- Home
- Who We Are
- What We Treat
- Hip
- Elbow and Arm
- Back Pain
- Low Back Pain
- Mid Back Pain
- Neck Pain
- Shoulder
- Wrist Pain
- Knee
- Foot and ankle
- Heel Pain
- Muscle Pain and Myofascial Pain Syndrome
- TMJ and Orofacial
- Womens Health
- Cervicogenic Headache
- Joint Hypermobility Syndrome
- Pelvic Pain
- Fibromyalgia
- Sciatica Pain (Sciatic Nerve)
- Shockwave Therapy for Lymphedema
- Carpal Tunnel Syndrome
- SI Joint Physical Therapy
- Golfers Elbow
- Holistic Podiatry Specialist
- Diagnosis
- Treatment
- Ultrasound Guided Procedures
- Physical Therapy
- Extracorporeal Shockwave Therapy ESWT
- Dynamic Neuromuscular Stabilization
- Fascia Manipulation Therapy
- Dry Needling
- Computer Assisted Rehabilitation Environment (C.A.R.E.N)
- High Energy Inductive Therapy (HEIT)
- Extracorporeal Magnetic Transduction Therapy
- Chiropractic
- Trigger Point Therapy
- Postural Reeducation and posture treatment
- Anatomy In Motion
- Acupuncture
- Tendon clinic
- Сupping therapy
- Gait Analysis LAB
- KINEO intelligent load and reactive neuromuscular training
- Pediatric Physical Therapy
- Neuromuscular therapy NYC
- Prolotherapy Specialist
- High Pressure Cryotherapy
- Blood flow restriction training
- INDIBA Tecar Treatment
- NESA Neuromodulation Therapy
- Sports Medicine
- Ultrasound Guided Procedures
- NYC Marathon
- 3D Running Gait Analysis
- Technology-Based Gait Analysis
- Computer Assisted Rehabilitation Environment (C.A.R.E.N)
- Dynamic Neuromuscular Stabilization
- Running Diagnosis
- Sports Injuries
- Running Services
- Return to Sports
- Sports Physical Therapy
- Sports Injury Prevention
- Golf Injury
- Anatomy in Motion
- Performance Lab
- 3D Motion Analysis
- Sonoelastography for Rehabilitation, Enhanced Performance and Injury Prevention
- Post-Exercise Recovery for Sports, Dance and Fitness
- The Most Comprehensive Assessment for Strength and Power is Driven by Technology
- Insurance
- Telehealth
- Contact Us






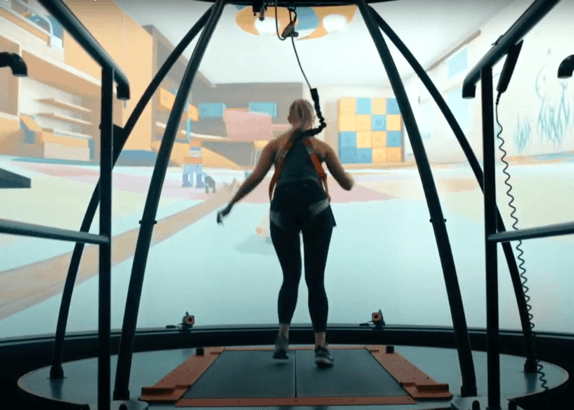



 Dr. Yuri Brosgol
Dr. Yuri Brosgol  Dr. Michael Goynatsky
Dr. Michael Goynatsky  Dr. Daniela Escudero
Dr. Daniela Escudero  Dr. Michelle Agyakwah
Dr. Michelle Agyakwah  Dr. Tatyana Kapustina
Dr. Tatyana Kapustina 


























