or
Dr.Kalika has revolutionized posterior knee rehabilitation by introducing high resolution diagnostic ultrasonography for structural diagnosis, combined with gait and motion analysis technology to visualize and objectify the functional movement of the knees and lower extremities.
The motion and gait analysis lab at NYDNRehab is the only private lab in the US to feature research-grade technology, normally found only at top research universities. We use our advanced technologies to provide our patients with the very best diagnostic and treatment options in Manhattan, NYC.
Our holistic and patient-centric approach makes NYDNRehab the clinic of choice for treatment of posterior knee pain in NYC.
Conventional posterior knee rehabilitation clinics often take a one-size-fits-all approach to knee pain, using cookie-cutter exercises and antiquated timelines that do not fully rehabilitate knee injuries or restore optimal movement.
In most cases, physical therapy does not provide a stand-alone solution for resolving posterior knee pain. Prior to beginning physical therapy, other issues need to be addressed that can undermine the effectiveness of physical therapy exercises.
Problems that need to be addressed before beginning
physical therapy include:
At NYDNRehab, we use advanced technologies to accurately diagnose and measure individual parameters for joint angles, force loads, muscle firing patterns and gait. We then design a personalized treatment protocol based on the patient’s unique profile, measuring progress along the way to ensure full recovery.
We understand that every patient has a unique anatomy, and that every knee injury has unique characteristics. We tailor our one-on-one treatment plans to the individual patient. Our holistic approach goes beyond treating symptoms, to identifying contributing factors and resolving them.
In addition to strengthening the structures that support the knee, our treatment for posterior knee pain includes real-time feedback training, to restore optimal muscle recruitment patterns that are often disrupted after an injury. By retraining the neural pathways between the brain and body, we eliminate compensation patterns and optimize neuromuscular communication channels. After posterior knee rehabilitation, our athletes are able to return to sport safely, with reduced risk of re-injury.
NYDNRehab is the top-rated posterior knee rehabilitation clinic in NYC. We accept most health insurance plans, and we are happy to set up payment plans for our patients.
Your common fibular nerve, also known as the common peroneal nerve, is one of the two major branches of the sciatic nerve that innervate your lower extremity. To work as it should, the nerve needs to glide freely among other structures. If the nerve becomes entrapped and is unable to glide, it can produce pain and restrict movement. There are a number of locations where the common fibular nerve can become entrapped, but the most common is in the osteo-fibrous tunnel, where the peroneus longus and soleus muscles attach to the head of the fibula. The tunnel has a fibrous roof made up of fascia.
The fibular nerve has to pass through the osteo-fibrous tunnel as it spirals from the back of the thigh to the front of the leg, where it further divides. Pain from an entrapped fibular nerve manifests behind the knee, and may cause numbness and tingling down the outer surface of the calf, and even to the dorsal foot.
Diagnostic ultrasound is the best means of identifying an entrapped fibular nerve because it allows us to visualize the nerve along its entire path, in real time.
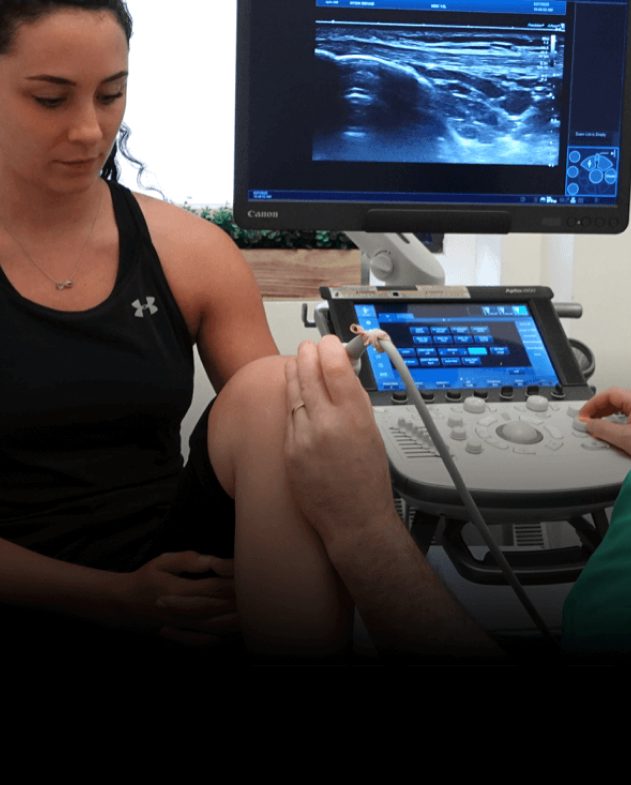
Treatment for an entrapped fibular nerve may include one or a combination of the following:
Another less common condition, usually occurring in runners and athletes, is entrapment of the popliteal artery, creating sensations of pressure or cramping in the posterior knee. The condition is usually caused by atypical gastrocnemius muscle anatomy.
For some, popliteal artery entrapment syndrome may seem like an innocuous annoyance, but in severe cases it could cause a life-threatening condition like deep vein thrombosis (DVT).

Dr. Kalika is a world-renowned expert in diagnostic musculoskeletal ultrasonography, with multiple research studies to his credit. Diagnostic ultrasound enables us to identify the structural causes of knee pain in real time, with the knee in motion. Ultrasound also lets us measure and compare characteristics between the injured and non-injured knee. It also equips us with sonoelastography, to test the elastic properties of tendons and identify degenerating tissue.
We use sophisticated 3D gait analysis technology to identify sub-optimal gait mechanics that contribute to knee pain. Our high-tech motion and gait analysis lab features some of the most advanced technologies for quantifying knee mechanics.
By visualizing the knee in motion and gathering quantitative data about gait mechanics, we are able to establish a baseline for measuring progress. Once the exact cause of knee pain is determined, the most effective treatment plan can be initiated and objectively measured for effectiveness.
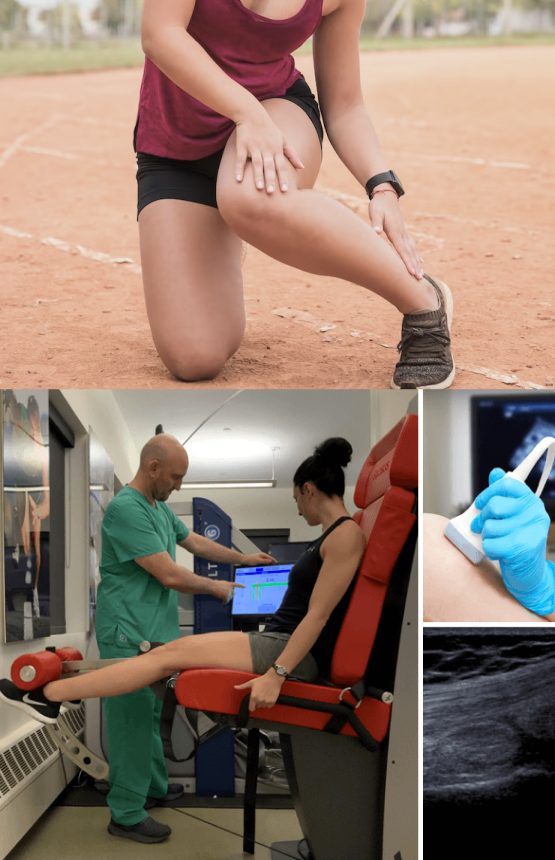
Knee pain can range from mild to excruciating, and many turn to surgery as a first line of treatment. However, most non-traumatic knee pain can be successfully resolved using conservative treatment methods, without drugs or surgery. Our state-of-the-art human movement lab features a growing array of high-tech tools for knee injury rehabilitation and return-to-sports. We emphasize brain retraining, to restore neuro-motor pathways that were disrupted by your injury.

Mechanical deficiencies in walking or running gait can cause the knee to become misaligned, placing undue stress on the structures surrounding the knee and producing pain. We use our state-of-the art gait lab to analyze joint angles and force loads associated with gait, to identify and quantify mechanical deficits and retrain the way you walk and run, to eliminate pain.

Our gravity-reducing treadmill unloads the knee joint, to enable retraining of gait patterns without placing undue stress on injured structures. This approach speeds recovery by allowing gradual reloading of the knee and gradual improvement of gait patterns.

C.A.R.E.N’s advanced technology uses a virtual reality environment to train healthy movement patterns and enhance sports performance. Real-time feedback is provided to optimize motor patterns, retraining the brain-body connection for efficient pain-free movement.
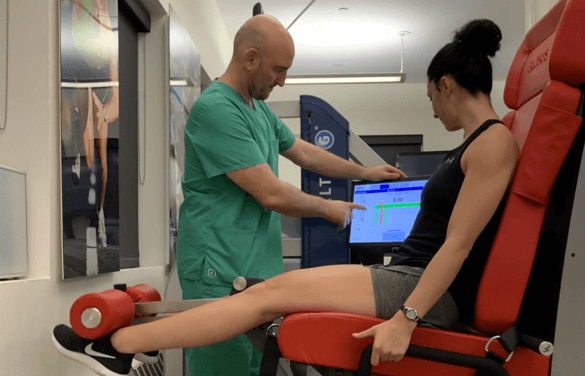
We use the Kineo intelligent loading system to create customized training and rehabilitation programs for our patients. With Kineo, we can customize variable load protocols for knee rehabilitation.
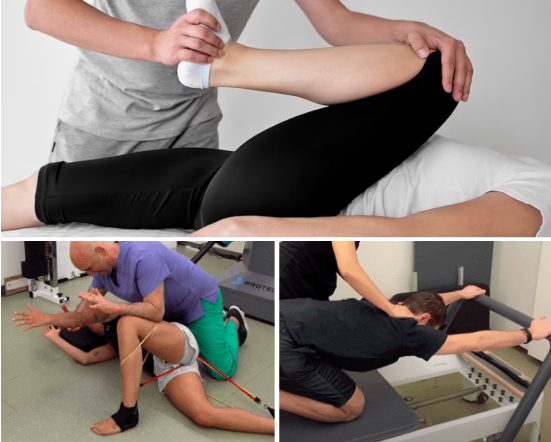
Physical therapy exercises work to strengthen and rebalance the muscles that support the knee joint, taking pressure off of nerves and connective tissue, and realigning the joint for optimal function.
Your physical therapy protocol may include additional corrective therapies, such as:
The human body has its own innate healing mechanisms, but it sometimes needs a nudge to accelerate the healing process. Regenerative technologies help to jump-start healing by stimulating tissue repair at the cellular level. Our outpatient regenerative therapies expedite recovery with minimal discomfort for the patient.

Focused Shockwave Therapy (ESWT)
Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT technology transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Electromagnetic Transduction Therapy (EMTT)

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels.

HIGH ENERGY INDUCTIVE THERAPY (HEIT)
Cold therapy has been used for centuries to treat soft tissue injuries, numb pain and reduce inflammation. Today, modern technology brings us a more efficient and effective means of leveraging cold therapy using nitrogen gas. When used with other therapies, localized cryotherapy helps to provide fast relief and speed recovery during the rehabilitation process.

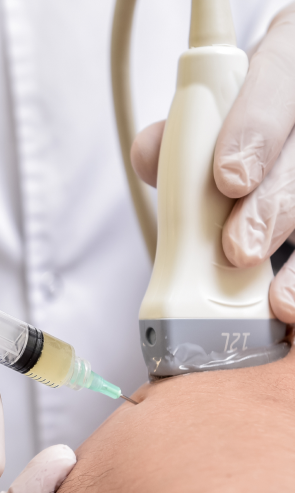
Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
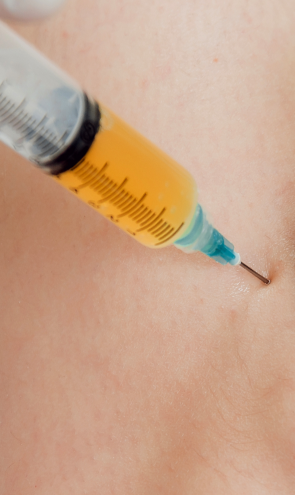
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament and tendon fibers.
The best way to avoid knee pain and injury is to remain physically active, moving your body in ways that recruit multiple muscle groups in multiple planes of motion. In addition, you should manage your weight and eat a nutrient-dense diet that provides the building blocks for lean muscle and connective tissue. Bone-based broth is a good dietary source of collagen, which plays a protective role in the knee joint.
If you are already physically active, you can benefit from a 3D gait analysis and/or a biomechanical analysis, to identify and correct any motor deficits that can potentially lead to knee injuries. Runners in particular can avoid knee pain by visiting the NYDNRehab Running Lab.
Keeping your hamstring and calf muscles flexible and strong, and your quadriceps strong and balanced will help you avoid knee pain. You should also maintain strong gluteal muscles and a strong core. Do not allow your foot to over-pronate, and maintain strong foot core muscles.
To avoid posterior knee pain, it is critical to fully rehabilitate any injuries to the structures of the lower extremity or the low back, including old injuries that were not fully rehabbed.

Strong healthy knees are fundamental to all physical activity, and chronic knee pain can cause compensation patterns that affect other areas of your body. Over time, knee pain can become debilitating, severely affecting your quality of life.
You don’t have to live with posterior knee pain and its consequences. The sports medicine specialists at NYDNRehab are seasoned experts who know how to accurately diagnose and successfully treat musculoskeletal pain and dysfunction. Contact NYDNRehab today, and get rid of posterior knee pain so you can get back to doing the things you love.
These case studies reflect real clinical conditions evaluated at NYDNRehab using advanced diagnostic methods and individualized rehabilitation strategies. All cases are evaluated and managed by Dr. Lev Kalika and the NYDNRehab clinical team.
Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.