The human body is designed to walk, run, jump and lift objects, and most people take everyday physical activities for granted. But for people born with hypermobility spectrum disorders, everyday activities become a minefield littered with risks of pain and injury. Learn more about joint hypermobility disorder, and things you can do to help manage it.
You can think of your musculoskeletal system as a network of levers whose joints form fulcra. When force is applied to levers (bones) via muscle contraction, the levers rotate around the fulcra (joints), producing movement.
But the fundamentals of movement go beyond that. The architecture of your muscles, tendons and ligaments dictate the functional range of motion of your joints, optimizing their performance while protecting them from overload.
For most people, joint integrity adapts to the specific types of force loads they are subjected to. For example, if you lift weights, your muscles will get stronger, and so will the connective tissues that surround and protect your joints.
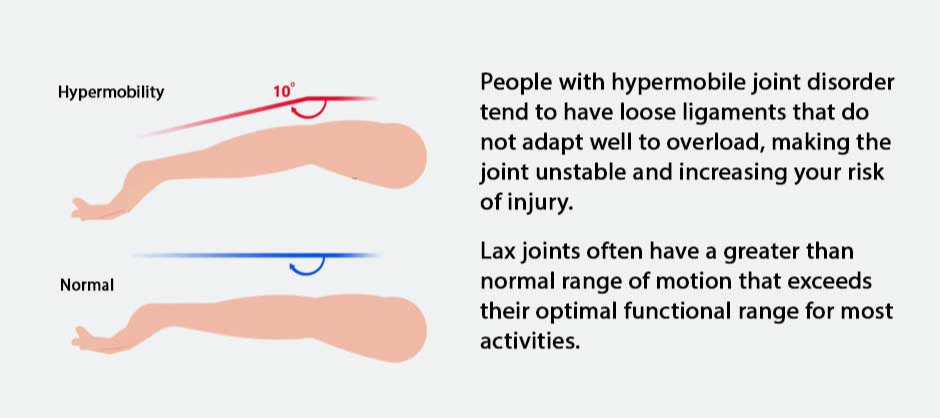
People with hypermobile joint disorder tend to have loose ligaments that do not adapt well to overload, making the joint unstable and increasing your risk of injury. Lax joints often have a greater than normal range of motion that exceeds their optimal functional range for most activities.
Connective tissue disorders are hereditary, meaning patients struggle with symptoms from birth. Connective tissues are made mostly of collagen, a tough substance that holds bones in place (ligaments) and connects muscles to bones (tendons). Fascia is also a type of connective tissue that encases muscles and enables nerves, muscles and blood vessels to glide freely among the body’s structures.
People who suffer from hypermobility spectrum disorders experience mutations in the way collagen fibers are arranged in connective tissue, impacting its behavior. This can lead to laxity in the ligaments surrounding joints, undermining joint stability, impairing movement and interfering with other body structures and systems.

Connective tissue disorder symptoms include:
Stiff achy joints and muscles
Clicking or snapping sensations in joints
Joints that easily pop out of position (dislocate)
Chronic fatigue
Clumsiness and recurrent injuries, like sprains
Digestive problems, irritable bowels and constipation
Bouts of dizziness and fainting
Thin and/or stretchy skin
Hypermobility disorders can affect multiple systems in the body, including the skin, blood vessels, joints, bones, muscles, organs and nerves. When joints are unstable, ligaments, tendons and muscles are at a greater risk of injury. People with unstable joints may also experience balance issues, and can be at a higher risk of falls.
Hypermobility can also affect other systems, including:
Gastrointestinal system
Cardiovascular system
Reproductive system
Nervous system
Being sedentary and sitting most of the time can worsen symptoms of hypermobility disorder. Regular exercise strengthens the structures that support the joints and promotes strong and supple fascia that glides smoothly. However, because hypermobility disorders make tissue more distensible and hyper-responsive, too much motion in an unstable joint can create painful microtraumas that cause post-exercise muscle soreness.
Proprioceptors are sensory nerves that send messages from the periphery to the brain about the body’s position in space. They also communicate how much force is needed to perform a physical task, and how much control is necessary to avoid injury.
Proprioceptors are mechanoreceptors located within the fascia, and proprioception is dependent on the fascia architecture. When collagen fibers surrounding mechanoreceptors are disordered, proprioception is impaired, and messages to the brain are disrupted. Consequently, the body may not know how much force is needed, or when optimal range of motion has been achieved. This can result in pain and injuries, including joint dislocation.
In addition to optimizing the strength and integrity of muscles and connective tissues through physical therapy to stabilize the joints, fascia tissue can be manipulated to promote gliding and enhance proprioception.
Motor control exercises using ultrasound imaging feedback can help retrain proprioception, for more accurate messaging to the brain. Ultrasound guided needling procedures like Prolotherapy can help to repair and strengthen tendons and ligaments, to reduce joint laxity. Ultrasound guided dry needling can eliminate trigger points in fascia that cause pain and interfere with proprioception.
Living with connective tissue disorders can keep you from living life to its fullest. The clinic at NYDNRehab features some of the most advanced technologies and treatment modalities for eliminating pain and promoting safe functional movement. Contact NYDNRehab today, and learn strategies for managing your hypermobility disorder, so you can enjoy everyday physical activities without pain or injury.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: