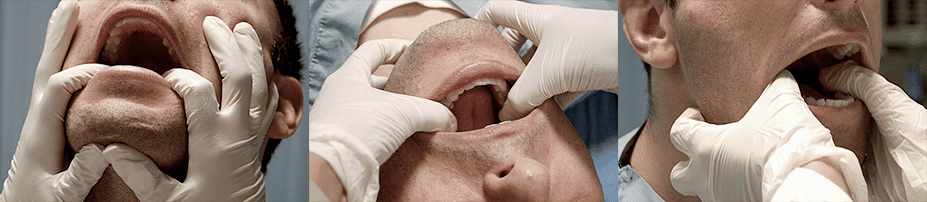
Our personalized one-on-one approach to TMJ dysfunction ensures that you will receive the very best care for your unique condition. We never take a one-size-fits-all approach to TMJ treatment. Our growing collection of diagnostic and regenerative treatment technologies gives us a huge advantage over run-of-the-mill physical therapy clinics.

TMJ conditions are typically diagnosed based on the patient’s reported symptoms, along with a physical exam of the jaw, neck, face and head. However, a recent study found that people with TMJ disorders often report widespread pain in other areas of the body, along with other medical conditions.
At NYDNRehab, we take a holistic approach to TMJ diagnosis. We understand that the human body is not just a collection of isolated parts, but rather an integrated system of interdependent structures that function together as a whole.
Because of the way US medical insurance is structured, doctors are only allowed to treat one body part at a time, even though pain in your jaw may be caused by issues in another area of your body. Isolating one body part from another often results in misdiagnosis and ineffective treatments that cost the patient time and money, without relieving their pain or resolving their disorder.
In addition to evaluating your symptoms and health history, and conducting a thorough physical exam, the TMJ specialists at NYDNRehab use the highest resolution diagnostic ultrasound to visualize the structures affecting your jaw function. Ultrasound enables us to view the jaw in motion, in real time, and explore associated structures that may be contributing to your TMJ pain.
With an accurate picture of your jaw and surrounding structures at hand, we are able to create a personalized treatment protocol that specifically targets all the factors contributing to your TMJ disorder.
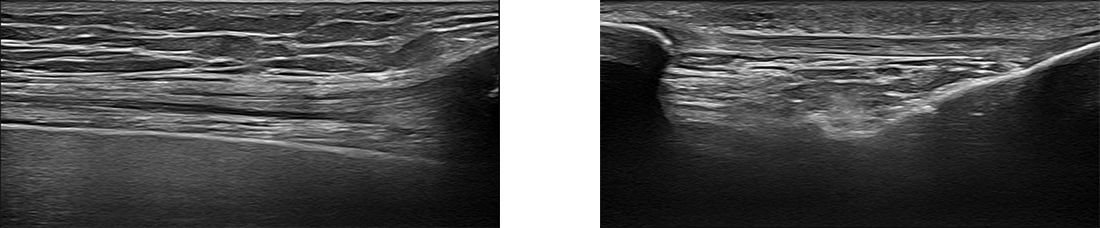
Please explore more advanced diagnostic option unavailable anywhere else:
Jaw pain and stiffness
Muscle pain while chewing
Pain that radiates to the face and/or neck
Locking of the jaw
Clicking, grating or popping sensations when moving the jaw
Tinnitus (ear ringing)
Misalignment of the upper and lower teeth
Headaches
Poor posture
Teeth clenching or grinding due to stress
Dental issues
Myofascial trigger points
Chronic systemic inflammation
Trauma
Infection
Anxiety
Middle aged
Female
Caucasian
Chronic Stress
Certain medical conditions
Poorly fitting dentures
Smoking
Use of contraceptives
The human body has its own innate healing mechanisms, but it sometimes needs a nudge to accelerate the healing process. Regenerative technologies help to jump-start healing by stimulating tissue repair at the cellular level. Our outpatient regenerative therapies expedite recovery with minimal discomfort for the patient.
Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels.

Our INDIBA Tecar therapy machine converts electrical current into a stable radio frequency current of 448 kHz, designed to increase and stabilize the exchange of ions in damaged cells, evoking a regenerative response that accelerates healing. INDIBA can be used to successfully treat joint and muscle disorders, low-back pain, sports injuries, surgical incisions and various pain syndromes. Another therapeutic effect of INDIBA is extreme and prolonged cellular hyperthermia. Due to this effect, INDIBA therapy combined with manual therapy and soft tissue tissue manipulation enables instantaneous release to occur, significantly shortening the number and duration of physical therapy sessions. What is normally accomplished in two months of physical therapy can be accomplished in 3-4 sessions with INDIBA.
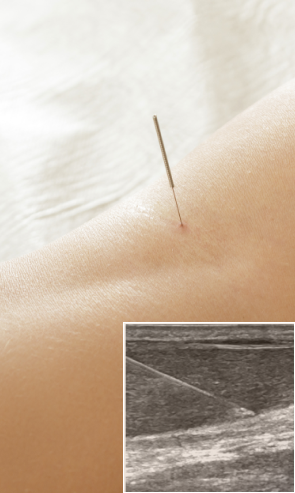
Myofascial trigger points often contribute to lower back pain. Dry needling is an outpatient procedure that inserts non-medicated needles into the trigger point to evoke a twitch response, releasing the trigger point and immediately relieving pain. Ultrasound guidance eliminates the need for multiple insertions, reducing pain and discomfort for the patient.
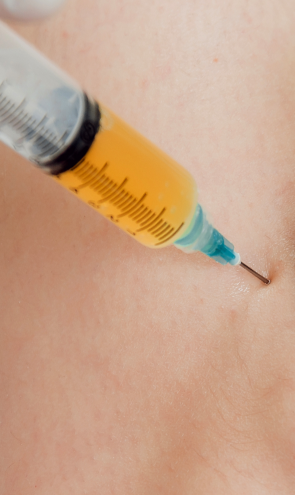
Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.
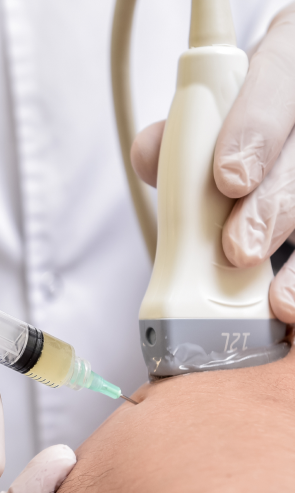
Ultrasound guidance allows us to visualize damaged and dysfunctional tissues for injection therapies, and to precisely target trigger points for dry needling. Our advanced technologies set NYDNRehab apart from run-of-the-mill physical therapy clinics that use antiquated and ineffective methods to treat TMJ syndrome.
Dr. Kalika is an experienced expert in ultrasound-guided procedures.
According to the National Institutes of Health (NIH), TMJ treatment should be as conservative as possible, and patients should avoid procedures that permanently alter the structure or alignment of the jaw or teeth.
Typical treatments for TMJ pain include:Stretching and relaxation techniques
Icing
Over-the-counter and prescription pain medications
Stabilizing devices that fit over the teeth
However, traditional treatment approaches provide only temporary pain relief at best, and do not fully resolve TMJ disorders.

At NYDNRehab, we use cutting-edge technologies combined with manual therapies to restore pain-free jaw function. Our evidence-based treatment methods require skills and experience that are rarely found in typical physical therapy clinics.
As a certified practitioner of Stecco method fascial manipulation, Dr. Kalika has had remarkable success in resolving TMJ syndrome. Oftentimes, the fascia surrounding and supporting the jaw becomes densified, preventing it from gliding and inhibiting jaw movement. Unlike common fascia approaches that are not evidence-based, the Stecco method is a very specific technique supported by research that requires special training. Dr. Kalika is one of the few certified practitioners of Stecco fascial manipulation therapy in NYC.
Manual oro-facial massage therapy, to relax and restore balanced tension in the muscles and connective tissues of the jaw.
Ultrasound guided dry needling, to target myofascial trigger points in the jaw and surrounding musculature. Research has shown dry needling to be effective for significantly reducing pain and improving jaw function in patients with TMJ disorders.
Dry needling is a successful approach for eliminating trigger points in the masticatory (chewing) muscles. We use ultrasound guidance to visualize trigger points, to ensure precise targeting of the inserted needle, inducing immediate release for rapid pain relief.
Extracorporeal shockwave therapy (ESWT) to relax jaw tension and improve jaw range of motion. A recent study found that ESWT significantly reduces pain and improves TMJ function and range of motion.

In many cases, TMJ resolves itself when treated with self-care strategies, like eating soft foods, applying ice to the TMJ, stretching exercises, and stress management. But if you are suffering from TMJ pain and dysfunction that doesn’t improve or even gets worse over time, you need professional intervention.
The clinic at NYDNRehab features the most advanced technologies available for treating pain syndromes, injuries and movement disorders. Our treatment approaches are backed by scientific evidence, and their effectiveness is proven by our patients’ success.
The clinical staff at NYDNRehab is constantly looking for new treatment approaches that can help our patients restore pain-free movement. We are dedicated to providing the best patient care possible. Our expertise and experience make NYDNRehab the clinic of choice for TMJ physical therapy in NYC.
February 21, 2026
Patients with Temporo-Mandibular joints (TMJ) pain often become victims of excessive fragmentation of our complex healthcare system. An individual with persisting pain in the TMJ area may very soon find himself on a long, if un-amusing, journey through the complicated maze of the medical profession. From a dentist office too often however such a patient would emerge from his quest with his insurance coverage strained and his TMJ pain fully intact.
Most of the time a patient with TMJ problem initially will be seen by an orthodontist or a neuromuscular dentist, because in theory TMJ pain falls within the scope of their expertise. The truth however is that even though TMJs are anatory of TMJ problems.
Due toms as TMJ pain syndrome.
TMD is a set of related pathological changes, which produce musculoskeletal sympto organize a variety of dysfunctions and disorders that result in abnormal function of the muscles and joints of the jaws.
In order tor system, meaning that TMJ movement is controlled by the same neurological mechanisms that control any movement in the body.
Temporo-Mandibular system is densely innervated and its mo Temporo-Mandibular system is one of the most active and powerful structures of human body. It works during the day and while we are asleep. Due to breakdowns. Fortunately for the patient the Temporo-Mandibular system is very resilient and capable of self-repair when a proper treatment is administered.
Causes of Orofacial pain arising from within the Temporo-Mandibular system:
Diagnosed TMDs fall into three basic etiological categories:
The first category belongs tonicity of muscle of mastication and muscles of the cervical spine.
The second category is a mixed etiology. Hypertory muscles in conjunction with some degree of intra-articular TMJ dysfunction (hypo- or hypermobility in one or both joints, with or without periarticular adhesions).
Resulting from true intra-articular pathology with locking of the jaw.
It must be mentioned that mixed etiology includes various contributing factors listed above.
TMDs of any etiology in general seldom require a surgical intervention. Histo be the most effective measures in treatment of TMJ pain disorders.
Conditions from Categories 1 and 2 (see above) fall intom made appliances.
TMDs caused by intra-articular pathology (category 3) require close cooperation between orthodontist or maxillofacial surgeon and neuromuscular specialist. The world’s scientific authority recommends treating these cases conservatively until maximum improvement is achieved before committing to make a sound judgment, based on good clinical skills and clear understanding of structural pathology of the TMJ, whether the conservative care is no longer effective and refer the patient for surgical consultation.
Although, most of TMJ pain disorders are self-limiting, they could generate excruciating pain and cause significant distress to a psychosocial specialist or a pain clinic may be warranted.
At DNR’s office located in Manhattan, Midto find even in New York.
TMJ pain can become chronic and resistant to treatment if professionals who specialize in TMJ therapy do not timely address it.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: