Tensegrity is the Secret to Pain-Free Mobility
Most people take everyday mobility for granted until an injury occurs or pain sets in. Sometimes pain and reduced mobility seem to arise out of nowhere, with no apparent cause of onset. Regardless of whether your pain is caused by trauma or by something less obvious, tensegrity plays a key role.
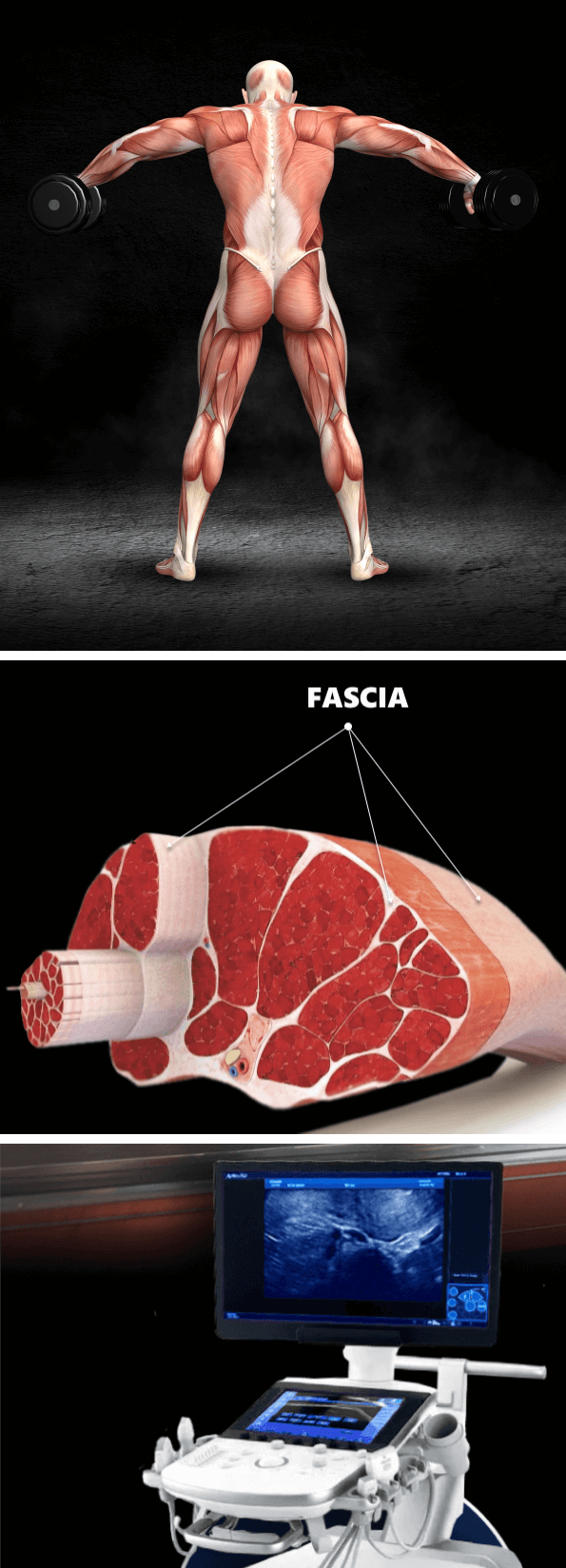
Tensegrity refers to tensile integrity – a state where a system of individual components is held together under continuous elastic tension. In the human body, tensegrity is created by the myofascial system, the network of muscles and fascia that work together to produce, control, and guide forces, and to hold the body’s various organs and structures in place during movement.
Tensegrity can be disrupted when myofascial tissues are injured or damaged in some way. When that happens, nerves and blood vessels can become entrapped, preventing them from gliding among other structures and producing pain. At the same time, the elastic tension that governs joint alignment and controls movement becomes compromised, creating motor deficits that undermine mobility and stability.
Factors that disrupt myofascial tensegrity include:
- Traumatic injury that affects multiple tissue types
- Overuse injuries from sports, exercise or occupation
- Old injuries that were never properly rehabilitated
- Sedentary lifestyle with excessive sitting
- Obesity that overloads the body’s structures
- Inadequate hydration that deprives soft tissues of water needed to function
- Diet high in sugar and carbs that causes myofascial tissue glycation, making it dense and sticky
Many doctors do not understand the crucial role of the myofascial system in preventing pain syndromes, movement disorders, and disease. In fact, most medical doctors have no idea how to correct myofascial dysfunction or even recognize it as a factor. They simply treat pain symptoms with medications and eventually recommend surgery.
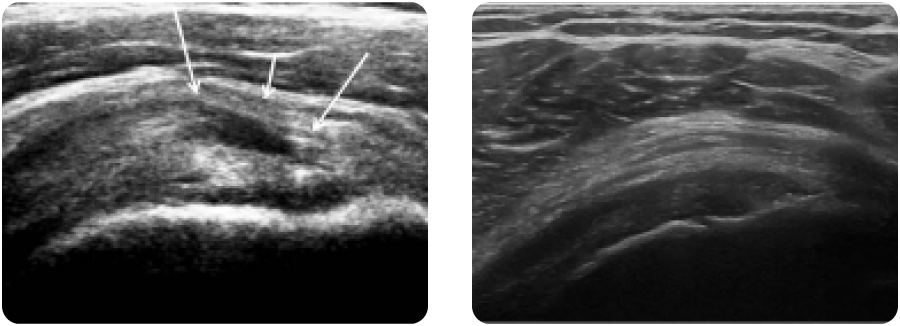
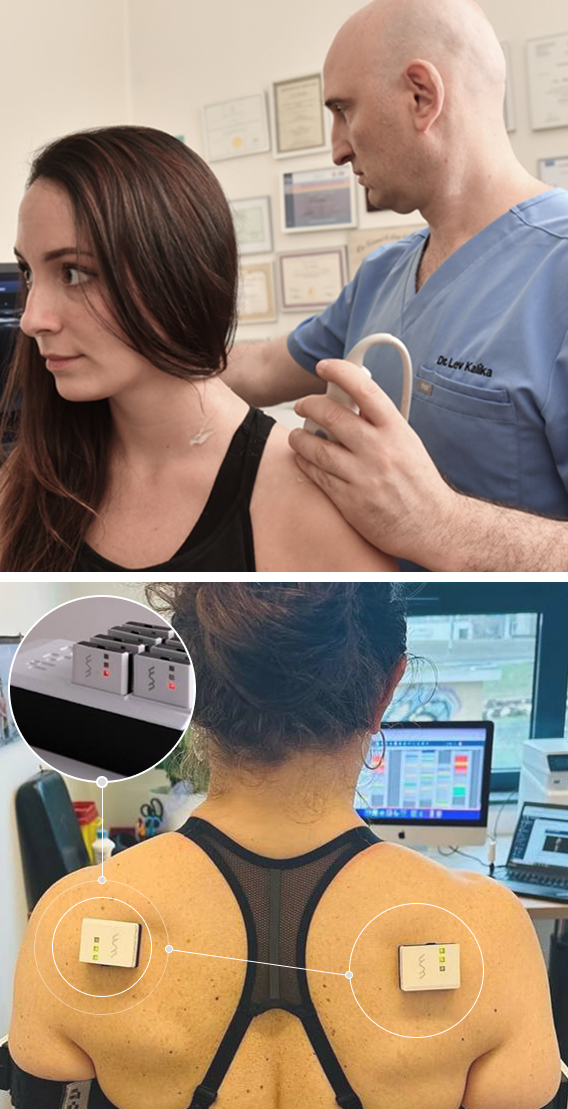
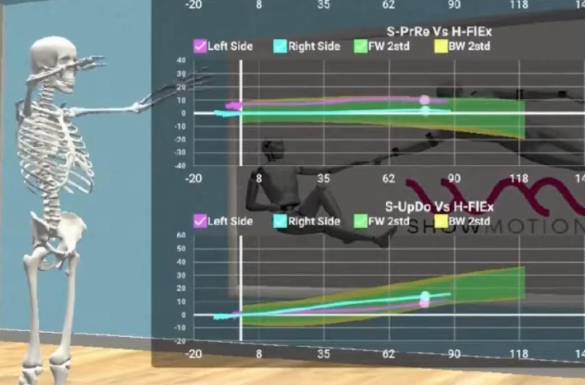
At NYDNRehab, we understand that the body’s systems work together as an integrated whole, and that treating pain is not enough to eliminate its source. We use dynamic high-resolution ultrasound to explore the myofascial system in real time. Ultrasound imaging lets us visualize muscles, fascia, nerves and other structures in motion, to identify places where tensegrity has been disrupted.
Once we identify the problem, we use the most advanced therapeutic approaches to restore myofascial integrity and promote tissue healing.