Your entire body operates via a complex network of nervous tissues that extend to the farthest reaches of your extremities. Your neural network serves to deliver and receive messages via electrical impulses between the peripheral nerves and the central nervous system of the brain. Without continual nervous impulses, your body would quickly shut down
Peripheral neuropathy is any condition that causes damage or dysfunction to the peripheral nerves — neural bodies that extend beyond the spinal cord. Peripheral nerves provide sensory information about the body’s position relative to gravity, the temperature of the environment and various surfaces, and sensations of pain or discomfort. They also carry messages from the brain to muscles, to tell them when, how quickly and how forcefully to contract, along with signals that regulate metabolism, digestion, circulation and more.
When peripheral nerves become damaged or compressed, they may send faulty information to the brain, or they may misinterpret directives from the brain. The goal of peripheral neuropathy treatment is to repair damaged nerve tissues and restore healthy channels of communication between the brain and body.
or
As a holistic practitioner of rehabilitative medicine, Dr. Kalika has devoted his life’s work to better understanding the intricate and interdependent nature of the body’s structures. Dr. Kalika specializes in nerve disorders that affect human movement and cause pain, using a broad array of evidence-based approaches, including:
Dr. Kalika has developed his own methodology for treating nerve disorders, combining various advanced approaches with neurodynamic physical therapy.
Dr. Kalika is a world expert in high resolution ultrasonography, with multiple peer-reviewed studies to his credit. He is currently collaborating on a book chapter about conservative treatment of peripheral mononeuropathies.
Getting effective treatment that delivers long-term results is the goal of every patient suffering from neuropathy. Medical doctors often look for pharmacological remedies that treat the symptoms of neuropathy without addressing its underlying causes. However, all medications have undesirable side effects, and many people do not want to be dependent on drugs long-term to control their symptoms.
Most neurologists only order electro-diagnostic tests, and if the diagnosis is a small fiber neuropathy, they tell you there is no treatment available. At NYDNRehab, we use new advanced technologies to detect neuropathies and treat them, to reduce pain symptoms and improve nerve function, without drugs or surgery.
The anatomy of nerve compression is unique to each nerve and its compartment. Nerves can become entrapped, stretched or compressed in the fascial tunnel, the myofascial tunnel, or the osteo-fibrous tunnel. Nerves glide with fascia in the spaces between muscles, and they also run within muscles, and next to bones. Before we treat a nerve with a procedure like hydrodissection, we need to address the surrounding fascia, muscles and joints.
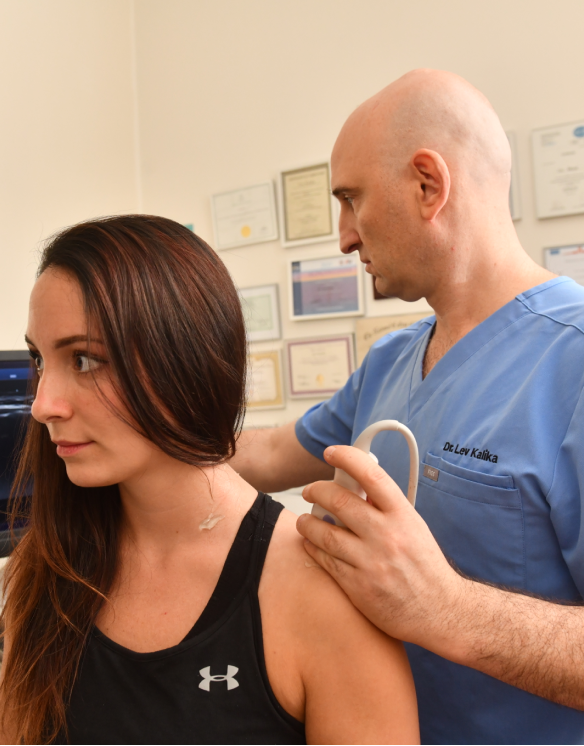
We treat compression syndromes of peripheral nerves in your arms, legs, hips, shoulders, spine and brachial plexus, along with mononeuropathies (pinched nerves) such as cubital tunnel, radial tunnel, carpal tunnel and tarsal tunnel syndromes, and median nerve entrapment in the pronator teres. We also treat the following nerves:
Axillary nerve
Musculocutaneous nerve
Suprascapular nerve
Dorsal scapular nerve
Long thoracic nerve
Thoracodorsal nerve
Spinal accessory nerve
Lateral pectoral nerve
Radial nerve
Ulnar nerve
Median nerve
Cluneal nerve
Sciatic nerve
Posterior and anterior femoral cutaneous nerves
Superior gluteal nerve
Peroneal nerve
Tibial nerve, and its heel and foot branches
In addition, we treat diabetic neuropathy, a condition that arises when blood vessels that feed peripheral nerves are damaged from high circulating glucose levels, depriving nerve tissue of oxygen and nutrients. We also treat post-radiation neuropathy that often develops in cancer survivors, sometimes appearing several years after radiation therapy.
Dr. Kalika uses a holistic and individual approach that addresses all components of nerve compression, entrapment and tension. Once we identify the type of neuritis, we are able to create a personalized treatment plan geared to restoring healthy functional neural pathways.
Our personalized one-on-one approach sets us apart from other clinics that rely on generalized protocols that treat the symptoms, not the patient. For lasting results without drugs or surgery, NYDNRehab is your clinic of choice for peripheral neuropathy rehabilitation in NYC.
Scientists have identified over 100 types of peripheral neuropathy, and symptoms can vary widely, depending on the type of nerves affected. There are three subcategories of peripheral nerves:
Motor nerves stimulate muscle contraction to produce movement. Symptoms of peripheral motor nerve damage include:
Muscle weakness
Muscle tingling or numbness
Muscle cramps
Muscle spasms
Muscle atrophy (shrinkage)
Sensory nerves transmit information about touch, temperature, pain and other sensations from the periphery to the brain. Symptoms of sensory nerve damage include:
Reduced or exaggerated sensitivity to touch or environment
Reduced balance or coordination
Loss of reflexes
Autonomic nerves control involuntary body processes such as breathing, digestion, circulation and gland and organ function. Symptoms of peripheral autonomic neuropathy include:
Excessive sweating
Heat intolerance
Inability to regulate blood pressure
Gastro-intestinal issues
Complex regional pain syndrome
Causes of peripheral neuropathy are as diverse as its symptoms. Some of the most common causes include:
Physical trauma that damages or disrupts nerves
Local or systemic infections
Diabetes
Smoking
Cardiovascular disease
Autoimmune disorders
Hormonal imbalances
Malnutrition
Kidney and liver disorders
Certain medications and cancer treatments
As is the case with many musculoskeletal disorders and pain syndromes, peripheral neuropathy often has its roots in unhealthy lifestyle behaviors and/or exposure to environmental toxins.
In addition to a comprehensive medical history and physical exam, there are a number of tests that can be conducted to identify peripheral neuropathy, depending on nerve type.
Muscle strength and function tests
Electromyography (EMG) tests
Nerve conduction tests
Blood tests
Tests using ultrasound imaging
Once we understand the nature and extent of your nerve damage, we create a personalized treatment protocol based on your results.
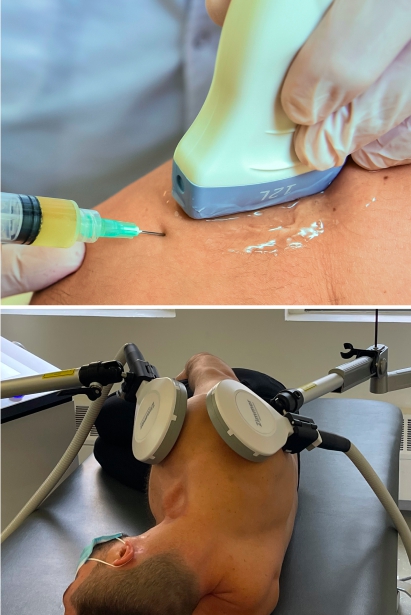
Neurodynamic physical therapy is generally a part of peripheral neuropathy rehabilitation, but prior to beginning physical therapy, we need to address other issues that interfere with nervous function. Your peripheral neuropathy therapy may include:

NESA delivers a biphasic low-frequency electrical current via semi-electrodes attached to the hands and feet. It emits a series of intermittent and cyclical stimuli that travel through autonomic neural pathways, restoring optimal neural signaling to the CNS.
INDIBA therapy is a type of transfer of energy capacitive and resistive (TECAR) therapy that helps to restore the ionic charge of damaged cells, for faster injury healing and rehabilitation.

When guided by high resolution ultrasound imaging, focused extracorporeal shockwave therapy (ESWT) is an evidence-based therapeutic approach to treating nerve entrapments, peripheral neuropathy and neuralgia.
Dr. Kalika is an expert in neural ultrasonography and extracorporeal shockwave therapy. The clinic at NYDNRehab features the highest-resolution research-grade ultrasound equipment currently available.
Ultrasound guided ESWT provokes the following effects in neural tissue:
Improved axonal transport
Provokes axonal regeneration
Promotes reinnervation
Limits and slows muscle atrophy associated with peripheral neuropathy
Accelerates remyelination
Modulates neurogenic inflammation
Improves intraneural vascularisation
The effects of ESWT are achieved via the following mechanisms:
Stem cell proliferation
Mediation of Schwann cell function
Endothelial cell recruitment/migration
Regulation of pro- and anti-inflammatory cytokines
Voltage-gated sodium channel blocking
Staying active and making healthy lifestyle choices is the best way to avoid developing peripheral neuropathy. You can make many positive changes right away that keep all your body’s systems running smoothly, including your nervous system.
Exercise daily — walking is the best exercise for most people
Stretch your joints and muscles daily
Get 7-8 hours of sleep nightly
Drink plenty of plain filtered water
Avoid processed, fast and fried foods
Eat a variety of organic fruits and vegetables
Stay away from sugary foods and beverages, and baked goods
Eat organic pasture-raised meats and wild caught fish
Take frequent breaks from sitting
Don’t smoke
Avoid excessive alcohol use
Minimize drug use (over-the-counter, prescription and street)

If you are ready to go beyond treating your peripheral neuropathy symptoms and want to find a solution that restores neural function, you need an experienced peripheral neuropathy specialist who has access to the latest treatment technologies. Dr. Kalika’s holistic patient-first approach ensures that you get the exact treatment you need for fast and effective results. Contact NYDNRehab today, and see why we are the best clinic for peripheral neuropathy recovery in NYC.
February 19, 2026
We specialize in treatment of compression and entrapment neuropathies.
The diagnosis of compression/entrapment neuropathies is made by nerve conduction studies and diagnostic ultrasound. We take a three step process to inquire about your condition.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including:Independent peer-reviewed research relevant to this treatment approach.