Your hamstrings are made up of three muscles at the back of your upper leg, with tendons crossing over both the hip and knee joints. Their actions include hip extension and knee flexion. Hamstring injuries are common in athletes and physically active people, They often involve tendon and/or muscle ruptures ranging from mild to severe. When hamstring tendon injuries are not properly rehabilitated, the tendon can degenerate, leading to long-term impaired mobility.
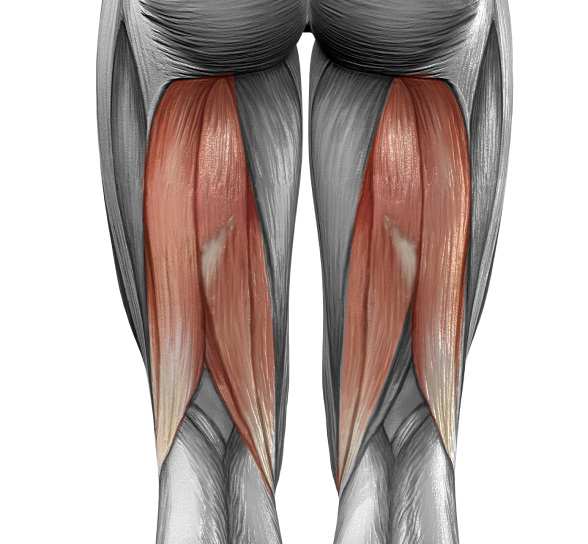
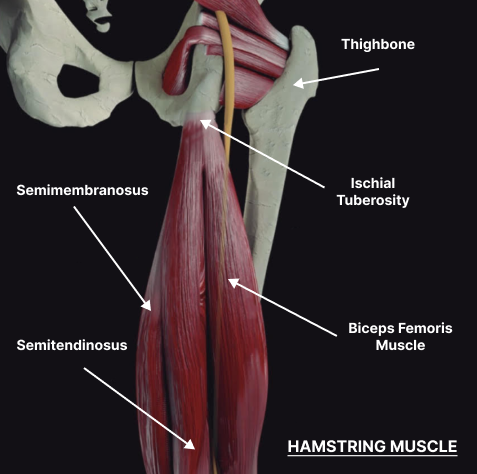
The three hamstring muscles are the semimembranosus, the semitendinosus, and the biceps femoris. All three muscles attach distally to the tibia, or shin bone, just behind the knee joint. At the proximal (hip) end, the tendons attach to the ischial tuberosity, or sit bones. Hamstrings produce two joint actions: hip extension — in conjunction with the gluteal muscles — and knee flexion.
Common types of hamstring injuries include muscle strains, muscle and tendon ruptures, and tendinopathy, a chronic condition of tendon dysfunction. High hamstring tendinitis is inflammation of the hamstring tendon where it attaches at the ischial tuberosity. High hamstring tendinopathy often begins as an overuse injury that can degenerate over time if not fully rehabilitated. Because tendons are thick and fibrous, they have a limited blood supply and are slow to heal.
or
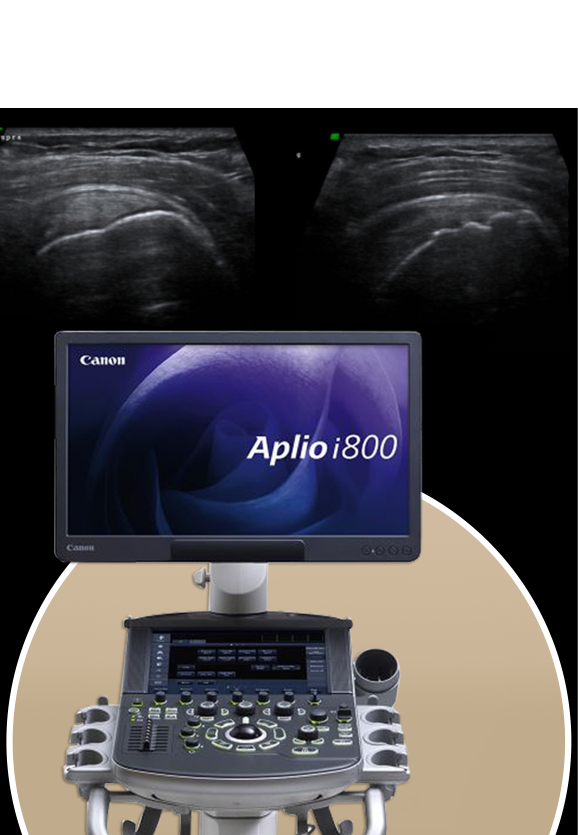
The clinic at NYDNRehab features the highest resolution ultrasound equipment available for diagnosis and ultrasound guided injections. This advanced technology gives us crystal-clear images of large structures like tendons, ligaments, nerves, muscles and bones along their entire length, in real time. It also gives us the capability to test tendon density via sonoelastography, and enables us to detect early signs of tendon fiber healing via superior microvascular imaging.
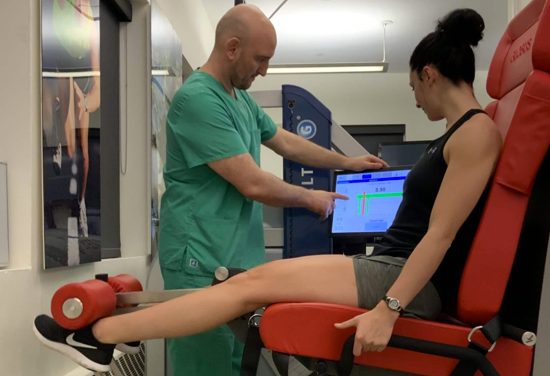
In addition to ultrasound capabilities, we use 3D motion analysis technology to accurately detect motor deficits that contribute to hamstring injuries. We use the most advanced regenerative technologies available to stimulate and accelerate the hamstring healing process.
Dr. Kalika has helped hundreds of athletes and physically active patients with hamstring injuries to return to their sport or activity in the shortest time possible.
NYDNRehab clinical director Dr. Lev Kalika has devoted his life’s work to revolutionizing the way physical pain syndromes and motor disorders are diagnosed and treated. Dr. Kalika is a world-renowned expert in diagnostic musculoskeletal ultrasonography, and has contributed multiple research articles to the growing body of scientific literature on its use in rehabilitative medicine.
At NYDNRehab, we treat the whole patient, not just their symptoms. Our personalized one-on-one approach to patient care means you get a customized treatment plan, based on your unique diagnostic profile.
There are dozens of physical therapy clinics in Manhattan NYC to choose from, but most rely on symptoms-based diagnosis, antiquated timelines and one-size-fits-all protocols to treat hamstring injuries.
Without ultrasound imaging capabilities, patients are often misdiagnosed and prescribed inappropriate treatment plans that only prolong their pain without resolving their condition. In some cases, inappropriate treatment can even make your condition worse.
Our high-resolution diagnostic ultrasound gives us dynamic images of your hamstring injury in real time, eliminating any guesswork. Ultrasound imaging is performed right in our office — no waiting for lab results — so we can quickly create your personalized treatment plan and put you on the path to recovery.
Prior to beginning physical therapy for hamstring strains and tendon injuries, we pre-treat your damaged tissues with regenerative technologies and therapies, to promote and accelerate healing.
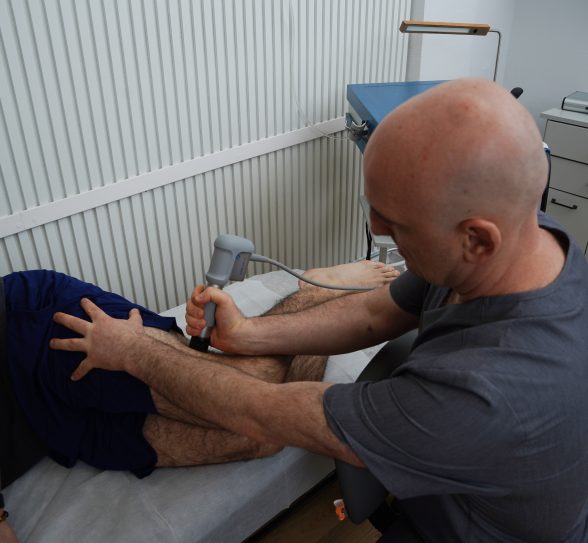
We diagnose your injury using the highest resolution diagnostic ultrasonography, for crystal-clear images of your hamstring injury in real time. Dynamic imaging lets us view your hamstrings in motion, to assess how the muscles interact with other structures. We are able to compare the injured and uninjured leg, to take into account your unique anatomical architecture. We assess tissue damage and pre-treat your injury with regenerative technologies, to prepare you for physical therapy.
In addition, our 3D motion analysis technologies enable us to precisely measure force loads, joint angles, center of mass, muscle firing patterns and other issues that affect hamstring muscle function. We use your collected data to establish a baseline, then provide feedback retraining to fine-tune your movement patterns to optimize performance and reduce your risk of injury.
Hamstring injuries are often misdiagnosed, leading to inferior treatment approaches that waste time and money, while pain persists and the tendon continues to deteriorate. At NYDNRehab, we know that hamstring rehabilitation takes time, and we believe that time should not be wasted.
Ultrasound lets us zero in on the injured tissues to identify their nature, severity, and scope. It also equips us with sonoelastography and superior microvascular imaging capabilities, to distinguish tendonitis from tendinopathy, rupture or avulsion. A tech-driven 3D biomechanical analysis lets us identify and quantify faulty motor patterns that can lead to hamstring injuries.
Dr. Kalika’s expertise as a hamstring doctor has helped scores of runners, athletes and physically active New Yorkers to quickly recover from hamstring injuries and confidently return to their sport or activity.
Our 3D motion analysis system was designed by Dr.Kalika and implemented by STT. USONO portable device, allowing for real-time visualization of muscle action via diagnostic ultrasound, and syncing it with data from our movement analyzing technology. This specific configuration is based on the latest evidence-based motion analysis research.
Our analysis is based on SEBT research. SEBT is considered the gold standard for motion analysis protocols. It is a full-body system, able to register movements in both the upper and lower body.
Our 3D motion analysis system gives us a broad range of quantitative data about movement:
A patient may present with prior ankle trauma that appears stable after clinical testing and diagnostic ultrasonography. However, those methods do not reveal potential sensory-motor ankle instability, which can alter motion along the entire kinetic chain. It can affect movement of the knee, hip, pelvis and lumbar spine. An in-depth 3D analysis can reveal whether a prior trauma is well compensated for, or if it is constantly altering movement, causing muscle over-recruitment in other joints, in an effort to absorb impact or create artificial stability.


Physical therapy is an important part of hamstring rehabilitation, but it is not a stand-alone solution. Prior to beginning physical therapy, we thoroughly assess and pre-treat tissue damage with regenerative solutions, to accelerate tissue healing and optimize the outcome of your physical therapy protocol.
Regenerative therapies leverage innovative new technologies that jump-start the healing process in damaged muscle and tendon cells. Your treatment protocol may begin with regenerative and/or needling therapies to accelerate tissue healing and prepare you for physical therapy.
Issues that should be addressed prior to physical therapy include:

Focused Shockwave Therapy
Focused ESWT is an evidence-based technology for treating damaged tendon, muscle and bone tissue. ESWT uses high frequency sound waves to stimulate the body’s own reparative mechanisms. ESWT is especially effective for degenerative hamstring tendon disorders.
EMTT transmits high energy magnetic pulses to targeted tissues that synchronize with the body’s own magnetic fields, triggering a regenerative response. EMTT waves can penetrate deep tissues to target difficult-to-reach tendons, muscles, bones and nerves.

Electromagnetic Transduction Therapy (EMTT)

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues, to speed up the delivery of oxygen and nutrients and stimulate cellular metabolism
HEIT uses electromagnetic fields to reactivate the electrochemical function of cells and cell membranes, to optimize ion exchange.

HIGH ENERGY INDUCTIVE THERAPY (HEIT)

INDIBA Radiofrequency Therapy
NESA generates a low-frequency electrical current of intermittent and cyclical stimuli that calms hypersensitized nerves and restores optimal signaling between the autonomic nervous system and the brain.
INDIBA therapy helps to restore the ionic charge of damaged cells, for faster injury healing and rehabilitation.

NESA Neuromodulation Therapy
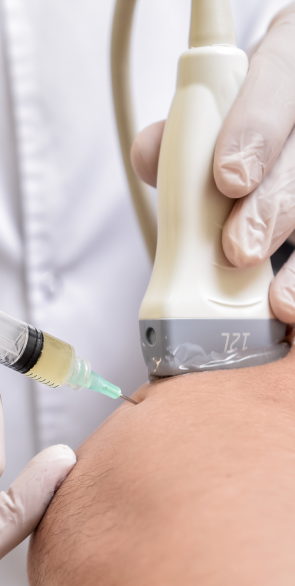
Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
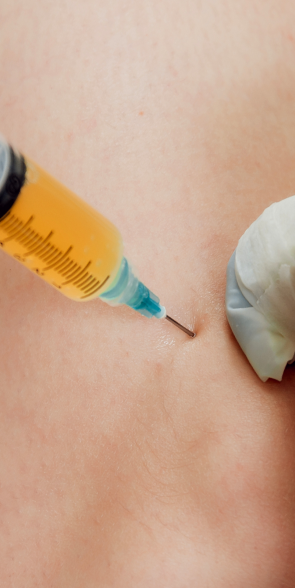
PRP therapy uses a sample of the patient’s own whole blood, spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors, to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution that irritates slow-to-heal connective tissues, to encourage growth of new normal ligament or tendon fibers.
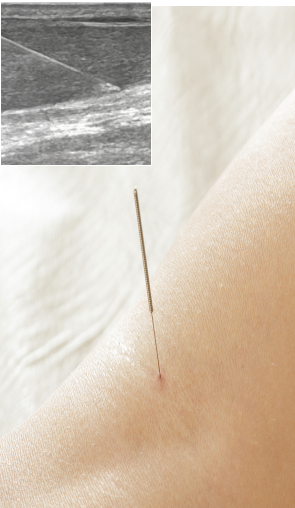
Myofascial trigger points are often present in hamstring injuries. Dry needling inserts thin non-medicated needles into trigger points to evoke a twitch response, releasing the trigger point and immediately relieving pain. Ultrasound guidance eliminates the need for multiple insertions, reducing pain and discomfort for the patient.
Hydrodissection is sometimes used to treat peripheral nerve entrapment. It uses a saline solution to separate entrapped nerves from surrounding fascia adhesions and/or adjacent structures.
Physical therapy is geared to enhancing tissue strength and integrity, and ultimately restoring pre-injury performance levels. Our cutting-edge technologies incorporate artificial intelligence, virtual reality feedback and quantitative data analysis to retrain your motor responses and accurately measure your progress.
Our advanced technologies eliminate guesswork by measuring and quantifying motor parameters and muscle firing patterns, to accurately track your progress and confirm your readiness to return to physical activity.
Your physical therapy protocol may include some or all of the following:
Measures taken before and after physical activity can have a profound impact on injury prevention. The hamstring muscles are especially vulnerable to injury due to their architecture and dual-joint action.
Follow these guidelines to reduce your risk of hamstring injuries:

Hamstring injuries can be painful and debilitating. If not properly treated, a hamstring muscle or tendon injury can be career-ending for athletes. For active adults, hamstring injuries that are not rehabilitated can lead to a steady decline in quality of life. Run-of-the-mill physical therapy clinics often lack the technology and expertise to thoroughly rehabilitate hamstrings, leaving you with long-term impaired mobility.
At NYDNRehab, our advanced technologies and cutting-edge methodologies take the guesswork out of injury rehab. We measure and monitor your progress every step of the way, from diagnosis to return-to-sport. Our personalized one-on-one approach ensures that you get an accurate diagnosis and customized treatment plan, based on your unique profile. Accurate diagnosis and cutting-edge therapies set NYDNRehab apart as New York’s rehabilitation clinic of choice for hamstring injuries.
These case studies reflect real clinical conditions evaluated at NYDNRehab using advanced diagnostic methods and individualized rehabilitation strategies. All cases are evaluated and managed by Dr. Lev Kalika and the NYDNRehab clinical team.
It’s never too late to rehab an old injury – in fact doing so can make a profound difference in your overall mobility as you age.
Pain and swelling may disappear on their own, but you may still have issues like scar tissue, trigger points, nerve entrapment, suboptimal muscle firing patterns and degenerating tendon tissue. Unless rehabilitated, all of those can cause long-term disability.
Pain is never normal, and early treatment can save you from a more severe injury down the road. There is a good chance your pain is related to mechanical deficiencies in your running gait. A 3D gait analysis helps to identify mechanical issues and gives you quantitative data for a baseline, so you can make corrections and improve your running performance.
Chronically tight hamstrings are sometimes related to posture issues involving the lumbo/pelvic/hip complex. They can also result from too much sitting, gait issues, and inadequate recovery after exercise. Physical therapy can help to loosen up tight hamstrings and enhance mobility.
Hamstring injuries are unique to each athlete, and the rate of recovery depends on many factors, including the cause of injury, the location and severity of damage, the type of treatment received, and the athlete’s level of compliance. Regenerative therapies can dramatically accelerate the healing process. Quantitative data generated by advanced technologies can help guide, track and confirm the healing journey.