Complex regional pain syndrome (CRPS) is a painful and sometimes debilitating neuro-inflammatory disorder that arises after a minor traumatic limb injury such as a sprain, strain, fracture or scrape, or sometimes after surgery or immobilization. Previously referred to as reflex sympathetic dystrophy (RSD), the condition affects roughly 80,000 Americans each year. The syndrome is marked by increased pain over time that is more severe than one would expect from the original injury.
CRPS is caused by a malfunction of the nervous and immune systems in response to tissue damage from trauma, causing nerves to misfire and send constant pain signals to the brain. CPRS normally affects an injured limb, but can also occur in the hands, feet, or back. The most common occurrence of CRPS is after a fracture to the distal radius, at the thumb side of the wrist.
CPRS can be divided into two subcategories:While CRPS can affect anyone at any age, it most commonly affects people in their mid 30s, with females 3.5 times more likely to report the condition than males.
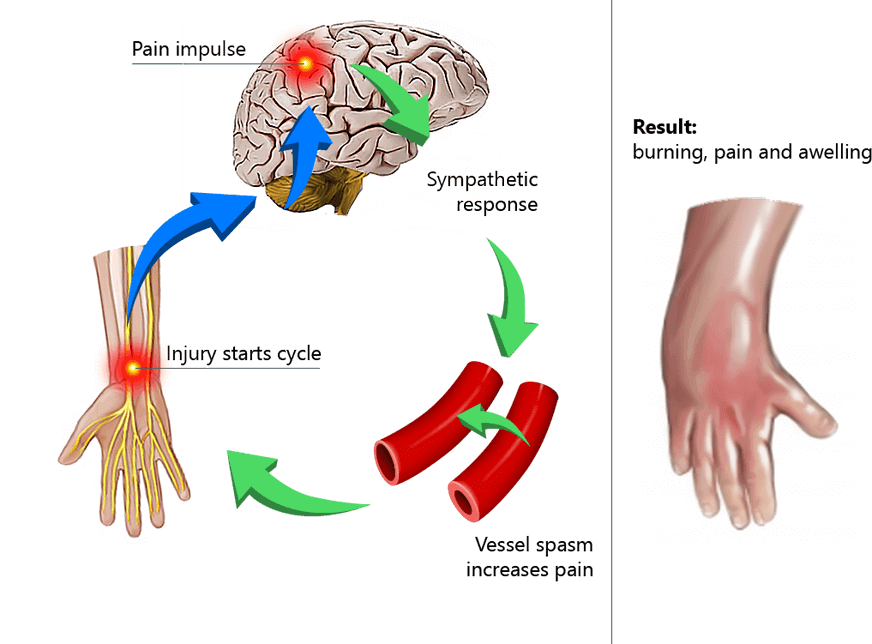
The main symptom of CRPS is pain that increases after an injury, rather than decreasing as the injury heals. Other symptoms may include:
There is no single or simple diagnostic tool for CRPS. Diagnosis is mostly based on patient history, clinical examination, and laboratory results. Other conditions that might be the source of pain must be ruled out before considering a diagnosis of CRPS.
Early diagnosis and treatment are important for resolving CRPS.
Conventional treatments for CRPS revolve around pain management, and most involve some type of pharmaceutical intervention. Common treatment approaches include:
It is important to note that conventional methods of treating CRPS are focused on managing the symptoms, rather than resolving the condition. Moreover, any type of cold therapy should be avoided, as it can accelerate the disease and worsen symptoms.
At NYDNRehab, we take a holistic approach to CRPS treatment, paying close attention to the unique needs of the individual patient. Physical therapy treatment is geared to increasing strength and mobility while gradually reducing and eliminating pain and other symptoms.
At NYDNRehab we mainly concentrate on:
Progressive desensitization techniques to stimulate and desensitize the painful area.
We also use our C.A.R.E.N system for pain modulationand cortical integration.
The end goal of treatment is to improve strength and range of motion while reducing the perception of pain, helping the patient achieve more normal function without pain.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: