June 12, 2016
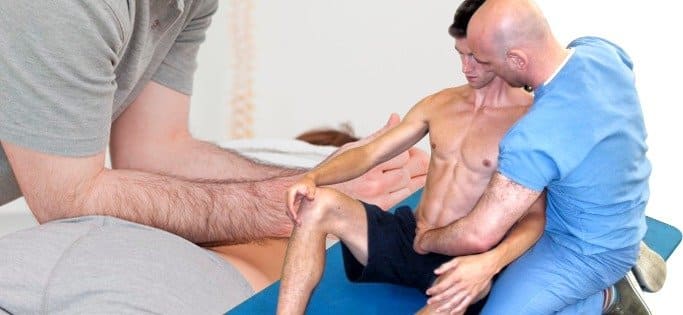
The European Spine Journal has released a study compiled by researchers in the Netherlands who claimed to have gathered some insight as to effective methods of sacroiliac joint treatment. By using a single-blind, randomly distributed trial studied the sacroiliac joint as connected to leg pain in patients.
51 patients took part in the study with sacroiliac joint pain, and all reported leg pain which was attributed to some damage sustained to their sacroiliac joint (SI joint). Determining how to alleviate SI joint pain, participants were randomly assigned to three different groups: Intra-articular steroid injections, manual therapy and physiotherapy. Success was determined if SI joint pain was lessened as reported by participants in the trial using the visual analog scale (VAS) and giving an appropriate score.
The manual therapy group saw great improvement in their SI joint pain. This was determined when 13 participants reportedly improved in respect to their mobility, while five reported no change or a worsening of their discomfort. Those who were given injections were evenly split, with nine patients feeling improvement and an equal number experiencing none. The physiotherapy group only had three participants report a lessening of SI joint pain, and the other 12 reported no improvement whatsoever.
Researchers attached success to VAS scores. Anything between 1.3-2 points would be signs of significant improvement in treating this particular kind of joint pain. This would line up with their findings in manual therapy, which reported an improvement by 1.9 points. But what does this mean for the treatment of patients suffering from SI pain at large?
With the trial concluded and the numbers collected, the researchers concluded that the best method of treatment for this kind of leg pain would at least incorporate manual therapy if the condition is to improve. However, they were quick to point out that these findings should not be uniformly applied. There were specific requirements that were established and the small sample size of the trial may have skewed results, and they urge the need of a larger sample size to see if these results can be replicated.
This highlights a complication that’s rather common with randomized studies such as these. In this particular trial, 23% of applicants came to researchers to preferred methods of treatment already in mind. One patient opted manual therapy, three wanted asked to join the physiotherapy group, 10 asked for injection as opposed to any kind of therapy and five outright refused injections at all. This may have a lot to do with preexisting conditions. Patients were questioned on past health issues, such as herniated lumbar discs and the need for radiculopathy in the past, and many were referred by their physicians, possibly to address the issue of their leg pain.
Biases like these may be a factor for these researchers going forward, and it may help to determine whether of not they’ll be able to replicate the results they collected the first time around. What is certain is the need for participants in the trial willing to be categorized as the researchers see fit.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: