Many people suffer from some form of chronic headaches, and most medical practitioners rely on drugs to help patients alleviate pain. But drugs only mask your headache symptoms – they do not get to the source. While it may be normal to have an occasional stress headache, chronic and recurring headaches signal a more complex problem that cannot be solved with drugs.
Most headaches originate along the cervico-mandibular-ocular axis and cervical spine, and eliminating headaches for good requires a holistic approach to treatment.
or
Dr. Kalika’s mission is to change the way chiropractors and physical therapists treat common conditions like headaches. Patients with chronic and recurring headaches often go from doctor to doctor without finding a lasting solution. Drugs only mask headache symptoms without addressing their source.
Dr. Kalika uses his expertise in diagnostic ultrasonography to visualize the cervical muscles and fascia along the ligamentum nuchae bridge – the main supporting structure of the cervical spine that cannot be visualized with MRI. Diagnostic ultrasound confirms the accuracy of our clinical assessment and reveals anatomical issues that contribute to your headaches. Accurate diagnosis is the ultimate key to successful treatment. The headache specialists at NYDNRehab go beyond treating your symptoms to discover the true source of your headaches, eliminating them for good. Satisfied patients agree that Dr. Kalika is the best headache specialist in New York.
Conventional medicine has attempted to treat chronic and migraine headaches for decades without success. Despite multiple drugs and treatment approaches, most interventions aim to mask headache symptoms without addressing the underlying cause. Today’s modern reductionist approach to headache treatment fails to acknowledge the integral relationship between recurring headaches and issues along the cervico-mandibular-ocular axis and cervical spine, where most headaches originate.
At NYDNRehab, we take a holistic integrative approach to headache and migraine treatment. Unlike conventional clinicians who only treat headache symptoms, our personalized one-on-one approach considers the whole patient to find key factors that contribute to frequent headaches. We use your unique patient profile to create a customized treatment protocol aimed at resolving issues that are the source of your headaches, to eliminate them for good.

Chronic headache syndrome is defined as having at least 15 recurring headaches in a given month. Headaches can be further categorized as primary or secondary headaches.

Primary headaches originate organically in the human body, with "short" headaches lasting less than 4 hours, and "long" headaches lasting longer than 4 hours. Chronic migraine and tension headaches typically fall into the "long" category.

Secondary headaches arise from other factors and conditions such as medications, tumors, infections, intracranial pressure, metabolic disorders and structural pathologies.
The underlying causes of chronic primary headaches are not well understood by medical practitioners. Chronic headaches can have multiple contributing factors, and clinicians should explore the full spectrum of possible causes before prescribing treatment.
Chronic migraine headaches are typically unilateral (one-sided), with pulsating moderate to severe pain. They may or may not have an aura.
Chronic tension-type headaches are normally bilateral and do not pulsate. The skull may be tender when palpated.
Medication overuse headaches are secondary headaches brought on by use of pharmaceutical medications and/or substance abuse.
Hemicrania continua headaches most commonly occur in adult females. They are unilateral and continuous, lasting more than three months, with intermittent high-intensity episodes. They may be accompanied by agitation and restlessness.
Daily persistent headaches are a rare and unpredictable phenomena, with ongoing symptoms that can last for years. The onset is sudden, with mild to severe pain. They occur most often in teen and adult females.
While each type of headache may have unique characteristics, they all share certain features, including sensitization of the trigeminal system, changes in brain structure and function, and various environmental factors.The trigeminal nerve is the fifth and largest of the cranial nerves, and innervates the muscles that enable mastication (chewing).
Cervicogenic headaches are a type of primary chronic headache that originates in the upper cervical spine. They are thought to be caused by a neck disorder, or by missignalling from the proprioceptors that are responsible for maintaining equilibrium.
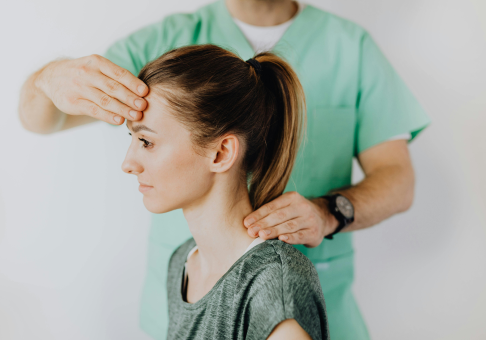
Chronic headaches and migraines rarely originate in the brain. They often involve the temporomandibular joint and masticatory muscles and fascia along the cervico-mandibular-ocular axis, or the upper cervical spine.
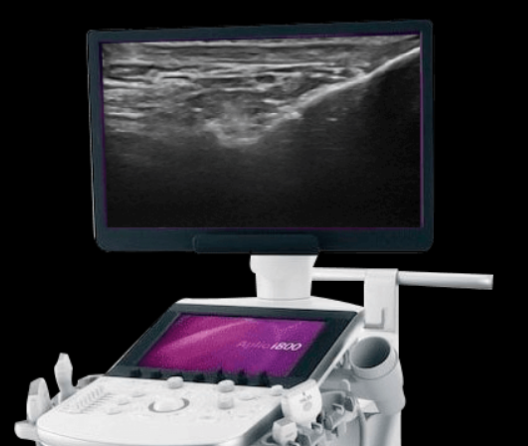
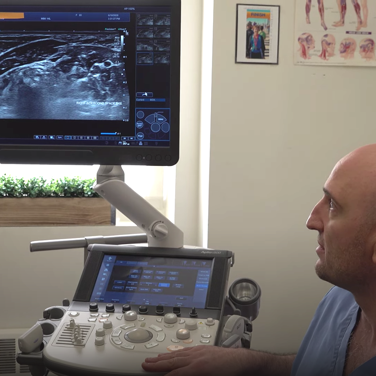
At NYDNRehab, we use high-resolution diagnostic ultrasound to visualize the structures and tissues most commonly associated with chronic headaches. Dynamic ultrasound imaging lets us view muscles, fascia, joints and nerves in real time, to see how they function and interact, to identify issues that may be contributing to your headaches.
As part of your clinical exam, we thoroughly review your health history and lifestyle behaviors to rule out secondary factors.
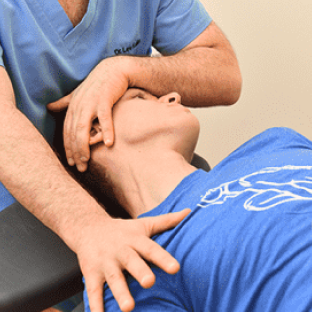
Depending on your diagnostic profile, we use a holistic multimodal approach to treat your chronic headaches at their source.
Your treatment protocol may include a combination of the following:
As is true of most chronic conditions, lifestyle factors can play a key role in the frequency and severity of headaches. Lifestyle factors that contribute to chronic headaches include:
Poor posture
Sedentary lifestyle
Alcohol and substance abuse
Muscle imbalances
Muscle tightness in the upper back and neck
Chronic stress
Poor sleep habits
Too much screen time
Fluorescent and LED lighting
Highly processed foods
Nutrient deficiencies
Chronic dehydration
All of these factors can be modified and controlled. Your physical therapist or chiropractor can help you make positive lifestyle choices that help get rid of chronic headaches. Without lifestyle changes, no amount of drugs or therapy can permanently get rid of your headaches or improve your health.

If your chronic headaches have sent you from doctor to doctor without satisfactory results, it's time to get drug-free holistic therapy that really works. You can find the best headache specialists in NYC at NYDNRehab in Midtown Manhattan. Don't let chronic headaches and migraines keep you from enjoying life to its fullest. Contact NYDNRehab today, and get personalized one-on-one headache treatment, designed just for you.

Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.