Plantar fasciitis is a painful condition that can severely limit your ability to walk, run and enjoy physical activities. As the weight of your body is added to your foot, inflammation can make it impossible to move and function in a normal manner. This problem has created an industry of professionals who attempt to eliminate foot and heel by getting to the source of the problem.
This article provides a brief overview of the condition and the diagnostic process involved in determining an effective treatment plan. Patients should keep in mind that approximately 80 percent of all plantar fasciitis cases will resolve themselves without any external intervention.
Plantar fasciitis is currently considered to be a degenerative condition. In the past, clinicians treated it as an inflammatory condition, but more recent research has revealed the presence of micro-tearing at the junction of the calcaneus bone on the medial side of the foot. This has led clinicians to treat the condition as a non-inflammatory degenerative pathology. The foot must be examined using imaging technology, because plantar fasciitis can be mimicked by a number of conditions that present with similar symptoms.
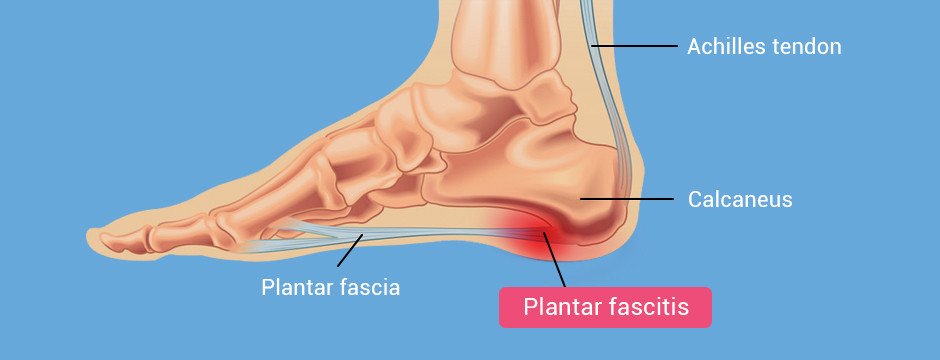
High frequency diagnostic ultrasonography is the gold standard modality for a variety of heel disorders, including plantar fasciitis. Recent innovations in diagnostic ultrasonography provide unparalleled diagnostic certainty due to:
Certain conditions present with similar symptoms to plantar fasciitis, and must be ruled out to avoid wasting time on ineffective treatment. Plantar fasciitis mimickers include:

There are many euphemisms for pain in the foot, and these alternative labels can be helpful when differentiating one type of inflammation from another.
Runner’s heel
Alternative terminology is used to highlight specific characteristics of heel pain that can assist in the treatment plan. These terms can also be helpful for other medical professionals who may be involved in the process. Understanding the specific aspects of the condition can help physical therapists and others to address the most pressing symptoms. For example, collagen tissue in the area may be visibly degenerating, and there may be signs of increased vascular tissues around the medial portion of the calcaneus, near the tubercle.
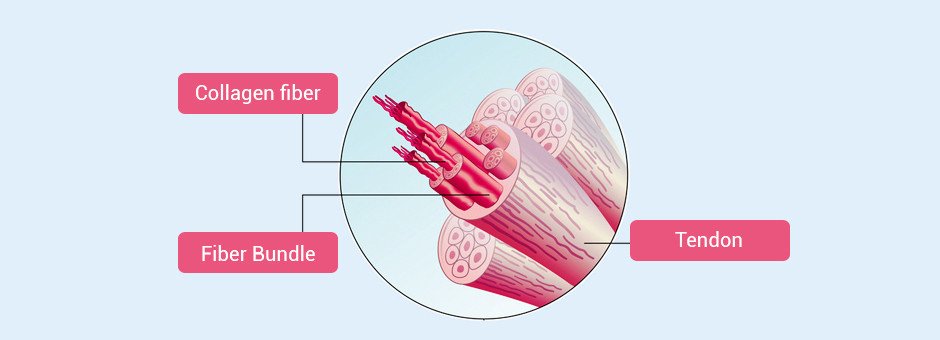
Tendinosis provides a close parallel, which can be helpful for explaining the causes and symptoms to the patient. For example, fibroblasts can be viewed under a microscope, communicating something entirely different to the clinician from the presence of inflammatory cells. This distinction, although important for accurate diagnosis, does not lead to a clear treatment plan by itself.
Professionals often take an approach to treating plantar fasciitis based on the particular strengths of their respective disciplines. Our clinic gives patients access to a variety of treatment options that have successfully reduced pain and improved range of motion in the foot for people with similar symptoms.
Plantar fasciitis affects up to 2 million people every year, and can be an incredibly dangerous condition for elderly patients with cognitive problems in addition to heel pain. Any effective treatment plan will reduce pain and discomfort if it addresses the root cause of the problem. Contributing factors must also be taken into consideration. They may include the patient’s body mass index, or BMI, and excessive pronation of the foot. Our clinic uses the most advanced methods available to treat the actual root of plantar fasciitis pain. We base our treatment protocol on evidence discovered during a thorough examination.
While there are many treatment options available, we have found that a combination of gait-specific physical therapy and extracorporeal shockwave therapy (ESWT) is highly effective, and these treatment approaches have been backed up by numerous good quality research publications. Plantar fasciitis massage techniques are also helpful for relieving pain and discomfort.
The clinical director of NYDNRehab, Dr. Lev Kalika, is a renowned chiropractor with extensive experience treating an array of musculoskeletal pain conditions. Our clinic now offers TeleHealth online services, so you can get the same quality care and treatment from the privacy and convenience of your home, office or hotel room.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: