Acute and chronic injuries to tissues like ligaments, tendons and cartilage can be slow to heal due to their limited vascularity. The complexities of interdependent joint structures and ligament laxity also present challenges. If left untreated, injured tissues can degenerate over time, reducing mobility and creating compensation patterns that snowball into more injuries.
At the same time, fascia that surrounds and supports joint structures can lose its tensile properties by tearing or becoming densified. Fascia plays a key role in joint integrity, governing joint alignment and providing tensegrity – tension that counteracts and mediates intrinsic and extrinsic forces. Densified fascia can compress nerves and inhibit tissue gliding. When rehabilitating a joint, we must address all tissues involved, and not limit our treatment to a single structure.
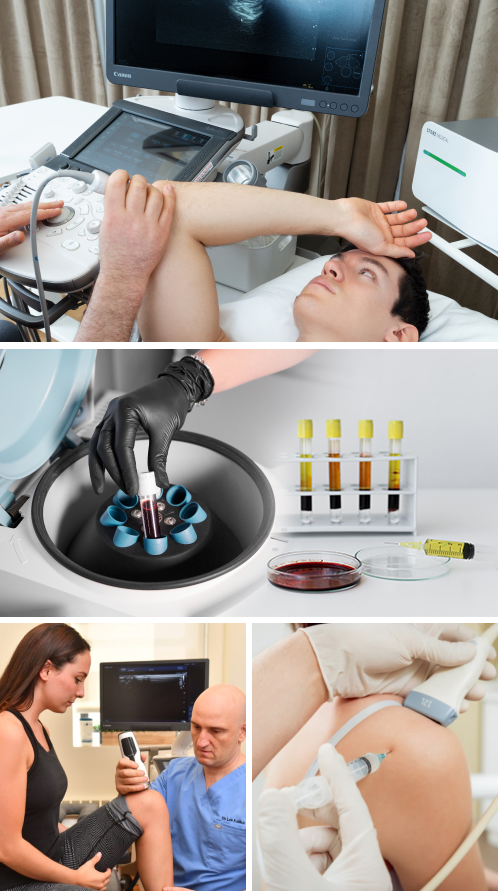
PRP therapy is an evidence-based treatment approach that stimulates the healing of connective tissues and degenerative joint disorders. It uses a sample of the patient’s own whole blood, spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active growth factors that stimulate healing at the cellular level.
However, PRP therapy is not a stand-alone treatment. Prior to injections, blood profiling is recommended, and the body may need to be prepared with physical therapy, osteopathic manipulation and/or other therapeutic treatments to optimize results.
or
NYDNRehab’s clinical director Dr. Lev Kalika is a tendon and biotensegrity specialist, and a recognized expert in diagnostic musculoskeletal ultrasonography. Dr. Kalika has published multiple research articles on the use of diagnostic ultrasonography in rehabilitative medicine. Working in collaboration with our injection therapy specialists, Dr. Kalika’s expertise in ultrasound imaging ensures that needling therapies like platelet rich plasma and prolotherapy accurately hit their mark.
The clinic at NYDNRehab features the highest resolution ultrasound imaging for diagnosis and treatment. Hi-Res ultrasound gives us clear dynamic images of the body’s structures in real time, and empowers us with sonoelastography to test tissue density, and superb microvascular imaging (SMI) to detect early signs of healing.
High resolution ultrasound guidance takes the guesswork out of PRP injection therapy, increasing its efficacy while minimizing discomfort for the patient. Hi-Res ultrasound ensures precision of interfascial plane injections, nerve hydrodissection, and fascia distortion injections. Dr. Kalika’s successful track record of rehabilitating sports injuries and restoring pain-free function makes NYDNRehab the clinic of choice for PRP therapy in New York.
Many clinics offer needling therapies, but most of them do not feature on-sight diagnostic ultrasonography, which requires a highly skilled and experienced doctor. Without the ability to visualize damaged tissues, it is impossible to accurately target them with PRP. We use the most advanced PRP processing equipment for blood profiling and platelet extraction, to ensure a high concentration of at least 4 billion platelets for effective results.
Prior to platelet rich plasma injections, we prepare the body with physical therapy, dry needling , osteopathic manipulations and fascia manipulation. The musculoskeletal system relies heavily on stability generated by fascia’s tensile properties. Fascia must be able to stretch and glide, to empower the body’s structures to move freely without friction.
Densified fascia and adhesions can pull against newly reinforced tissues, causing them to fray or break. Damaged fascia and torn non-tendinous muscle attachments can interfere with coordinated muscle activation patterns, creating overload on other structures, causing pain and limiting mobility.
Identifying damaged fascial planes requires a sophisticated clinical skill set, to determine loss of tensegrity and load transfer failures. Once identified, we use interfascial plane hydrodilatation injections, prior to or in conjunction with PRP, to release fascial densifications and restore gliding and tensegrity.
At NYDNRehab, extracorporeal shockwave therapy (ESWT) and prolotherapy are used in conjunction with PRP to optimize its regenerative effects, and to enhance the integrity of stabilizing structures surrounding the treated joint. ESWT prolongs the activation time of PRP while simultaneously stimulating production of the body’s own growth factors. In many instances, ESWT is more effective for cellular repair than PRP, and less invasive. Patients choose NYDNRehab over other clinics based on our expertise and experience. Our integrative holistic approach and our proven track record of successful results, along with our cutting-edge technologies and therapies, make NYDNRehab the clinic of choice for PRP therapy in NYC.