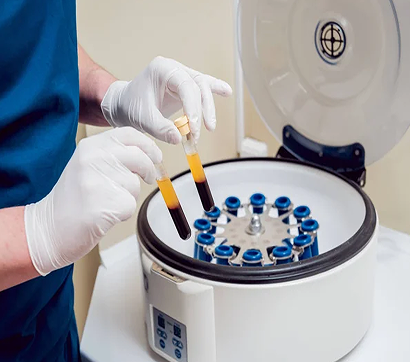
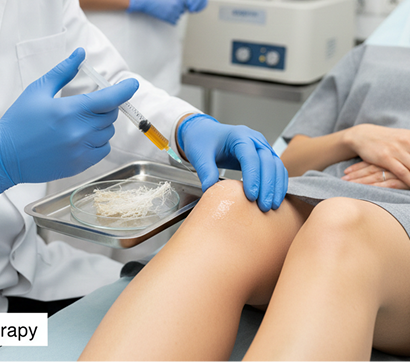
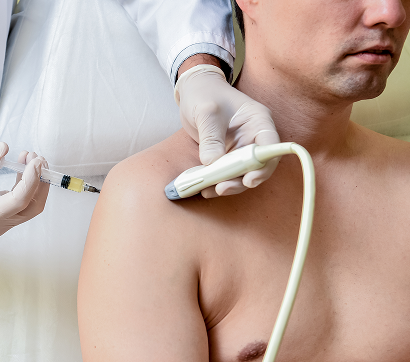
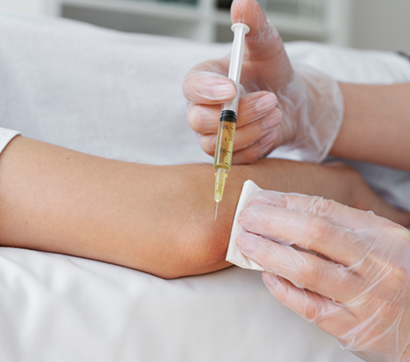
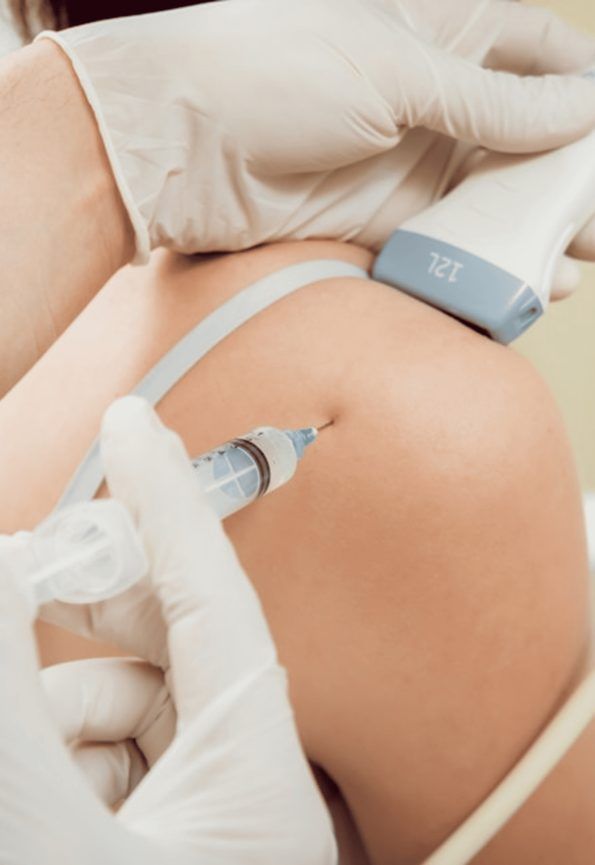
Ultrasound Guided Injection Therapies
Personalized boutique services supported by cutting-edge integrative diagnostics and advanced holistic therapies.
Dr. Kalika and Dr. Brosgol are at the Cutting
Edge of Integrative Medicine
Dr. Lev Kalika, DC, RMSK, clinical director and founder of NYDNRehab, is an expert in integrative physical rehabilitation with over 20 years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. He is an active member of the American Institute of Ultrasound in Medicine (AIUM), and his expertise in diagnostic ultrasonography is recognised by his peers on the world stage, where he frequently presents his own research on ultrasound-guided procedures.
Dr. Kalika is certified by the International Society for Medical Shockwave Therapy (ISMST) to perform extracorporeal shockwave therapy. He has developed his own unique approach to dynamic functional and fascial ultrasonography and has published peer-reviewed research on the topic. He works closely with Dr. Brosgol, providing ultrasound guidance during orthobiologic procedures.

Dr. Yuri Brosgol, MD,is a neurologist with 25+ years of experience in treating myofascial and chronic pain conditions. In addition to being a pioneer in orthobiologics and fascial release techniques, Dr. Brosgol is a functional medicine specialist, providing a holistic and nuanced approach to treating common sports injuries and chronic pain syndromes.
Together, Dr. Kalika and Dr. Brosgol are revolutionizing the way musculoskeletal pain is diagnosed and treated. The clinic at NYDNRehab features some of the most advanced technologies and therapies available for rehabilitative medicine.
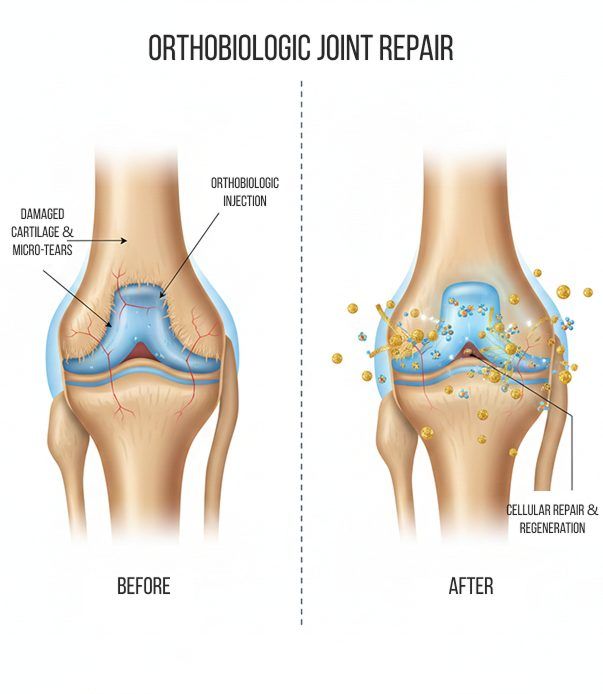
Orthobiologic Injection Therapies
Orthobiologic procedures use biological substances derived from the patient’s own body (autologous), or from a matched donor, to treat damaged tissues. The injected solutions stimulate cellular repair by either nourishing or irritating the targeted cells, triggering an immune response that releases biologically active agents such as growth factors, cytokines, lysosomes, inflammatory mediators, and adhesion proteins.
Orthobiologics are primarily used to treat orthopedic injuries or degenerative conditions involving joints, tendons, ligaments, fascia, cartilage, and spinal structures. Rather than simply masking pain or surgically replacing tissues, orthobiologics contain signaling molecules that trigger the body’s own self-healing mechanisms.
Orthobiologics are not stand-alone miracle cures, and injections are not appropriate for all cases. They work best when incorporated into a personalized treatment protocol based on the individual patient’s blood work, and their metabolic and hormonal profiles. In properly selected cases, orthobiologics can accelerate healing and help patients to delay surgery or avoid it altogether. Best results come from a carefully planned protocol that includes energy therapies and physical rehabilitation.
Evidence-Based Use Cases for
Orthobiologics
The use of orthobiologics is supported by a growing body of research, and its use cases continue to expand as patients experience positive outcomes. However, orthobiologics do not present an all-encompassing solution for musculoskeletal complaints, and consumers should be wary of clinics that promote them as a quick fix for pain and dysfunction.
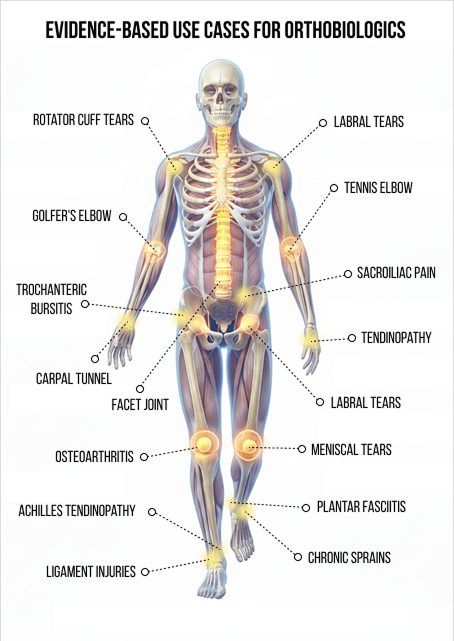
- Osteoarthritis of the knee, hip, shoulder, ankle, wrist, and foot
- Tendinopathies affecting the lateral and medial epicondyle (tennis and golfer’s elbow)
- Tendinopathies of the patella, Achilles, rotator cuff and gluteal tendons
- Partial tendon and ligament tears of the rotator cuff, ulnar collateral ligament (UCL), and chronic ankle ligament injuries
- Plantar fasciitis
- Meniscal tears – especially degenerative tears in older patients
- Low back pain from facet or sacroiliac joints
- Chronic ligament sprains (e.g., chronic ankle instability)
- Cartilage erosion or defects
- Trochanteric bursitis and gluteal pain syndrome
- Labral tears of the hip and shoulder
The list of use cases continues to grow, but it is important to emphasize that orthobiologics do not provide a stand-alone solution. For effective and lasting results, injections should be used in conjunction with energy therapies and physical rehabilitation, and treatment should be personalized to match the patient’s unique pathology and medical profile.
Diagnosing Candidates for Orthobiologic Therapies
At NYDNRehab, not every patient who comes through our doors is a viable candidate for orthobiologics. We do not have a preset formula for screening patients or delivering injections – our diagnosis is based not only on a structural diagnosis, but on a clinical correlation with the patient’s condition, their health status, and their blood, metabolic and hormonal profiles.
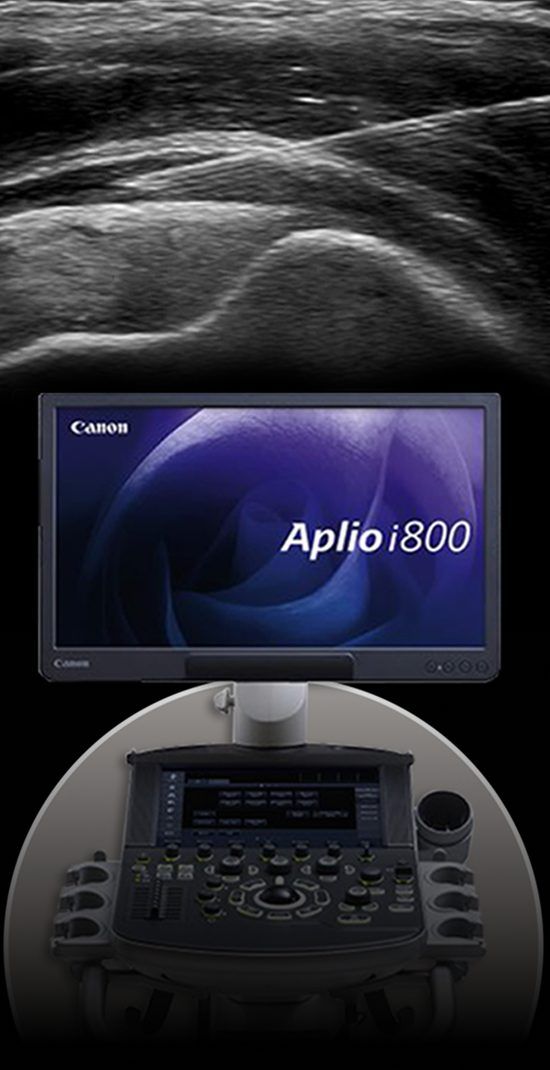
Our treatment decisions are based on our findings from a multi-tissue, multi-joint examination of the entire kinetic chain using high-resolution diagnostic ultrasound, recognizing that most musculoskeletal pathologies originate from structures outside the locus of pain. Diagnostic ultrasonography exceeds the limitations of MRI, giving us the ability to visualize multiple tissues, joints, nerves, and blood vessels in a single session, in real time.
In general, a good candidate for orthobiologics meets most of the following criteria:
- The condition is mild-to-moderate, with enough healthy tissue to work with.
- Healthy tissues in younger patients respond better to orthobiologic-generated growth factors, although older patients may benefit on a case-by-case basis.
- Patients with metabolic comorbidities are generally less responsive to injections.
- Chronic injuries lasting more than 3-6 months will benefit more than acute injuries.
- The patient’s pathology should be well-defined.
- The affected tissues should not be severely atrophied or unstable.
- The patient’s expectations should be realistic, knowing that healing takes time, and more than one injection may be necessary.
In most cases, orthobiologics are contraindicated for:
- Patients at end-stage “bone-on-bone” osteoarthritis.
- Severely obese patients.
- Young, active patients with complete full-thickness tendon ruptures.
- Patients with a history of ongoing corticosteroid and/or NSAID use.
- Patients with active rheumatoid or psoriatic arthritis.
- Patients with an active infection or malignancy.
- Heavy smokers.
Criteria for Successful Outcomes
While the early use of orthobiologics was somewhat hit-or-miss, today’s procedures have become more refined and targeted, thanks to multiple high-level studies and professional registries that define the criteria for highly successful outcomes.
- Appropriate patient selection based on biologic markers, lifestyle factors. and NSAID/cortisone use that interferes with the inflammatory healing response.
- Appropriate disease pathology, based on severity, chronicity, and complexity.
- High quality and concentration of the selected orthobiologic.
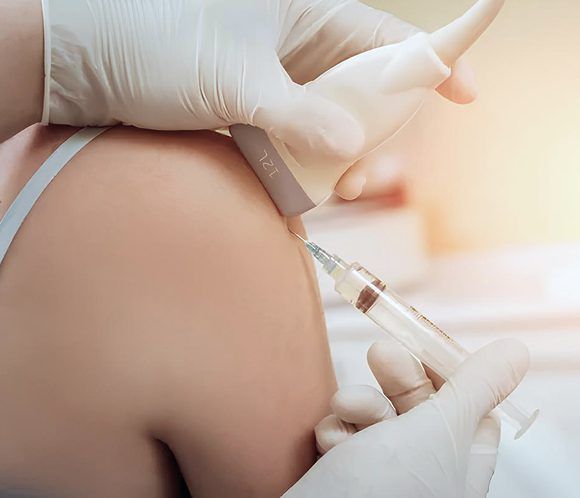
- Injection accuracy – blind injections miss the target 30–60% of the time, and they can accidentally penetrate nerves and blood vessels. Guidance with high resolution ultrasound dramatically improves precision.
- Appropriate pre- and post-injection protocols, including energy therapies and physical rehabilitation.
At NYDNRehab, our holistic approach means our injection procedures are not just intratendinous or intra-articulate – we inject the entire kinetic chain, ensuring optimal fascial and ligament tensegrity, proper force transfer, and restoration of fascial and nerve gliding. We look at the whole person and the entire kinetic chain, paying special attention to the interactions of ligaments, nerves and fascia during movement. Each injection is personalized, based on these factors.
The following table highlights the success rates of injections that meet these criteria:
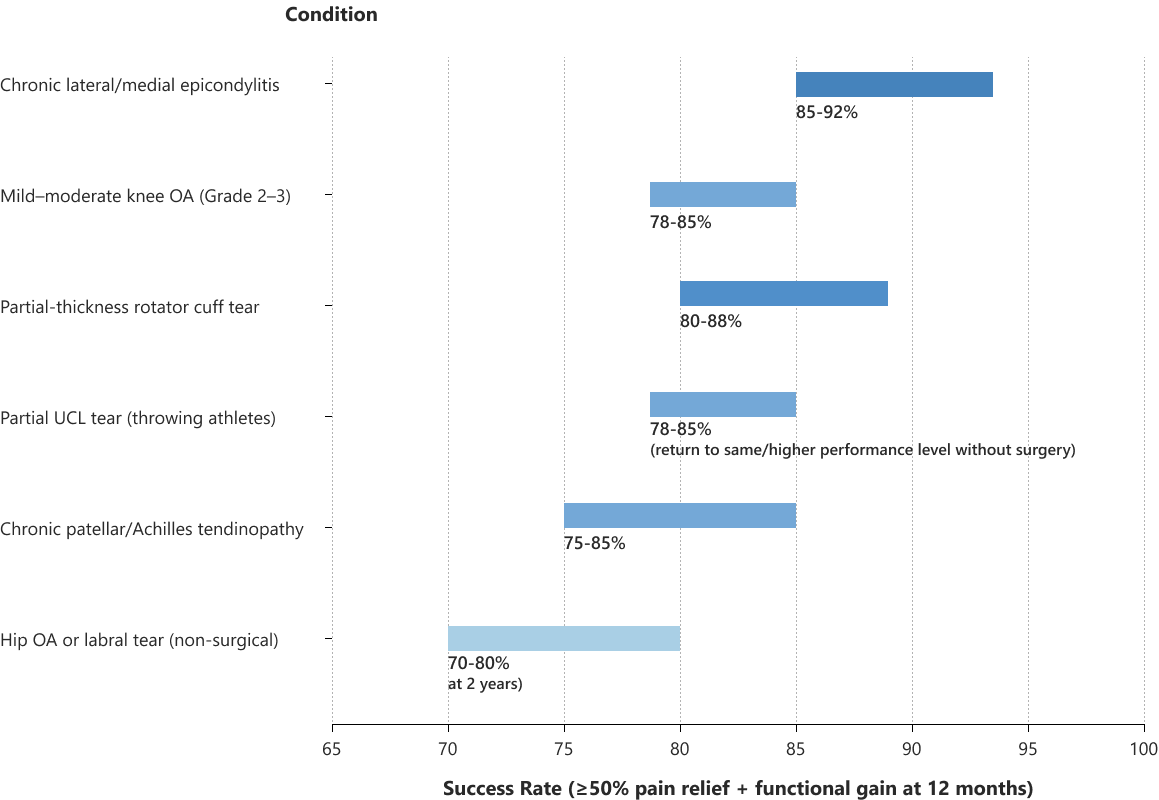
Today, the success of injection therapies is highly predictable for healthy patients with an accurate diagnosis, and treated with a high-quality biologic, injected under ultrasound guidance, and supported by energy therapies and targeted physical rehab.
Orthobiologics at NYDNRehab
At NYDNRehab, our personalized holistic approach means that each patient receives customized treatment, based on their unique profile. Our selection of the type of orthobiologic solution is based on multiple factors, and no two patients receive the exact same treatment.
The patient’s biologic profile, level of inflammation, location of the pathology within the kinetic chain, and the specific tissue dysfunction are all considered. We may choose to use energy technologies before or after the injection, depending on the synergistic effect we are after.
Multiple factors make orthobiologic procedures at NYDNRehab superior to those offered by other clinics:
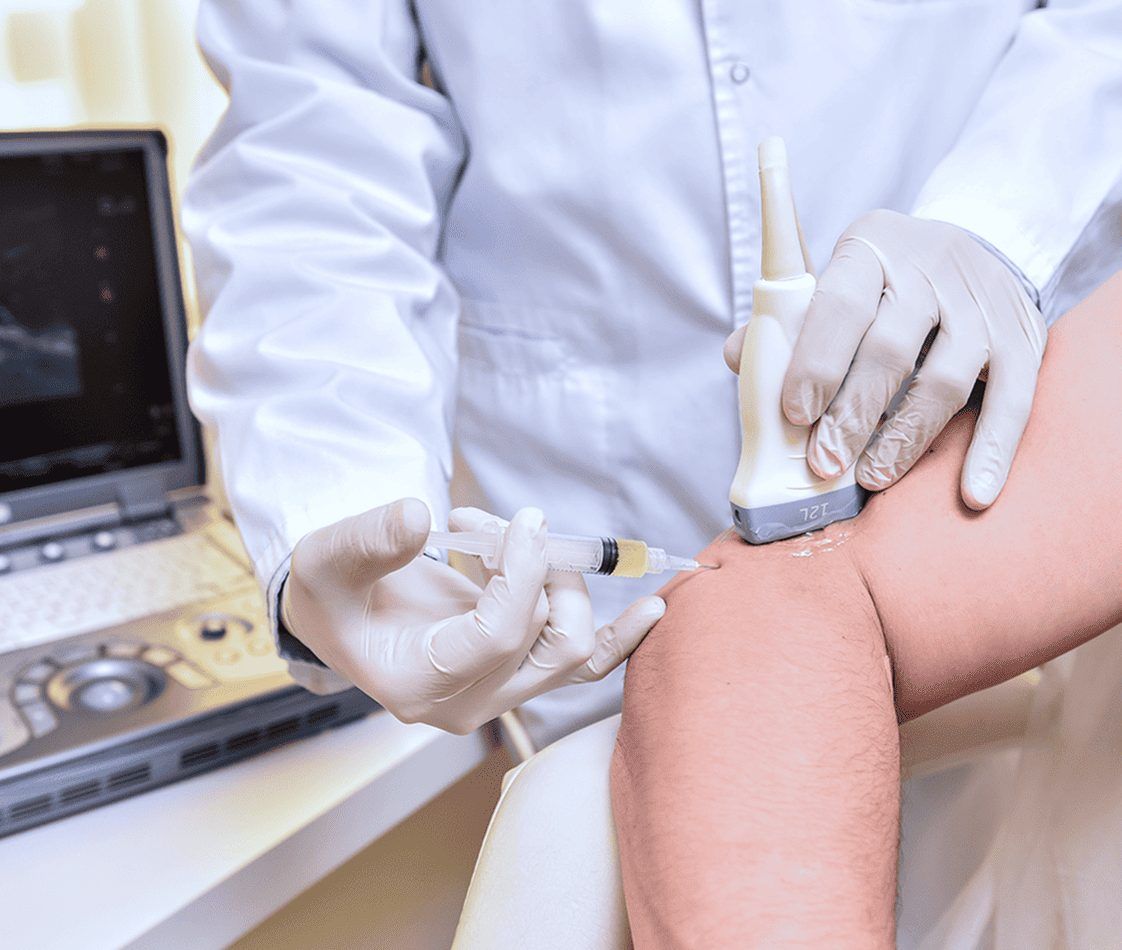
- All procedures are guided by high-resolution ultrasound imaging, ensuring that the orthobiologic solutions precisely penetrate targeted tissues.
- We use the highest-resolution ultrasonography available, with capabilities for sonoelastography and superb microvascular imaging.
- Our platelet-rich plasma (PRP) solutions are formulated with the highest and most efficacious concentration of platelets.
- We offer multiple types of PRP, for tissue-specific results.
- Our ultrasound-guided Prolotherapy injections enhance tissue regeneration.
- Fascial and nerve hydrorelease procedures free up entrapped nerves and blood vessels and restore fascial gliding.

Energy Technologies Support and Synergize
with Orthobiologics
Energy technologies use sound, light, radiofrequency and electromagnetic pulses to reduce pain and inflammation, and stimulate a regenerative response, By carefully selecting and combining the most appropriate therapies, we are able to harness the synergistic effects of both energy technologies and orthobiologics, for superior and enduring results. Depending on the individual patient case, energy technologies may be used before or after your injection, or both.

- Stimulates resident tenocytes/chondrocytes/MSCs; complements PRP/BMAC’s cytokine effect.
- Promotes microvascular regeneration, opening biologic access to hypoxic tendons and their enthesis (point of attachment to bone)
- Upregulates angiogenic growth factors
- Induces nitric oxide and substance P modulation, to provide pain relief without blocking inflammation
- Supports bone–tendon junction healing
- Creates microtrauma and mechanotransduction, releasing growth factors that synergize with injected biologics.
- Induces neovascularization, improving nutrient and oxygen delivery to injected tissues.
- Enhances the homing and activation of stem cells through SDF-1 and VEGF pathways.
- Improves extracellular matrix remodeling, preparing a scaffold for PRP/stem cell integration.
Therapy (EMTT)
- Synchronize with the body’s own magnetic fields
- Helps to extend PRP’s anti-inflammatory effects, prolonging matrix remodeling and angiogenesis
- Promotes remodeling of the extracellular matrix and collagen fiber reorganization
- Reduces fibrotic adhesions and minimizes scarring, especially in tendons, fascia and joint capsules
- Acts as a biological booster to prolong PRP regenerative effects
- Promotes long-term structural repair of tendons, ligaments and joints
- Enhances cell membrane permeability, improving migration, adhesion, and integration of injected PRP/stem cells.
- Stimulates ion channel activity (Ca²⁺, Na⁺, K⁺), supporting regenerative signaling.
- Promotes angiogenesis and microcirculation, improving survival of transplanted cells.
- Reduces oxidative stress and inflammation, creating a favorable niche for stem cell activity.

- Restores the ionic charge of damaged cells, for faster injury healing
- Boosts blood flow and enhances local circulation to improve delivery of nutrients and immune cells to the treatment site
- May improve PRP dispersal
- Promotes fibroblast activity and collagen remodeling at PRP treatment site
- Assists in eliminating fascial densifications and adhesions, and restoring tissue gliding
- Increases deep tissue perfusion and oxygenation, boosting injected cell survival.
- Enhances metabolic activity and waste clearance, optimizing the healing environment.
- Enhances cell membrane permeability, improving migration, adhesion, and integration of injected PRP/stem cells.
- Stimulates ion channel activity (Ca²⁺, Na⁺, K⁺), supporting regenerative signaling.
- Promotes angiogenesis and microcirculation, improving survival of transplanted cells.
- Reduces oxidative stress and inflammation, creating a favorable niche for stem cell activity.
- Provides analgesia and reduction of muscle spasm, facilitating early functional rehab after injections.
- Improves viscoelasticity of tissues, allowing better integration of regenerative cells.
When delivered at the most effective levels under ultrasound guidance, ESWT + EMTT prime the microenvironment via mechanical and electromagnetic stimulation. TECAR + Laser therapy optimizes tissue metabolism, circulation, and cellular energy. Together, they extend and amplify the biological effects of PRP and stem cells, accelerating tissue integration, repair, and functional recovery.
When used post-procedure, energy therapies dramatically reduce pain and discomfort, reinforce soft tissue healing, and promote collagen fiber realignment.
Physical Therapy is Fundamental to Rehab Success
Some clinics may try to convince you that orthobiologics and energy technologies can replace physical therapy to resolve musculoskeletal pain and dysfunction, but nothing could be further from the truth. While regenerative therapies promote tissue healing, they do not address key factors involving neuromuscular pathways, compensation patterns, fascial restrictions, muscle imbalances and strength deficits.
To be effective, physical therapy must be personalized and targeted. Yet most physical therapists rely on generalized cookie-cutter treatment protocols that fall short of their goals, leaving patients with only moderate improvements in mobility and pain reduction. Other clinics routinely delay physical therapy until after a completed injection cycle, when certain cases call for physical prehab prior to injections.
At NYDNRehab, we sometimes precede injection therapy with targeted physical therapy to improve motor patterns and release dysfunctional tissues like densified fascia. In such cases we delay injecting the biologic solution until it is most likely to produce maximal benefits, not only for the damaged tissue but for the entire system. In other cases, we do injection therapy after prior attempts at physical therapy have failed, or to heal and fortify damaged tissues before loading them.
Many physical therapists do not know how or when to successfully progress patients from one treatment modality to the next, relying on standardized protocols that produce mediocre results. At NYDNRehab, we know exactly what therapy to use, for which tissues and conditions, and when to introduce physical therapy to get the best results for our patients.

NYDNRehab Sets a High Bar for Injection Therapies
When new medical technologies and therapies emerge, there is a high incentive for businesses to quickly adopt and market them. However, many clinicians do not possess the skillset or experience to use them appropriately or effectively, leaving patients with disappointing outcomes that fall short of the hype. Such is often the case with orthobiologics.
Orthobiologics are only maximally effective if:
- They align with the patient’s pathology
- They are injected with precision under ultrasound guidance
- The solutions are of high quality and the right concentration
- The clinician uses proper techniques
- Injections are supported by energy technologies
- Results are optimized with physical rehab
At NYDNRehab, our customized treatment protocols strategically combine the most advanced therapies and technologies, transforming the way musculoskeletal conditions are diagnosed, assessed and treated. We are one of the few private clinics in the USA to provide high-resolution ultrasonography, biologic injections, energy technologies, and targeted rehab under one roof.
Our holistic and multifaceted approach is backed by years of training and experience. Our customized patient-first philosophy, combined with Dr. Kalika’s expertise and successful track record, set a high bar for the appropriate use of orthobiologics, and regenerative technologies. We never promote a therapy or product unless we firmly believe it will benefit the patient in ways that accelerate healing and restore functional mobility.
If you’re ready to radically improve your mobility with the most advanced therapies in NYC, contact NYDNRehab today.
Ultrasound Guided Injection Therapies
Regenerative Injection FAQs
Orthobiologic solutions use substances derived from the patient’s own body, such as blood plasma, bone marrow or adipose tissue, The solutions are highly concentrated, and injected into damaged tissues to reduce pain and inflammation, and stimulate a regenerative healing response. Orthobiologic injections are evidence-based and considered safe for most patients when proper procedures are followed. Beware of birth-tissue “stem cell” products that don’t contain viable stem cells and are not FDA-approved for musculoskeletal use.
The number of injections should be based on your unique condition. Steer clear of clinics that sell injection “packages.” For tendon and ligament treatment, you may need up to 2-3 injections, spaced 4-8 weeks apart. For joint osteoarthritis that responds well to the initial treatment, you may need 1-3 boosters per year.
In the first 1-4 weeks after treatment, your symptoms may temporarily worsen due to inflammation, but you should see noticeable improvement by 6-12 weeks, with peak benefits realized within 3-6 months.
For tendon conditions like tennis elbow or Achilles tendinopathy, results may last for 1-5 years, and they may be permanent if the injury is properly rehabilitated. For mild to moderate osteoarthritis, results typically last for 1-3 years, although some last for up to 5 years. For partial ligament tears, results are often permanent after sufficient physical rehab.
Look for a clinic that does everything in-house, including high resolution ultrasonography for diagnosis and injection guidance. Transparency is key, not only in pricing, but in documenting the quality and concentration of biologic solutions. Steer clear of clinics that sell packages of multiple injections, use birth tissue derivatives instead of patient-derived substances, or promote orthobiologics as a replacement for physical rehab.