
Acupressure is an offshoot of Acupuncture, the ancient Chinese practice of inserting thin needles at strategic points to align the body’s energy meridians. Acupressure is a non-invasive approach for activating certain pressure points to alleviate pain and dysfunction. Nine specific pressure points can be easily targeted to quickly relieve pain from headaches and migraines.
Using correct technique is key to effectively activating your body’s headache pressure points. You can have a friend or family member perform acupressure for your headache, or you can do it yourself.
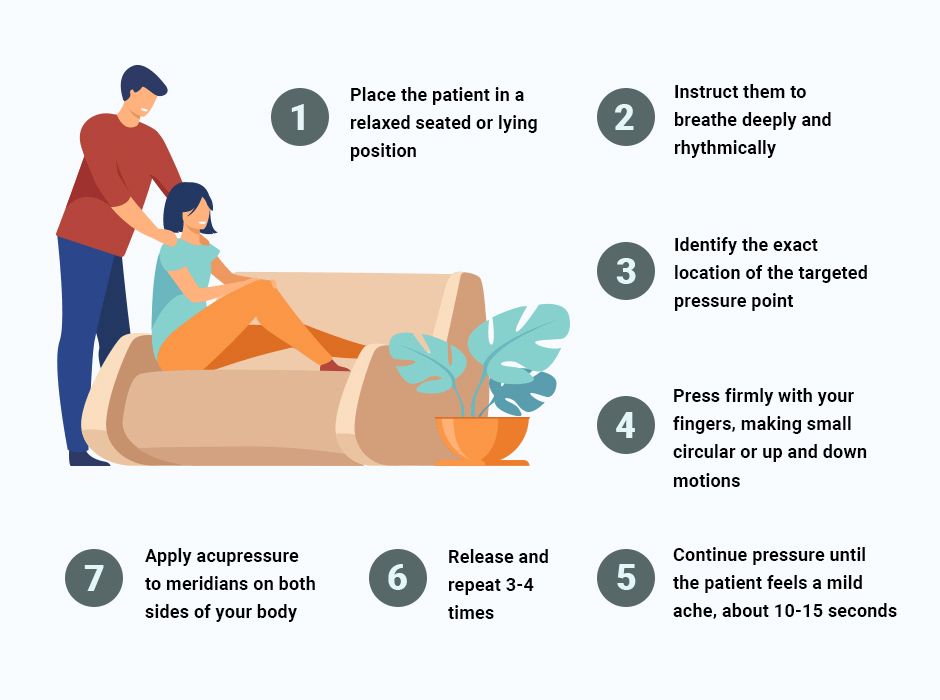
Follow these tips for acupressure success:
Place the patient in a relaxed seated or lying position
Instruct them to breathe deeply and rhythmically
Identify the exact location of the targeted pressure point
Press firmly with your fingers, making small circular or up and down motions
Continue pressure until the patient feels a mild ache, about 10-15 seconds
Release and repeat 3-4 times
Apply acupressure to meridians on both sides of your body
You can perform acupressure several times per day, but be sure to give your body a rest. Begin with light pressure and gradually increase as needed, according to the patient’s tolerance.
Remember that headaches and migraines are often caused by stress. Learning to manage stress is the best way to avoid headache pain.
Acupuncture, and its offshoot acupressure, are based on various meridian lines that run along the surface of your body. To accurately locate acupressure points, you can reference the Atlas of Acupuncture Points. The main pressure points for headaches are located in the following meridians:
Follow these tips for acupressure success:
LU lung meridian
LI large intestine meridian
GB gall bladder meridian
SI small intestine meridian
SP spleen meridian
ST stomach meridian

It is important to keep in mind that everyone has a unique anatomy, and your headache pressure points may be slightly above or below the indicated location. To find your own pressure points, close your eyes and gently probe with your fingers along the meridian line near the location of the pressure point.
All points are referenced with the body in anatomical position, that is, standing erect with the arms at your sides.
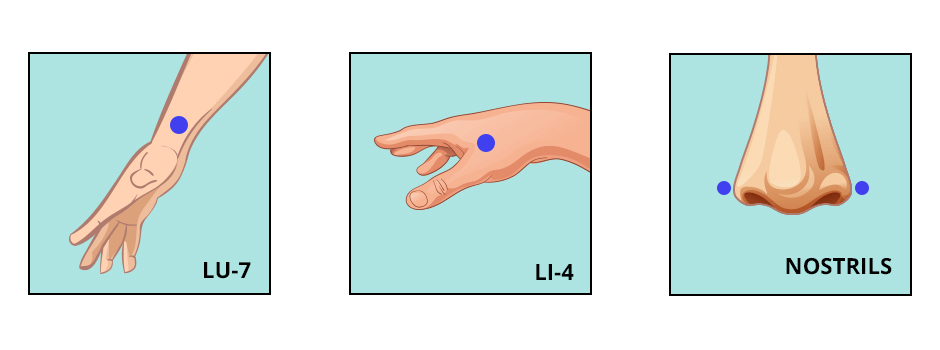
LU-7. This point is located at your wrist, above the distal epiphysis of your radius. In layman’s terms, it is on the thumb side of your wrist, above the place where your radius bone protrudes, in line with your thumb.
LI-4. Find this pressure point about an inch-and-a-half above the webbed junction of your thumb and forefinger, below the protuberance of your radius.
Nostrils. Pinch your nose cartilage just below the bony protuberance.
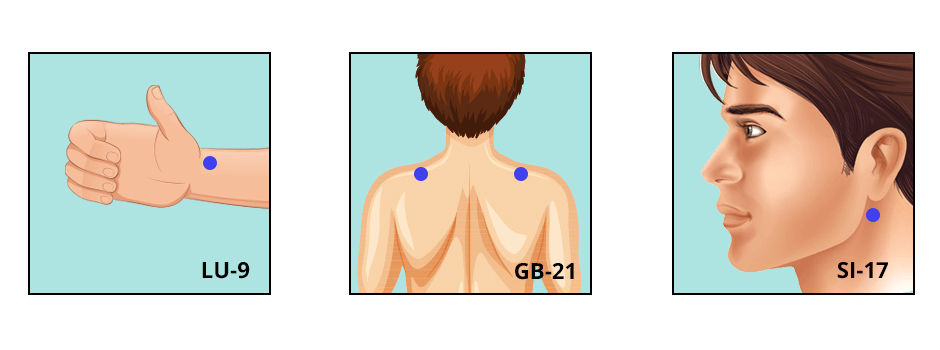
LU-9. Located at the crease of your inner wrist, in line with your thumb.
GB-21. Find this point midway between the bony prominence formed by your 7th cervical vertebra and the highest point of your trapezius muscle.
SI-17. Located at the back edge of the jawbone, just below the ear.
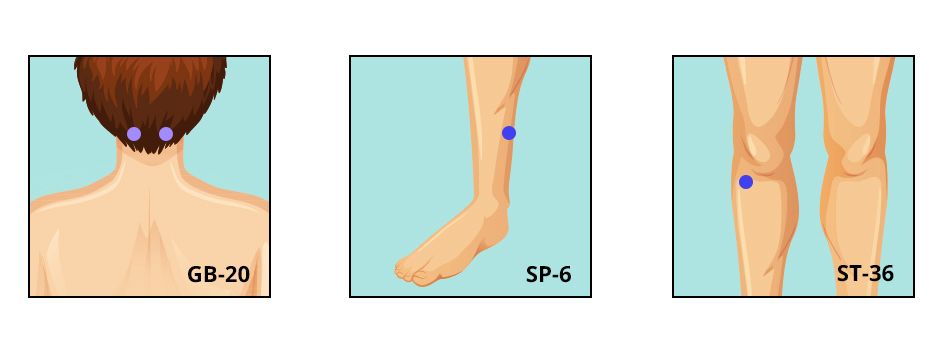
GB-20. Find it at the base of the back of your skull, on either side of the groove formed by your neck muscles.
SP-6. Located just above your inner ankle bone, along the edge of your tibia (shin bone).
ST-36. This point is found about 4 inches below your kneecap, on the outer edge of your shin bone.
In addition to stress, headaches and migraines can stem from poor posture, muscle imbalances and compensation patterns adopted after an injury. They can also be associated with degenerative disc disease in your upper spine.
Common musculoskeletal conditions that cause headaches include:
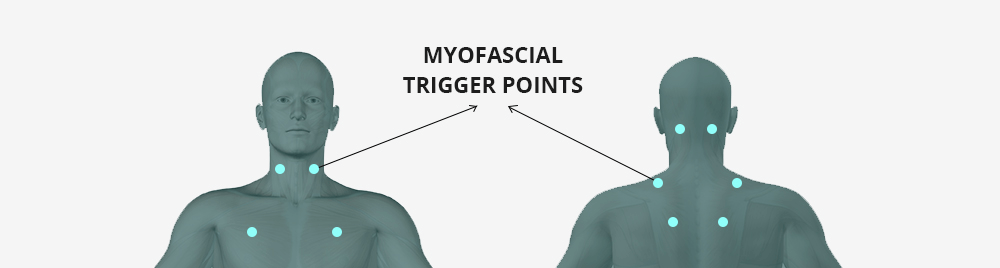
Referred pain from myofascial trigger points located in the muscles that support the neck and head. Superficial trigger points can be felt as tiny hard knots just below the skin’s surface, and can be released using pressure and massage. Deep tissue trigger points cannot be palpated from the surface. Effective treatment requires ultrasound guided dry needling to accurately target the trigger point and stimulate release.
Cervicogenic headaches arise from issues in the cervical spine that put pressure on the nerves that innervate the head and brain. Treatment may require chiropractic care and physical therapy, to restore neck alignment and function, and alleviate headache pain.
TMJ syndrome, a disorder where the temporomandibular joint becomes misaligned and malfunctions, causing pain and stiffness in the jaw, and sometimes causing headaches. TMJ syndrome requires intervention by a chiropractor or physical therapist.
Text neck, a 21st Century postural phenomenon where the head is thrust forward for extended periods of time while viewing a mobile device, altering the alignment of your upper spine, and causing neck pain and headaches.
While learning to manage stress and using acupressure for headache symptoms can be effective approaches for self-treatment, chronic headaches may be caused by musculoskeletal issues that are not so easily resolved.
At NYDNRehab, we use the latest technologies and innovative treatment methods to identify the underlying cause of your headaches and resolve them. You don’t have to live with chronic headaches. Contact NYDNRehab today, and get rid of your headaches for good, so you can get on with your busy life.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: