The structures surrounding your hip and pelvic region are a complex system of muscles, tendons, ligaments, nerves, joints and bones. They all interact together to transfer force loads between your upper and lower body, stabilize your spine, and support and protect your visceral and reproductive organs. As with any complex system, many moving parts means there are a number of things that can go wrong, and when something is out of whack, it often manifests as some type of hip pain.
Hip pain can present at the front, side, or back of the hip region, or in the groin area, and the exact cause can be difficult to diagnose. However, there are five common causes of hip pain that can be distinguished with a thorough diagnosis.
- Damage to the hip joint itself. Your hip joint is formed by the trochanter (ball) of the femur (or thigh bone), where it fits snugly into the socket of your pelvis. The structures are held in place by a strong network of ligaments, and facilitated by cartilage that allows the ball to glide freely within the socket. Damage to the hip joint itself is most often associated with wear and tear due to aging. Pain from hip joint damage is often felt at the front of the hip or groin area.
- Bursitis of the Hip. Bursae are fluid-filled sacs found in joints that provide a cushion between boney structures and soft tissues. An inflamed bursa at your hip joint can be quite debilitating, causing pain at the lateral or outside area of the hip that sometimes radiates down the side of the leg. Bursitis can be caused by overuse during sports or exercise, or can result from muscle weakness or obesity.
- Lumbar nerve compression or irritation. The nerves that govern your hip and leg movement descend from your lumbar spine, and they can become compressed or irritated as they exit the spinal canal. While the problem originates in your low back area, you may feel pain at the back of your hip or in your buttocks region.
- Deep gluteal syndrome. Previously called piriformis syndrome, deep gluteal syndrome occurs when the sciatic nerve becomes irritated or entrapped in the subgluteal space, where it passes beneath the piriformis muscle. The pain is deep beneath your gluteal muscles and can radiate down your leg.
- Hamstring insertional tendonitis. Your hamstring muscles originate at your pelvic region, beneath your buttocks. Pain in your lower buttock area that sometimes radiates down the back of your leg may indicate an inflamed hamstring tendon.
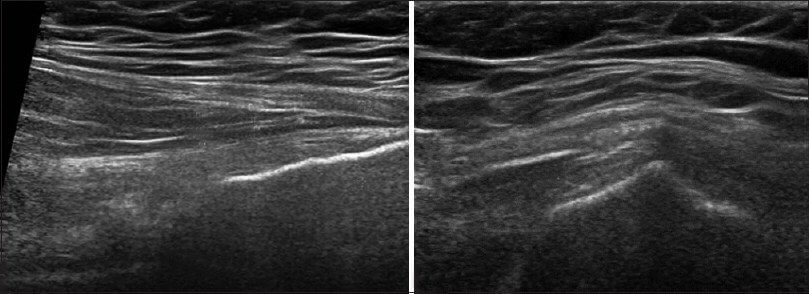
Hip pain can result from overuse, underuse or abuse of your muscles. Poor flexibility is often a contributing factor. The hip pain specialists at NYDNRehab use diagnostic ultrasonography, computerized gait analysis and other advanced diagnostic tools to identify the exact cause of hip pain. An individualized rehabilitation program is then designed to treat and correct the underlying cause of your pain, so you can return to an active lifestyle, pain-free.