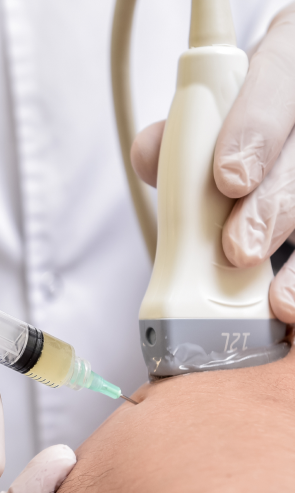
About Herniated Discs
Intervertebral discs serve as spacers and shock absorbers between the vertebrae of your spine. They prevent bones from rubbing together and provide a space for nerve roots to exit the spinal canal and travel to structures throughout your body.
The discs are made up of a tough rubbery exterior called the annulus, and a soft center called the nucleus. The annulus is composed of fibrous layers of collagen and proteins, while the gel-like nucleus is made up of mostly water and collagen. The discs give your spine its mechanical flexibility and shock-absorbing properties.
A disc can become ruptured, or herniated, when a portion of the nucleus bulges through a crack in the annulus. Most herniated discs occur in the lower back, but they can also arise in the neck. A herniated disc can be asymptomatic if it does not affect a nerve. But when a bulging disc compresses a nerve root where it exits the spinal column, it can cause severe pain and restricted mobility.
Herniated discs are common among adults. In fact, Most people after age 40 have some degree of bulged and herniated discs, and foraminal compressions to the spinal nerve roots. The majority of them are asymptomatic, producing no pain at all, and where pain is present, herniated discs are often not the sole generators of pain.
Pain is often caused by a combination of soft tissue lesions, pelvic /hip misalignment, ligamentous and fascial deterioration, muscular trigger points, and cutaneous nerves entrapment within the toraco-lumbar fascia. Unfortunately, MRI does not show those details, and doctors often focus on disc lesions, unaware of other factors that contribute to disc herniation.

Orthobiologic, Sports Medicine and Regenerative Medicine Specialist
The conventional approach to herniated disc diagnosis is often symptoms-based, with little consideration of structures located beyond the locus of pain. Yet there are numerous other causes of back and neck pain that produce similar symptoms, and a complete and accurate diagnosis relies on more than symptoms alone.
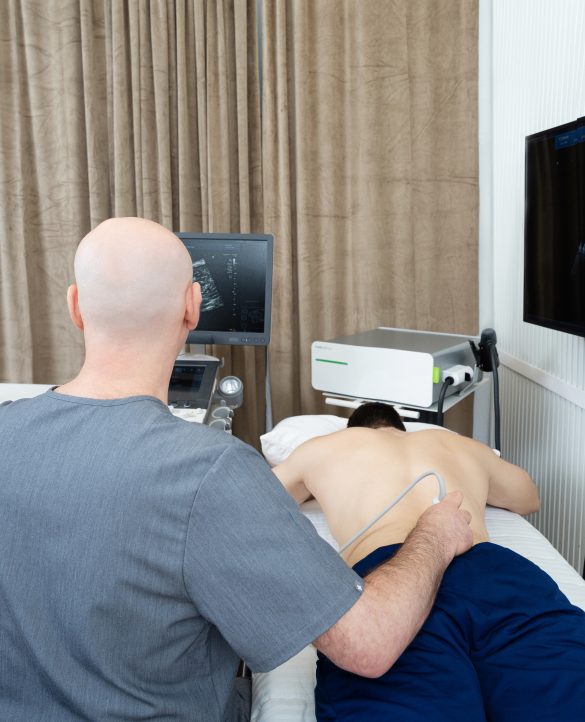
At NYDNRehab, we use the highest resolution diagnostic ultrasonography to view dynamic images of your spine, discs and surrounding structures in real time, to uncover every potential cause of pain. Your ultrasound exam takes place on your first visit, in the comfort of our Manhattan clinic. On-site imaging means a speedy diagnosis, with no waiting for lab results.
Once we have a clear picture of what’s going on, we design a personalized treatment plan based on your unique diagnostic profile. We never take a one-size-fits-all approach to patient care – we treat the whole patient, not just your symptoms. Our advanced technologies enable us to objectively measure your progress every step of the way, to ensure your therapy is effective. Our holistic and personalized approach to diagnosis and treatment sets NYDNRehab apart as the clinic of choice for herniated disc treatment in NYC.
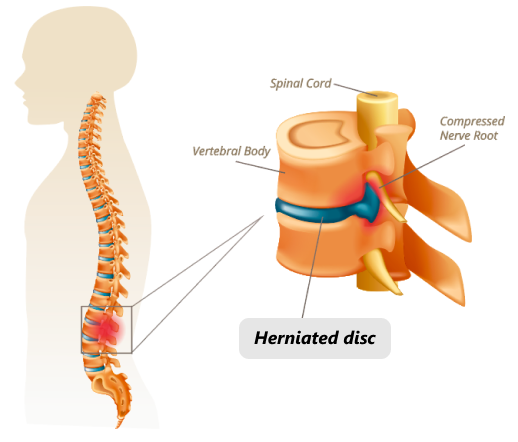
Herniated discs are common among adults. In fact, Most people after age 40 have some degree of bulged and herniated discs, and foraminal compressions to the spinal nerve roots. The majority of them are asymptomatic, producing no pain at all, and where pain is present, herniated discs are often not the sole generators of pain.
Pain is often caused by a combination of soft tissue lesions, pelvic /hip misalignment, ligamentous and fascial deterioration, muscular trigger points, and cutaneous nerves entrapment within the toraco-lumbar fascia. Unfortunately, MRI does not show those details, and doctors often focus on disc lesions, unaware of other factors that contribute to disc herniation.
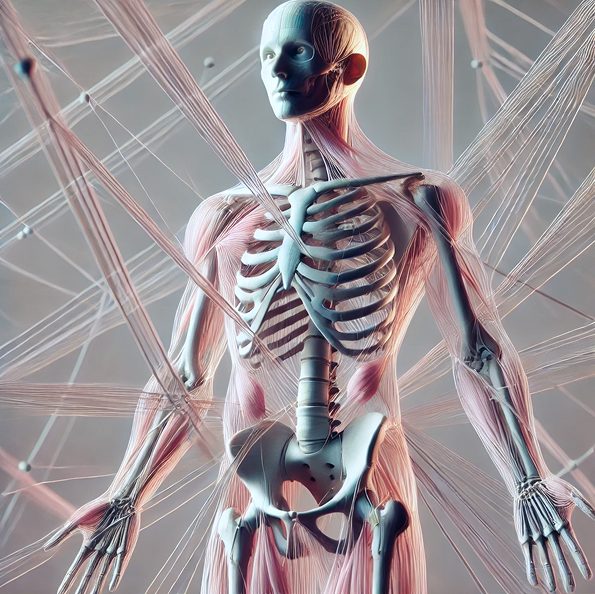
Fascia is a complex network of connective tissues that surrounds and connects structures, tissues and organs throughout the body. Fascia works together with muscles to guide and control movement, and mediate outside forces. Together, muscles and fascia – aka the myofascial system – creates tensegrity that plays a key role in mobility and stability, and a significant role in herniated disc pain.
Fascia is rich with nerve endings, and capable of transmitting tension and pain signals to the brain. Fascia in the lumbar region is intimately connected to the spinal muscles and nerves. Inflammation can spread from the disc to the fascial layers, causing them to stiffen, and triggering fascial pain receptors to generate pain signals beyond the disc itself.
Fascia is highly adaptive to chronic tension or injury, which can lead to fascial adhesions or thickening. Nerves can become entrapped by densified fascia, preventing them from gliding, and densification can interfere with muscle action, restricting mobility and causing pain. Densified fascia loses its elastic properties, and can pull on adjacent structures, creating a feedback loop of widespread pain and tension that doesn’t necessarily align with the disc’s location.
Therapies like myofascial release and dry needling can help to ease fascial tension and relieve pressure on entrapped nerves, interrupting the cycle of herniated disc pain.
Back and neck pain does not always indicate a herniated disc, and a diagnosis based on symptoms alone can result in ineffective treatment that prolongs your pain. In many cases, back pain is non-specific in nature, with no mechanical cause detected on MRI. MRI imaging of herniated discs gives us only partial information – diagnostic ultrasonography completes the picture, helping us to define all pain generators involved.
The clinic at NYDNRehab features the most advanced high resolution ultrasonography currently available. Diagnostic ultrasound lets us examine all the structures affecting the spine in real time. Ultrasound imaging lets us view long bodies like bones, nerves and fascia along their entire path, to pinpoint the true source of pain. In many cases, pain arises from nerves entrapped by fascial adhesions, or from other factors such as muscle strains and trigger points.
Diagnostic ultrasound ensures that you get an accurate diagnosis on your first visit, without having to leave the clinic or wait for lab results, so your treatment can begin right away.

Once we identify a disc herniation as the primary cause of pain, we create a personalized treatment plan based on your unique results. Prior to beginning physical therapy, we pretreat your disc to reduce pain and inflammation.
Pre-treatment may include:
Depending on the underlying cause of your pain, your treatment plan may include:


Focused ESWT technology produces high frequency sound waves to reduce pain and inflammation and stimulate the body’s own reparative mechanisms.
Our new PiezoWave shockwave machine features MyACT, a new type of focused shockwave technology that allows for deeper compression of the focused waves. Its higher frequency allows for precise neuro modulation under ultrasound guidance, with a special linear head for treating myofascial pain.
This innovative shockwave technology transforms the mechanical energy of shockwaves into biochemical signals that precisely target damaged tissues. Its versatile system of controls lets us fine-tune its output levels for precise and personalized patient care. With MyACT, we are able to repair and regenerate damaged tissues by stimulating the body’s own reparative mechanisms.

EPAT, also called radial shock wave therapy, is not a true shockwave, but uses mechanical pressure waves that are much weaker than focused shockwaves. EPAT is most useful in regenerating fascia fibroblasts and eliminating fascia densifications.
EMTT transmits high energy magnetic pulses that synchronize with your body’s own magnetic fields, triggering a regenerative response in tendons, muscles, bones and nerves.


INDIBA therapy helps to restore the ionic charge of damaged cells, for faster injury healing.
The NESA device generates a biphasic low-frequency electrical current that travels through autonomic neural pathways, to restore optimal neural signaling to the brain.


High Energy Inductive Therapy (HEIT) is a new technology that uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT relieves pain by restoring peripheral nerve function.
Laser therapy is a non-invasive approach to treating chronic pain that reduces inflammation, eliminates pain and speeds up tissue healing. The treatment uses light energy to penetrate your skin, muscle, nerve, and connective tissues, stimulating a photochemical reaction that changes the chemical and physical properties of the affected area at the molecular level

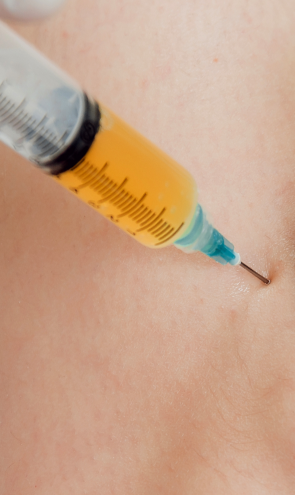
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.