GTPS is a painful condition affecting tissues surrounding the greater trochanter of the femur (the “ball” in the hip ball-and-socket). Once called “trochanteric bursitis,” the name was modified after multiple studies revealed that the greater trochanteric bursa — the fluid-filled sac that separates the trochanter from surrounding soft tissues — was not involved in 85% of patients suffering from the condition.
GTPS is marked by pain and tenderness around the lateral hip, but does not affect the bursa, or the hip joint itself. Once believed to be caused by inflamed bursae, GTPS is now believed to be a degenerative overuse condition. Running and jumping activities are thought to contribute to GTPS.
or
Dr. Kalika has developed his own unique approach to treating hip labrum tears, helping patients to avoid surgical repairs. His expertise in hip preservation therapy is sought by elite athletes, runners and professional dancers across the USA.
Dr. Kalika’s work has preceded multiple research studies that prove that most hip labrum tears and femoroacetabular impingement (FAI) can be successfully treated with conservative care. His approach is based on technological 3D analysis, high resolution ultrasonography, cutting-edge physical therapy, neuromodulation, ultrasound guided dry needling, and regenerative technologies and injection therapies.
Dr. Kalika also specializes in treating post-surgical arthroscopic FAI and labral repairs, where surgery was unsuccessful in alleviating pain and restoring hip function.
Pain on the outer hip, thigh and/or buttock
Pain when pressure is applied to the outer hip
Pain that worsens when rising from sitting to standing
Pain when climbing stairs
Overuse from sports, exercise or occupation
Poor posture and excessive sitting
Previous hip surgery
Calcium deposits or bone spurs
Hip mobility is fundamental to everyday movement, and hip pain can really slow you down. As a ball-and-socket joint, the hip has a broad range of motion, governed by multiple structures, including muscles, tendons, ligaments and nerves. Because of the complexity of hip and greater trochanter anatomy, it can be difficult to pinpoint the exact cause of hip pain. This often leads to misdiagnosis, excessive use of pain pills and unnecessary surgeries.
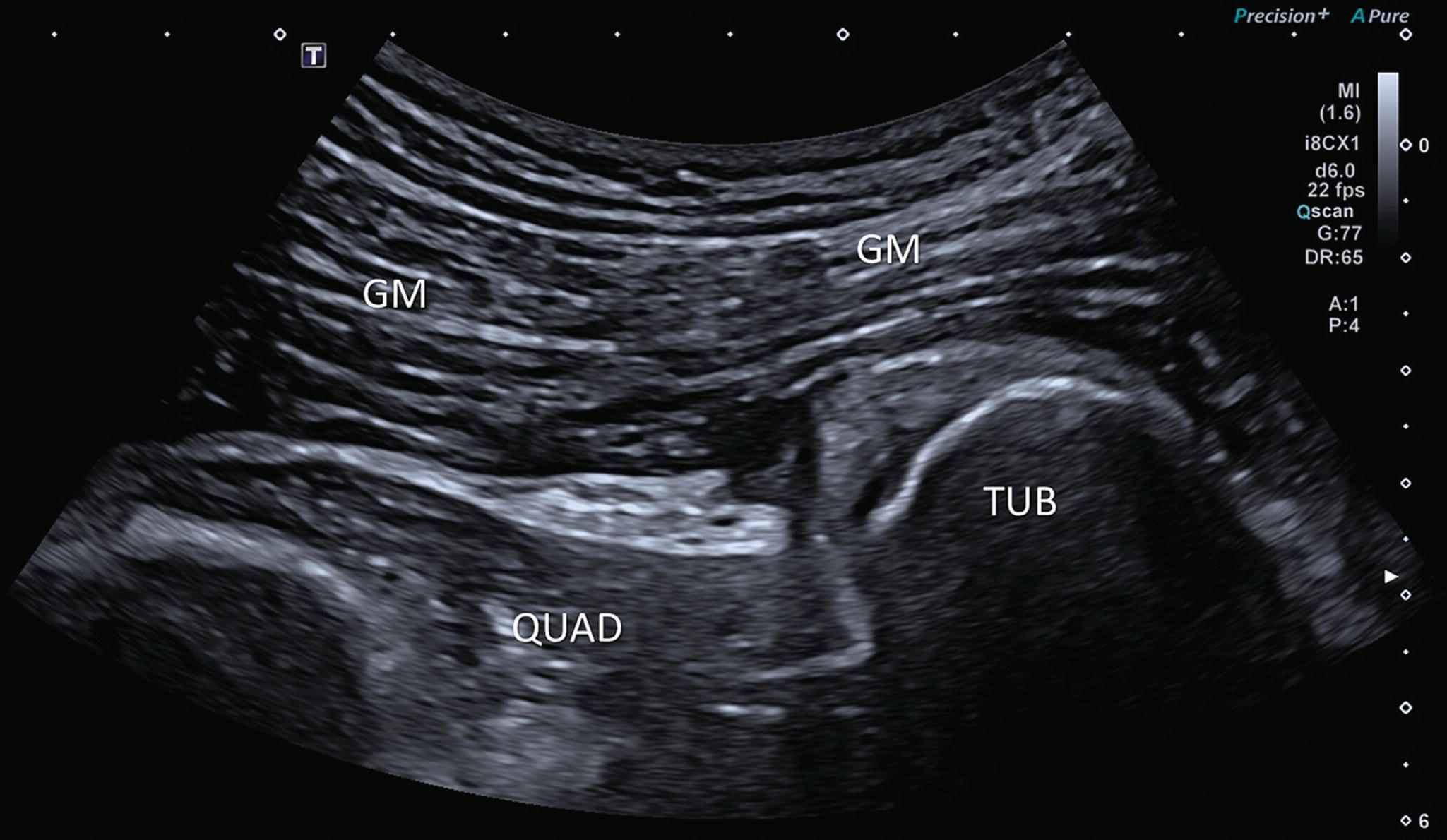
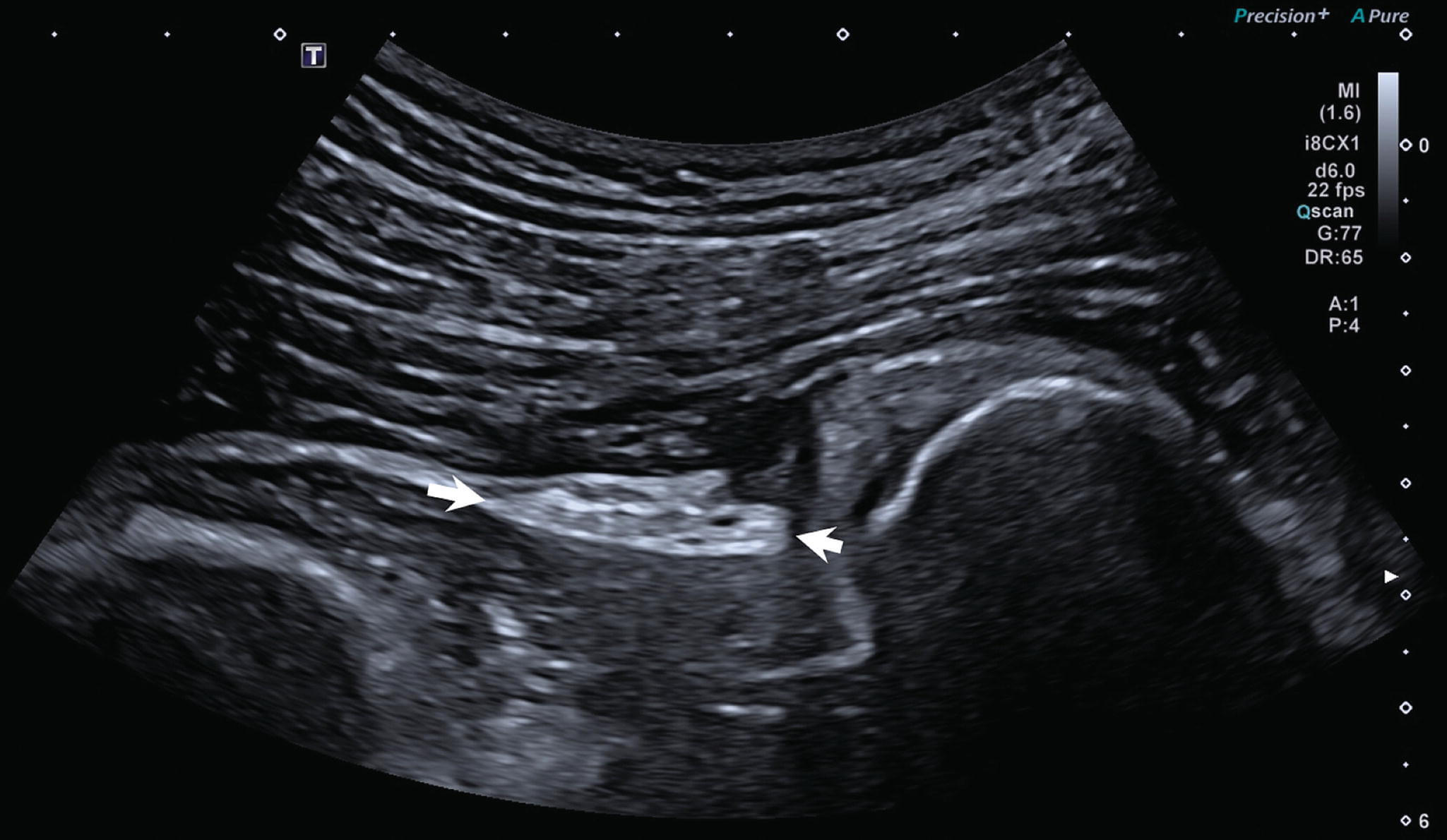
At NYDNRehab, we use high-resolution diagnostic ultrasound to visualize the structures surrounding the hip in motion, in real time, to accurately pinpoint the underlying cause of hip pain. We then create a personalized treatment protocol, based on your unique diagnostic results.
Unlike run-of-the-mill physical therapy clinics that take a one-size-fits-all approach to patient care, and divide their attention among multiple patients at once, our one-on-one therapy sessions ensure that your therapist is focused on getting you the best results, saving you time and money. Our high-tech regenerative tools help to speed up the healing process, so you can get back to normal activity in the least possible amount of time.

Any of the complex structures that make up hip and greater trochanter anatomy can contribute to GTPS, and misdiagnosis is common. When diagnosis is based on symptoms alone, serious issues can be overlooked, and the wrong treatment protocol can prolong your pain and suffering while draining your resources.
At NYDNRehab, we use the most advanced high-resolution ultrasound equipment to visualize the structures of the hip in motion. Our high-tech 3D gait analysis lab is able to detect and quantify gait deficiencies that may contribute to your pain and disability.
Dr. Kalika is an expert in diagnostic ultrasonography, and has published multiple scientific papers on the topic. His experience and expertise ensure that your hip condition is accurately diagnosed and appropriately treated.
Please explore more advanced diagnostic option unavailable anywhere else:
Prior to beginning physical therapy, we make sure your hip joint is both stable and mobile, so you get the most from your therapy sessions. Our regenerative therapies reduce pain and inflammation, and jump-start the healing process by stimulating your body’s own healing mechanisms.
Focused ESWT produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields to trigger a regenerative response.

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes.
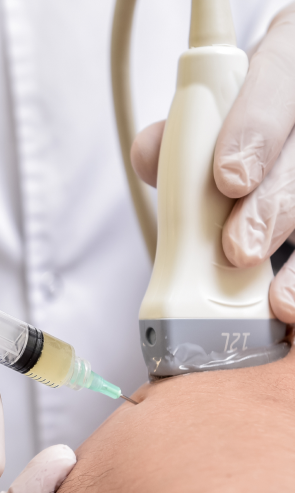
Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution that irritates the affected tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new cells.
Staying physically active is key to maintaining good health, avoiding metabolic disease and remaining pain-free from musculoskeletal issues. Your body is designed to move and perform physical work. Sitting all day in front of a screen is the fastest route to poor health and reduced mobility.
At the same time, relentless exercise without adequate recovery time, combined with suboptimal movement mechanics, can lead to repetitive use injuries, and set you up for acute injuries.
Take the following actions to avoid greater trochanter injury, hip bursitis pain, and other pain syndromes:
Anyone can benefit from a 3D gait analysis, or a total body biomechanical analysis, to identify motor deficits that could cause pain and injury down the road. Catching them early and correcting them can help you stay active and pain-free for years to come.

November 19, 2025
Greater trochanteric pain syndrome (GTPS) is a condition that was formerly known as trochanteric bursitis. Bursa are fluid-filled sacs located in your joints that prevent friction between your bones and soft tissues as you move. In your hip, a bursa is positionedocks.
In the past it was thought that the bursa itself becomes irritated and inflamed, causing hip pain and discomfort. However, recent research has revealed that hip pain at the trochanter is not cause by an inflamed bursa, but rather by inflammation of the tendons that attach muscles to the hip joint.
GTPS is marked by pain and tenderness at the side of the hip that becomes worse while standing, and during physical activities like walking, running and jumping.
Degenerative repetitive overuse is the primary cause of GTPS. The syndrome is most commonly seen in middle aged runners, middle aged females, and patients suffering from low back pain.
Other causes include:
A health histo diagnose GTPS. However, real-time diagnostic ultrasound can be useful in confirming diagnosis, and in determining the severity of GTPS.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: