August 14, 2023
Ankle sprains are common sports injuries that occur when the ankle rolls in a lateral motion, doing damage to more injuries down the road.
A suspected catalyst for CAI is peripheral nerve damage that occurs with a lateral ankle sprain. Inflammation and scar tissue at the injury site can reduce the space around a nerve structure, putting pressure on the nerve and interfering with optimal neural function. Remember that your nerves send and receive information to do, so a compressed or damaged nerve can undermine normal joint movement and cause instability.
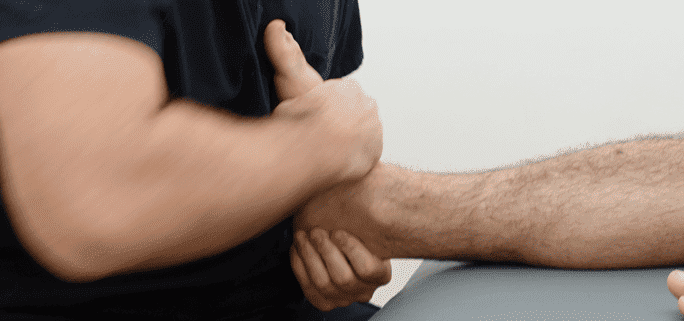
Manual nerve mobilization is a therapeutic technique applied tore optimal function and reduce foot and ankle pain. Nervous tissue is sensitive and must be mobilized gently. When done correctly, manual nerve mobilization can enhance the outcomes of traditional therapies by helping entrapped nerves function freely.
Traditional therapy for CAI includes strengthening and balance exercises, along with proprioceptive training. A 2016 study by Plaza-Manzano et al. sought to conventional therapies.
Fifty-six physically active subjects with CAI were randomly assigned tors over the course of four weeks. The second group of 28 received the same balance and strengthening programs, but also received manual therapy consisting of grade 3 joint mobilizations and peroneal nerve mobilizations.
Subjects were assessed before and at the end of the four week intervention, and again after one month of treatment. A battery of assessment instruments was used to assess pain, ankle stability, joint range of motion and strength. While both groups improved in all assessment categories, the researchers observed greater improvement in the group who received manual therapy.
The results of this study make a compelling case for the inclusion of manual peroneal nerve mobilization therapy in rehab proto improve ankle stability and relieve foot and ankle pain.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: