During sports and high intensity physical activities, the hip and pelvic region mediates the transfer of enormous force loads between the upper and lower body. When forces exceed the integrity of the muscles, tendons, ligaments and bony structures, tissues can become ruptured, bones and joints can become fractured, and nerves can become entrapped, causing instability and reduced mobility. Accurately diagnosing the underlying cause of hip and groin pain is key to treatment and recovery.
or
Dr. Kalika has dedicated his entire career to revolutionizing the way injuries and pain syndromes are diagnosed and treated. By embracing advanced technologies and unique therapeutic approaches, he has transformed the realms of chiropractic and physical therapy, offering patients alternative solutions to run-of-the-mill hip and groin pain treatment that really work.
As a seasoned and certified practitioner of diagnostic ultrasonography, Dr. Kalika’s expertise has been a game-changer for thousands of patients over the past 15 years. Elite athletes, runners and ballet dancers from across the US frequent the NYDNRehab clinic for motion analysis, injury rehab and performance enhancement.
Physical therapy is a valuable and effective approach to resolving musculoskeletal pain and dysfunction, but in many cases, physical therapy does not provide a stand-alone solution. Prior to beginning physical therapy, patients often need to address underlying issues that contribute to their pain and disability.
Unfortunately, mainstream physical therapy clinics are often not adequately equipped or experienced to identify and treat complications that undermine the effectiveness of physical therapy. They often rely on one-size-fits-all treatment protocols that overlook the unique characteristics of the individual condition, opting to treat the symptoms and not the patient.
Identifying and treating underlying issues prior to beginning physical therapy is key to getting fast and effective results. Failure to do so can completely undermine your treatment protocol, and in some cases, your condition may even worsen.
At NYDNRehab, we use a broad range of advanced technologies and innovative therapeutic approaches to resolve issues that can potentially undermine the success of physical therapy.
Our talented staff is certified in a diverse array of treatment methodologies, rarely found in run-of-the-mill physical therapy clinics. Our one-on-one sessions are personalized, based on the patient’s unique diagnostic profile.
If you are a physically active person, you don’t want to take months away from your sport or activities to heal from pain and injuries. You want to fully recover as quickly as possible so you can get back to doing the things you love.
The sports medicine specialists at NYDNRehab understand your need to get back in the game in record time. They also understand that every patient is unique, and every injury has its own distinct characteristics. Run-of-the-mill therapy clinics often use a cookie-cutter approach to patient care, prescribing the same cookie-cutter treatment protocols to patients, based on the location of pain and injury.

Intermittent pain in the hip and groin region that comes and goes
Sharp pain in the groin during certain movements
A dull persistent ache in the groin or hip while at rest
Stiffness and reduced range of motion
Difficulty climbing stairs
Reduced muscle strength in the hip and pelvic region
Loss of balance on the affected leg
Change in gait (limping)
Tendinitis or tendon rupture
Muscle strains and sprains
Hip bursitis
Tearing of the hip socket labrum
Sacroiliac joint injury
Piriformis syndrome
Sciatic nerve impingement or entrapment
Sports that require rapid cutting or pivoting, like basketball, tennis and soccer
Repetitive overuse from exercise
Activities on uneven terrain
Excessive sitting
Being out of shape
Obesity
Low bone mineral density

The hip and pelvic complex houses numerous structures, systems and vital organs, any of which can contribute to hip and groin pain. For that reason, diagnosing the exact cause of your hip and groin pain can be challenging. Without sophisticated diagnostic equipment operated by an experienced specialist, it is easy to misdiagnose hip and groin pain, making treatment a total waste of time and prolonging the patient’s discomfort.
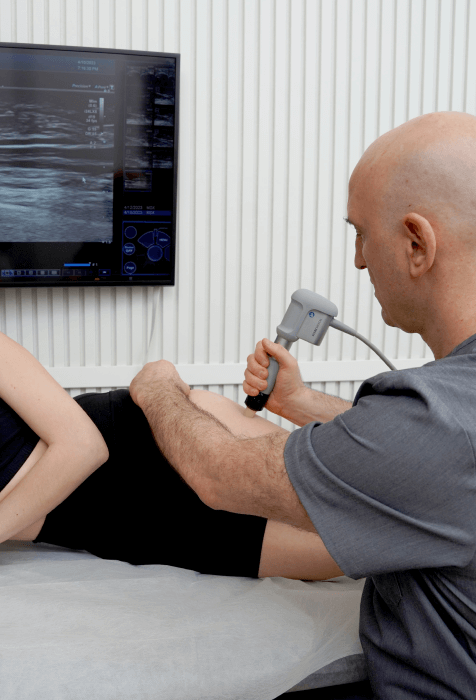
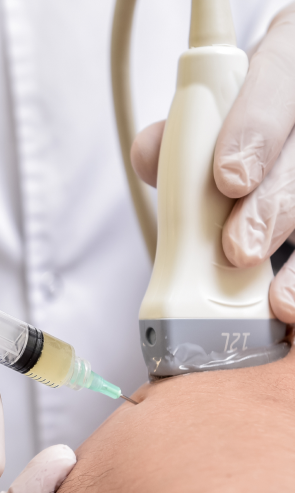
At NYDNRehab, we use the most advanced and accurate diagnostic ultrasound equipment available. Ultrasound lets us visualize the structures of the hip and pelvic region in real time, with the patient in motion.
In addition, we use our groundbreaking motion analysis technology and high resolution diagnostic ultrasonography to run a battery of tests that perfectly reveal the dynamic functional pathology of the hip and pelvic region. Our tests are evidence-based protocols, considered to be gold standards in the world of research. Integrative motion analysis allows our hip and groin physical therapy to achieve fast and long-lasting results.
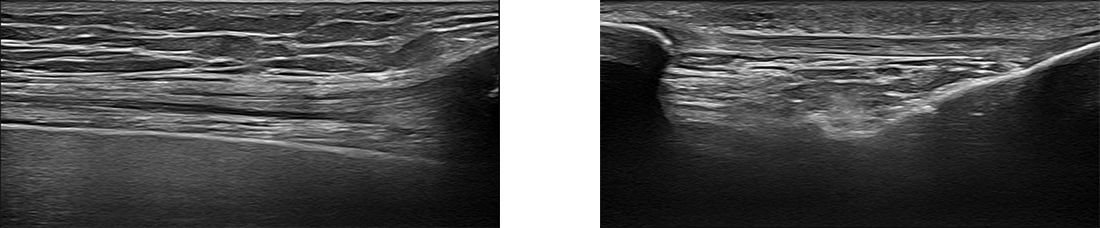
Please explore more advanced diagnostic option unavailable anywhere else:
Our proprietary battery
of tests includes
DLEST hip stability test using C.A.R.E.N, our computer assisted rehab environment
3D star excursion banner test (SEBT) for assessing the role of hip muscles in postural stability
3D walking and/or running gait analysis
3D kinematic joint angle analysis during squats, lunges, drop jumps and pelvis-on-hip rotation
Rehabilitative ultrasonography to view activation patterns of the hip stabilizer muscles
Regenerative pulse therapies work together with your body’s own innate healing mechanisms to stimulate the progenesis of new cells. Structural damage to the muscles, tendons, ligaments, fascia, nerves and bones cannot be reversed with physical therapy alone, and patients can sometimes undergo months of physical therapy without relieving pain.
Once degenerative changes occur in your hip and pelvic region, or chronic inflammation sets in, your body may need extra help to halt and reverse the degenerative cascade. Regenerative pulse therapies and ultrasound guided dry needling and injections may be used to accelerate the healing process.
Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels.
Our INDIBA Tecar therapy machine converts electrical current into a stable radio frequency current of 448 kHz, designed to increase and stabilize the exchange of ions in damaged cells, evoking a regenerative response that accelerates healing. INDIBA can be used to successfully treat joint and muscle disorders, low-back pain, sports injuries, surgical incisions and various pain syndromes. Another therapeutic effect of INDIBA is extreme and prolonged cellular hyperthermia. Due to this effect, INDIBA therapy combined with manual therapy and soft tissue tissue manipulation enables instantaneous release to occur, significantly shortening the number and duration of physical therapy sessions. What is normally accomplished in two months of physical therapy can be accomplished in 3-4 sessions with INDIBA.

Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
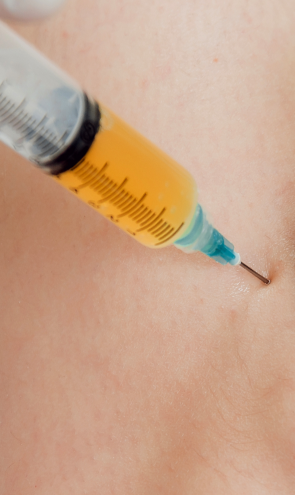
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.
Sometimes hip and groin injuries are beyond your control, but there are many proactive measures you can take to reduce your risk of pain and injury:
Ignoring your hip and groin pain can cause it to get worse, increasing your risk of serious injury and diminishing your quality of life. Accurate diagnosis, cutting-edge technologies and innovative treatment methods can help to accelerate healing and ensure that the strength, range of motion and function of your hip and pelvic region are fully restored.
If you want fast and effective treatment for your hip and groin pain that really works, contact NYDNRehab today, and see what a difference technology makes in hip and groin physical therapy in NYC.
Hip pain is a very a frequent musculoskeletal complaint that affects all age groups. Most frequently it occurs due to structural and functional misalignments in the hip joint itself or in combination with neighboring articular structures suffering from compensatory overuse, muscle strains, tendinosis, hip bursitis, femoral acetabular impingement (FAI), labrum tears and finally damage to the hip joint cartilage.
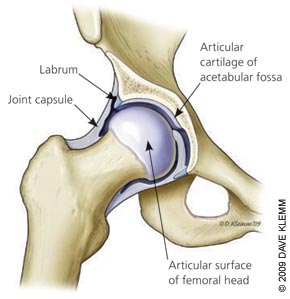
Hip joint is the deepest and the biggest joint in the human body. The increased depth of this joint in combination with its perfectly round shape provides most stability while allowing great degree of mobility in multiple directions and in different planes simultaneously.
This joint is second to shoulder joint in its versatility and motion complexity. Just like the shoulder joint, the hip joint is, in evolutionary terms, the newest structure of the body and developed to accommodate the need for vertical locomotion. Joints versatile mobility is what makes it so susceptible to injuries of its extra-articular structures (ligaments, tendons, muscles and fascial tissue).
Joint is frequently affected later in life due to the structural misalignments occurring at the early stage of life because of the abnormal bone formation. These are not so infrequent as the scientific community thought before.
In adult stages of life hip misalignment usually occurs due to ever increasing demand for the weight bearing stability. Also many sporting and fitness activities cause hip joint pain by nature of excessive movement produces through the hip joint. Most frequently it occurs in: soccer, hockey, figure skating, martial arts, ballet and yoga.
It has been recently established that even a little misalignment or any deviation of the anatomical structure of the joint can lead to the development of the degenerative hip disease.
The following is a list of the predisposing factors:
Even though, radiological examination of the hip joint is used to confirm the diagnosis of degenerative joint disease, it cannot predict or define the degree of dysfunction or pain with which the patient is affected. For example, radiological examination in-patient without symptoms may discover moderate to severe degree of degeneration, while patients with minimal degenerative changes in the joint can be in extreme pain and disability. Therefore, the relationship of degree of degeneration to degree of disability is not predictable. This is due to multiple extrarticular and regional factor involved in hip pain syndromes.
Due to unique anatomical shape of the hip joint and its proximity to other joints of the lumbopelvic region, its movement dysfunction is initially well compensated by the structures located above and below the ailing area. This compensatory freedom of movement in the state of the dysfunction is notable however by the excessive movement (hypermobility). The joint might stay unaffected for a long time under these conditions until stresses created by inefficient repetitive hypermobility build up, eventually compromising the stability of the entire lumbopelvic region.
Another reason for the hip joint pain syndrome symptomatology delay is because stiffness of the dysfunctional hip joint elements and tissues is greater than the stiffness of the knee and the lumbopelvic joints. In the compensatory effort, the main burden of the hip movement is transferred to the less-affected articular structures of the region. This brings loading and shearing forces exerted by powerful contractions of long levered muscles of the upper leg to the knee and lumbo-pelvic joints.
And for these forces neither the knee nor lumbo-pelvic joints have been designed. Consequently tremendous new stresses exerted on the compensating structures will wear them out first. Therefore the dysfunction of the hip joint will initially cause pain in the neighboring joints long before the joint itself shows any pathology symptoms.
This is exactly why so many problems are discovered only when pain appears. Unfortunately, when that is the case, radiological images of the joint already show some degree of degeneration (hip arthrosis), which usually means eventual hip replacement.
The risk factors of developing chronic hip pain are divided into local and systemic .The local factors are: sports specific activity, trauma, occupation, surgery and obesity while the systemic risk factors are: age, gender, ethnicity, nutrition, anatomical variations and systemic diseases. Women, not only have a possibility to develop OA more often than men, but also with a more severe form ( Srikanth et al, 2015) .
With advancements in radiological, arthroscopic and functional clinical examination methodology of the hip, a new model of the joint disease has been established. This model enables doctors and practitioners to diagnose hip joint pain and dysfunction at a very early stage. The early diagnosis allows commencing the treatment at the stage when hip joint degeneration has not yet set in and is therefore reversible. For those patients who already have developed some early signs of degeneration, further progression can be arrested or significantly slowed down. Unfortunately, this recent scientific development, has not reached the majority of clinicians or therapists yet.
The most distinct early sign of the hip joint dysfunction is not the pain but the abnormal movement in the joint area. Unfortunately you cannot see movement abnormality on X-ray or any other radiological examination. Abnormality can manifest itself in the variety of ways. This movement could be limited, excessive or imprecise. The patient however rarely notices these developments, as the compensation will be provided by other articular structures in the lumbo-pelvic region.Hip joint pain may occur in seemingly unrelated areas causing patients to look for medical advice. Unfortunately the vast majority of the doctors rely solely on the MRI and other imaging diagnostic procedures and movement examination of the hip joint is rarely, if ever, conducted on the patient complaining, for example, of the low back pain.
Another very frequent complaint is pain radiating down the thigh known as sciatica. In almost every case of the true sciatica it is the abnormal movement of the joint that either is the cause or one of the causes of the shooting pain down the leg.
True hip joint pain and pain in the groin area:
We maintain that successful hip pain treatment depends on the diagnostic precision.
Because of the limited ability of medical imaging to reveal all causes of the joint problem, we conduct computerized Gait (walking) analysis with highly advanced technological equipment. Our Gait (walking) analysis Lab is the first outpatient facility in NYC providing these types of services. The various data acquired through Gait analysis allows very precise diagnosis of movement pattern dysfunction in the hip joint and pelvis. Rehabilitation to address abnormal movement patterns and muscle weakness may help to restore joint precision and dynamic stability, reduce excessive stresses, and allow healing of injured tissues.( Marcie Harris-Hayes et al, 2016)
We use diagnostic ultrasonography and X-ray imagery to analyze the integrity of the tissues around the hip joint as well as to rule out bone anomalies and anatomical misalignments. If, however, these procedures fail to explain patients symptoms we may opt to ordering the MRI or CT scan study.
The most precise imaging diagnosis of early hip disease at this time is CT-scan. However, the specific CT-scan has an enormous dose of radiation. It should not be used initially, unless surgery is considered. The newest ultrasonography methods of diagnosis combined with X-ray and MRI and good clinical examination should be sufficient to establish proper diagnosis and treatment plan.
Based on Gait analysis data and clinical examination our pain treatment focuses on elimination of the faulty movements and rebuilding strength and coordination of the hip, lumbo-pelvic area . We also use some of our Gait lab equipment for feedback training of precise hip movement. We
use combination of DNS method, Shirley Saharmann method, Chris Power’s hip strategy method as well as video and force plates’ feed-back training. Our extensive rehabilitation program integrates the aforementioned methods with various manual techniques. If the integrity of the tendons or the muscle tissues is affected, we combine our rehabilitation protocols with biological treatment. Extracorporeal shockwave therapy is used to regenerate damaged tendons and muscles. Frequently hip problems arise due to asymmetrical weight bearing. Our C.A.R.E.N (computer assisted rehabilitation environment) therapy is breakthrough rehabilitation technology available for the first time in NYC (please review our slide presentation) is able to detect this with its innovative force plate and motion capture analysis. The feedback/feed forward treatment by C.A.R.E.N is most unique in the field of modern rehabilitation. Please check out our pages for the C.A.R.E.N (computer assisted rehabilitation environment), running gait lab, the alter-g treadmill, and shockwave therapy to see how these technologies can help you.
Our extensive rehabilitation program integrates the aforementioned methods with various manual techniques. If the integrity of the tendons or the muscle tissues is affected, we combine our rehabilitation protocols with biological regenerative treatment such as ESWT( Extracorporeal shockwave therapy ).
ESWT is used to regenerate damaged tendons and muscles.
 Dr. Yuri Brosgol
MD
Dr. Yuri Brosgol
MD
 Dr. Michael Goynatsky
DPT
Dr. Michael Goynatsky
DPT
 Dr. Daniela Escudero
DPT
Dr. Daniela Escudero
DPT
 Dr. Michelle Agyakwah
DC
Dr. Michelle Agyakwah
DC
 Dr. Tatyana Kapustina
L. Ac.
Dr. Tatyana Kapustina
L. Ac.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including:Independent peer-reviewed research relevant to this treatment approach.