August 14, 2023
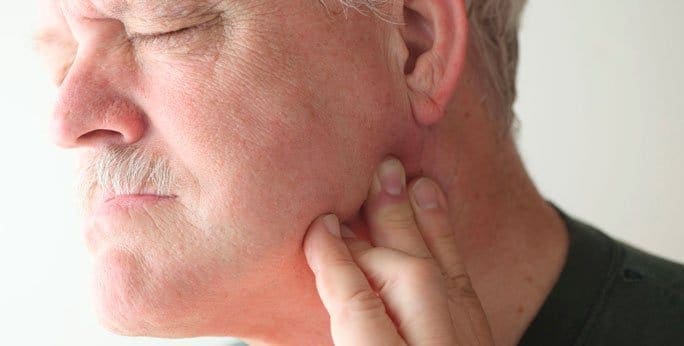
The temporomandibular joint, also known as the TMJ, joins your jaw to your skull. Try feeling it; it lies just in front of your ear hole. There are many causes for tmj disorder, some of which are poor posture, growth disorder, bad habits, inflammation, or injury.
The lower jaw bone, called the mandible, and the socket on the skull, called the temporal bone, make up the TMJ, or the temporomandibular joint. The articular disc, held in place by muscles and ligaments, lies between these two parts and causes the smooth opening and closing of the joint.
You may experience jaw joint pain or uncomfortable facial muscles, experience a clicking, grinding, or locking in the jaw, or suffer headaches and dizziness. If you have trouble opening and closing the mouth or feel pain when chewing hard food or yawning, you very likely have temporomandibular joint (TMJ) trouble.
Usually there is a combination of causes of tmj disorder: overactive jaw muscles, trauma, arthritis, neck stiffness or dysfunction, or even a sensitivity to stress-related pain.
Physiotherapy reduces pain and stiffness while restoring function and teaching management strategies. It is very thorough in giving tmj relief.
Massage the muscles that lie near the joint, using heat or ice for ten minutes to rest your phone between your shoulder and your ear, avoiding the joint.
Holding your neck stiffly, sitting or lying poorly, and holding your jaw in a back position can all hurt, as well as straining your neck. Simply be aware of how to keep your neck strong and mobile. Ask your physiotherapist for further information.
Ask your physiotherapist for further, more specific management techniques for tmj relief. The following are for starters.
Try standing or sitting upright. Draw your chin in until you give yourself a double chin, keeping your head straight on the whole while. Hold this position for at most 5 seconds, repeating it 8-10 times.
Lightly place your to relax the jaw muscles.
On to partially open and then fully open. Push it up with your finger. To keep the movement straight, practice in front of a mirror 6-8 times and 4-6 times daily.
Place the to keep the movement straight. Repeat this exercise 6-8 times 4-6 times per day.
Put the jaw into a neutral position, first partially open, then a knuckle width apart. Meanwhile, apply a gentle pressure with the thumb.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: