Shoulder Specialist for Chronic and Unresolved Shoulder Pain
Our holistic systems-based approach integrates advanced diagnostics with non-surgical shoulder rehab.
Advanced Non-Surgical Care for Persistent and Unresolved Shoulder Conditions
Most shoulder pain improves with standard physical rehabilitation and conservative care. However, some patients continue to experience symptoms, even after physical therapy, injection procedures, and surgery.
Due to the shoulder’s complex architecture, stubborn and persistent shoulder pain often involves more than one structure. Complex shoulder cases often require a more detailed clinical evaluation, with a coordinated, systems-based, non-surgical strategy.
When to Consider a Shoulder Pain Specialist
Consult a shoulder specialist if:
In persistent cases, contributing factors are often involved that were not previously identified. Evaluation by a specialist can help to identify secondary factors and provide the foundation for a new treatment strategy.
Specialist Expertise for Complex Shoulder Disorders
Dr. Lev Kalika, DC, RMSK, clinical director of NYDNRehab, has advanced training in musculoskeletal ultrasound and movement-based rehabilitation. His clinical focus includes complex and persistent shoulder conditions where symptoms do not clearly match imaging findings.

Dr. Yuri Brosgol
Dr. Kalika works alongside Dr. Yuri Brosgol, MD, whose medical background contributes to comprehensive evaluation of persistent or difficult-to-diagnose shoulder problems. Their collaborative approach emphasizes identifying the dominant pain driver and integrating targeted non-surgical treatment with rehabilitation.
Why Persistent Shoulder Pain Can Be Complex
The shoulder is a complex joint comprising and interacting with multiple structures, and shoulder pain cannot be effectively evaluated or treated in isolation. Multiple factors come into play, such as scapular mechanics, kinetic chain coordination, and neural factors that influence shoulder pain patterns.
Persistent symptoms often involve a combination of factors:
In one clinical case, persistent dysfunction continued after a rotator cuff tear was overlooked during initial care, demonstrating how an incomplete early assessment can delay recovery.
Read our case study: “Missed Full-Thickness Rotator Cuff Tear”
Our Specialist-Led Diagnostic Approach
When shoulder pain persists after initial treatment, precise evaluation becomes critical.
Our advanced diagnostic process helps to clarify the underlying drivers of persistent symptoms, where standard imaging and routine therapy has failed to provide lasting relief
Conditions like adhesive capsulitis (frozen shoulder) typically have a gradual onset, with no specific trauma. Without thorough clinical evaluation, such conditions can be difficult to identify early-on. A specialist-led diagnostic evaluation can uncover key factors that were overlooked during routine care.
Read our case study: “Adhesive Capsulitis / Frozen Shoulder”
Our Shoulder Evaluation Process
Persistent shoulder pain requires more than a routine assessment. Our advanced process follows four key phases, aimed at uncovering hidden drivers of pain, and laying the foundation for a targeted recovery plan.





Our Treatment Strategy

Advanced Treatment Approaches Often Prevent or Delay Surgery
Patients with persistent post-treatment shoulder pain are often told that surgery is their only remaining option. However, in many cases, persistent symptoms may be caused by factors that do not directly involve the shoulder joint. Factors such as uncoordinated muscle firing patterns, fascial dysfunction, imbalanced muscle tension, and neural factors can all be addressed without surgical intervention.
As experienced shoulder specialists, our role is to determine whether a targeted non-surgical plan would be beneficial before considering surgical intervention. In one clinical case, the patient’s symptoms persisted, not because of structural failure, but due to movement coordination issues that were successfully resolved with conservative rehabilitation.
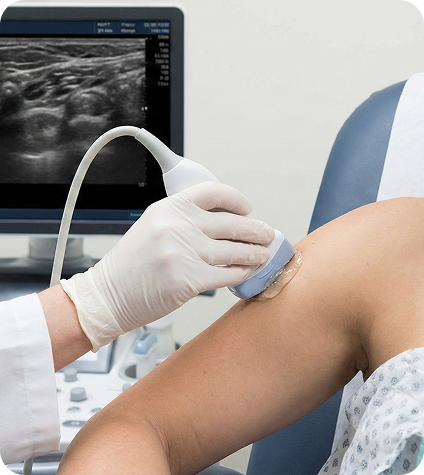
We Use Targeted Procedures When Clinically Indicated
Many clinics are eager to adopt the latest procedures and approaches, cashing in on their popularity in response to customer demand. But not every patient benefits from the latest trends. We use precision ultrasound-guided procedures only when appropriate, as an integral component of your broader rehabilitation plan. When used strategically, ultrasound-guided energy technologies and injection therapies can help to reduce pain and inflammation, accelerate healing, improve tissue gliding, and support functional recovery.
These approaches are not used as stand-alone solutions, but rather as part of a coordinated treatment strategy.

Identifying and Treating the True Drivers of Shoulder Pain
Mechanical factors often play a major role in persistent shoulder pain. Even when standard imaging does not show significant structural damage, uncoordinated movement patterns, inefficient load transfer, and soft tissue restrictions can continue to undermine shoulder stability and mobility.
When performed by an experienced clinician with expertise in shoulder and scapular motion analysis, dynamic high-resolution ultrasound can often detect hidden functional problems. Imaging results must be considered alongside findings from the clinical exam and motion analysis, and interpreted through an expert lens.
Treatment of complex shoulder cases focuses on the underlying mechanical, neural, and fascial drivers of pain. Rehabilitation may include improvement of tissue mobility, nerve irritation relief, restoration of fascial integrity, support of tendon healing, and retraining coordinated shoulder and scapular movement patterns to promote long-term recovery.
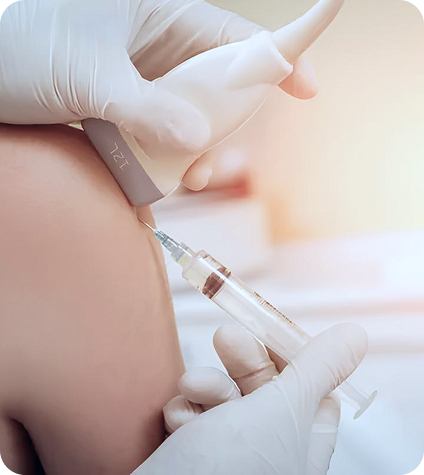
Ultrasound Guided Injection Procedures
Medical doctors often overlook critical factors that stand in the way of tissue healing and functional restoration. Fascial dysfunction, myofascial trigger points, entrapped nerves and blood vessels, and slow-to-heal avascular tissues can delay or even prevent full recovery.
When appropriate, we use injection and needling procedures to stimulate healing in stubborn tendons and ligaments, and to restore the functional properties of fascia, freeing up nerves and blood vessels so they can glide among other structures. Our orthobiologic solutions are used selectively, and guided by high-resolution ultrasound to ensure precision.
While injections and needling procedures do not provide stand-alone solutions, they can be invaluable assets when strategically incorporated into your holistic treatment protocol. In many cases, injection therapy can delay surgery or prevent it altogether.
Integrated Rehabilitation for Long-Term Results
Once we address pain sensitivity and tissue healing, we begin a strategic customized rehabilitation plan.

























































