August 29, 2023

Chronic pain arising anywhere in the pelvic region can have far-reaching repercussions that impact your health and undermine your quality of life. For many people, especially men, pelvic pain is embarrassing, and patients often put off seeking treatment for as long as possible. But ignoring your pelvic issues and delaying treatment can lead to further complications that harm your health and intensify your pain. Standard pelvic pain physical therapy often involves manual manipulation of the pelvic floor muscles, an invasive and embarrassing pelvic pain approach that rarely renders lasting results. Integrative care for pelvic pain is a conservative non-invasive methodology that aims to identify the core cause of your pelvic pain and resolve it for good
For most people seeking pelvic pain treatment, physical therapy is a last resort. Patients often suffer for months on end as they go from doctor to doctor, turning to gynecologists and urologists for help. When those specialists are unable to identify the cause of pelvic pain or resolve it, they prescribe pelvic pain physical therapy as a final alternative.
Standard pelvic pain physical therapy often involves intra rectal and intra vaginal muscle massage, an invasive and embarrassing pelvic pain approach that patients are reluctant to submit to. This methodology is based on the premise that hyper-tense pelvic floor muscles are the primary cause of chronic pelvic pain, and patients are often led to believe that there is no alternative to invasive pelvic pain treatment.
But practitioners who zero in on the pelvic floor muscles alone for chronic pelvic pain treatment are overlooking the numerous other factors that contribute to pelvic pain, and trying to stretch and relax the pelvic floor can actually do more harm than good. Results from this invasive pelvic pain approach are often temporary at best, relegating the patient to ongoing invasive therapy sessions without lasting results.
To truly understand pelvic pain, we need to have some rudimentary knowledge of pelvic anatomy.
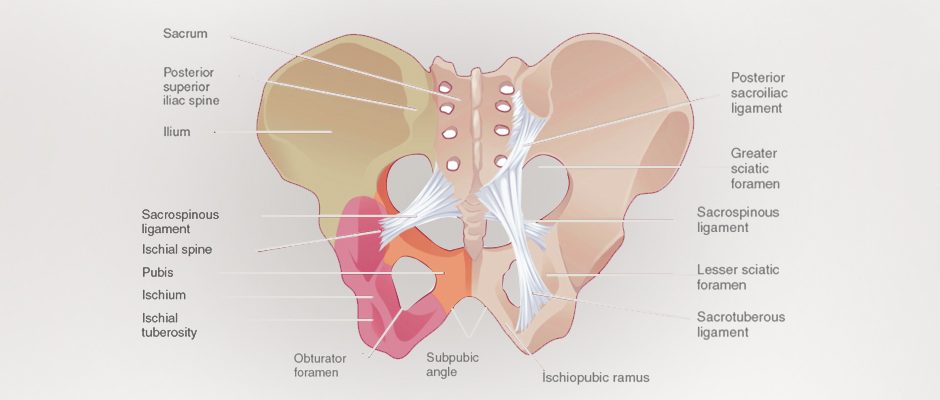
Your pelvic bones form a bowl that articulates (joins) with the sacrum of your lower spine at the back of your body, and with the pubis symphysis in front. Each pelvic bone is composed of three fused bones, the ilium, ischium, and pubis, that are stabilized by ligaments.
The lateral (side) walls of the pelvic bowl are formed by the right and left hip bones, padded by a muscle called the obturator internus. On the posterior side, the obturator internus becomes tendinous as it passes through the lesser sciatic foramen, to attach to the lateral femur (thigh bone).
Most of the obturator internus muscle is covered by fascia that thickens on its medial side to form a tendinous arch, which gives way to the muscles that form the pelvic diaphragm. The fascia divides the obturator internus muscle into an upper pelvic portion, and a lower perineal portion.
On the posterior side, the spinal sacrum connects to the hip bones on both sides, forming the sacroiliac joints, which are supported by ligaments. The gluteus maximus and coccygeus muscles attach to the coccyx, commonly called the tailbone. The main muscle forming the posterior and side walls of the pelvic bowl is the piriformis.
The pelvic floor muscles span the bottom of the pelvic bowl, separating the pelvic region from the perineal region. They perform two important functions:
In addition to bones, muscles and organs, the pelvic bowl houses a complex network of ligaments, blood vessels, neural bodies and fascia.
Given the complex architecture of the pelvic region, it doesn’t make sense to limit pelvic pain treatment to the pelvic floor muscles alone. And given the supportive role played by the pelvic floor muscles, it follows that stretching and relaxing them could potentially undermine their intended function.
Now that we know a bit about pelvic anatomy, it becomes clear that pelvic pain is a multifactorial syndrome and needs to be addressed as such. Let’s look at some alternative causes of pelvic pain that don’t directly involve the pelvic floor muscles.
Considering the many possible causes of pelvic pain — and there are undoubtedly more — we can see why intrapelvic physical therapy does not effectively address its causative factors, yielding only temporary results and failing to break the vicious cycle of pelvic pain.

Your body’s structures do not exist in a vacuum — they are interactive and interdependent, and what goes wrong in one area can profoundly affect the integrity of another.
Integrative care for pelvic pain takes into account the interplay between the various structures that make up pelvic anatomy, along with more distal and seemingly unrelated elements that can cause pelvic pain. By taking a holistic approach, we can intervene to restore optimal pelvic function and eliminate pain.
We have at our disposal a vast array of conservative tools and therapeutic approaches for integrative pelvic care that do not rely on drugs, surgery, or invasive intrapelvic manual therapy.
ESWT is a highly effective, evidence-based therapeutic approach for pelvic pain and pelvic floor treatment. Its benefits include:
EPAT uses acoustic pressure waves to enhance blood circulation to targeted tissues. When used for pelvic pain treatment, EPAT helps to relax and release large areas of tissues. It also has a fibroblastic remodeling effect on fascia, which plays a significant role in pelvic pain.
Ultrasound guidance enables the use of dry needling for deep intrapelvic trigger points that cannot be reached manually, providing superior results compared to manual compression. Moreover, manual release of pelvic floor trigger points does not produce long-lasting results. By releasing trigger points, precise dry needling can quickly ease pressure on intrapelvic nerves, immediately relieving pain.
This approach augments traditional acupuncture needles inserted by hand with a device that generates electrical current, for neuromodulation and the regulation of autonomic balance. The acupuncturist is able to alter the frequency, intensity, and pulse duration of the electric current, to elicit the desired results.
TECAR stands for “transfer of energy capacitive and resistive” therapy. TECAR helps to restore the ionic charge of damaged cells, to accelerate tissue healing.
Fascia is a type of connective tissue that encases muscles and organs, allowing nerves and blood vessels to glide freely among other structures. Healthy fascia is slippery and elastic. When injured, fascia can develop densifications and sticky adhesions that undermine its functional properties. Facial manipulation helps to restore fascia to its healthy state.
Your pelvis houses organs that sometimes move out of place, especially after pregnancy and childbirth. Visceral Manipulation is a gentle technique that uses soft manual forces to restore normal mobility, tone and motion to the connective tissues and ligaments that support visceral organs and hold them in place.
Botox is sometimes used to relax tight pelvic floor muscles, but it should be used with caution, and its effects naturally wear off after several months.
Sometimes used as a diagnostic aid, nerve blockers help us narrow down the source of pelvic pain. Their effect is very temporary.
Physical therapy helps to maintain the integrity of the body’s structures by keeping muscles and connective tissues strong, elastic and balanced. When you’re out of shape, weak and inelastic muscles force your body out of alignment, shifting force loads to structures that are not designed to withstand them. Physical therapy helps to restore optimal alignment, for pain relief and enhanced ease of movement.
Ultrasound is an invaluable tool for assessing muscle activation in the pelvic floor. It allows us to see the pelvic muscles in motion, in real time. Following the release of trigger points via dry needling, ultrasound allows us to detect changes in muscle activation patterns that confirm the effectiveness of dry needling procedures.
Recent research sought to investigate the true causes of pelvic pain and dysfunction, in particular myofascial pain syndrome and muscle trigger points in various parts of the body. The study’s holistic approach examined the ribs, spine, abdominal wall, diaphragm, and pelvic floor to assess movement control, pain generators, fascia restrictions, and trigger points. Ultrasound guided dry needling was used to restore muscle function, eliminate motion restriction, and improve postural balance.
Results revealed that multiple systems are at play in the generation of pelvic pain, and restoring pain-free unrestricted movement in other regions of the body helps to alleviate pelvic dysfunction.
The researchers concluded that:
Invasive manual pelvic pain physical therapy has a poor track record of success, yet it is commonly used to address pelvic pain and dysfunction. Integrative care offers an alternative approach that focuses on restoring pain-free movement throughout the body. By taking a holistic approach, we are able to provide personalized treatment that gets to the core of pelvic pain.
The pelvic pain specialists at NYDNRehab pull out all the stops to get to the bottom of your pelvic pain. By treating the whole patient and not just their symptoms, we have built an impressive track record of success in chronic pelvic pain treatment.
You don’t have to live with embarrassing pelvic pain, or subject yourself to invasive manual therapy. Contact NYDNRehab today, and let us help you get your body back on track, to resolve your pelvic pain for good.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: