
Childbearing is a natural biological process that the female anatomy is uniquely designed to handle, but it places an enormous amount of stress on the pelvic structures. While a few aches and pains are inevitable during pregnancy, intense pelvic pain can indicate excessive strain on your joints and connective tissues. Prenatal physical therapy can help you manage prenatal pelvic girdle pain (PPGP), and help prepare your body for a successful delivery.
Growing another human being is demanding work, and the mother’s body goes through multiple adaptations as the baby develops. Depending on your unique anatomy, you may have difficulty drawing a complete breath as your diaphragm has less room to contract. Women with a shorter trunk often feel as though they are carrying the baby in their rib cage. With the baby taking up so much room, you may experience digestive problems and constipation.
As the baby grows and the volume of amniotic fluid increases, you gain weight in your breasts and pelvic region, and your center of gravity shifts upward, making your body less stable and your body weight harder to balance. Pressure on your pelvic muscles makes them stretch, reducing their ability to stabilize your core, and adding stress to your pelvic joints.
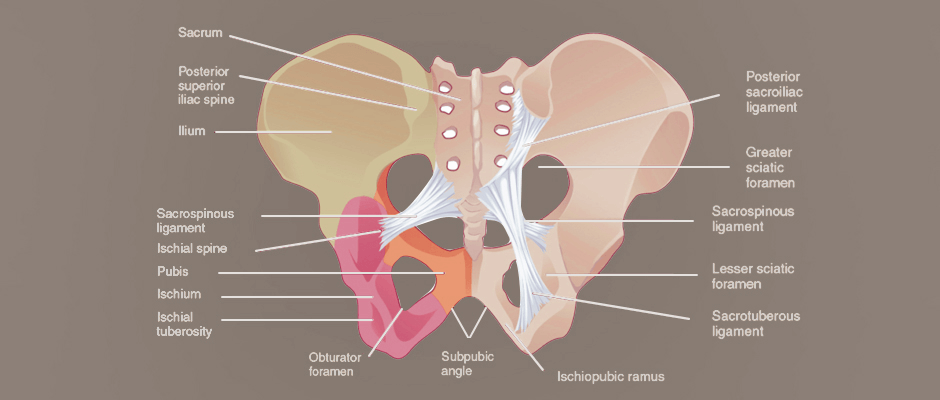
Your pelvic girdle is formed by the bones of your pelvis, the ilium, ischium, and pubis. Together, they create a bowl-like enclosure to house your reproductive organs. The pelvic bones are connected by two sacroiliac joints in the back and the pubic symphysis joint in the front. The joints are supported and held in place by strong ligaments.
During pregnancy, your body releases a hormone called relaxin. As its name implies, relaxin causes the ligaments to become looser and more relaxed, allowing for the pelvic girdle to widen as the baby grows, and to open up as the child travels through the birth canal.
While relaxed ligaments are essential for a successful pregnancy and delivery, they also make the pelvic joints less stable. In some women, instability in the sacroiliac joints and the pubic symphysis causes excess strain on the joints that manifests as pain.
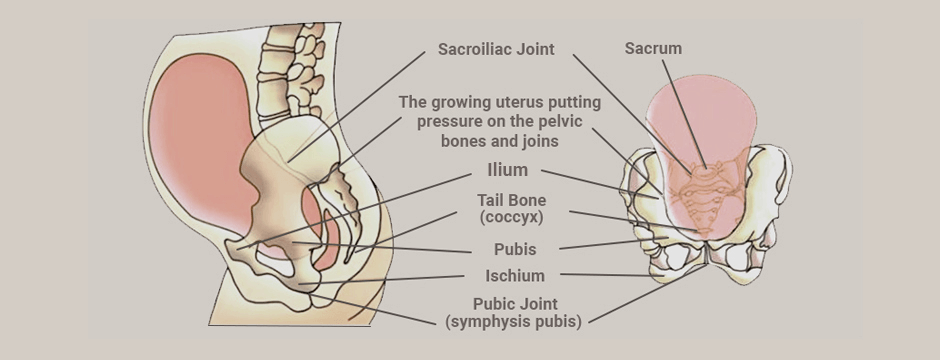
PPGP is often described as stabbing, dull, shooting, or burning. Pain may be felt close to the sacroiliac joints and extend to the gluteal area, or it may occur in the front of the pelvis near the symphysis pubis. PPGP sometimes radiates to the groin, perineum or hamstrings. Because of their location in the lumbopelvic region, pain in the sacroiliac joints can mimic symptoms of sciatica.
Symptoms of PPGP include:
Pelvic girdle pain can lead to muscle pain in the inner thighs and buttocks as those muscles are overused to maintain stability.

The primary means of diagnosing pelvic girdle pain are health history, physical exam and assessments for hip joint function and range of motion. The clinician may use the FARBER test for flexion, abduction, and external rotation of the hip.
An experienced prenatal clinician will be able to distinguish pelvic girdle pain from sciatica, based on reported symptoms. Ultrasound imaging may be used to confirm a PPGP diagnosis, since ultrasound does not pose a threat to the health of the mother or baby.
Physical therapy can help you manage PPGP by relieving pain, improving muscle function and pelvic stability, and adjusting your pelvic joint position. Your therapist can show you strategies for alleviating pain and pressure on your pelvic girdle and strengthening your pelvic muscles.
Chiropractic care can also be effective for managing PPGP. A chiropractor may use ligament release techniques, blocking strategies to relieve pain and pressure, diaphragmatic release, manual therapy and pubic bone adjustments.
Early treatment is recommended, to prevent more intense pain and symptoms in the late stages of pregnancy.
The women’s health specialists at NYDNRehab can help you stay strong and healthy throughout your pregnancy and beyond. We individualize our prenatal and postpartum care plans to meet the specific needs of the mother. Physical therapy and chiropractic care begun in the early stages of pregnancy can help you enjoy an easy and care-free pregnancy and successful delivery. Postpartum care can help you bounce back more quickly after your baby is born.
Get all the benefits of physical therapy and chiropractic care via safe and effective online sessions, all from the privacy and convenience of your home, office or hotel room. Never miss a session, and keep moving toward your physical therapy goals.
At NYDNRehab we combine multiple approaches to improve pelvic stability, by enhancing active muscular control of the pelvic stabilizer muscles. Our approaches include:
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: