Your lower spine is made up of a series of interconnected joints that house the sciatic nerve roots as they branch out to innervate your lower body. When your spine or pelvis is out of alignment, or when nerve roots become entrapped, even breathing can cause mild to moderate back pain. If you feel pain in your lower back when breathing deeply, there are certain things you can do to improve your alignment, release your sciatic nerve and alleviate pain.
Following are five reasons you feel pain in your back when breathing, and what you can do about it.
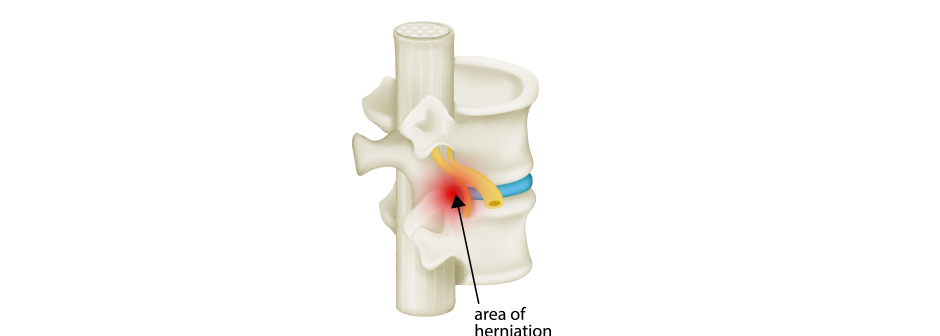
Because your spine is always in motion and load-bearing, the bones in your vertebra sometimes rub against the discs that separate them, causing them to become irritated and inflamed. A swollen (herniated) disc can bulge out between your vertebrae and put pressure on the nerve roots, causing pain.
When you breathe, the entire apparatus of your ribcage and spine goes into motion, increasing pressure on intervertebral discs and nerves. Icing your low back with a bag of frozen peas throughout the day can dramatically reduce inflammation, numb pain receptors and relieve pressure on your nerve roots. If pain persists, seek help from a chiropractor or physical therapist.
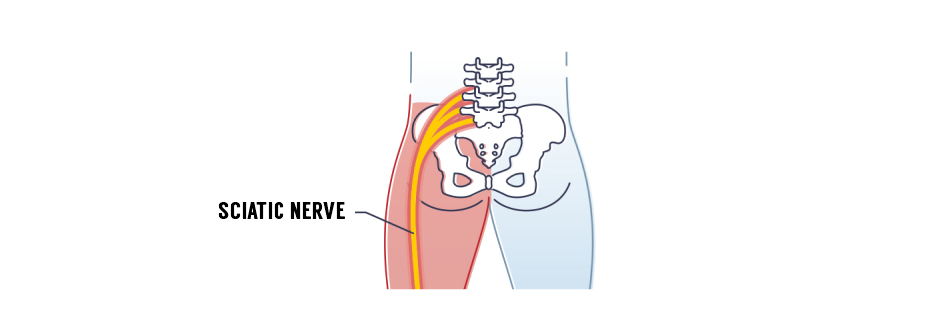
Your sciatic nerve is the longest and widest nerve in your body. Its nerve roots branch out from your lumbar vertebrae and converge as they travel from your low back, across your buttocks and down the backs of your legs, all the way to your feet.
The sciatic nerve can become entrapped anywhere along its pathway where it glides among other structures in your body. An entrapped nerve can be extremely painful, and deep breathing, coughing or sneezing can increase pressure at the point of entrapment. A physical therapist can teach you nerve flossing exercises that release the sciatic nerve and restore unrestricted gliding.
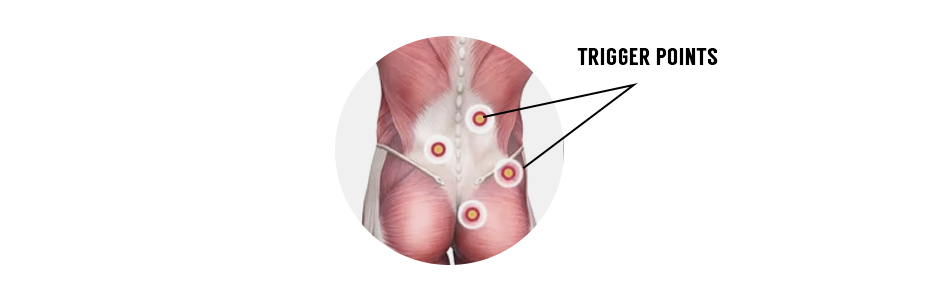
Trigger points are tight knots of muscle or fascia fibers that can cause pain and restrict movement. They often arise after intense activity like lifting heavy boxes or furniture, or after intense sports or exercise. Spinal movement as you breathe can make the pain more noticeable.
Trigger points can sometimes be felt as nodules just below the skin’s surface, and superficial trigger points can be successfully treated with myofascial massage. Deep trigger points occur in deep muscle tissue and cannot be palpated from the surface. Dry needling by a trained professional is an effective way to release deep trigger points, especially when done under ultrasound guidance, to ensure accurate targeting.
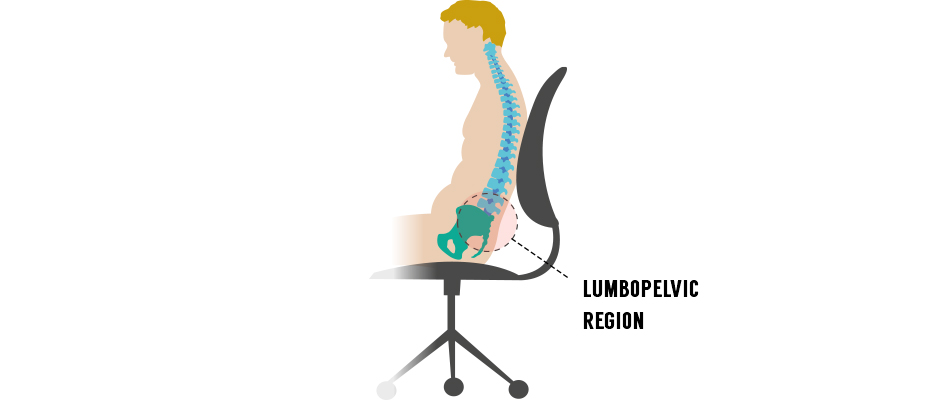
Being sedentary and sitting for long hours on end can cause the muscles that support your lumbopelvic region to become imbalanced, causing your lumbar vertebra to compress their intervertebral discs. Becoming physically active and working with a physical therapist can restore balanced muscle tension to your low back and pelvis, and relieve pressure on lumbar discs and nerve roots.
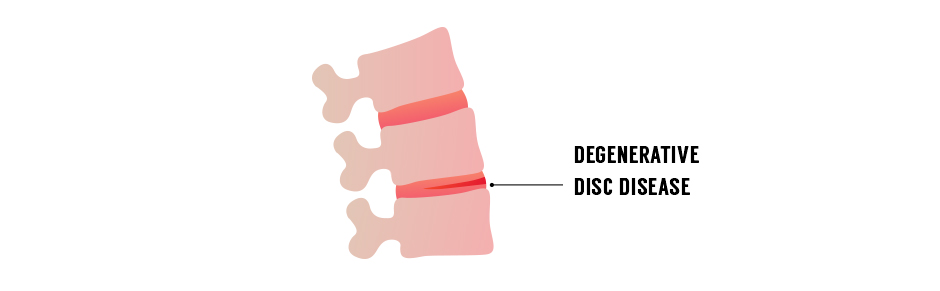
Sometimes the discs between your vertebrae can begin to deteriorate, reducing their shock absorbing ability and narrowing the distance between your vertebrae. That can cause the bones of the spine to rub against the nerve roots and irritate them, causing pain as the vertebrae move when you breathe. Regenerative therapies like focused shockwave therapy (ESWT) and electromagnetic transduction therapy (EMTT) can help to relieve pain and inflammation and slow and reverse the degenerative process.
Chronic low back pain is not normal, and you should never let it go untreated. Taking pain medications can mask the symptoms, but drugs do not get to the underlying cause of your problem, and they can be addictive and damage your liver.
Chiropractic care and physical therapy are your best bets for successful low back pain treatment. When combined, they can help you eliminate back pain for good. Look for a practitioner who uses advanced treatment methods like regenerative shockwave therapy and ultrasound guided dry needling.
For the best low back pain treatment in NYC without drugs or surgery, contact NYDNRehab in Manhattan.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: