This condition affects the common plantar digital nerve, which innervates the muscles in the foot. Symptoms will usually appear on only one side.
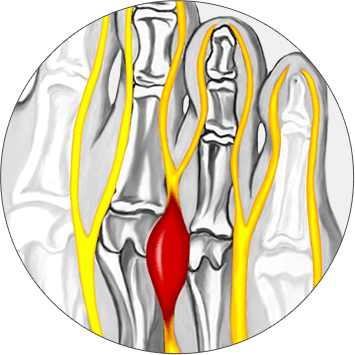
There are some variations, but the pain normally concentrates around the third and fourth metatarsal joint. Pain may radiate in several directions, and some people experience pain in the toes. Sensations of burning, numbness or cramps may appear. Burning sensations appear when the patient wears shoes that exacerbate the condition.
Additional sensations may appear odd to the patient. Examples include a sensation of walking on a pebble or walking on a piece of cramped fabric. The pain increases on hard surfaces and decreases when walking on carpet or other soft surfaces. Pain is often intermittent, and it may appear and recede several times during the week. Most people will only have one lesion per foot, and it is unusual to see two neuromas on the same foot. The lesion can develop when the nerve becomes compressed or irritated by small spaces around the transverse inter-metatarsal ligament.
Diagnosis of Mortons neuroma requires careful examination to exclude similar conditions and neuropathies that may affect the foot.
In addition to physical test, our doctors perform diagnostic ultrasonography to identify and quantify lesion of the interdigital nerve.
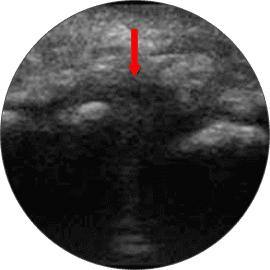
The combination of the physical examination, medical history and ultrasonography provide a complete picture of the actual condition.
If a neuroma is present, there will be pain at the area of palpation at the third and fourth metatarsals. If the clinician observes or palpates swelling around the painful area, this indicates a different condition. Physicians may also use standard tests for diagnostic purposes. For example, Tinel’s Sign test produces a sensation of pins and needles. Mulder’s Sign is performed with the patient in the supine position. The clinician compresses the foot bilaterally and presses directly on the suspected neuroma. If the pain appears directly on the point of contact, this test is positive. A neuroma can also be present if these tests are negative; however, these tests assist in the diagnosis.
Accuracy is essential for proper diagnosing and treatment planning. There are a variety of medical conditions that share similar symptoms, so other dysfunctions must be ruled out. Many of the conditions listed below involve nerve entrapments, inflammation or referral pain. The accuracy of every diagnosis involves determining the actual source of the problem. This can appear counter-intuitive in certain cases because the cause of the pain may be located distally from the presenting symptoms.
Common conditions that mimic this particular neuroma include:
This condition is more prevalent in women than men. Women over 50 who wear high heels face thehighest risk ofdeveloping this problem.
However, this neuroma is also present in young girls who practice ballet.
Intense involvement in high-impact sports can also lead to this condition, and this risk factoraffects allgenders equally.
However, any athletic sport that requires tight-fitting footwear can contribute to the development of the neuroma. Examples include ice hockey, skiing, ice skating and running in narrow shoes. Individuals who have pre-existing conditions may be predisposed to developing the condition. People who experience an unusually high rate of this condition are people with existing foot deformations. Examples include individuals who have bunions, collapsed arches, hammer toes and corns.
The professionals at our clinic strongly believe in customized treatment plans for patients. We are proud to recommend only the protocols that address your actual problems while considering your unique medical history. We encourage every patient to provide a detailed list of all previous treatment attempts. We can offer an appropriate course of action after we fully understand what you have already tried. Failed attempts can be helpful in designing a customized treatment protocol for your needs. This will often involve several disciplines, and we combine the best therapies according to the best practices in healthcare.

In order to individualize a treatment for Morton’s neuroma we perform gait and pressure analysis in which deviation of COP ( center of pressure) allows us to find a window for biomechanical intervention where we can unload the narrowed and collapsed arch that compresses the interdigital nerve.

We use specific gait correctional therapeutic exercises together with arch supports.To decrease inflammation and regenerate the affected interdigital nerve we use low energy focused extracorporeal shockwave. In our experience 85% of patients with Morton’s neuroma can be saved from the surgery.Te surgical excision of the neuroma ha frequent consequences which often times are irreversible, therefore we recommend that every patient tries conservative care first. Be ware that general physical therapy with massage, ultrasound, electrotherapy and foot strengthening exercises is totally useless.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: