The sciatic nerve is the largest nerve in the human body, with its roots emerging from the lower spinal vertebrae L4 to S3, and merging to form a single nerve that runs down the leg, all the way to your feet. When sciatic nerve roots are compressed, usually by an inflamed disc, pain is most commonly felt on one side of the lower back. But sciatic nerve compression or entrapment can occur anywhere along the nerve’s path, causing pain, numbness and tingling in the buttocks and the back of the legs.
Sciatic nerve compression often arises in the subgluteal space, where the nerve glides among various muscles and structures on its path to innervate the lower extremities. Muscle hypertrophy from exercise, or muscle inflammation from injury, can narrow the spaces where the sciatic nerve glides among other structures, causing painful compression.
Subgluteal pain syndrome can also arise from damaged fascia that has become densified and sticky, interfering with the nerve’s ability to glide. The nerve can become entrapped at the site of fascial adhesions, causing pain and disrupting muscle action. And recent research suggests that subgluteal pain may be associated with suboptimal movement in the hips and pelvis.
For decades, the space where the nerve passes near or through the piriformis muscle was thought to be the main site of subgluteal nerve compression. But thanks to advancements in diagnostic ultrasonography and MRI neurography, we now know that sciatic nerve compression can occur at multiple sites within the subgluteal space.
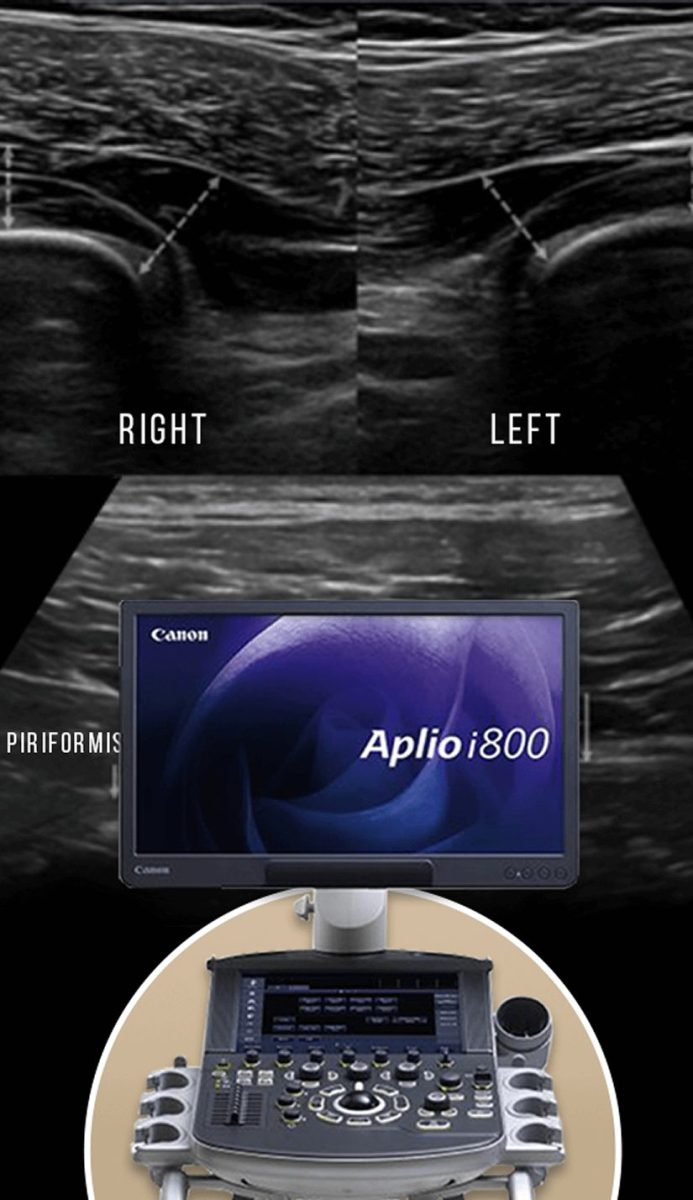
High-resolution ultrasound allows us to visualize dynamic nerve compressions with remarkable clarity, as they happen. Ultrasound allows us to trace the entire path of the sciatic nerve from its roots to the distal thigh, and provides the ideal tool for visualizing the sacroiliac ligaments. The technology allows us to consider anatomical nuances that distinguish one patient from the next, allowing for more personalized treatment.
We also use ultrasound imaging to guide our regenerative and orthobiologic therapies, for precision in targeting different tissue types.
Dr. Lev Kalika, DC has over 20 years of clinical experience in successful injury rehabilitation, and effective treatment of pain syndromes and movement disorders. Throughout his career, Dr. Kalika has remained on the cutting edge of new research, advanced technologies and innovative therapies that support the human body’s innate ability to regenerate and self-heal. Dr. Kalika is a recognised expert in diagnostic ultrasonography, with multiple research publications to his credit.

Orthobiologic, Sports Medicine and Regenerative Medicine Specialist
As a pain syndrome, sciatica is often painted with a broad brush, and many chiropractors and physical therapists take a cookie cutter approach to sciatica treatment, despite vast differences in patient anatomy and the location of nerve compression. It is important to remember that pain is a symptom, and not a condition in and of itself, and to only treat the pain is to ignore its cause.
A painful sciatic nerve is often inflamed, and efforts to treat it with physical therapy exercises and stretches can actually cause further compression, doing more harm than good. At the same time, pain management efforts using steroid injections and nerve blocks may relieve pain in the short term, but they inevitably fail because they don’t address the underlying source of pain.
At NYDNRehab, we conduct dynamic testing of the subgluteal space using high resolution ultrasound. By visualizing the sciatic nerve along its path, we can identify the exact location where muscles or fascia compress or entrap the nerve, often due to abnormal movements in the hips and pelvis. Such precision cannot be achieved with static images generated by MRI.
We never take a one-size-fits-all approach to patient care. Our one-on-one personalized treatment protocols are tailored to the patient, based on their specific diagnostic results. Understanding the underlying mechanisms of sciatic nerve pain ensures successful treatment that quickly eradicates sciatica.
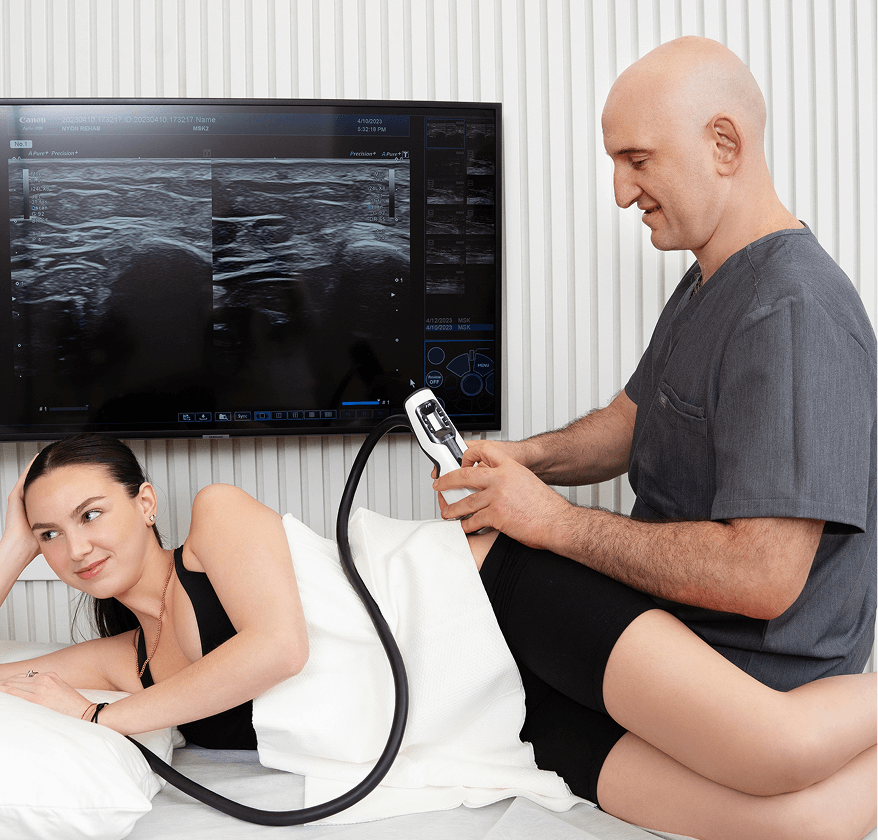
When guided by high resolution ultrasound imaging, focused extracorporeal shockwave therapy (ESWT) is an evidence-based therapeutic approach to treating nerve entrapments, peripheral neuropathy and neuralgia. Dr. Kalika is an expert in neural ultrasonography and extracorporeal shockwave therapy. Shockwaves not only relieve pain and reduce inflammation, but their regenerative properties attract growth factors and stem cells to the treatment site, to promote tissue regeneration.
Most injuries involve more than one tissue type, and different tissues respond best when the shockwaves are fine-tuned in terms of frequency, intensity, depth and width of penetration. At NYDNRehab we use multimodal shockwaves to optimize patient outcomes. Dr. Kalika’s expertise in shockwave therapy coupled with his mastery of dynamic ultrasonography ensures that patients receive the most appropriate and efficacious shockwave therapy for their unique condition.
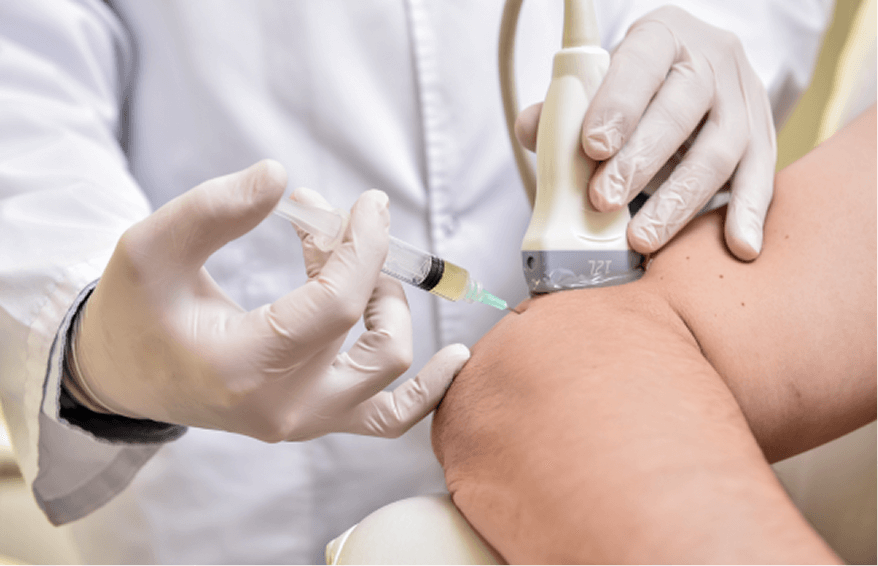
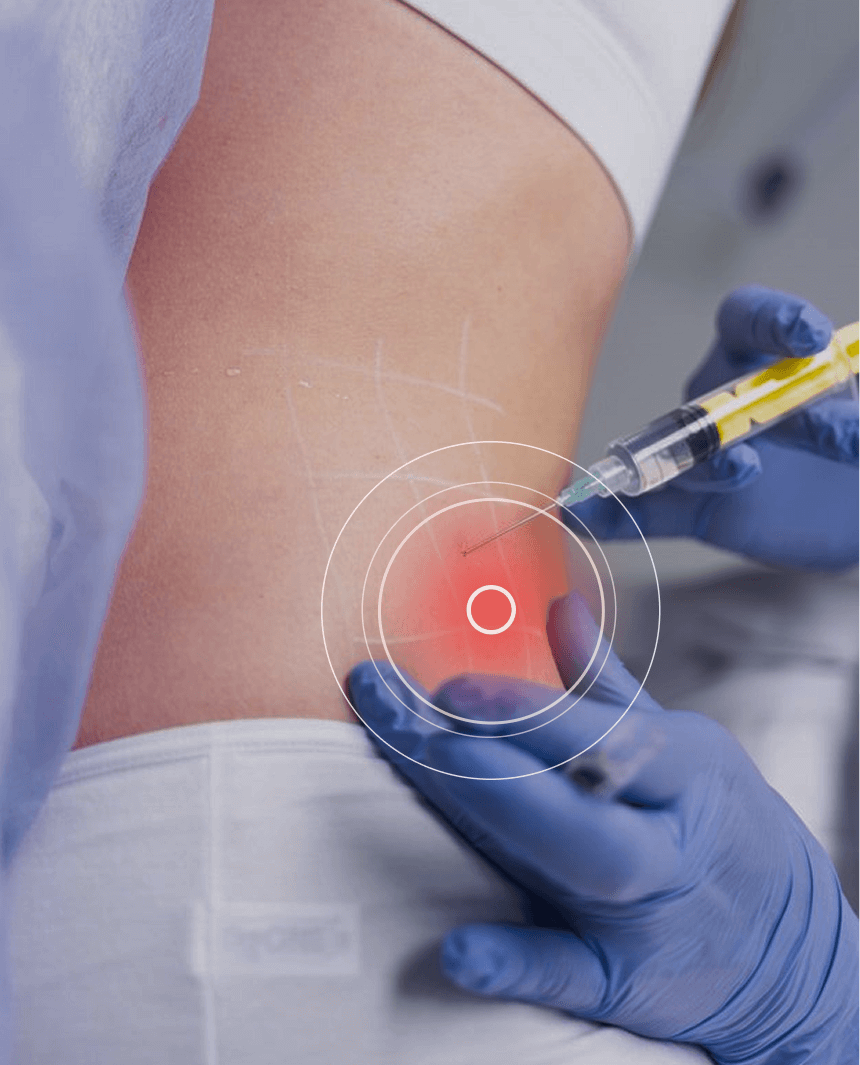
Sciatic nerve pain is often caused by nerve entrapment in the subgluteal space, captured by densified fascia that prevents the nerve from gliding. Hydrodissection is a procedure where a saline solution is injected into densified fascial layers under ultrasound guidance. The solution works by separating fascial layers and freeing up entrapped nerves and blood vessels. We often use hydrodissection in conjunction with ESWT and manual fascial manipulation.
Fascia is a thin tough web of collagenous tissue that connects and encases soft tissues and organs throughout the body. Fascia and muscles work together to create elastic tension that guides and controls movement, holds various structures in place, and helps to distribute force loads. Healthy fascia is elastic and slippery thanks to its high concentration of hyaluronic acid, a gel-like substance that holds water within the tissue. Fascia can become injured by trauma, repetitive overuse, or disuse, losing its slippery and elastic properties, and becoming dense and sticky.
It is estimated that densified fascia is responsible for up to 50% of musculoskeletal pain and reduced mobility. Research shows that deep friction fascial manipulation can help to separate densified hyaluronic acid (HA) chains, disentangling them to restore their functional properties. Dr, Kalika is certified in Stecco Fascial Manipulation, an evidence-based methodology for treating densified fascia that restores its ability to stretch and glide.
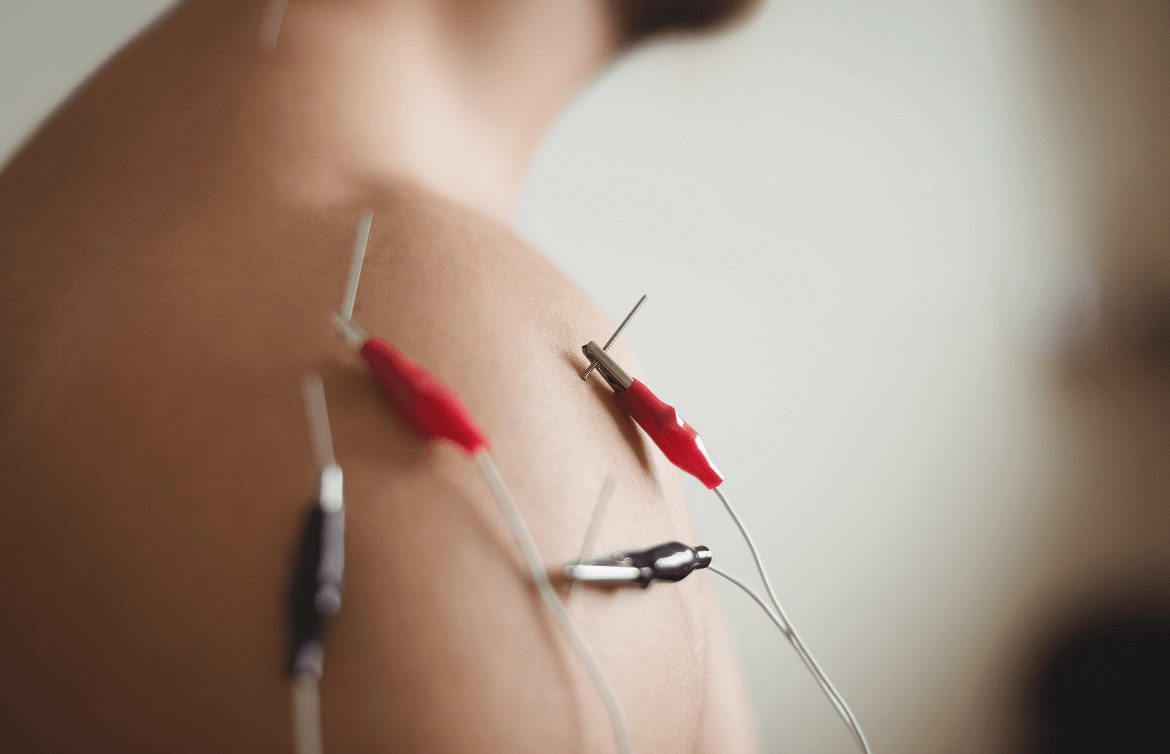
During PENS treatment, filament-thin needles are inserted through the skin into muscle tissue adjacent to the targeted nerve. A low frequency electrical current is then delivered via the inserted needles to stimulate the dysfunctional nerve. PENS normalizes nerve activity, improves brain plasticity and optimizes muscle coordination patterns.
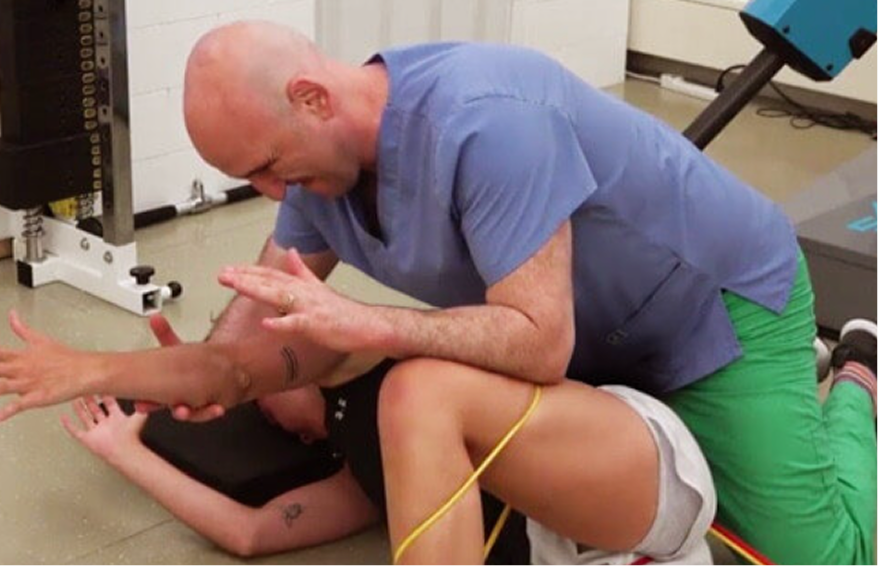
Only after pain and inflammation have been addressed, and fascial gliding has been restored, can physical therapy be effective in correcting posture, normalizing joint movement, and balancing muscle tension in the lower back and subgluteal space. Nerve flossing exercises may be introduced to eliminate friction and restore uninhibited sciatic nerve gliding.
A recently published 2025 study compared the efficacy of corticosteroid injections to that of ESWT in patients suffering from piriformis syndrome, where the sciatic nerve becomes entrapped by an enlarged piriformis. The researchers concluded that both approaches were equally effective in significantly relieving pain. However, unlike steroid injections, ESWT does not cause long-term degenerative side effects. In fact, ESWT has regenerative properties that build up tissue rather than breaking it down.
In the majority of cases, sciatic nerve pain does not arise out of nowhere – nerve compression often develops over time due to habitual behaviors and lifestyle factors that change the way your body’s structures interact. Subtle changes can have a huge impact on your sciatic nerve and overall health.
Try these strategies to reduce your risk of developing sciatic nerve pain:

These case studies reflect real clinical conditions evaluated at NYDNRehab using advanced diagnostic methods and individualized rehabilitation strategies. All cases are evaluated and managed by Dr. Lev Kalika and the NYDNRehab clinical team.
Independent peer-reviewed research relevant to this treatment approach.
Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.