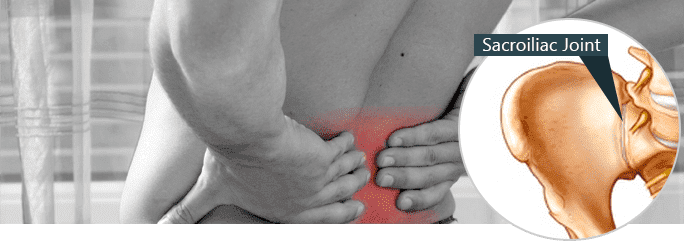
A particularly painful condition, disorders of the sacroiliac joint affect millions of people. Often experienced as a dull pain in the lower back that radiates sharp pain throughout the upper back, buttocks, groin, and thighs, sacroiliac joint disorders are responsible for between 15-30% of all conditions involving back pain.
The medical term for the upper part of the pelvic bones are the “ilia”, the plural form of “ilium”. The top of each pelvic bone is joined to the sacrum, a triangular-shaped bone located near the bottom of the spine. If this joint, connecting the sacrum and the ilium, becomes inflamed, it can lead to chronic pain known as sacroiliac joint pain.
Inflammation of the sacroiliac joint (SIJ) can be the result of an injury, too much motion of the joint, or not enough motion of the joint. The two SIJs in the human body form a rather rigid connection to the pelvic bones and can become inflamed after repetitive irritation from being twisted beyond their normal range. The SIJ is cushioned by a small amount of cartilage on either side and damage to this cartilage can lead to irritation of the SIJ. Abnormal flexion of the SIJ can lead to the joint becoming permanently or chronically misaligned, causing pain.
Additionally, unrelated illnesses like Ankylosing Spondylities can cause the SIJ to become excessively rigid or stiff, leading to irritation that promotes SIJ pain.
The chronic condition of experiencing SIJ pain goes by a number of names, including SIJ Pain Syndrome, SIJ Disorder, SIJ disease, SIJ Syndrome, and Sacroiliac Syndrome.
Only a doctor can properly diagnose SIJ Pain Syndrome but confirmed cases usually involve individuals regularly experiencing SIJ pain for more than 4-6 weeks.
Only a trained medical professional can diagnose SIJ pain after ruling out potentially related causes for the condition. Symptoms of SIJ pain include:
It can be very difficult to diagnose SIJ pain due to the fact that it often resembles many other similar disorders of the back, hips, and pelvis. Generally, an X-Ray, CT scan or MRI will be unable to distinguish any determining characteristics to reliably identify abnormalities or inflammation of the SI joint. Furthermore, palpation (touch) tests have been shown to be unreliable in identifying abnormal positions or range of motion of the SIJ joint.
To properly diagnose SIJ pain, a series of orthopedic motion tests are used. These include:
Gaenselen Torque Test – The patient lies on his or her back with the knee lifted and pushed towards their chest while the other leg is flexed over the edge of the examination table.
Femoral Shear Test – Sometimes called the “thigh thrust” test, this involves bending the leg while slowly pressing on the upper part of the leg.
Iliac Gapping Test – With the patient lying flat on the table, the doctor places pressure on the upper part of the leg, pushing in an outward motion.
Iliac Compression Test – With the patient lying on his or her side the examiner presses on the upper part of the hip.
Sacral Thrust Test – With the patient lying prone (facedown), the examiner applies pressure at the base of the spine.
FABER’s Test/Patrick’s Test – With the patient lying flat on the table, one leg is bent and slowly rotated.
The above tests consist of placing the patient’s body in specific positions and applying pressure in order to precisely identify the source of the pain.
Additionally, the doctor can insert a needle into the SIJ to inject a a numbing solution and a special dye. When scanned by an X-ray, an arthrogram is produced, a special diagnostic image of the dye that can identify SIJ dysfunction. To increase accuracy of diagnosis, the process of injecting a numbing solution in to the area is usually conducted on two separate days. If the injection results in the temporary cessation of pain and the arthrogram reveals inflammation, this is generally consistent with a diagnosis of SIJ disorder.
A new imagining technique called the SPECT test has been shown to result in the successful diagnosis of abnormalities or inflammation of the SI joint. The SPECT test stands for Single Photon Emission Computed Tomography. A small injection of a non-harmful radioactive isotope is injected into the area and then scanned by a SPECT device which then constructs a highly accurate three-dimensional model of the area. The SPECT scan will record blood flow through the region, useful in identifying constrictions or inflammation of in and around the SI joint.
For conditions of minimal SI joint pain, a number of therapeutic treatments can be used to minimize or eradicate discomfort in the area. These include:
Ice – Applying ice or cold packs to the affected area for approximately 15-20 minutes for an interval of between two days and two weeks. This will help reduce inflammation. If the pain is eradicated or greatly reduced after two weeks, it should be possible to return to normal activities.
Heat – The use of a heat wrap or taking hot baths can be useful for helping the affected area to heal.
Rest – The immediate cessation of strenuous activities or any motion that provokes pain.
OTC Medication – Your doctor may recommend certain over-the-counter pain medications such as acetaminophen to reduce pain. OTC medications like ibuprofen or naproxen may also be appropriate to help reduce swelling.
Soft tissue massage – This can help loosen and relax constricted ligaments and the SI joint.
Taping – The hip area can be taped in place to provide immediate relief of pressure on the injured joint.
Acupuncture – acupuncture for si joint can be a useful therapy to increase and improve blood flow to the area.
Electrotherapy – A mild electric current applied to the area can be useful in increasing blood flow to the SI joint.
For moderate cases of SI joint pain, more active measures may be appropriate. These include:
Cortisone Injections – An injection of these steroids can strongly reduce the amount of inflammation in the area.
Prolotherapy – A therapy known as prolotherapy involves injecting a combination of saline and pain relievers into the joint in order to help relax overly tight SI ligaments.
Chiropractic Treatment – The manual manipulation of the area by a doctor, chiropractor, or health professional can help loosen and re-align a stuck or rigid SI joint. Chiropractic treatments must always be undertaken with great care as it is very easy to exacerbate the problem with improper manipulations.
Braces/Belts – If the SI joint is too loose, a special kind of orthotic brace similar to a wide belt is applied around the waist to stabilize the joint. In some cases, the hip and waist area can be taped to provide stability to the pelvic region.
Mobility Devices – If only one SI joint is painful, the use of a cane, walker, or other mobility device can be useful in reducing pressure on the affected side.
For more severe cases of SI joint pain, the long-term treatment plan involves a regimen of stretching, strengthening and motion exercises. The purpose of these exercises is to restore the normal alignment of the pelvic region and to improve the strength of the muscles in the area. In many cases, physical therapy will be required to correct abnormalities in the gait (how you walk), balance, and posture.
Your doctor will design a specific course of physical therapy exercises in order to improve the tension, range, and strength of the muscles in your lower back, hip, and glutes. Special exercises to strengthen your lower abdomen and “core” will also be highly useful in preventing future overextension or flexion of the SI joint, and thus minimize new incidences of inflammation and abnormal motion. The hip muscles will follow a program of first strengthening and toning the deep muscles, followed by the intermediate group of muscles, and then the superficial muscles.
As the muscles and core strength is improved, the next step of therapy to heal SI injuries and prevent future damage is to correct pelvic alignment and improper motions during certain body positions. Your physical therapist will design a course of therapy to correct the patterns of walking, sitting, moving, and standing that initially led to inflammation and abnormal motion of the SI joint.
While every course of physical therapy and strengthening exercises are uniquely tailored to the individual, generally long-lasting relief can be achieved in approximately six to eight weeks.
Certain orthotic devices, including the use of bands, belts, and/or shoes may be required to correct and stabilize the area. Over time, as the body is permitted to heal and strengthen, it will be possible to slowly wean off the use of orthotic stabilization aids.
For extreme cases of unremitting SI joint pain, an injection to block the nerve signals from the SI joint to the brain may be necessary. Additionally, a surgical procedure known as a fusion of the SI joint may become necessary. A SI joint fusion surgery involves permanently soldering the SI joint in place to lock it into place, preventing any further abnormal flexing or motion.
Unfortunately, even after SI joint pain has been eliminated and a corrective course of therapy has been applied, there is a strong tendency for SI pain to return. Experts believe that insufficient rehabilitation of the related muscles, particularly insufficiently strengthened abdominal and hip muscles, leads to a return of improper motion and renewed irritation and inflammation of the SI joint. Therefore, it is imperative to fully implement a complete course of physical therapy to fully strengthen the muscle groups in order to prevent a reoccurrence of SI joint pain.
A number of stretching and strengthening exercises have been shown to proactively prevent injury or re-injury of the SI joint, including special SI joint strengthening forms of astana yoga. Additionally, a number of techniques can be used to prevent damage or stress to the SI joint:
Warm Up Properly – Before engaging in any activity involving lifting weights or playing sports, it is important to properly warm-up all of the related muscle groups.
Identify Causes of Pain – Certain motions, activities, and actions will cause immediate pain. It is important to identify these and refrain from engaging in them.
Stretching – Stretching the back, abdominal, and hip muscles wll help keep them loose and limber, avoiding the overextension and inflammation of the SI joint.
Avoid Lifting Heavy Weights – The SI joint is directly related to the spine’s ability to help lift weights.
Get Plenty of Rest – Tired muscles are more susceptible to injury. Thorough rest will also help the body heal more rapidly from minor damage or inflammation of the SI joint.
The most effective course of action to prevent onset or the re-occurrence of SIJ is the maintenance of strong muscles in the hips, hamstrings, back, and abdomen.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: