August 14, 2023
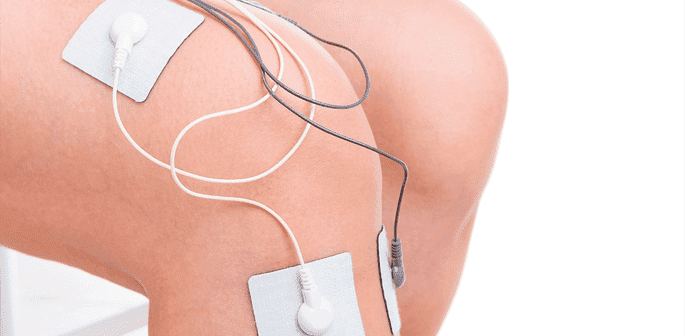
In the center of each of your knees, there’s an anterior cruciate ligament (ACL). These ligaments are positioned diagonally. ACL injuries are fairly common, especially for athletes. To repair the damage, surgeons will sometimes graft tissues onto an ACL. That operation is an ACL reconstruction.
After such a reconstruction, it’s easy for the muscles around the knee, including the hamstrings and the quadriceps, to aid their patients.
In 2012, the medical journal “Clinical Rehabilitation” published the results of a study that examined the effects of electro-stimulation on ACL reconstruction patients. This survey was set up as follows:
The results of this study were clear. The people who were administered electro-stimulation saw their swelling go down considerably after the first week. They experienced less pain as well. These three benefits were also noteworthy:
Granted, this research project was merely a pilot study. Among its deficiencies, it didn’t have a large group of subjects, and it didn’t involve a placebo. Nevertheless, it represents a starting point for scientific inquiry into electro-stimulation and ACL reconstruction recovery, and its conclusions are promising.
At this time, it’s almost certain that people who go through ACL reconstruction lose less muscle mass with electro-stimulation treatments than they would if they relied on exercise alone. Now, that’s not toning muscles and maintaining cardiovascular health. It’s just that, with the help of electro-stimulation, a patient will likely end up dealing with less pain, swelling, and atrophy.
With all of this information in mind, if you’re a docto their electro-stimulation sessions, which can be really soothing. Indeed, they can ease some of the anxiety that often accompanies injuries.
Then, once your patients realize how much faster they are recuperating, they’re sure to you and the electro-stimulation technology that you’ve adopted.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: