
Orthobiologic, Sports Medicine and Regenerative Medicine Specialist

Sedentary lifestyle and excessive sitting
Being overweight or obese
Weak core and pelvic muscles
Weak and imbalanced spinal stabilizers
Fascial dysfunction
Poor posture
Deficits in gait mechanics
Inefficient lifting technique
Repetitive overuse from sports, exercise or occupation
Old injuries that were never properly rehabilitated
It is commonly thought that low back pain begins in the spine, but in reality, while symptoms are felt in the lower spine, the problem often starts elsewhere. Unlike conventional medical doctors who focus on treating the spine itself, holistic practitioners seek to identify and correct the causes of low back pain, with the goal of restoring pain-free mobility.
The lumbar spine and pelvis are primary sites of load transfer between the upper and lower body, and the spine houses sensitive neural bodies that respond to movement, posture, and mechanical stress. Inefficient gait mechanics, poor load distribution, fascial restrictions, and nerve irritation often originate in the lower kinetic chain, with the lower back absorbing the consequences.
Treatment centered on the spine may provide temporary pain relief, but the symptoms are likely to return if other issues are not addressed. Our integrative approach takes into account biomechanical factors, lifestyle behaviors, inefficient motor strategies, and postural habits. By identifying multiple factors that contribute to the patient’s low back pain, we can design a customized plan to treat and correct them, without drugs or surgery.
Benefits of holistic vs conventional LBP treatment include:

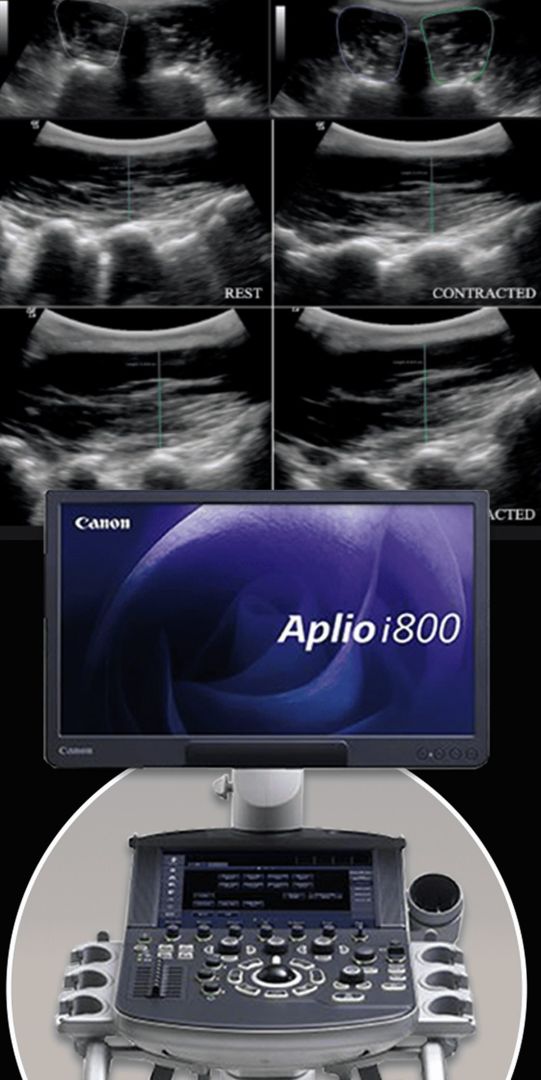
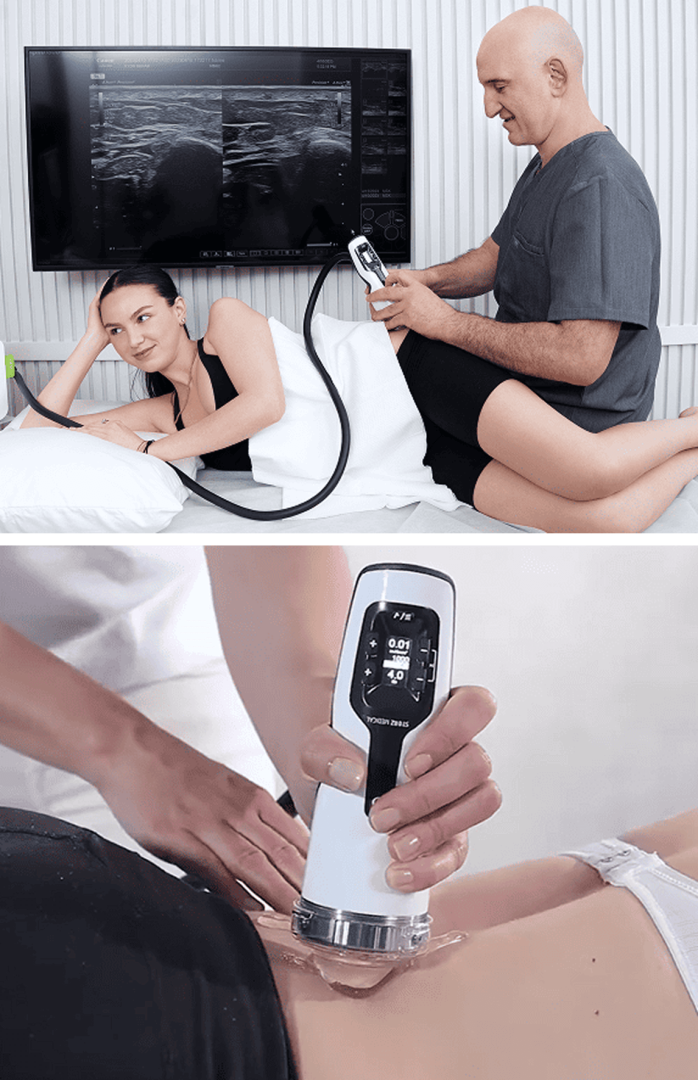
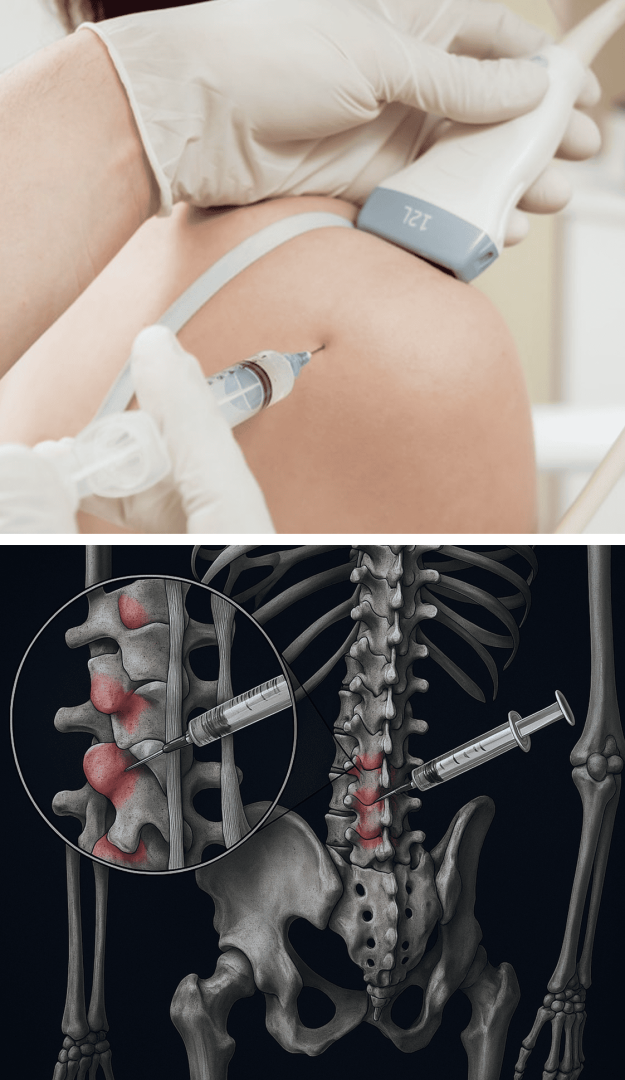
At NYDNRehab, we guide our Prolotherapy procedures with high-resolution ultrasound, to ensure the solution precisely reaches its target. Injections performed without imaging often miss their mark, and can bleed into adjacent tissues, reducing their efficacy. When combined, Prolotherapy and ESWT can dramatically reduce low back pain and set the patient up for physical therapy success.

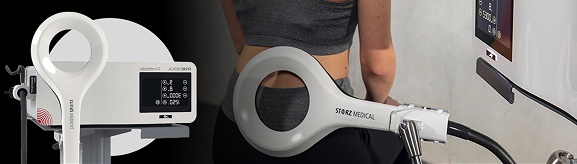


When delivered at the most effective levels under ultrasound guidance, ESWT + EMTT prime the microenvironment via mechanical and electromagnetic stimulation. TECAR + Laser therapy optimizes tissue metabolism, circulation, and cellular energy. Together, they extend and amplify the biological effects of PRP and stem cells, accelerating tissue integration, repair, and functional recovery.
In addition, when used post-procedure, regenerative therapies dramatically reduce pain and discomfort, reinforce soft tissue healing, and promote collagen fiber realignment.
Despite the effectiveness of these cutting-edge therapies, without a multifaceted approach that addresses not only symptoms and tissue healing, but also causative and biomechanical factors, the patient is unlikely to restore and maintain efficient pain-free mobility over the long term. At NYDNRehab, our goal is to not only address symptoms and heal tissues, but to optimize mobility and prevent future injuries.
The lower back is supported by strong ligaments, muscles, and fascia that hold the spine in alignment, control movement, and distribute forces. Healthy, fascia is smooth, slippery and elastic, enabling muscles, nerves and blood vessels to glide among other structures. But damaged fascia can become dense and sticky, inhibiting coordinated movement, and compressing nerves, which generates pain signals.
The Stecco technique of fascial manipulation targets densified fascial layers, helping to restore their gliding and elastic properties. Stecco Fascial Manipulation is a highly systematic approach that requires specific training. When applied correctly, Stecco not only restores tissue gliding – it reactivates sensory receptors within the fascia, recalibrating the neuromuscular system and restoring efficient motor control.
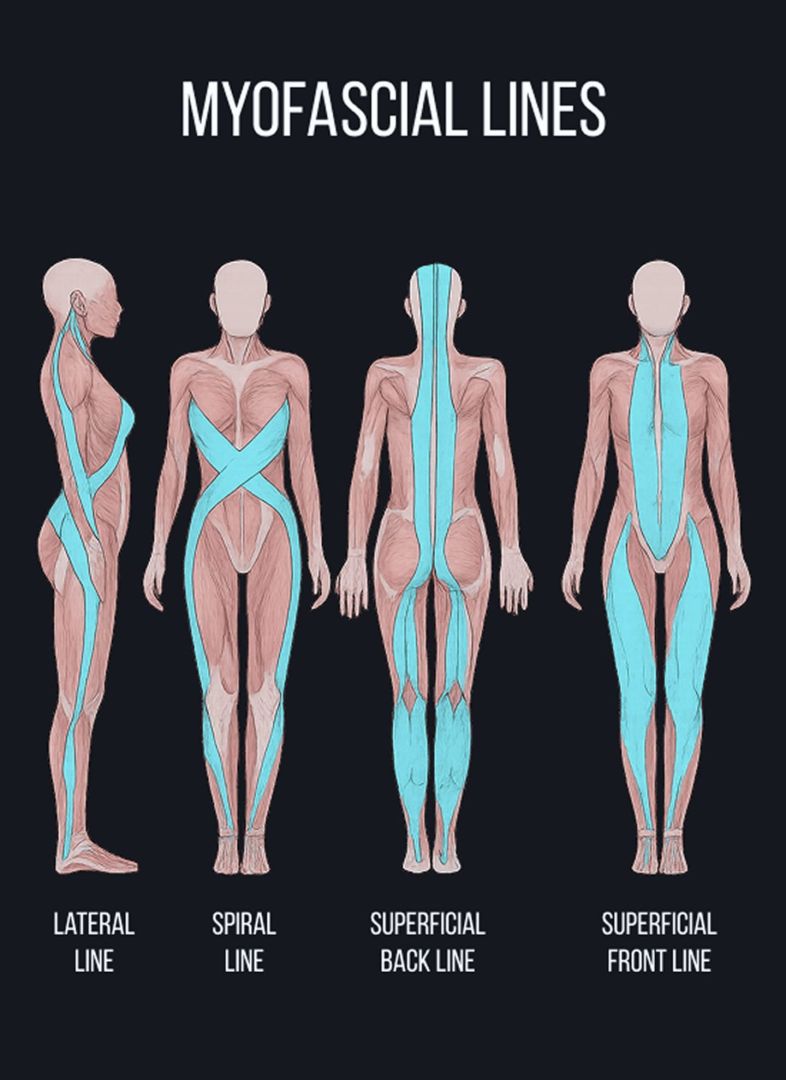
Progression of Stecco Fascial Manipulation involves:
This advanced methodology works to alleviate lower back pain, eliminate restricted movement, enhance physical performance, and optimize whole-body mobility and stability. Dr. Kalika has received advanced training in the Stecco Method directly from its creator, Dr. Carla Stecco, the world’s leading specialist in fascial science.
All human movement affects and is affected by the spine, and good spinal alignment is fundamental to overall health. Holistic physical therapy for low back pain seeks to optimize spinal mobility and stability by addressing factors that disrupt alignment, compress nerves, and alter muscle recruitment patterns.
Prior to beginning physical therapy, we pre-treat your tissues to reduce pain and inflammation and promote healing. It is not uncommon for medical doctors to recommend physical therapy after managing pain with medications, but that approach can do more harm than good if the tissues remain damaged. At NYDNRehab, we make sure the structures surrounding and supporting your lower back are ready to handle loads, without pain or risk of injury.
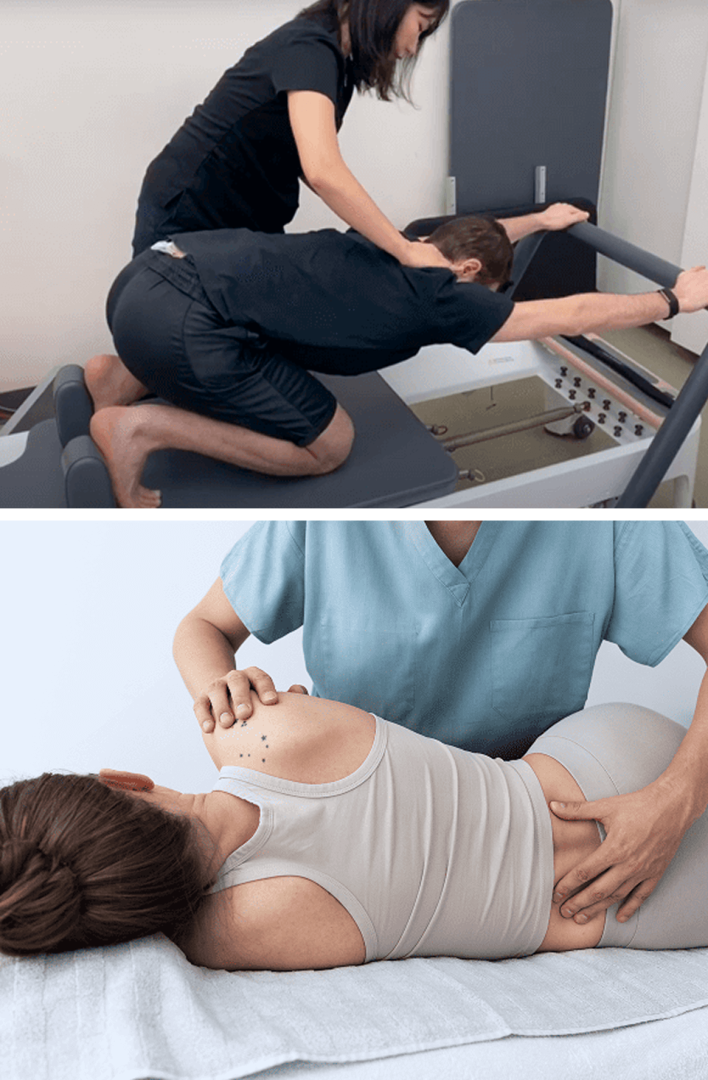

Mainstream approaches to back pain treatment often involve pain medications, muscle relaxants, steroid injections, and admonishments to “take it easy.” When those methods fail to alleviate pain and dysfunction, surgery is often the next step. However, research shows that conservative care can be just as effective as surgery, without the risk and expense of unnecessary invasive procedures.
At NYDNRehab, we work with you to resolve the underlying causes of lower back pain. Our personalized one-on-one approach ensures that you get the very best treatment for your unique condition. If you are ready to eliminate lower back pain for good, contact us today, and get back to doing the things you love.
These case studies reflect real clinical conditions evaluated at NYDNRehab using advanced diagnostic methods and individualized rehabilitation strategies. All cases are evaluated and managed by Dr. Lev Kalika and the NYDNRehab clinical team.
Traditional approaches to back pain treatment often involve pain medications, muscle relaxants, steroid injections, and admonishments to “take it easy.” When those methods fail to alleviate pain and dysfunction, surgery is often the next step. However, research shows that conservative care is at least as effective as surgery, without the risk and expense of unnecessary invasive procedures.
At NYDNRehab, we work with you to resolve the underlying causes of lower back pain. Our personalized one-on-one approach ensures that you get the very best treatment for your unique condition. If you are ready to eliminate lower back pain for good, schedule a consultation with our lower back pain specialists today, and get back to doing the things you love, pain-free!
 Dr. Yuri Brosgol
MD
Dr. Yuri Brosgol
MD
 Dr. Michael Goynatsky
DPT
Dr. Michael Goynatsky
DPT
 Dr. Daniela Escudero
DPT
Dr. Daniela Escudero
DPT
 Dr. Michelle Agyakwah
DC
Dr. Michelle Agyakwah
DC
 Dr. Tatyana Kapustina
L. Ac.
Dr. Tatyana Kapustina
L. Ac.
Independent peer-reviewed research relevant to this treatment approach.
Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.