September 13, 2023

Any dedicated people-watcher will tell you that people’s posture varies as much as their height, weight, hair color and taste in fashion. The way you carry yourself is part of what defines you as a unique individual. That being said, your posture is not set in stone — it can be modified and improved to enhance your health, appearance and quality of life.
Learn what factors define posture, what internal and external forces influence it, the negative health impact of suboptimal posture, and how retraining your posture can spare you from musculoskeletal pain and dysfunction, now and in the years to come.
You are a dynamic living organism, but in order to move without pain and dysfunction, your body’s systems and structures need to work in harmony like a well-tuned machine. Optimal posture is attained when your joints align in such a way that your body requires minimal energy to hold itself in an upright position. It is estimated that only 10% of the human population functions with optimal posture.
Your posture is governed by multiple systems and structures, including:
Postural alignment is determined by tension generated from muscles, fascia and connective tissue, which in turn is governed by sensory information processed in the brain. When the body is injured, or when neural pathways are impeded, tension forces can become imbalanced, causing joints to become misaligned.
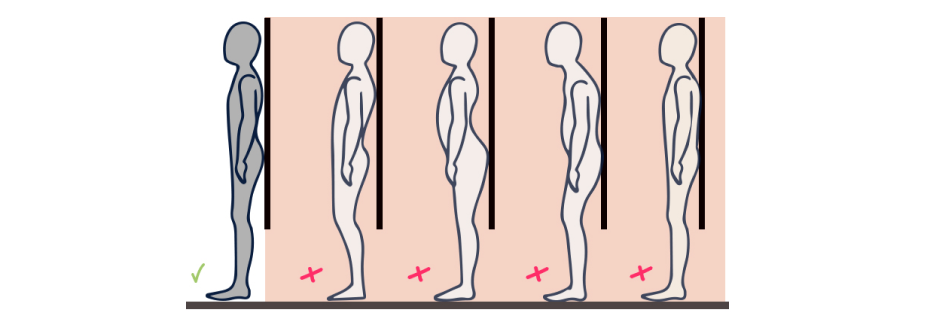
We tend to think of posture in terms of standing or sitting alignment. For example, soldiers are taught military posture to conserve energy while standing at attention. Upright posture with chest out and shoulders back projects strength and confidence. But posture is also dynamic, changing constantly while your body is in motion. In fact, all movement is basically a succession of different postures.
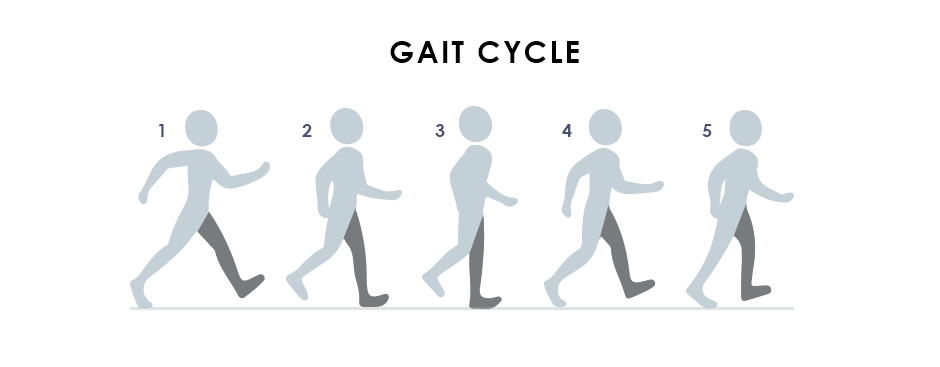
Dynamic posture has to do with efficiency of movement. Athletes strive for optimal dynamic posture as they train to perfect their sports skills. Good posture enables them to conserve energy while generating force. It protects their joints, optimizes their athletic performance, and minimizes their risk of injury.
Whether standing, sitting or moving, good posture allows your body’s structures to move and glide in harmony, without inhibition or pain. Good posture reduces stress on your joints, enables deep breathing, and promotes structural stability.
There are multiple factors and forces that influence posture, some of which are beyond your control, and others that can be easily modified. Nevertheless, anyone can improve their posture by deliberate training and specific interventions. Following are some of the major factors that influence posture.
At its core, posture is dictated by the skeletal system, which provides a rigid framework for the body’s soft structures, much like the chassis of a car. But unlike machines made of metal with identical parts, human bones come in unique shapes and sizes, making posture as individual as personalities. Bone structure variability combined with individual differences in lifestyle factors such as physical activity, nutrition, hydration and daily habits, all work together to define individual posture.
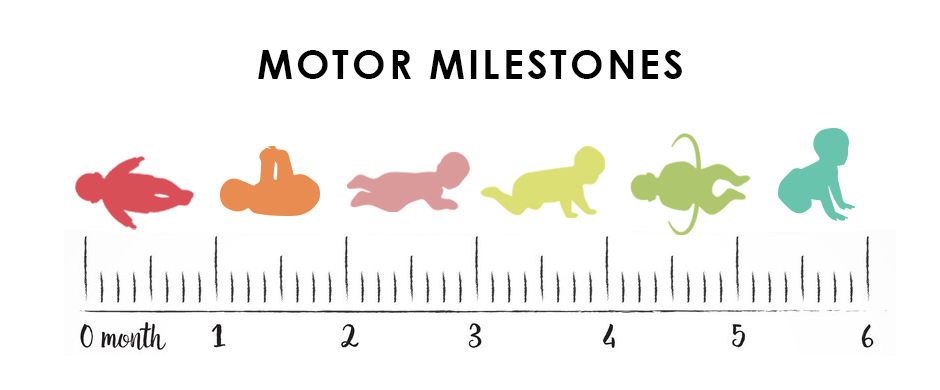
In addition to skeletal variability, humans vary in their neural development (ontogenesis), and their inborn reflexes. For an infant to develop from a helpless bundle of soft tissues to a thriving toddler, he or she must overcome the force of gravity in incremental stages. Infant development is guided by innate reflexes that drive progression from one stage to the next, a process called reflex locomotion.
The concept of reflex locomotion was pioneered by child neurologist Prof. Vaclav Vojta (1917-2000) in the 1950s to treat children with cerebral palsy. During his research, Professor Vojta discovered that complex muscle reactions and movement patterns could be traced to an innate locomotor pattern of movement, and that these innate movement patterns could be stimulated in adults to correct motor deficits and restore good posture. Today, Vojta therapy is used widely in Europe and increasingly in the US to treat patients with postural deficits and movement disorders.
Another factor that plays into posture is dexterity, defined as the ability to physically adapt to environmental changes. For example, you tap into dexterity when you slip on a patch of ice and recover your balance, or when you adapt to changes in terrain while hiking. Our understanding of dexterity is based on the research of Nikolai Alexandrovic Bernstein (1896-1966), a scientist who devoted his life’s work to understanding how the brain controls movement.
Unlike sports training where athletes try to perfect a specific pattern of movement, dexterity is the process of solving motor problems imposed by environmental factors as they arise, correctly, quickly, rationally and resourcefully. It is a means of physically coping with an ever-changing environment. Athletes need dexterity to respond successfully to changes and challenges during play. We all rely on dexterity to perform daily tasks.
Dexterity depends on the plasticity, adaptability and flexibility of the brain in response to messages from proprioceptors — mechanosensory neurons located in fascia, muscles, tendons, and joints — that convey messages about the body’s position in space. Dexterity enables you to manage static and dynamic posture in response to environmental changes.
Tensegrity describes a state of optimal mechanical function, where joints are stabilized and supported by tension generated from healthy myofascial tissue. Fascia tension enables joints to remain perfectly aligned, and to move freely through their functional range of motion.
Fascia is a slippery, strong and elastic tissue that encases and connects muscles and organs, enabling them to glide freely among other structures. When fascia is injured or becomes densified, it loses some of its elastic properties, causing pain and dysfunction, and undermining posture.
Fascia is highly embedded with proprioceptors, delivering valuable information to the brain about your body’s position in space. Densified fascia interferes with neural signaling, often entrapping nerves and blood vessels, and predisposing you to uncoordinated muscle firing patterns that affect your postural system.
All other factors aside, skeletal alignment begins from the feet up. Your foot architecture plays a critical role in determining your posture and overall quality of movement.
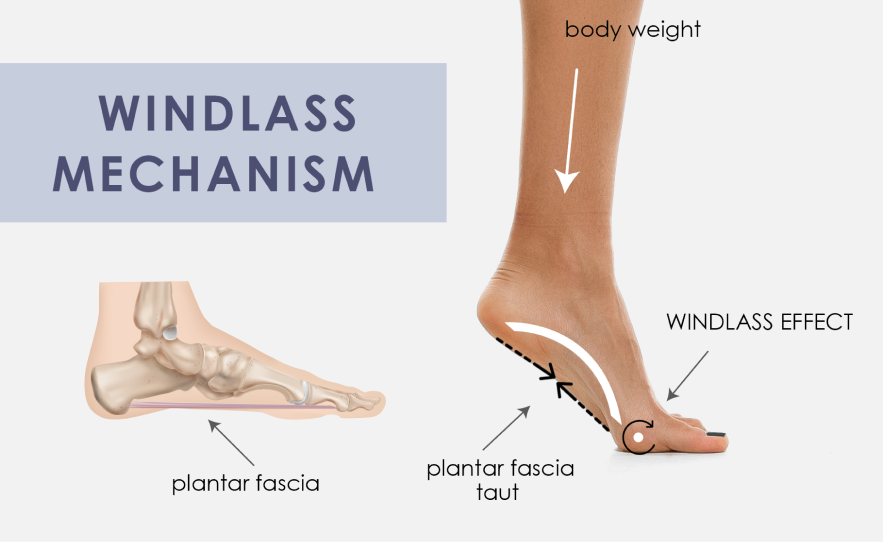
The human foot serves five key functions:
Human feet come in a vast array of shapes and sizes, with variances in arch length and height. From your toes to your heels, your feet have a significant impact on the way you stand and move.
Spinal alignment, both passive and dynamic, depends on coordinated muscle firing patterns governed by motor neurons. In vertebrates, the postural-locomotor nervous system has bilateral symmetry, allowing for symmetrical locomotion and postural alignment.
However, postural symmetry can be disrupted by developmental issues or injuries, altering neural organization and creating asymmetrical motor patterns. To compensate, the body creates suboptimal alternative muscle firing patterns that can become habitual, resulting in poor posture and impaired locomotion.
In addition to signals from your feet and fascia, your posture depends on sensory input from your visual, vestibular and proprioceptive systems. Your somatosensory system — the system that perceives touch, pressure, pain, temperature, movement, and vibration — provides information about joint motion and muscle action, while the plantar surfaces of your feet provide information about the terrain beneath them.
It is hard to imagine that your jaw can affect your posture, yet research has drawn a strong correlation between the alignment of your temporal-mandibular joint and your foot plantar surface.
In one study, 168 subjects were divided into two groups: a temporomandibular joint disorder (TMD) group, and a control group. The researchers used a baropodometric platform to measure load pressure on the foot plantar surface under three dental occlusion conditions: rest, teeth clenching, and with cotton rolls between the upper and lower dental arches. They found that varying temporo-mandibular conditions had a profound effect on the foot arch, and on loading of the plantar surface, both factors that impact posture.
Posturology, also known as Global Postural Recalibration, is a multidisciplinary treatment approach developed in Europe by Dr. Bernard Bricot, a renowned French orthopedic surgeon. The methodology aims to treat musculoskeletal conditions by evaluating and correcting the postural system.
Posture affects multiple aspects of human health, including:
Many common pain syndromes are directly linked to the postural system. Certain conditions, such as joint hypermobility, can undermine posture and pose challenges to everyday movement.
Poor posture has been linked to:

People with such conditions often turn to medical doctors for relief, only to be prescribed drugs and orthotic devices that do little to alleviate symptoms. Only by addressing the underlying causes of health issues can patients hope to restore optimal posture, reclaim health, and enjoy pain-free movement.
Good posture begins with a healthy body. If you are sedentary and get very little exercise, your postural system is most likely out of balance. Simply walking for as little as 30 minutes a day is a good start toward getting your posture back on track. A 3D gait analysis can help you identify and correct motor deficits that cause pain and undermine posture.
Balanced muscle tension is also key to improving your posture. Czech neurologist and physiatrist Dr. Vladimir Janda developed his own approach to evaluating and managing pain syndromes, based on neuromuscular balance. Janda identified patterns of muscle tightness and weakness that cause postural imbalances, classifying them as “Crossed Syndromes.” Janda’s crossed syndromes help clinicians to detect and predict imbalanced muscle patterns, which can then be corrected through stretching and exercise.
Healthy fascia also plays an important role in posture restoration. Fascia should be strong and elastic, able to stretch and glide as the body moves. Healthy fascia is smooth and slippery, enabling nerves and blood vessels to travel unimpeded among the body’s structures. Injured fascia can become dense and sticky, losing its elastic properties and causing adhesions that entrap nerves and blood vessels. Fascia manipulation therapy, dry needling and shockwave therapy are therapeutic approaches that restore elastic integrity — aka tensegrity — to fascia.
Proprioceptors are located throughout your body in fascia, muscles, tendons and joints. Deficits in proprioception are key culprits in causing postural misalignment. Dr. Dario Riva, a highly recognized sports medicine specialist and athletic trainer, developed his own methodology for training proprioceptive control of the postural system. Proprioceptive training is an integral component of postural restoration.
Poor posture often arises due to compensation patterns developed in response to internal problems – a response called somato-visceral compensation. For example, a person with respiratory challenges may subconsciously jut their head forward to create more room for the airway and lungs.
In correcting posture, it is important to understand that our musculoskeletal system will always compensate to protect the internal organs. This important factor is often overlooked by body workers, physical therapists and chiropractors who lack an in-depth understanding of the interdependence of the body’s systems, and are not trained in various postural approaches.
Common conditions that affect posture include:
Failure on the part of clinicians to identify and address the full spectrum of factors that may influence posture can result in suboptimal outcomes for patients seeking to improve their posture.
Contrary to popular belief, aches and pains are not inevitable as you age. More often than not, common pain syndromes and musculoskeletal conditions are closely linked to posture. Many patients go from doctor to doctor, seeking a remedy for their pain and dysfunction. When drugs and surgeries fail to help, they often give up, resigning themselves to a life of pain and reduced mobility.
Postural restoration therapy is a holistic approach to pain treatment. It seeks to restore optimal alignment by addressing the factors that influence the postural system. At NYDNRehab, we take a multimodal approach, combining evidence-based treatment methods that work together to restore healthy alignment, eliminate pain, and improve quality of movement. Contact NYDNRehab today, and start your journey toward improved posture, enhanced mobility, and a better quality of life.
Resources
Cuccia, Antonino Marco. “Interrelationships between dental occlusion and plantar arch.” Journal of bodywork and movement therapies 15.2 (2011): 242-250.
Le Ray, Didier, and Mathias Guayasamin. “How does the central nervous system for posture and locomotion cope with damage-induced neural asymmetry?.” Frontiers in Systems Neuroscience 16 (2022): 828532.
Saltzman, Charles L., and Deborah A. Nawoczenski. “Complexities of foot architecture as a base of support.” Journal of Orthopaedic & Sports Physical Therapy 21.6 (1995): 354-360.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: