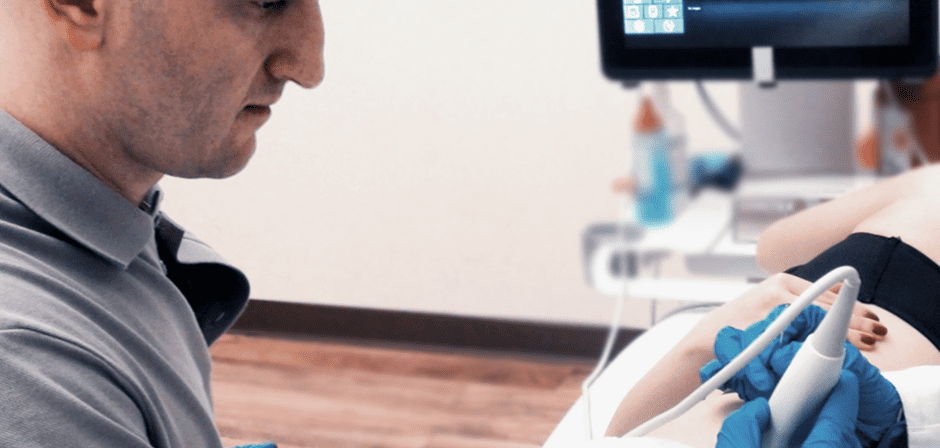
Chronic pain syndromes and motor dysfunction are among the top medical complaints of adults in the 21st Century. Excessive sitting, sedentary lifestyles, chronic stress and obesity are all contributing factors. For physically active adults, overuse during sports and exercise can result in reduced performance and increased injury risk.
Sadly, most approaches to treating chronic pain yield less-than-satisfactory results. Prescription pain medications are fueling an out-of-control opioid crisis, and over-the-counter alternatives do little to alleviate pain. Moreover, medications only treat pain symptoms, without getting at their source.
Surgery is another approach that often falls short of getting to the root cause of chronic pain. Considering its invasive nature, low rate of success and astronomical cost, surgery is simply not an option for many sufferers of pain and dysfunction.
Dry Needling is a treatment approach that has hovered in the shadows of alternative medicine for decades. Its genesis dates back to 1979, when it was introduced by Czech doctor Karel Lewit for myofascial pain relief. The technique was further explored by Travell and Simons in the 1990s, and research on the use of trigger point dry needling under ultrasound guidance was published by Bubnov in 2010.
In recent years, Dry Needling has been getting a closer look as an inexpensive and minimally invasive alternative therapy for resolving pain and motor dysfunction. Dry needling is distinct from injection therapies that use drugs, irritants or other substances to elicit a curative response. When used in conjunction with guided imaging, Dry Needling accurately targets trigger points to provide pain relief and restore motor function.
Following are 10 little-known facts about Dry Needling that shed light on its mechanisms and efficacy:
Dry Needling is not the same as acupuncture. While both procedures employ the use of long thin needles without medication, their purposes and outcomes are unique. Dry needling zeros in on myofascial trigger points to evoke a physiological response, while the ancient practice of acupuncture works with the body’s energy meridians, or chi, to restore balance.
Targeted Dry Needling can work better than physical therapy, and requires fewer sessions. When performed by a trained practitioner under ultrasound guidance, Dry Needling can rapidly get to the root of muscle dysfunction. In the case of myofascial trigger points in the rotator cuff of the shoulder, Dry Needling is the most effective method for treating frozen shoulder syndrome. Dry needling is the preferred personalized monotherapy for pain relief and the prevention of trigger point relapse.
When guided by ultrasound imaging, Dry Needling falls under the umbrella of interventional radiology. Multiple clinical studies confirm that the use of guided imagery during Dry Needling can significantly reduce the number of trigger points needled, as well as the number of treatment sessions required.
Dry Needling taps into muscle physiology. Trigger points are tiny muscle spasms that can interfere with muscle function and cause pain. Dry needling works by evoking a twitch response in the muscle tissue, to disrupt and release muscle spasm.
Dry Needling is minimally invasive and not painful. The idea of being punctured by needles can be off-putting for some patients, but measures of pain are comparable to or less than intramuscular injections, or the pain of regular physiotherapy. When compared to the pain of surgical procedures, the discomfort of Dry Needling is negligible.
Dry Needling practitioners are highly qualified medical professionals. Performance of Dry Needling requires extensive expertise in anatomy, ultrasonography, muscle physiology, neurology and orthopedics. At present, physical therapists are the primary representatives of the medical community who practice Dry Needling.
Dry Needling can alter posture and improve motor function. Trigger point-induced muscle spasms can cause restricted movement, pain and postural imbalance. Ultrasound guided Dry Needling releases myofascial trigger points to reduce pain, restore posture and eliminate muscle spasticity.
Dry Needling is often more effective for treating pain and dysfunction than orthopedic surgery. Under ultrasound guidance, Dry Needling can effectively reduce myofascial pain, mitigate symptoms of neuropathy and increase local muscle motility in patients with low back pain. Surgery has a poor track record for successfully treating non-specific low back pain and other pain syndromes.
Dry Needling can be effective for treating tendons, fascia, and athletic injuries. Trigger points often arise as overuse injuries during sports and exercise. If left untreated, they can cause pain, increase injury risk and undermine performance. Dry Needling can be effective for treating both acute and chronic injuries in elite sports, ranging from mild to severe. Many athletes report a noticeable improvement in performance after treatment, although more clinical evidence is needed.
Many health insurance plans cover Dry Needling procedures. The acceptance of Dry Needling as a viable therapy by the insurance industry further validates its efficacy as a treatment option.
Ultrasound guided dry needling has proven safe and effective across populations, including children and elderly patients, with few complications. However, caution should be taken to ensure the practitioner is well-qualified. The procedure poses greater risks to vessels, pleura and neural structures when performed in deep structures without imaging guidance.
Dry Needling is considered a monotherapy, meaning it is used independently of other treatments. As such, its efficacy cannot be challenged when treatment outcomes result in pain relief and restored function.
During the procedure, some patients report soreness and discomfort from the local muscle twitch response. This can be interpreted as a very positive and expected phenomena, indicating that the procedure has hit its mark. The level of pain and discomfort can vary, depending on the technique and skill of the individual practitioner.
Patients should beware of sham practitioners who lack the skills or qualifications to effectively perform Dry Needling. The practitioner should be a trained ultrasound specialist with a successful track record for positive outcomes.
Resource:
Bubnov, R.V., et al. Personalized monotherapy vs protocol therapy complex for frozen shoulder. Comparative study. EPMA J 2014, 5 (Suppl 1): A163. https://doi.org/10.1186/1878-5085-5-S1-A163
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: