FAI is a fairly common athletic hip injury that occurs in sports like football or rugby that involve cutting, pivoting and rapid directional changes. Your hip is a ball-and-socket joint, where the head of the femur (thigh bone) rotates within the acetabulum capsule. The capsule is lined with a fibrocartilaginous band called the labrum, and is lubricated by synovial fluid to allow the femur head to glide smoothly.
The labrum can become damaged or torn when the femur head pinches up against the acetabulum, causing the hip to become stiff and painful, and limiting range of motion. If left untreated, FAI can lead to hip arthritis and long-term disability.
or
Approach is based on technological 3D analysis, high resolution ultrasonography, cutting-edge physical therapy, neuromodulation, ultrasound guided dry needling, and regenerative technologies and injection therapies.
Dr. Kalika also specializes in treating post-surgical arthroscopic FAI and labral repairs, in cases where surgery was unsuccessful in alleviating pain and restoring hip function.
Not all physical therapy clinics are equipped to help athletes and physically active people to fully rehabilitate injuries. They may help you to restore basic function, but they are often unable to fully prepare you to return to sport.
The clinic at NYDNRehab features some of the most advanced technologies for sports physical therapy and FAI rehab. Our high-tech diagnostic tools, regenerative therapies, AI-empowered feedback equipment and computer-assisted analysis technologies are rarely found in average physical therapy clinics.
Our personalized one-on-one treatment programs are designed specifically for the individual, based on the patient’s diagnostic profile. We never rely on generic timelines or one-size-fits all protocols. Our high-tech tools let us quantify and measure your progress, with the end goal of getting you back to play safely, both physically and mentally.
Stiffness in the upper thigh
Pain and stiffness in the hip and/or groin
Reduced hip range of motion
Hip pain after prolonged sitting
Pain ranging from dull to sharp when squatting
Clicking or locking of the hip joint
Formation of a bony growth on the head of the femur (Cam FAI)
Formation of a bony growth in the hip socket (usually in early childhood)
High intensity physical activity with cutting and pivoting
Repetitive overuse
Trauma from a fall or accident
Age-related wear and tear
FAI is often diagnosed based on symptoms and a physical exam, along with Xray or MRI. At NYDNRehab, we use the highest resolution diagnostic ultrasound imaging to examine the hip in real time, with the patient in motion and providing feedback. Ultrasound allows us to see the extent of damage, as well as the limitations it imposes on movement.
We also use computer assisted 3D motion analysis, along with other assessment tools, to measure and quantify the quality of hip movement pre-treatment, and periodically throughout the treatment process, to confirm and measure progress.
With a thorough and accurate diagnosis in hand, we are able to design a personalized treatment plan, geared to the specific needs of the patient.
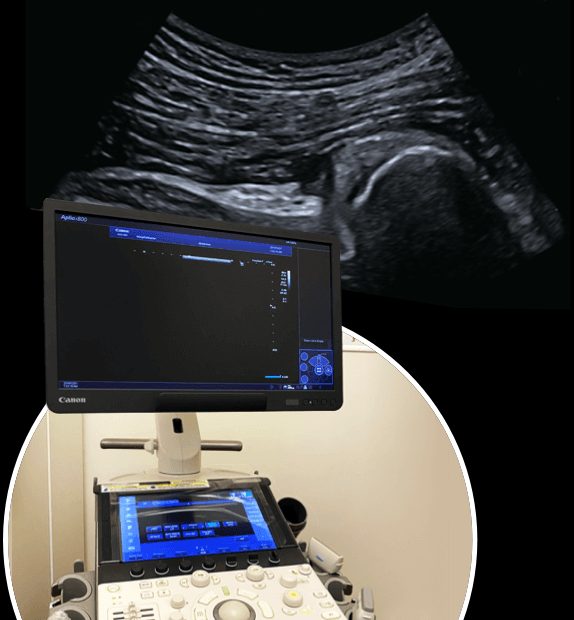

The clinic at NYDNRehab features advanced technologies rarely found in private physical therapy clinics. Combined with our experience and expertise, our high-tech diagnostic and treatment tools ensure fast and effective recovery.
Your personalized femoroacetabular impingement treatment plan may include:
Your body has its own innate healing mechanisms, but they sometimes need a nudge to stimulate the healing process. Regenerative technologies help to jump-start healing at the cellular level, for fast and effective recovery with minimal discomfort for the patient.
Focused ESWT technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for treating fibrocartilaginous structures like the hip labrum.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissue, to stimulate cellular metabolism and accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes.

The NESA device generates an algorithm that delivers a biphasic low-frequency electrical current via semi-electrodes attached to the hands and feet. It emits a series of intermittent and cyclical stimuli that travel through autonomic neural pathways, restoring optimal neural signaling to the brain.
INDIBA converts electrical current into a stable frequency of 448 kHz, designed to increase the exchange of ions in damaged cells. The current evokes a regenerative response that accelerates healing.

Injection therapies like platelet rich plasma (PRP) and prolotherapy use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
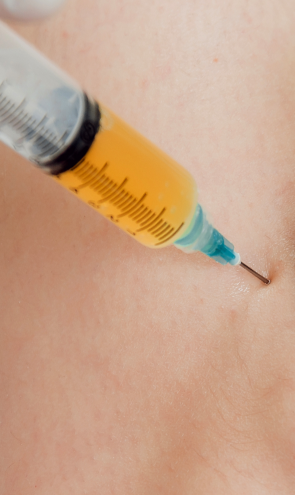
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.
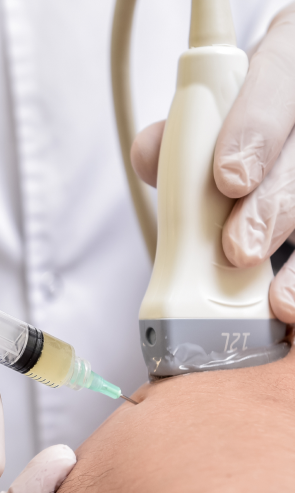
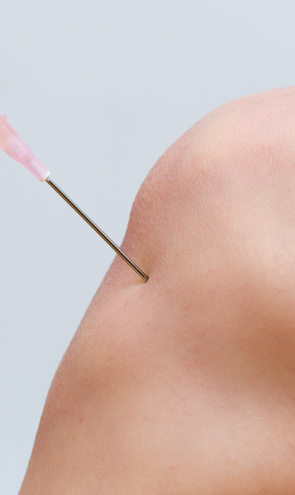
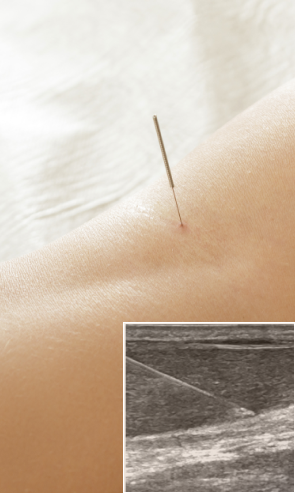
Dry needling targets myofascial trigger points that may contribute to FAI pain and stiffness. Ultrasound guidance ensures accuracy, to minimize pain and discomfort for the patient.
When it comes to staying physically active, run-of-the-mill physical therapy won’t do. You need a clinic that specializes in sports injury rehabilitation that gets you back to play as quickly as possible. Many people make the mistake of trying to “play through the pain,” only to end up with debilitating injuries that may never fully heal.
If you have hip and groin pain that limits your ability to do the things you love, you may need FAI physical therapy. Contact NYDNRehab today, and let our sports medicine specialists work their magic, so you can get back into the game of life.

November 19, 2025
This is a list of anators:
Other predisposing facto distant trauma resulting in alteration of biomechanical relationship in the kinetic chain.
The progression of this disease is interesting occurrence. One may ask himself that if all anatoms in the second decade)?
The answer is simple. In FAI congenital bone anomalies are varied in combination of it’s severity and overplay with joint and movement dysfunction in other regions of the body. Majority of people with these congenital anato the hip with congenital imperfections.
Many people with FAI suffer from back pain and herniated disc disease for years prior toms of hip pain. Majority of these patients are operated for disc hernia without successful outcomes or only with temporary pain relieve.
The golden standard of radiological diagnosis for FAI is special CT scan series. This is, however only necessary in case surgical intervention is entertained as there is enormous dose of radiation involved in this special procedure.
Otherwise, a combination of X- ray with MRI or diagnostic ultrasound and clinical examination can be specific enough for treatment.
FAI pain treatment depends on precise structural and functional diagnosis as well as consideration of compensator control and the biomechanics of the whole human body.
Femoraceabular (FAI) pain treatment also depends on careful elimination of provoking movement and postures.
Video gait analysis is the best technological modality to human eye and therefore biomechanical relationship of all the components of lower kinetic chain cannot be properly addressed without it.
Please explore our gait analysis page.
Even with all the complexity of the FAI pain syndrome, conservative care is successful in experienced hands within 6-8 weeks in initial presentation and up to 6 month of rehab in chronic cases.
Surgical intervention should only be reserved to professional athletes or very few patients with greater damage of hip intrarticular tissues.
The surgical intervention does not correct the cause of impaired movement but only remove the bone conflicting anatomy.
Since data for arthroscopic FAI repairs is relatively new , we can not estimate yet how successful these surgeries are. Especially giving very , very long recovery from this surgery this type of procedure should only be reserved as a last reserve.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: