
The Achilles tendon plays a key role in all types of physical activity, including walking and running gait, jumping and landing, and a broad range of sports movements. Acute and overuse injuries to the Achilles tendon can severely restrict your ability to move about and participate in sports. One treatment showing promise for accelerated healing of Achilles tendinopathy is extracorporeal shock wave therapy (ESWT).
Extracorporeal shock wave therapy was first invented in Germany as a tool for breaking up kidney stones. However, doctors soon discovered that ESWT could be an effective method for treating injured soft tissues like muscles and tendons. Shock wave therapy is a non-invasive and relatively painless method for treating tendinopathy, with extensive research to vouch for its efficacy. The procedure is quick and simple, with a track record of successful results.
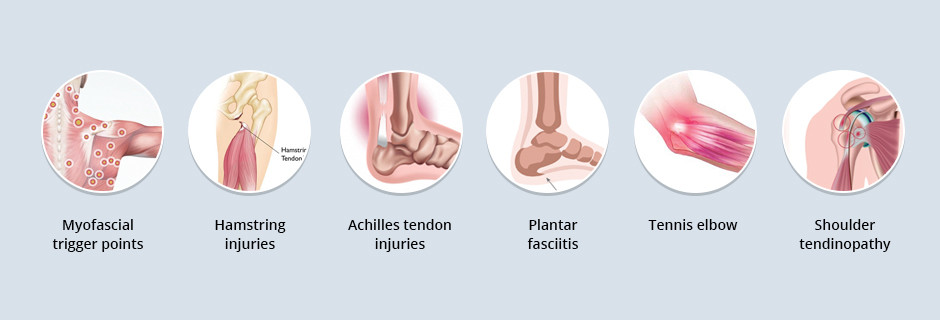
ESWT is useful for treating the following conditions:
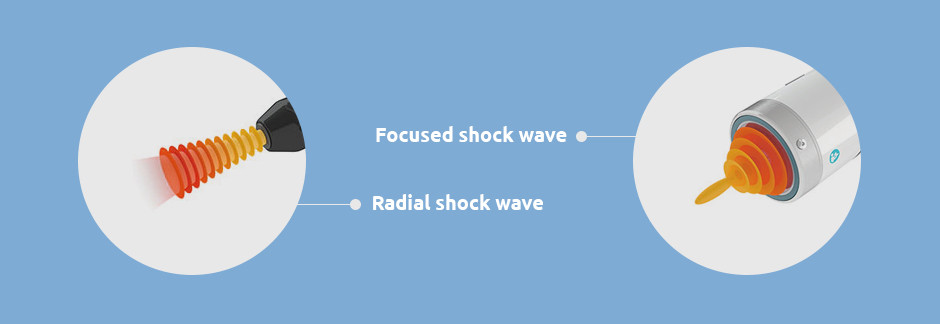
ESWT uses two types of shock waves. Radial shock waves are not true shock waves, but rather radial pressure waves that are generally too shallow and dispersed to penetrate deep tissues. Radial shock wave therapy is often not effective for treating tendon tissues that lie close to the bone (proximal tendinopathy).
Focused shock waves are able to penetrate up to 7 cm into the body, with focused energy that allows for precise soft tissue treatment. When used in conjunction with ultrasound guidance, focused shock waves can precisely target damaged tissues without impacting surrounding structures.
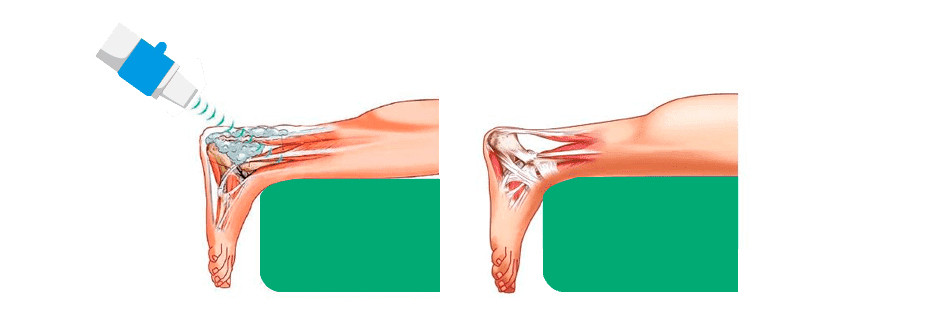
Tendon tissue has less blood supply than muscle, slowing the healing process for ruptured or damaged tendons. Shock wave therapy provides a wave of energy that penetrates tendons on the molecular, cellular, and tissue levels.
Focused ESWT evokes a reaction called neovascular regenesis, which is the growth of new blood vessels, in areas of the tendon that have little or no blood supply. Increased vascularity means that more oxygen and nutrients can be delivered to tendon cells, accelerating the healing process.

In addition to guiding the ESWT process, high resolution ultrasonography offers capabilities for superior microvascular imaging (SMI) and sonoelastography. SMI can reveal vascular activity in the target tissue that indicates where inflammatory activity exists, and where healing has begun. Elastography measures tissue density and elasticity, which helps gauge the effectiveness of EWST treatment.
Despite evidence that focused shockwave therapy is effective for promoting tendon healing, its precise mechanisms of action remain a mystery. Scientists have proposed four possible phases of action:

ESWT stimulates new functional proteins that induce the following effects:
Shock wave therapy is often used in conjunction with other therapies, or as a last resort when other treatment measures have failed to promote healing. The International Society for Medical Shockwave Treatment has provided guidelines for ESWT use.
Clinical indications for ESWT include:
Shock wave therapy is not recommended for conditions that involve lung tissue, malignant tumors, epiphyseal (growth) plates, brain or spinal regions, or during pregnancy.
Achilles tendinopathy can be subcategorized into insertional and non-insertional tendinopathy. Insertional tendinopathy occurs close to the bone, where the tendon attaches muscle to bone. Non-insertional tendinopathy affects tissues in the middle portion of the tendon.
Popular treatment methods for Achilles tendinopathy include:
Of those, eccentric loading and physical therapy are standard protocols for treating athletes with Achilles tendinopathy. Multiple studies have been conducted to gauge the efficacy of ESWT for treating Achilles tendinopathy. While results are varied, the general consensus is that ESWT is an effective treatment for both insertional and noninsertional Achilles tendinopathy when other conservative treatment options have failed, especially when combined with eccentric loading.
The clinical director at NYDNRehab, Dr. Lev Kalika, is an expert in ultrasound guided shock wave therapy. He has published multiple peer-reviewed papers on the subject and successfully treated hundreds of patients.
The NYDNRehab clinic in Manhattan features some of the most advanced medical technologies for tendinopathy treatment, rarely found in private clinics, including:
For accelerated healing and successful return to sports, contact NYDNRehab today. We offer physical therapy and chiropractic care, along with TeleHealth services so you can receive treatment on the go. Get the best treatment available in NYC at NYDNRehab in Manhattan.
Resource:
Moya, Daniel, et al. “The role of extracorporeal shockwave treatment in musculoskeletal disorders.” JBJS 100.3 (2018): 251-263.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: