
Because tendons are subjected to repetitive loading during sports and exercise, tendon pain and dysfunction are common complaints among athletes and physically active populations. Isometric muscle contractions and eccentric loading have long been favored as treatments of choice by sports physical therapists, to manage tendon pain and improve function.
New research gives us greater insight into the benefits of isometric loading, and how isometric exercises promote tendon healing. We also understand more about the most effective isometric loading protocols in terms of intensity, duration, frequency and exercise selection.
Voluntary muscle contractions occur when a motor neuron delivers a message from the brain that sets a reactive impulse in motion. Each motor neuron is responsible for exciting a given number of muscle fibers. The motor neuron and the fibers associated with it are collectively referred to as a motor unit.
Each motor unit functions according to the all-or-nothing principle, meaning that each impulse from the motor neuron elicits a contractile response in all its associated muscle fibers, at the same time. During isometric contraction exercises, the motor units involved produce a consistent amount of contractile force, called torque, throughout the duration of the exercise.

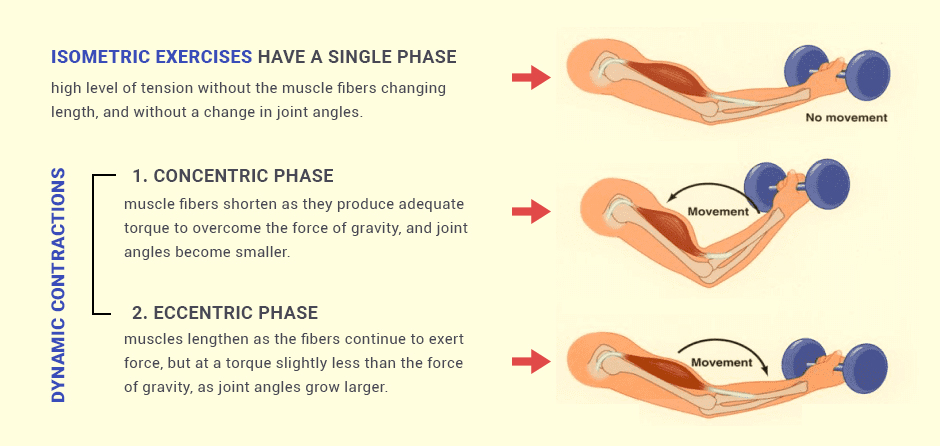
One of the most popular exercises to illustrate isometric muscle contraction is the plank. During this highly effective total body exercise, your muscles develop a high level of tension without the muscle fibers changing length, and without a change in joint angles. By contrast, dynamic exercises require dynamic changes in muscle length and joint angles to produce movement.
Unlike isometric exercises that have a single phase, dynamic contractions take place in two phases. In the concentric phase, muscle fibers shorten as they produce adequate torque to overcome the force of gravity, and joint angles become smaller. In the eccentric phase, the muscles lengthen as the fibers continue to exert force, but at a torque slightly less than the force of gravity, as joint angles grow larger.
Both eccentric loading and isometric strengthening exercises are used to treat tendon pain, promote healing, and restore strength and function. While many studies have compared the relative effectiveness of the two, they are often used in tandem during tendon rehabilitation.
Factors that influence tendon loading rehab protocols include:
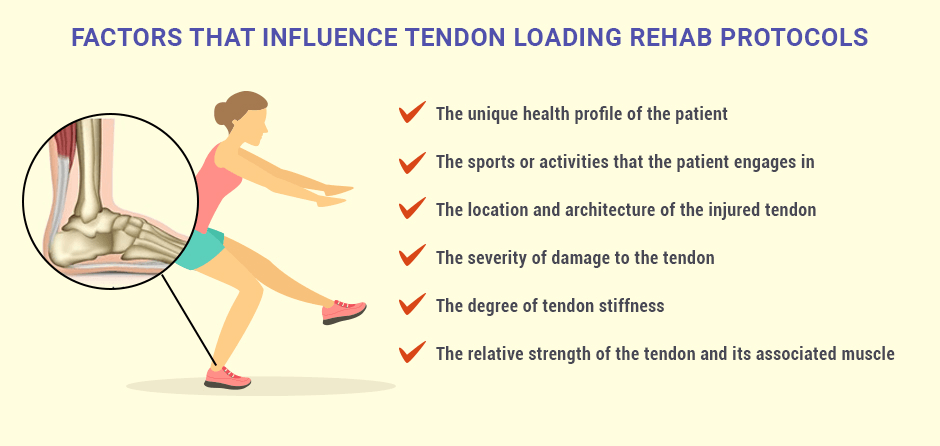
The body of research on tendon loading protocols for treating tendinopathies is extensive and growing. Many recent studies compare various approaches to tendon loading and testing.
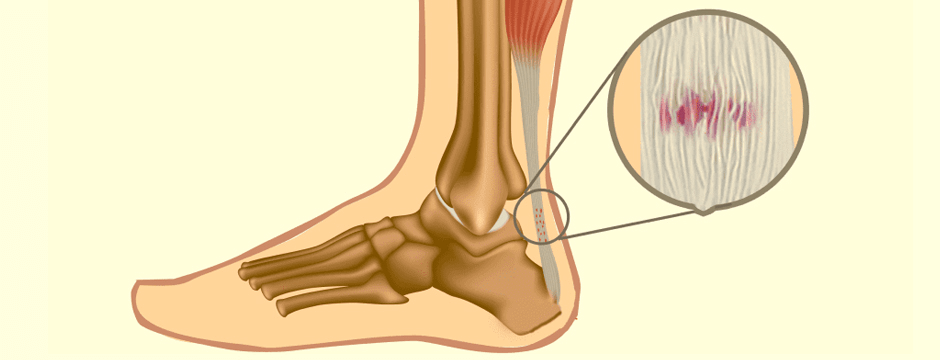
If you are in the habit of working out on a regular basis, you may find it difficult to take time off to heal a sore and inflamed tendon. But failing to allow your tendons ample time for recovery can be a serious mistake. Unlike muscle tissue that is highly vascular, tendons are made up mostly of collagen and have a limited number of blood vessels.
When tendons are injured, their low vascularity means that the delivery of oxygen and nutrients needed for healing is restricted. Over time, placing repetitive demands on an injured tendon can cause its collagen matrix to deteriorate even further, a condition called tendinosis. Unless you take proactive measures to reverse the process and heal the tendon, you could end up with a dysfunctional tendon that inhibits your ability to exercise or play sports.
Accurate diagnosis is fundamental to establishing a baseline and designing a personalized treatment program to promote tendon healing. Once treatment is underway, technological tools help us test the patient’s progress, to ensure our treatment is effective.
Tools for tendinopathy diagnosis and testing include:

Advanced technologies enable us to precisely measure the patient’s progress, eliminating guesswork and ensuring that the patient is fully healed before they return to full activity.
At NYDNRehab, we embrace the latest technologies to bring 21st Century treatment options to our patients. High-tech equipment allows us to precisely measure your progress, so we know without a doubt when it is safe for you to return to your active lifestyle.
Exercise selection and mode can both make a difference in the effectiveness of your tendon rehab program, in accelerating your recovery and restoring full function. However, that is only one small part of the total equation.
For the quickest tendon rehabilitation with the highest likelihood of returning you to full activity, you need the following elements:
Training with an injured tendon can cause it to deteriorate, potentially taking you out of the game for good. To accelerate healing and restore tendon function, you need advanced treatment methods that cannot be found in most physical therapy clinics.
/At NYDNRehab, we design personalized treatment plans based on your unique diagnosis, and we measure your progress every step of the way. We know that rehabilitation is time consuming, and we believe that time should not be wasted. Contact us today, and heal your injured tendon so you can get back to your favorite sport or activity.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: