Meniscus tears are common athletic injuries, often occurring in sports that require pivoting on a loaded knee or rapid directional changes as the athlete moves at high velocities. Basketball, volleyball, soccer, football and skiing are sports that see a high incidence of knee injuries, including torn menisci. A torn meniscus does not mean you need surgery. Most meniscus tears are self-healing, and respond well to conservative care.
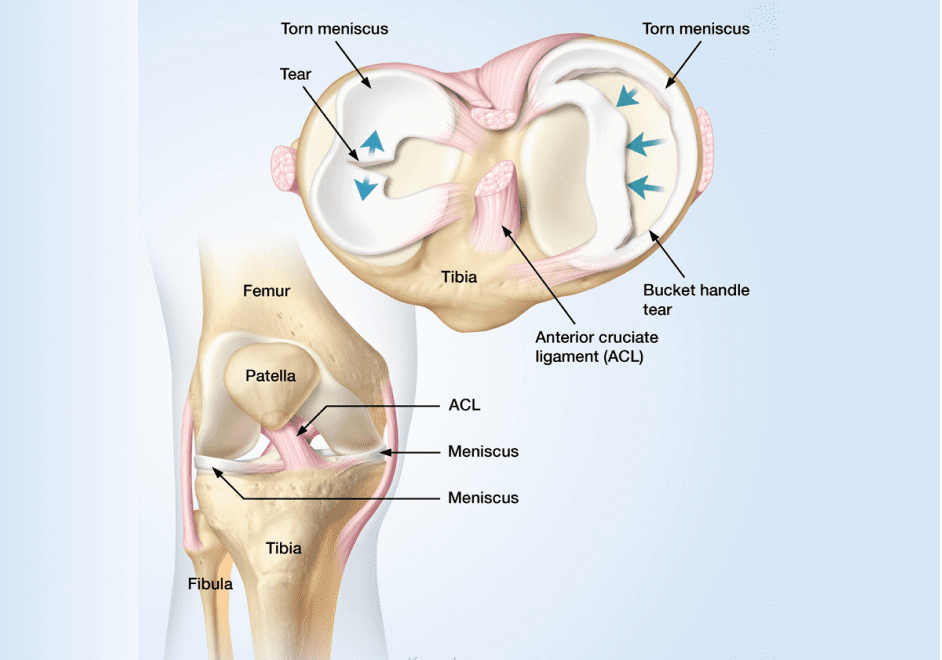
Each knee has two large C-shaped pieces of cartilage that cushion the knee, preventing the tibia in the lower leg from rubbing against the femur. The menisci act as protective shock absorbers during physical activities like running, landing from a jump, decelerating and cutting. Menisci are tough and rubbery, but they can tear when the knee is torqued while loaded. Meniscus tears are seen mostly in athletes, but they are also common in deconditioned older adults.

Many patients report a “popping” sound or sensation when a meniscus succumbs to force and tears. While you will likely be able to walk or even continue playing on your injured leg, it will eventually become swollen and painful.
Common symptoms of meniscus tear include:
Failure to treat a torn meniscus can lead to knee instability and the development of compensation patterns that reduce performance and increase injury risk.
Athletes are at the highest risk of meniscus injury. When force loads exceed the ability of the knee’s structures to stabilize the joint, ligaments, tendons, cartilage and menisci are placed at risk. Pivoting or changing directions on a loaded knee are common causes of meniscus tears. Training injuries like deep squatting and heavy lifting can also overload your knee joints.
After age 30, the menisci often become weaker and thinner, especially in sedentary populations. Older adults can suffer meniscus tears from everyday movements, such as getting up out of a chair. Osteoarthritis can increase the risk of meniscus tears, and conversely, a meniscus tear can cause osteoarthritis to develop.
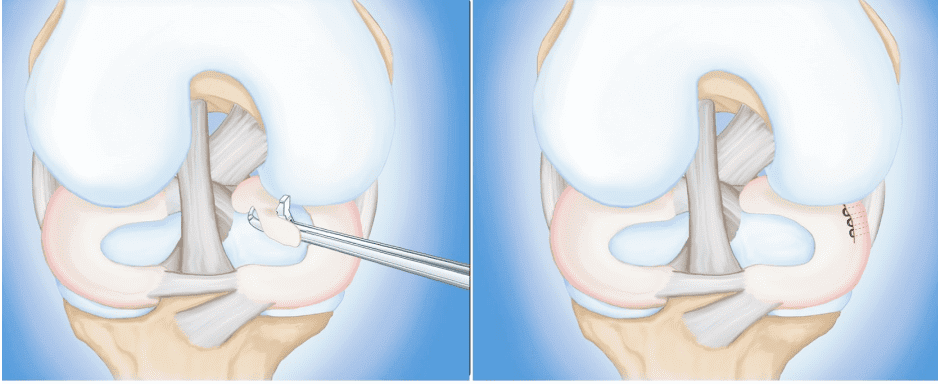
The first step in diagnosing a meniscus tear is a clinical exam. The clinician will ask you what you were doing at the time of injury, ask you about previous injuries and gather other relevant information. They will test you for strength and range of motion and palpate along the meniscus line.
Diagnostic ultrasonography is one of the best technologies available for diagnosing knee injuries. Unlike MRI or Xray, ultrasound allows for real-time imaging with the patient in motion, enabling the clinician to view the knees’ structures at different angles while the patient provides feedback. Because ultrasound imaging delivers instantaneous results, the patient is able to begin treatment immediately.
In the early stages after a meniscus tear, you should follow the RICE protocol for soft tissue injuries: rest, ice, compression and elevation. NSAIDs may help to alleviate pain. Once the swelling has gone down, you can begin rehab exercises like knee extensions, squats and hamstring curls, and gradually progress to more challenging exercises like single-leg squats and lunges. It is recommended that you begin exercises under the supervision of a sports medicine physical therapist, especially if you intend to return to sport.
Menisci have a limited blood supply that delivers nutrients and oxygen to the tissues to help them heal. When combined with physical therapy to strengthen the surrounding muscles and connective tissues, knee stability can be completely restored in most cases.
For athletes who want to return to sport, cell regenerative treatments are a popular option. Ultrasound guided injections of platelet rich plasma or prolotherapy can stimulate meniscus healing and accelerate the rehab process. Because your meniscus is already trying to heal itself, US guided injection therapy can give it an extra boost to speed up healing and get you back on the playing field.
Meniscus tears are fairly common among athletes, runners and older adults. Accurate diagnosis and conservative treatment for a torn meniscus is essential if you want to remain active and return to sports.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: