Advanced Diagnostics are Key to Successful Achilles Tendinitis Treatment
Achilles tendon injuries can range from mild tendinitis marked by pain and inflammation, to full-blown acute ruptures that can be crippling. Getting a quick and accurate diagnosis is the first step to developing an effective treatment protocol
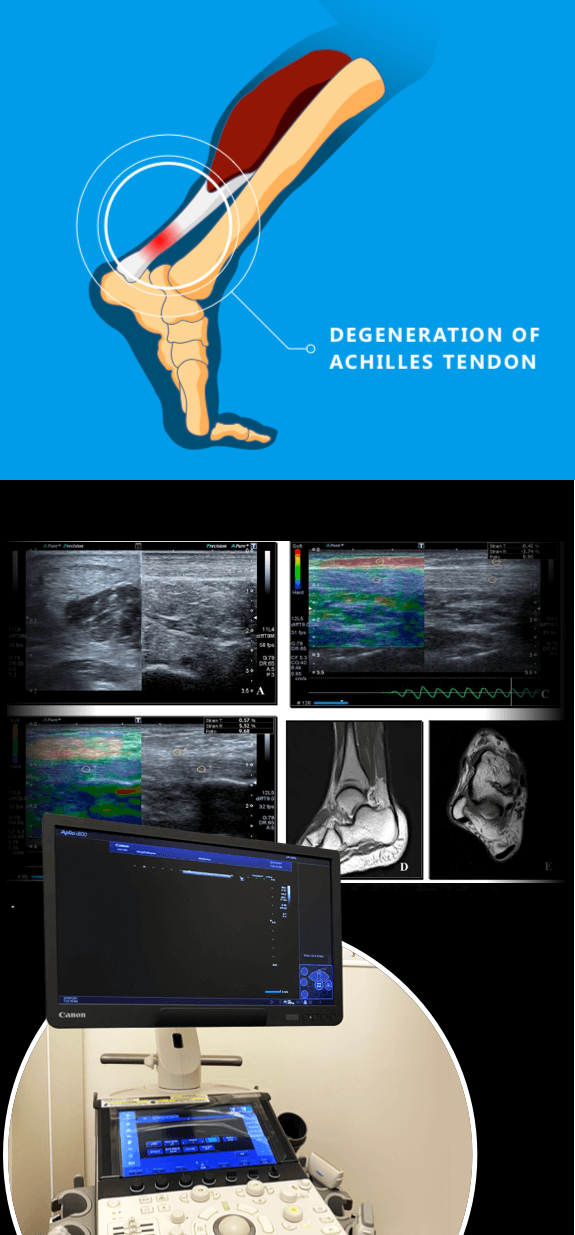
At NYDNRehab, we use the most advanced high-resolution diagnostic ultrasound available to visualize the damaged tissues in real time, with the patient in motion. Once we identify the type and extent of damage, we dive deeper to create a baseline profile for Achilles tendonitis physical therapy.
Your baseline assessment may include:
Sonoelastography, a unique technology that enables us to measure tendon stiffness.
Force plate jump testing to evaluate elastic recoil and force production.
Kineo Intelligent Load system to measure eccentric tendon strength.
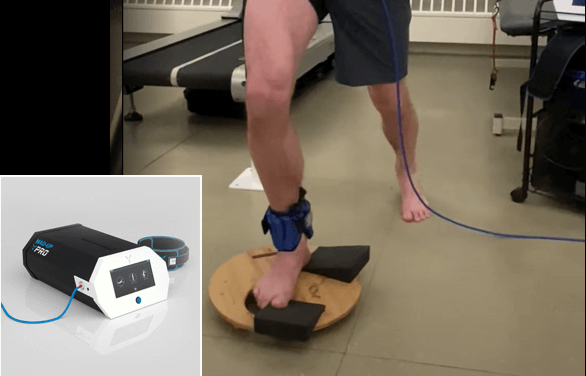
Platform perturbation on C.A.R.E.N, our computer assisted rehab environment, to assess tendon landing on an unstable surface.
Tendon tolerance testing, to assess load tolerance for training and rehab.
Superior microvascular imaging (SMI), to detect healing activity at the capillary level and monitor the healing process.
Our thorough and accurate diagnosis of your Achilles tendon ensures that our treatment protocol is effective, and that no time is wasted on ineffective treatment methods. Our goal for Achilles tendon physical therapy is to restore full function in the shortest time possible, so you can get back quickly to your sport or activity.