August 14, 2023
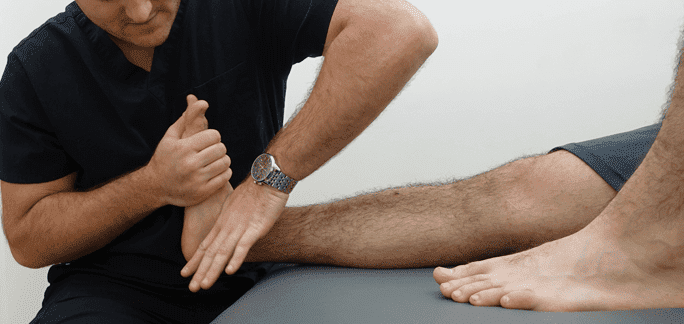 Ankle sprains are very common injuries, and people who suffer from them may suffer ongoing problems, including recurring sprains. Each year, seven ankle sprains occur for every 1,000 people. Up to address dysfunctions of the joints may result in better outcomes.
Ankle sprains are very common injuries, and people who suffer from them may suffer ongoing problems, including recurring sprains. Each year, seven ankle sprains occur for every 1,000 people. Up to address dysfunctions of the joints may result in better outcomes.
Joint dysfunctions that can occur with inversion ankle sprains, which happen when the outer ligaments around the ankle are over-stretched.
Researchers have studied the ankles of people who suffer from recurring ankle sprains in order to suffer from re-injuries. They have found that people may suffer from a variety of joint dysfunctions, including:
By directly addressing all existing joint dysfunctions, therapists who use manual therapy in the treatment of ankle sprains may be able to minimize the risk of ongoing ankle problems.
While several studies have demonstrated the potential short-term benefits of using manual manipulation for the treatment of sprained ankles, the long-term benefits were unknown until a 2013 study. In that study, seventy-four people were randomly placed in one of two groups, including one that performed home exercises as directed by their physical therapists and one in which the patients received manual therapy in addition to performing home exercises as directed by their therapists.
The patients’ ankles were given a baseline assessment prior to the study’s start. Their ankles were then reassessed at four weeks and at six months using multiple scales, including the Foot and Ankle Ability Measure ADL and sports subscales, the Lower Extremity Functional Scale, the NPRS and the 15-point global scale of change.
The participants in the home exercise group saw their physical therapists for 30 minutes once a week for four weeks. They were each given research-based exercise routines to manipulate their joints during their sessions. The people also completed the same home exercise regimens that the home exercise group participants did.
Sixty-five of the original 74 participants completed both their four-week and six-month follow-up appointments. The people who had received manual therapy in addition to the 15.6 percent recurrence rate among those who did not receive manual therapy.
By addressing joint dysfunctions with manual therapy, patients may enjoy better outcomes and fewer re-injuries of their ankles. People who have suffered inversion ankle sprains may want tocols.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: