Dr. Kalika, clinical director of NYDNRehab, has dedicated his life’s work to revolutionizing the way pain syndromes and movement disorders are diagnosed and treated. He was among the first in his field to embrace technology as a game-changer for patient diagnosis and treatment. The NYDNRehab clinic is one of the best-equipped physical therapy clinics in the world.
Dr. Kalika is an expert in functional podiatry, a holistic approach to foot health that does not involve steroid injections or surgery. His approach entails advanced diagnostics, including:
Our holistic treatment approach focuses on foot functionality and its impact on the entire lower kinetic chain. We combine the most advanced regenerative treatment methods with sophisticated foot and ankle physical therapy to restore pain-free functional mobility.
For injection and regenerative therapies, Dr. Kalika teams up with Dr. Uri Brozgol, a neurologist with 20+ years of experience in treating pediatric and adult myofascial pain. Dr. Brozgol is an expert in orthobiologic injection procedures and fascial release techniques.
Dr. Kalika is certified in biomechanics and gait analysis, and is an expert in diagnostic ultrasonography. He has over 20 years of experience in successful treatment of foot and ankle conditions, and has published multiple research papers on the use of ultrasonography, dry needling and shockwave therapy for treating a variety of conditions.
Dr. Kalika’s successful track record in rehabilitating musculoskeletal injuries combined with Dr. Brozgol’s expertise in treating myofascial pain makes NYDNRehab the clinic of choice for heel pain in NYC.
Kalika, Lev, and Rostyslav Bubnov. “Targeted Ultrasound-Guided Shockwave Therapy of Low Back Pain Using Focused, Defocused and Radial Shockwave” Neuromodulation 25.7 (2022): S339. Link to article
Bubnov, R., and L. Kalika. “Comparative Study of Dry Needling under Ultrasound Guidance and Extracorporeal Shock Wave Therapy for Myofascial Pain and Spasticity Management.” Movement Disorders 34 (2019). Link to abstract

Orthobiologic specialist
New Yorkers are constantly on the go, often walking for blocks on end as a routine part of daily life. But walking on concrete, especially in shoes that do not provide adequate support or shock absorption, can put you at risk for foot and heel pain. Traditional physical therapy clinics often make heel pain diagnoses based on symptoms alone, resulting in frequent plantar fasciitis misdiagnosis that delays the healing process and prolongs pain.
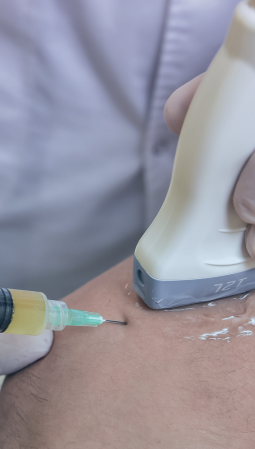
At NYDNRehab, we use the highest resolution diagnostic ultrasound to pinpoint the exact cause of your heel pain in real time, without having to wait for results from X-ray or MRI. Rapid and accurate diagnosis means we can get right to work with a personalized treatment plan designed just for you. Our advanced treatment technologies enable us to accelerate the healing process without drugs or surgery, to get you back to doing the things you love in the shortest time possible.

We never use a one-size-fits-all approach to patient care. Your treatment plan is based on your condition’s unique characteristics and your individual needs. Our experienced professionals work with you one-on-one, to ensure that you receive the very best care for resolving your heel pain.
Because your heel is part of a complex system of muscles, nerves, bones and connective tissues, there can be multiple underlying causes of heel pain. Many clinics take a hit-or-miss approach to diagnosis, beginning with the most common condition and re-evaluating when you don’t respond to treatment. Without the benefits of ultrasound imaging, heel pain diagnosis becomes a guessing game that wastes the patient’s time and money, while prolonging your pain and disability.
At NYDNRehab we use high-resolution diagnostic ultrasonography to dynamically visualize the structures of your foot-heel-ankle complex in real time. Clear images of the foot and ankle in motion enable us to identify the exact cause and extent of your heel pain, so we can quickly initiate effective treatment.
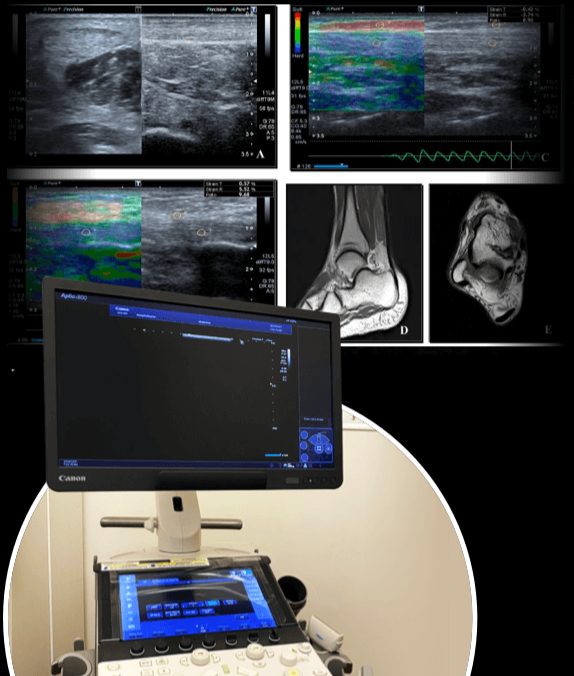
Many podiatrists and physical therapists are quick to diagnose heel pain as plantar fasciitis, the most common type of heel pain. But plantar fasciitis misdiagnosis can result in weeks or months of unnecessary pain and disability, not to mention expensive treatments and procedures that eat up your time and drain your bank account.
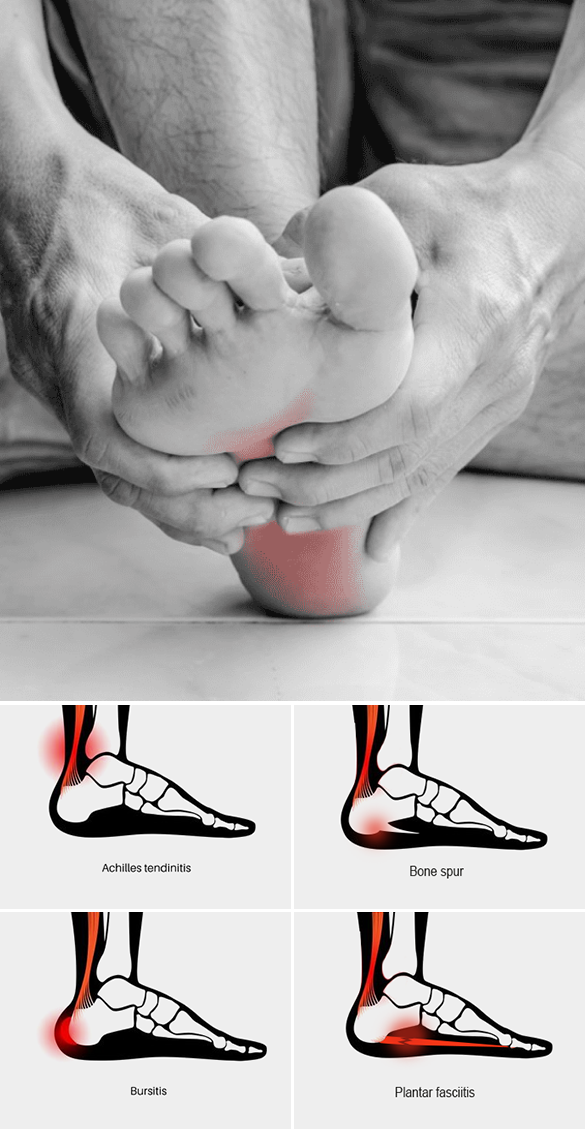
Heel pain can stem from a variety of conditions, including:
With such a diverse range of potential conditions, a quick and accurate diagnosis that does not involve guesswork or rely on symptoms-based decision-making can mean the difference between rapid healing and pain relief, or months of prolonged pain.
There is a broad range of options for treating heel pain, with some being more effective than others. Run-of-the-mill physical therapy clinics often rely on orthotics and taping to facilitate healing. However, those methods have a poor track record of providing satisfactory results, and patients often resign themselves to living with a certain level of pain.
At NYDNRehab, our technological toolbox gives us a variety of treatment options that are clinically proven to speed healing and eliminate pain. Your treatment plan may include:
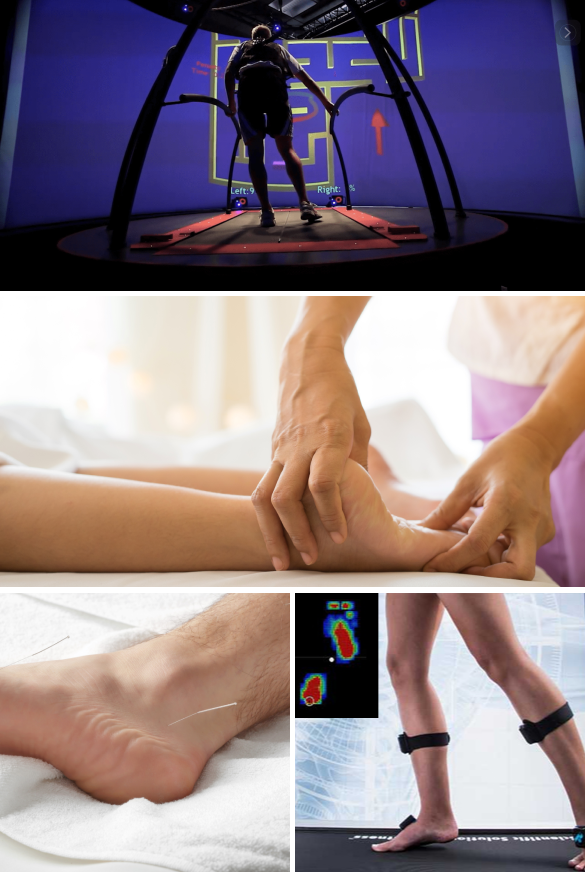
The human body has its own innate healing mechanisms driven by the immune system, but some tissues are more resistant to healing than others. Regenerative technologies help to jump-start the healing process by introducing and/or activating biological factors that stimulate and speed up healing.

Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.


EPAT, also known as radial shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels.



PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.