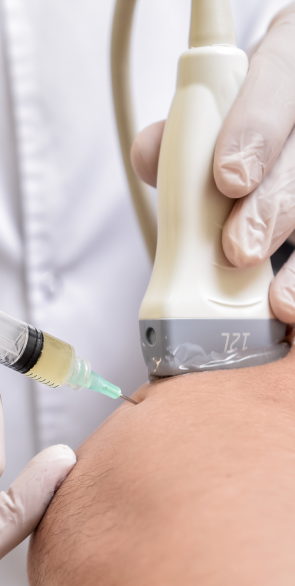
About Fibromyalgia
Fibromyalgia is a pain syndrome that affects the muscles and nerves throughout the entire body. While fibromyalgia symptoms may occur at any age in both males and females, it is most prevalent in women, beginning in middle age. The underlying cause of fibromyalgia is not fully understood, but there is growing evidence to suggest that symptoms are caused by a hypersensitized autonomic nervous system that sends amplified pain signals to the brain, in the absence of structural damage or injury. Chronic systemic inflammation is suspected to be a contributing factor.
New research sheds significant light on how the body becomes hypersensitized, and new technology offers hope for patients suffering from fibromyalgia symptoms.
Dr. Kalika has devoted his career to finding the most advanced and effective ways to treat physical pain, dysfunction and injuries. He has embraced new technologies and sought out innovative therapeutic treatment methods to provide his patients with the best and fastest treatment solutions.
Patients suffering from fibromyalgia pain and fatigue often wander from doctor to doctor, spending untold time and money seeking medical solutions, or exploring alternative treatments like acupuncture, without resolving their pain. When they run out of options, they often give up hope, resigning themselves to a life of pain and fatigue that infringes on their quality of life.
The human body is an extremely complex organism, and chronic pain requires an integrative approach. Early in his career, Dr. Kalika studied under world renowned professors Karel Lewit and Vladimir Janda, both pioneers in integrative medicine. It soon became clear that allopathic medicine had tunnel vision, and that more effective diagnostic tools and treatment options were available to treat pain syndromes.
Dr. Kalika is an innovator when it comes to applying technology to fibromyalgia treatment. He has published multiple scientific papers on myofascial trigger points, ultrasound guided dry needling, and the application of shockwave therapy to treat fibromyalgia. He is a skilled and seasoned expert in diagnostic ultrasonography.
For injection and regenerative therapies, Dr. Kalika teams up with Dr. Uri Brozgol, a neurologist with 20+ years of experience in treating pediatric and adult myofascial pain. Dr. Brozgol is an expert in orthobiologic injection procedures and fascial release techniques. Dr. Kalika is an active member of the International Myopain Society. You can find more information about Dr. Kalika’s research here.
Orthobiologic specialist
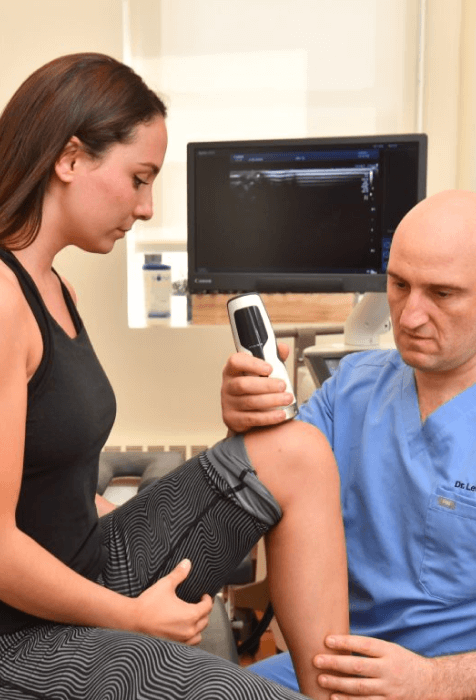
Identifying and treating underlying issues prior to beginning physical therapy is key to getting fast and effective results. Failure to do so can completely undermine your treatment protocol, and in some cases, your condition may even worsen.
At NYDNRehab, we use a broad range of advanced technologies and innovative therapeutic approaches to resolve issues that can potentially undermine the success of physical therapy. Our talented staff is certified in a diverse array of treatment methodologies, rarely found in run-of-the-mill physical therapy clinics. Our one-on-one sessions are personalized, based on the patient’s unique diagnostic profile.
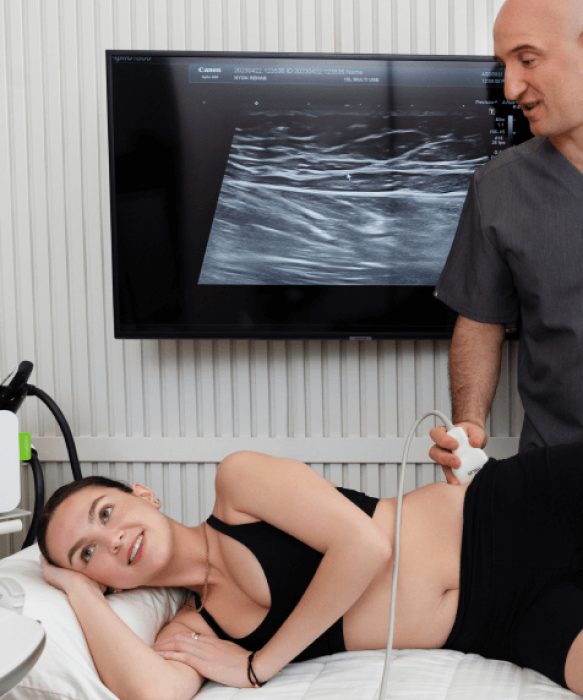
NESA neuromodulation is a new type of therapy that uses the body’s own electrical pathways to manipulate the autonomic nervous system. Neuromodulation works by actively stimulating nerves to produce a natural biological response in nervous tissue. NESA is a non-invasive neuromodulation therapy that helps to calm overstimulated nerves, to restore the autonomic nervous system to a balanced state where it can function at its best.
Dr. Kalika recently traveled to Spain to learn about NESA neuromodulation therapy, and to receive first-hand training from the technology’s source. NYDNRehab is one of the few clinics in NYC to offer NESA neuromodulation therapy to our patients. Dr. Kalika is one of a handful of practitioners with advanced training and experience in Zimmer and NESA neuromodulation therapy.
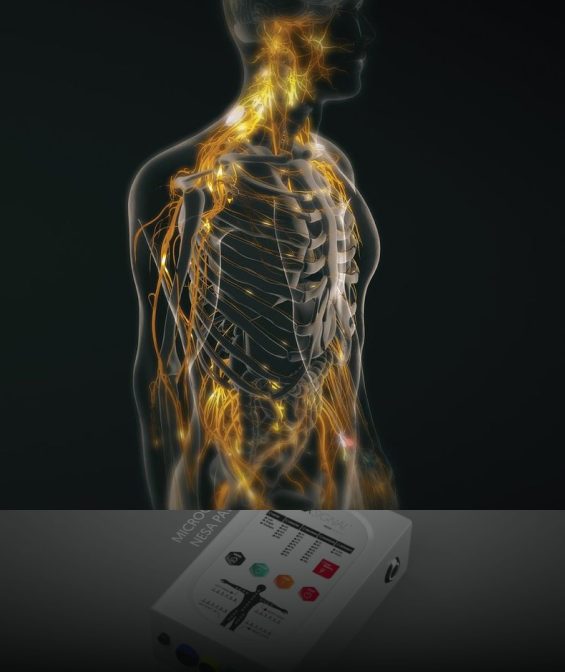
People suffering from fibromyalgia symptoms are often willing to try anything to ease their pain. Many try to modify their diets or take nutritional supplements in hopes of reducing symptoms. But while improving a poor diet is bound to have a positive impact on overall health, there is very little scientific evidence to support a dietary approach to fibromyalgia treatment.
At its core, fibromyalgia is a central sensitization disorder, with systemic inflammation as a contributing factor. As such, we believe the primary course of treatment should be geared to restoring optimal function of the nerves and muscles, which may help to alleviate symptoms.
The clinic at NYDNRehab features some of the most advanced technologies available, to calm hypersensitized nerves and elicit a prolonged anti-inflammatory effect.

Focused ESWT technology produces high frequency sound waves to reduce pain and inflammation and stimulate the body’s own reparative mechanisms.
Our new PiezoWave shockwave machine features MyACT, a new type of focused shockwave technology that allows for deeper compression of the focused waves. Its higher frequency allows for precise neuro modulation under ultrasound guidance, with a special linear head for treating myofascial pain.
This innovative shockwave technology transforms the mechanical energy of shockwaves into biochemical signals that precisely target damaged tissues. Its versatile system of controls lets us fine-tune its output levels for precise and personalized patient care. With MyACT, we are able to repair and regenerate damaged tissues by stimulating the body’s own reparative mechanisms.

EPAT, also called radial shock wave therapy, is not a true shockwave, but uses mechanical pressure waves that are much weaker than focused shockwaves. EPAT is most useful in regenerating fascia fibroblasts and eliminating fascia densifications.
EMTT transmits high energy magnetic pulses that synchronize with your body’s own magnetic fields, triggering a regenerative response in tendons, muscles, bones and nerves.


INDIBA therapy helps to restore the ionic charge of damaged cells, for faster injury healing.
The NESA device generates a biphasic low-frequency electrical current that travels through autonomic neural pathways, to restore optimal neural signaling to the brain.


High Energy Inductive Therapy (HEIT) is a new technology that uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT relieves pain by restoring peripheral nerve function.
Laser therapy is a non-invasive approach to treating chronic pain that reduces inflammation, eliminates pain and speeds up tissue healing. The treatment uses light energy to penetrate your skin, muscle, nerve, and connective tissues, stimulating a photochemical reaction that changes the chemical and physical properties of the affected area at the molecular level

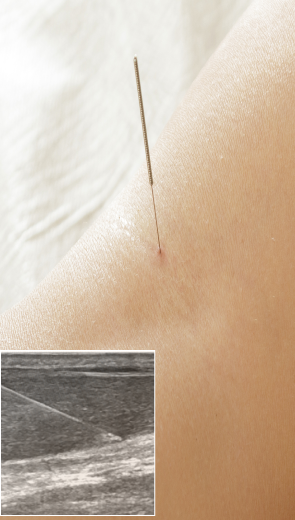
Myofascial trigger points often contribute to lower back pain. Dry needling is an outpatient procedure that inserts non-medicated needles into the trigger point to evoke a twitch response, releasing the trigger point and immediately relieving pain. Ultrasound guidance eliminates the need for multiple insertions, reducing pain and discomfort for the patient.
Hydrodissection is a technique for treating peripheral nerve entrapment. It uses a saline solution to separate entrapped nerves from surrounding fascia adhesions or adjacent structures.