
Dizziness, clinically called vertigo, is a feeling of being off-balance as the world around you seems to spin. When your jaw is poorly aligned and inflamed, it can put pressure on your inner ear, disrupting the organs that help you balance.
Your inner ear’s vestibular system is located in your temporal bone, where your jawbone attaches to your skull. Pressure from a poorly aligned jaw can throw your vestibular system off, confounding the signals sent to your brain about your body’s position in space and leading to feelings of vertigo.
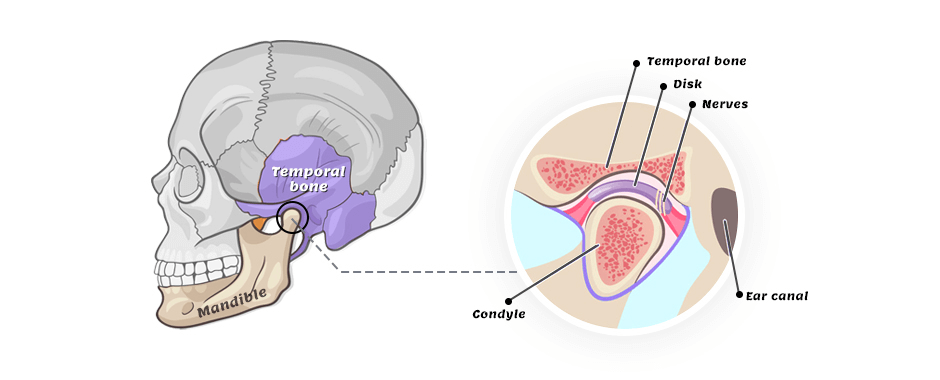
Your temporomandibular joint (TMJ) is located directly beneath your eustachian tube, or ear canal, and connects your jawbone to your skull. It is a sliding hinge joint that allows you to talk and chew. Because of its proximity to the ear canal, pain that originates in the TMJ is often mistaken for ear pain.
Problems with the TMJ have been linked to several seemingly unrelated conditions, including:

TMJ syndrome may arise due to postural issues in the upper body that cause the joint to misalign. Texting and computer use may be primary contributors. The condition may also be caused by stress that makes you grind or clench your teeth at night.
TMJ syndrome is often associated with pain and dizziness due to a heightened vestibular response to jaw inflammation. A Korean study (Chung et al. 2012) was conducted on rats whose jaws were injected with an inflammatory agent. The experimental group subsequently displayed heightened vestibular nuclei activity, compared to controls that were injected with a neutral substance.
Another study (de Toledo et al. 2017) found that 40.8 percent of TMJ patients experienced vertigo associated with the syndrome, and 55.1% experienced otalgia (ear pain). While vestibular issues are not always caused by TMJ syndrome, it should not be ruled out as a potential cause of chronic dizziness.
Dizziness associated with TMJ syndrome can be effectively treated with chiropractic care and physical therapy. The first step is accurate diagnosis, to ensure that other issues are not affecting the vestibular system.
Conventional medical treatments for TMJ syndrome include bite devices, Botox injections, orthodontic care and surgery. However, there is little scientific evidence that any of those approaches are effective, and most are costly.
Effective conservative treatment options for TMJ syndrome include:
Once the TMJ is restored to proper function, dizziness symptoms should subside. If you still experience vertigo, your dizziness may have another underlying cause.
If you are experiencing ear and jaw pain with dizziness, you may have TMJ syndrome. The clinical director at NYDNRehab, Dr. Kalika, is a world-renowned chiropractor with extensive experience treating TMJ patients. Chiropractic care combined with physical therapy can resolve the root causes of TMJ syndrome and eliminate headaches and dizziness.
Our state-of-the-art clinic features:
NYDNRehab now offers TeleHealth services to patients who prefer remote treatment. Contact us today, and let our team of TMJ experts resolve your pain and discomfort, so you can get back to your active pain-free life.
Resources
Chung, Sung-Won, et al. “Inflammation of temporomandibular joint increases neural activity in rat vestibular nucleus.” Neuroscience Letters 528.2 (2012): 126-130.
De Toledo, Isabela Porto, et al. “Prevalence of otologic signs and symptoms in adult patients with temporomandibular disorders: a systematic review and meta-analysis.” Clinical oral investigations 21.2 (2017): 597-605.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: