Ankle Injury Rehabilitation
Personalized boutique services supported by cutting-edge integrative diagnostics and advanced holistic therapies.
Doctors Kalika and Brosgol are Revolutionizing
Ankle Injury Rehab
Dr. Lev Kalika, DC, RMSK, is an accomplished expert in functional podiatry and high resolution diagnostic ultrasonography, with 20+ years of hands-on clinical experience.
Dr. Kalika’s holistic approach focuses on ankle function in the context of the entire lower kinetic chain. His diagnostic approach combines high-resolution ultrasound, advanced gait and motion analysis technology, and gold-standard testing to accurately identify injured and dysfunctional structures that interfere with optimal ankle mechanics.
Dr. Kalika is certified in human biomechanics, gait analysis, Dynamic Neuromuscular Stabilization (DNS), extracorporeal shock wave therapy (ESWT), and other integrative approaches. The clinic at NYDNRehab features some of the most advanced technologies for ankle injury diagnosis and treatment in NYC.

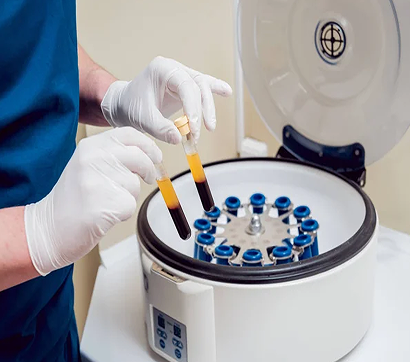
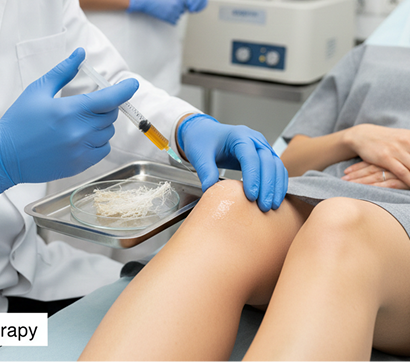
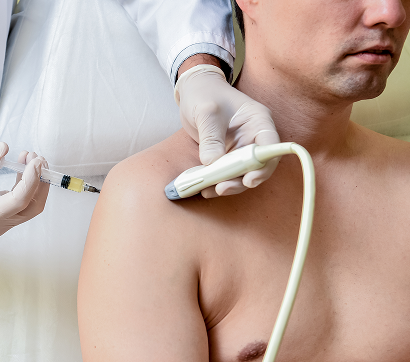
Dr. Yuri Brosgol specializes in advanced ultrasound-guided regenerative medicine for the non-surgical treatment of musculoskeletal pain, osteoarthritis, and sports injuries. His clinical approach includes prolotherapy, neuroprolotherapy, PRP injections, and stem cell-based procedures. His expertise and years of clinical experience inform his selection of personalized procedures, based on specific tissue pathology and individual patient profiles.
Dr. Brosgol’s holistic orthobiologic approach goes beyond injection therapy – he factors in biomechanics, inflammation, nerve irritation, recovery potential, and systemic contributors to healing. His background in functional medicine equips him to successfully treat patients with complex, chronic, or recurrent musculoskeletal conditions.
Patients seeking alternatives to surgery, active individuals with osteoarthritis, athletes with overuse or sports injuries, and patients who have not improved with conventional treatment can all benefit from Dr. Bosgol’s expertise.
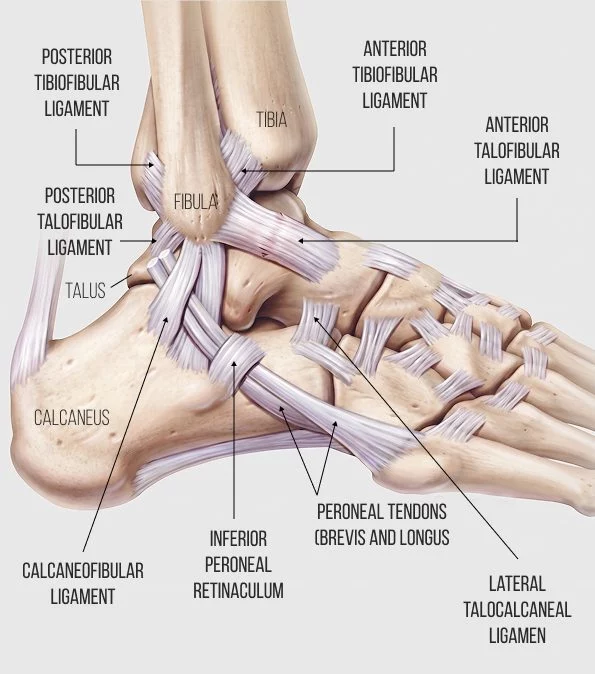
The ankle is intricately connected to the foot and lower extremities, with the foot and ankle complex encompassing the 26 bones of the foot, along with the long bones of the lower leg – the tibia and fibula. Altogether, the bones of the ankle complex form a total of 33 joints, including the tarsal and metatarsal joints of the foot. The foot and ankle complex is richly embedded with nerves and blood vessels that glide among bones, muscles and connective tissues.
The ankle governs gait mechanics, provides balance and stability, and serves as a point of load transfer for forces generated by the muscles of the lower leg, distributing them to the foot and ground to create forward and upward propulsion.
An injured or dysfunctional ankle can cause impaired mobility that affects multiple structures along the lower kinetic chain. Failure to rehabilitate your ankle injury can cause long-term disability and increase your risk of falls and future injuries.
In our opinion, most ankle injuries can be rehabilitated without surgery using a conservative, integrative approach. To optimize results, the ankle should not be treated in isolation, but rather in the context of its function as part of the entire lower kinetic chain.
Types of Ankle Injuries We Treat at NYDNRehab


- Ankle sprains, the most common type of ankle injury, where the ligaments that stabilize the ankle become stretched and/or torn, usually from rolling the foot inward during physical activity. If not properly rehabilitated, an ankle sprain can cause chronic long-term ankle instability, increasing your risk of future injuries.
- High ankle syndesmotic sprains, a less common type of sprain where the ligaments connecting the tibia and fibula at the upper ankle are stretched and torn.
- Ankle strain, where the muscles that act at the ankle are stretched or torn.
- Achilles tendinopathy, where the Achilles tendon develops lesions or ruptures from repetitive overuse or acute injury. If left untreated, tendinopathy can degenerate over time, affecting mobility and impacting other structures of the lower kinetic chain.
- Ankle Fractures, where one or more of the ankle bones – the tibia, fibula or talus, is broken. Fractures can range from mild stress fractures to serious compound fractures involving multiple bones. The most common ankle fracture is a broken lateral malleolus – the knobby bump on the outside of the ankle.
- Peroneal nerve injury or entrapment, disrupting innervation of the foot and ankle, and causing pain and dysfunction.
- Tarsal tunnel syndrome, where the tibial nerve is compressed within the tarsal tunnel – a narrow space made up of the ankle bones and a band of ligament called the flexor retinaculum, which forms the roof of the tunnel.
- Plantar fasciitis, where the plantar fascia that spans the bottom of the foot develops lesions, becomes densified, and loses its elastic properties, making it painful to stand and walk.
- Multiple less common ankle conditions such as bursitis, osteoarthritis, sinus tarsi syndrome, and ankle hypermobility.
Accurate Diagnosis Ensures Appropriate and Effective Treatment
The ankle’s complex architecture brings together a variety of structures and tissue types within a very compact space, posing a challenge for ankle injury diagnosis. Most medical doctors have limited capabilities when it comes to visualizing the ankle’s structures in detail, and they are often quick to misdiagnose non-traumatic ankle pain as Achilles tendonitis, based on reported symptoms. Such hasty diagnosis can lead to inappropriate treatment that prolongs the patient’s pain and suffering.
On your first visit to NYDNRehab, after your clinical exam and a thorough review of your health history, we use high-resolution diagnostic ultrasound to visualize the affected structures in real time. Dr. Kalika’s expertise in interpreting ultrasound images ensures that your diagnosis is accurate, and nothing is missed.
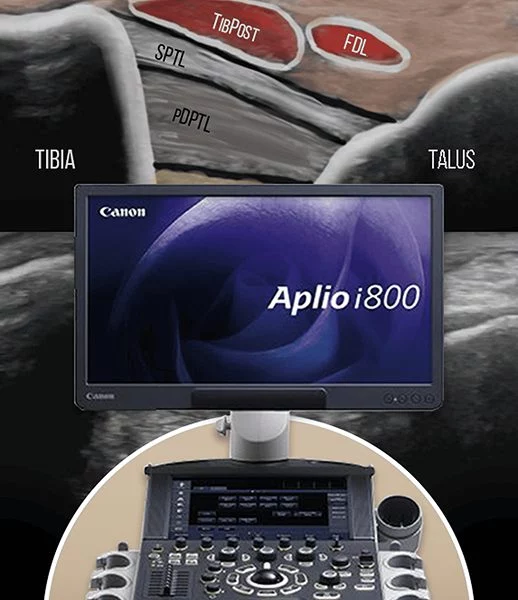
We use advanced technologies to diagnose your ankle injury:
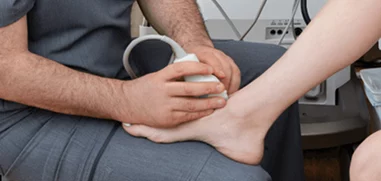
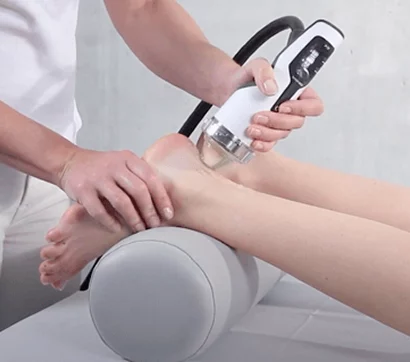
High resolution ultrasonography to view the ankle in motion, in real time.

Quantitative 3D gait analysis, to evaluate multiple markers of ankle dysfunction.
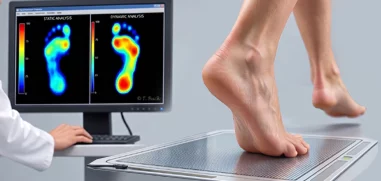
Foot pressure analysis, to capture data on pressure distribution across the sole of the foot during static and dynamic activities.

Kinematic analysis of ankle stability using the Star Excursion Banner Test (SEBT).

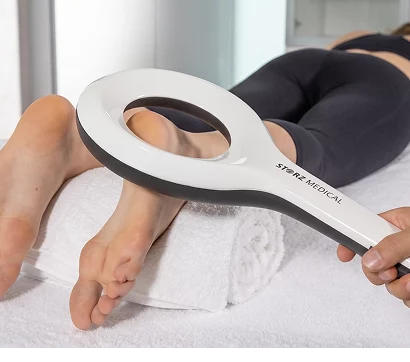
Myolux AI ankle envelope of function analysis tool for objective quantification of ankle function.
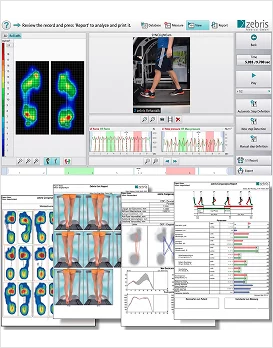
The gait and motion analysis lab at NYDNRehab leverages cutting-edge 3D technology and proprietary software to measure and quantify all parameters involved in human locomotion. We also run a battery of standardized assessments, such as the anterior drawer test, talar tilt test, and functional balance tests like single leg stance, and hop test.
The collected data is analyzed and collated into a comprehensive report that provides a baseline for measuring your progress. Once your diagnostic data is collected and analyzed, we create a personalized treatment plan, based on your unique results.
Why Physical Therapy Alone is Not Enough
to Rehabilitate Your Ankle Injury
Identifying and treating underlying issues prior to beginning physical therapy is key to getting fast and effective results. Failure to pre-treat your damaged tissues can completely undermine your treatment protocol, and in some cases, your condition may even worsen. Physical therapy comes into play in the later stages of rehab, after your tissues have healed and are ready to bear loads.
Obstacles to physical therapy success include:
- Scar tissue and fascia adhesion
- Myofascial trigger points
- Neurogenic inflammation
- Compressed or entrapped nerves
- Joint edema
- Tendons that have degenerated and lost their elastic properties
- Inflamed soft tissues
- Compensation patterns developed post-injury
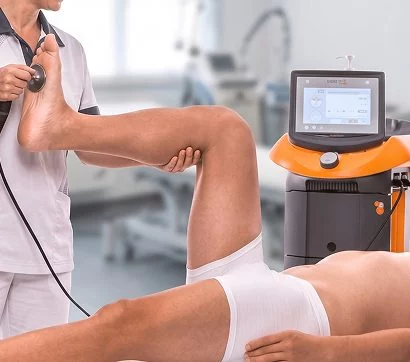
At NYDNRehab, we use a broad range of regenerative technologies and integrative therapeutic approaches to resolve issues that can stand in the way of successful physical therapy. Our staff is certified in a diverse array of holistic treatment methodologies, and our one-on-one treatment sessions are personalized, based on your unique diagnostic profile.
Once we pre-treat your damaged tissues and eliminate compensation patterns, your ankle will be ready to begin physical therapy.
Targeted Ankle Physical Therapy Restores
Strength and Function
At NYDNRehab, we treat the whole patient, not just your symptoms. We never use one-size-fits-all rehab protocols or antiquated recovery timelines. We believe that every injury is unique, and treatment should be based on a holistic approach that factors in the patient’s unique profile.
Once we have successfully pre-treated damaged tissues, we can begin one-on-one physical therapy to restore strength and stability, optimize mobility, and re-establish optimal neuromuscular pathways and muscle coordination patterns.
Your physical therapy protocol may include a combination of the following approaches:
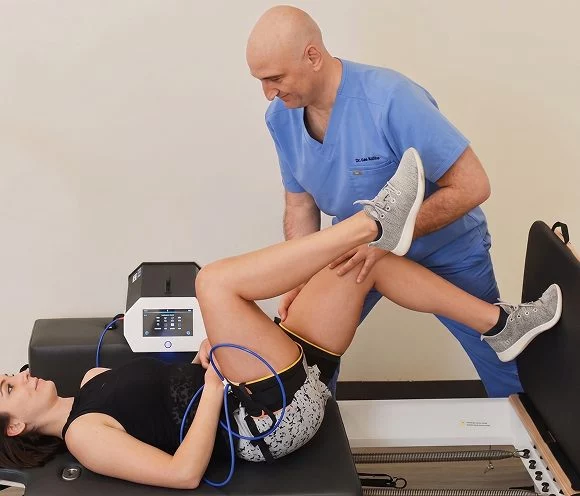

- Stecco fascial manipulation, to eliminate densifications and adhesions and restore fascia’s gliding properties.
- Biofeedback training for balance, gait, and proprioception.
- Stabilization exercises, with real-time visual feedback from the Myolux Medik device.
- Postural restoration therapy to optimize total-body joint alignment.
- Dynamic neuromuscular stabilization (DNS) to restore developmental motor strategies.
- Neurodynamics, to restore communication pathways between the brain and body.
- Dynamic balance exercises using Wobble boards, Bosu balls, or perturbation platforms.
- Blood Flow Restriction Training (BFRT) to increase local muscle strength at substantially lower training volumes.
- Conventional eccentric loading and strengthening exercises.
- Foot core training to strengthen the foot and ankle complex.
- Kineo intelligent loading system, for customized training and rehabilitation exercises. Kineo lets us design a personalized variable load curve based on the needs of the individual patient.
Your back-to-sports physical therapy protocol may include sport-specific training to optimize motor skills and restore peak athletic performance. We carefully monitor patient progress with ultrasound imaging to confirm complete recovery, before releasing athletes back to their sport.
Strategies for Preventing Ankle Injuries
Ankle injuries can arise from a number of factors and scenarios, many over which you have no control. However, there are many things you can do to optimize your ankle strength and stability, to reduce your injury risk and severity.
Strategies for ankle injury prevention:
- Maintain a healthy body weight with an optimal fat-to-lean ration for your age and sex.
- Get regular exercise multiple days per week. Include endurance exercises like walking, running, swimming and cycling, along with total-body resistance training that addresses all major muscle groups.
- Include ankle strengthening exercises like heel raises, plyometric jumps, and foot core exercises.
- Stretch your ankles and surrounding structures after weight-bearing exercise to optimize ankle range of motion.
- Choose comfortable athletic footwear that provides support, shock absorption and stability, and frequently replace worn shoes.
- Allow for adequate recovery time between training sessions.
- Avoid exercising on broken or uneven pavement, or poorly maintained athletic fields.
- Get a 3D gait and biomechanical analysis to identify and correct inefficient ankle mechanics.


I have been a fan of this guy for years and he finally gave his first lecture in English, in London. Dr.Carles Pedret is a world-class medical consultant for muscle injuries in soccer players, tennis players and Olympic sprinters. He is called upon by EPl, Ligue One and LaLiga teams to asses when elite athletes like Messi , Ronaldo or Bale can safely return to the playing field after injury. Dr. Pedret reminds us that the most brilliant people are often the humblest. It was a great experience learning to combine MRI , ultrasonography and advanced functional technology to estimate and provide optimal treatment.

Best ankle rehab nyc
Testimonials
Ankle Injury FAQs
If you have a bad sprain that is affecting your mobility, you should get it checked out right away. If there is serious structural damage, your ankle should be rehabilitated as soon as possible. Failure to do so can lead to more problems down the road, as the ankle provides stability for the entire body. An unstable ankle can cause problems in the knees, hips and low back, and increase your risk of falling.
Ankle injuries vary greatly, and so do injured patients. Adhering to a timeline without any means of monitoring the healing process can put you back in harm’s way before you have fully recovered from your injury. Look for a clinic that uses high-resolution ultrasound and biomechanical technologies to assess and monitor your healing journey.
Bone fractures are often point tender, with discoloration and bruising around the locus of pain. However, there is no way to be certain of a fracture without imaging technology. Diagnostic ultrasound allows for dynamic imaging of the ankle’s structures in real time. It not only confirms the presence of a fracture, but can also identify other tissues injured by a traumatic episode.
Some people have hypermobile joints, meaning they have a greater than average range of motion, making them less stable. This is often due to genetics, where the ligaments are longer or more lax than average. Specialized physical therapy for ankle instability can help you strengthen the structures that support your ankles and make them more stable.
The Achilles tendon plays a major role in most sports, and loading a ruptured tendon is asking for trouble. You can potentially increase the size of the rupture and increase your risk of injury due to compensation. You should wait until your tendon is completely healed before going back to sports. Regenerative therapies can help accelerate the healing process.

Dr.Kalika revolutionized foot and ankle care by using high resolution diagnostic ultrasonography for structural diagnosis, combined with with gait and motion analysis technology. Dr.Kalika’s motion and gait analysis lab is the only private lab in the US that features research-grade technology found only at top research universities, made available to patients in his private clinic.
Our Specialists
 Dr. Yuri Brosgol
MD
Dr. Yuri Brosgol
MD
 Dr. Michael Goynatsky
DPT
Dr. Michael Goynatsky
DPT
 Dr. Daniela Escudero
DPT
Dr. Daniela Escudero
DPT
 Dr. Michelle Agyakwah
DC
Dr. Michelle Agyakwah
DC
 Dr. Tatyana Kapustina
L. Ac.
Dr. Tatyana Kapustina
L. Ac.
Foot, Ankle and Heel Pain Treatment
The human foot design is unique in the animal world. From the evolutionary standpoint human foot is a highly innovative anatomical structure that had developed to serve as the main weight receptor of the newly achieved bipedal support base. It evolved to be the most durable anatomical formation in the entire human body. Aside from the time of infancy when the body is horizontally aligned, the foots intricate structures provide, in conjunction with the ankle bones and powerful connective ligaments, the perfect biomechanical apparatus for ambulation or bipedal locomotion. Read more
Heel Pain and Plantar Fasciitis Treatment
Many people deal with heel pain on a regular basis. Although there are many different causes of heel pain, plantar fasciitis is the most common cause. Plantar fasciitis results when the plantar fascia, or the ligaments that connect the heel to the bones in the foot and provide support to the arch, become strained. A strained plantar fascia causes weakness, swelling, and inflammation as well as thickening, which leads to a great deal of pain. Plantar fasciitis occurs most often in individuals 35 and over, however, those who regularly participate in activities that requires a great deal of standing, or runners, might experience this condition way in advance of middle age. Read more
Heel Pain, Runners Heel and Plantar Fasciitis Treatment
Typically plantar fasciitis is pain in the heel, especially during the initial few steps after waking up. Some other symptoms are: sensitivity and tightness in the heel or the he arch while walking or running.
Patients who suffer from this condition still use old medical terminology, which is no longer used by medical professionals. It was believed previously that heel pain is caused by formation of heel spur. However, this has been disproved a long time ago. Since it is visually appealing for patients to imagine that they step on a sharp bony outgrows, patients still believe that the heel spur is what is causing their heel pain. Read more
Ankle Instability and Ankle Sprain Treatment
Every day 25,000 people sprain their ankle and more than 1 million people a year visit the emergency room due to an ankle injury. Although half of all ankle sprains are caused by athletic activity ankle injuries can happen to anyone at any age not just athletes or weekend warriors. There are different kinds of ankle injuries including sprain, ankle strain, and ankle fracture. Read more
Ankle Instability/Sprain
Ankle instability is a common issue for many people. They may be athletes like basketball players who have stretched their ligaments with regular athletics, or they may be people who discovered their weak ankles aren’t supporting new activities like walking on broken New York sidewalks, or uneven trails. This may be a result of use, limber ligaments, or heredity. This can lead to a lack of support on the foot and high risk of an ankle sprain. For many cases, there are a number of nonsurgical treatments for ankle sprain here at NY Dynamic Neuromuscular Rehabilitation. In extreme cases, surgery may be required. The purpose of rehabilitation exercises within the ankle sprain treatment is to improve muscle strength, range of movement, and sensorimotor control, which are commonly impaired after ankle sprain. Read more