
Meniscus tears in the knee are common sports injuries that cause pain and instability. A torn meniscus most often occurs in court sports like basketball, tennis and volleyball, where the knee is torqued while bearing your body weight, or from impact upon landing from a jump. They also occur in field sports that require jumping, sprinting and rapid directional changes, like soccer and football.
While less common in non-athletic populations, traumatic meniscus tears can occur from a fall or a misstep on uneven surfaces. Risk factors for torn menisci among non-athletes include obesity and age-related wear and tear on the knee joints. Older adults sometimes tear a meniscus during simple everyday movements, like getting up from a chair.
Meniscus tear treatment often involves either a partial or total meniscectomy, a surgical procedure where damaged meniscal tissue is removed from the knee capsule. Although meniscectomy is considered standard procedure among some clinicians, there is little empirical evidence to support its widespread use.
The menisci are C-shaped pads of rubbery cartilage in your knees that absorb shock and stabilize your joints, enabling them to glide smoothly without the bones making contact, and helping to evenly distribute force loads during physical activity. Each knee has two menisci. The medial meniscus cartilage is located on the inner side of your knee joint. It attaches to the medial collateral ligament (MCL), making it more vulnerable to injury. The lateral meniscus is set at the outer side of the knee and is larger and thicker than the medial meniscus. It does not attach to a ligament.
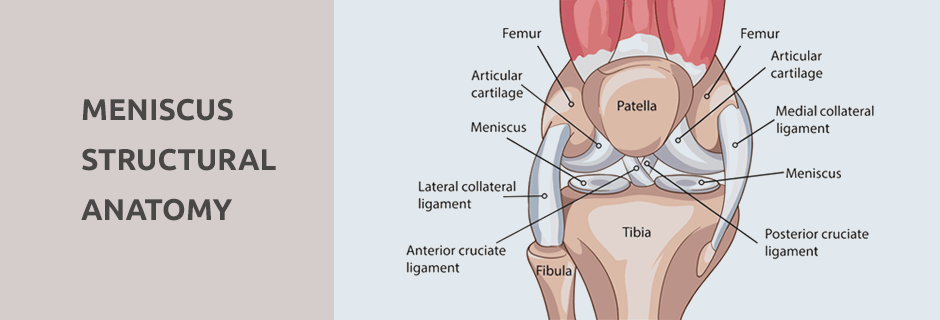
Because the medial meniscus absorbs 50 percent or more of shock to the medial compartment, medial meniscus tears can be debilitating. Failure to rehabilitate a medial meniscus tear can lead to reduced stability and knee osteoarthritis. Lateral meniscus injury often occurs while pivoting on a loaded knee, or from direct impact to the outer knee. Rehabilitation is key to functional recovery.
There are six basic categories of meniscus tears:
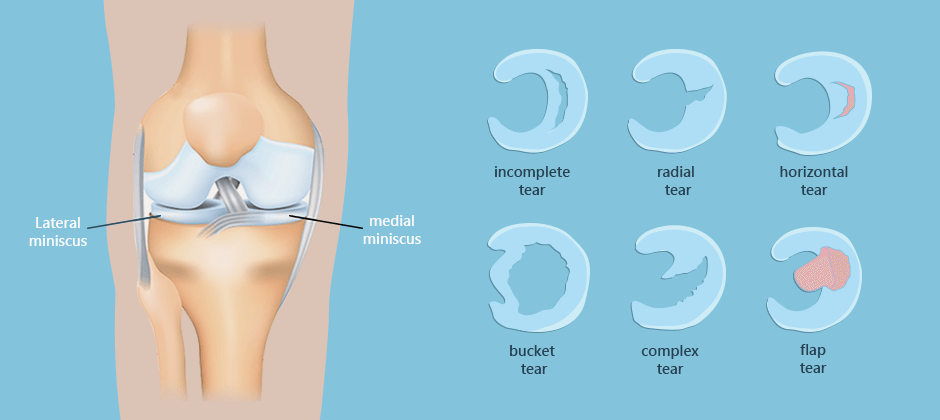
The severity and degree of meniscus tears can vary. If the tear occurs closer to the periphery, there is a greater chance of healing via the formation of fibrocartilage scar tissue. More central tears have a much lower capacity to heal. Torn meniscus symptoms include pain, inflammation, joint stiffness, and difficulty extending the joint.
Imaging technology plays a key role in accurately diagnosing damage to an injured meniscus. Until recently, MRI was the imaging method of choice for meniscus tears, but advances in technology have dramatically intensified the resolution of diagnostic musculoskeletal ultrasound (MSUS), making it a better choice in many instances over MRI.
There are six basic categories of meniscus tears:
In a 2018 paper, Kopf et al. discussed the findings of the ESSKA European consensus on traumatic meniscus tears. Scientists convened with knee experts and surgeons to uncover scientific evidence that would provide guidelines for managing and treating meniscus tears. Surgery that removes part or all of the meniscus is frequently recommended for meniscus tears, but after conducting a detailed study, the group arrived at the consensus that every effort should be made to preserve the meniscus whenever possible. The group based their conclusion on evidence that preservation yields better outcomes for meniscus patients in the long run. They further agreed that there were certain rare and infrequent scenarios where surgery is recommended, including older tears, long tears, tears in the knees of obese patients, and when root lesions are present.
The knee is a complex joint where multiple structures converge, and knee injuries can be complicated and difficult to accurately diagnose. Dr. Lev Kalika is an expert in the field of musculoskeletal diagnostic ultrasonography, with 12 years of hands-on experience.
Our clinic features a research-grade ultrasound machine with the highest resolution available in NYC, with capabilities for sonoelastography and superior microvascular imaging (SMI). At NYDNRehab, we use MSUS and other advanced technologies to diagnose, quantify and treat knee injuries, with the goal of restoring pain-free function.
Resources:
Kopf, Sebastian, et al. “Management of traumatic meniscus tears: the 2019 ESSKA meniscus consensus.” Knee Surgery, Sports Traumatology, Arthroscopy (2020): 1-18. Mahdy, Nada Sayed, Hossam Mousa Sakr, and Allam Elsayed Allam. “The Role of Ultrasound in Evaluation of Meniscal Injury.” The Egyptian Journal of Hospital Medicine 72.10 (2018): 5490-5494.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: