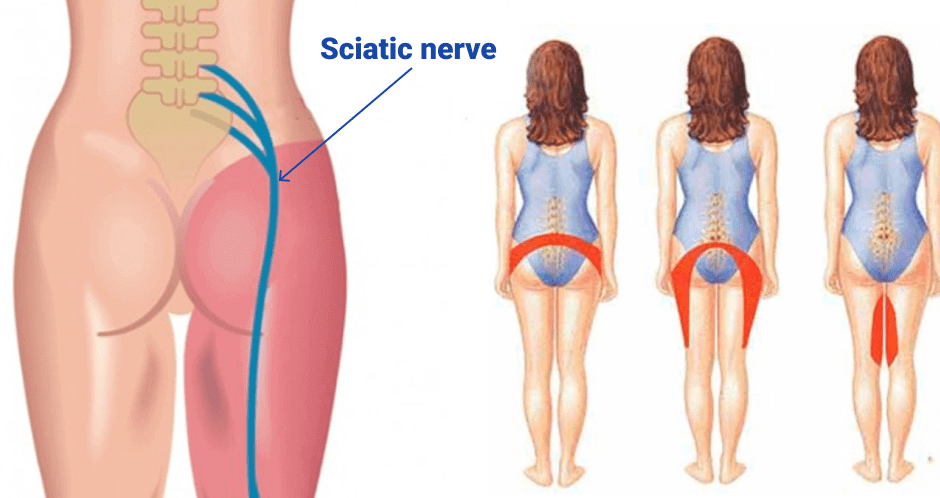
It is indisputable that sciatic nerve pain can be distracting and debilitating, interfering with your daily routine and making your life miserable. But what many people don’t know is that low back and leg pain caused by sciatica is not only treatable, but relapse is preventable with conservative care.
In November 2019, clinical guidelines for sciatica treatment were updated in Denmark, the US, and the UK, emphasizing conservative care as the first line of treatment for sciatica
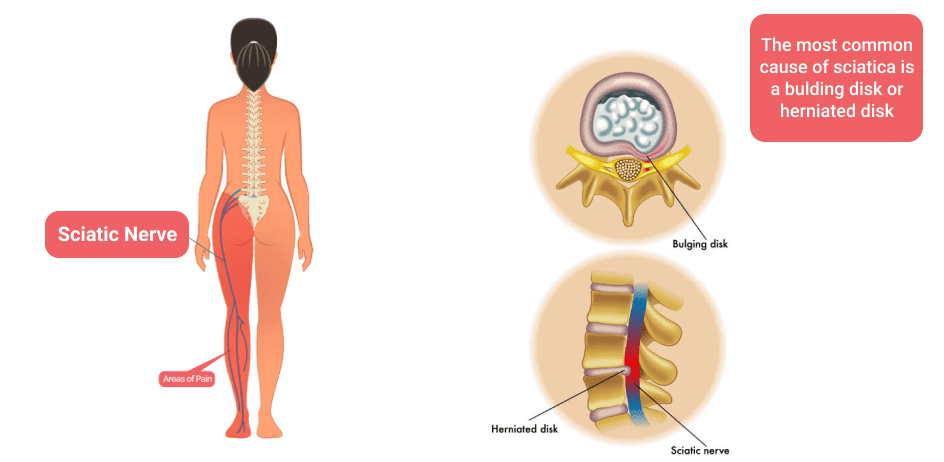
Your sciatic nerve is formed by the nerve roots L4-S1 of your lumbosacral spine, and innervates the muscles in your legs. When the sciatic nerve becomes compressed and inflamed, you may experience aching and sharp pain on one side of your low back that radiates down your leg, often reaching below your knee and into your foot and toes. The onset of pain may be gradual or sudden, and its severity may vary throughout the day.
Additional sciatica symptoms include:
The causes of sciatica vary from one patient to the next. Certain risk factors have been identified, including smoking, obesity and physical labor. The most common cause of sciatic pain is disc herniation that compresses the L5 or S1 nerve root, with pain that radiates down the back or side of the leg, all the way to the foot and toes. Herniation and compression of the L4 nerve root can cause pain at the front and side of the thigh.
The most common cause of disc herniation is age-related degenerative changes. However, adults of all ages may experience sciatica. The condition is uncommon in children, and most often caused by trauma.
There is no single test for sciatica, and MRI imaging is not recommended, as it often leads to unnecessary testing, referrals and expenses, without lending insight into the root cause of pain. Diagnosis of sciatica is mostly based on the patient’s symptoms and a clinical examination. Leg and back pain, pain and tingling below the knee, numbness and muscle weakness are common indicators of sciatica.
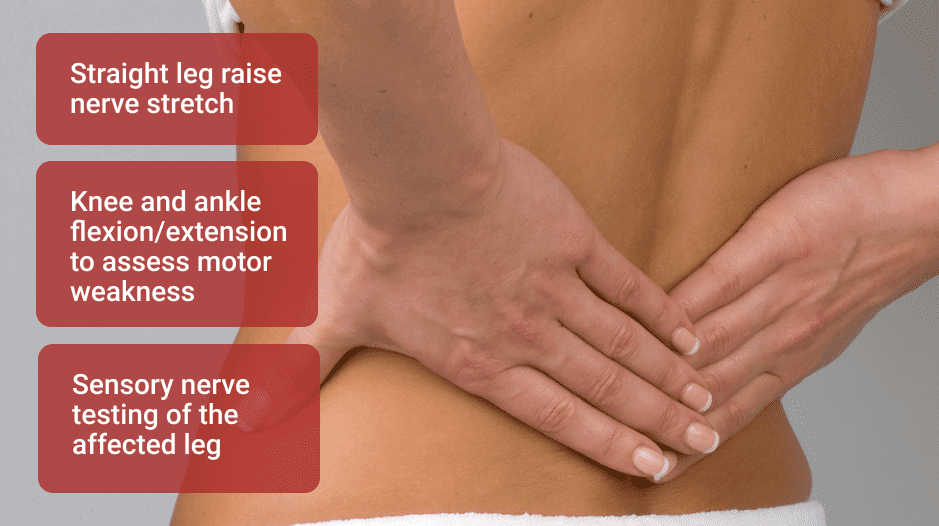
In addition to recording your symptoms, your care giver may run a few simple tests, including:
In addition, other possible causes of pain will be ruled out, based on your health history and clinical exam.
Because the underlying causes of sciatica are often non-specific, general practitioners are often at a loss for treatment options. The first resort for treatment is often a combination of opioid pain killers, anti-inflammatory drugs and bed rest, followed by steroid injections when the initial treatments fail to resolve the issue. However, those approaches often mask the pain of sciatica without eliminating its source.
When drugs and steroid injections fail, patients are often referred to a neurosurgeon to eliminate sciatica pain. Surgery poses much higher risks and is much more expensive than conservative treatments like chiropractic care and physical therapy, yet surgical procedures are common. Statistics show that the outcomes of surgery for sciatica are no different from those of conservative care.
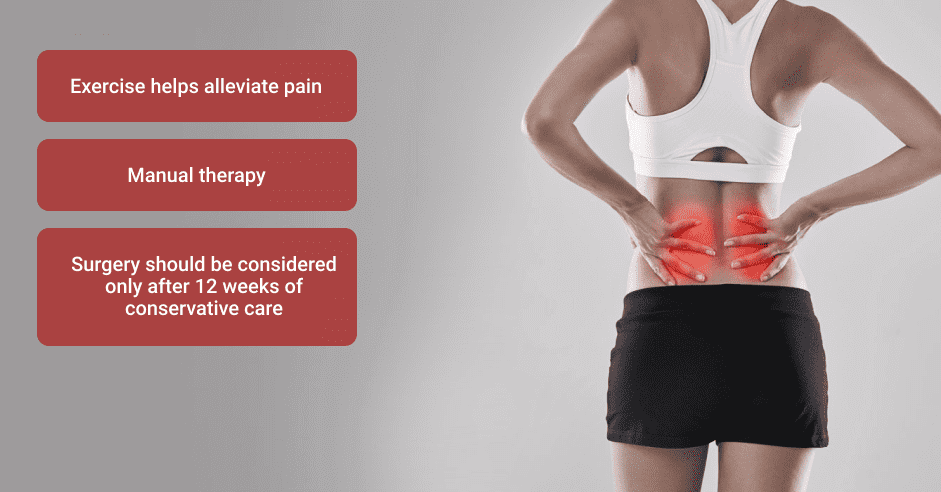
In 2019, the US, UK and Denmark updated their clinical guidelines for sciatica diagnosis and treatment. Key recommendations include:

Persistent sciatica pain can be so debilitating that people often assume surgery to be the only option. Moreover, sciatica sufferers often shy away from physical activity for fear of making the pain worse, or doing further damage. However, numerous studies have shown that conservative care is the best way to treat sciatica.
Conservative sciatica treatment approaches may include:
Physical therapy combined with chiropractic care can effectively relieve pain while correcting postural habits, muscle weakness and other issues that contribute to disc herniation and sciatica pain. Treatment should be geared to preventing future relapses and encouraging better long term self-care habits
The back pain specialists at NYDNRehab are dedicated to eliminating the source of sciatica pain, not just treating its symptoms. We use the most advanced technologies and innovative treatment methods to diagnose, treat and rehabilitate sciatica patients. Our ultimate goal is to wipe out pain at its source, so you can enjoy pain-free movement and an enhanced quality of life.
Contact NYDNRehab today, and get rid of your sciatica pain for good.
Resource
Jensen, Rikke K., et al. “Diagnosis and treatment of sciatica.” bmj 367 (2019).
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: