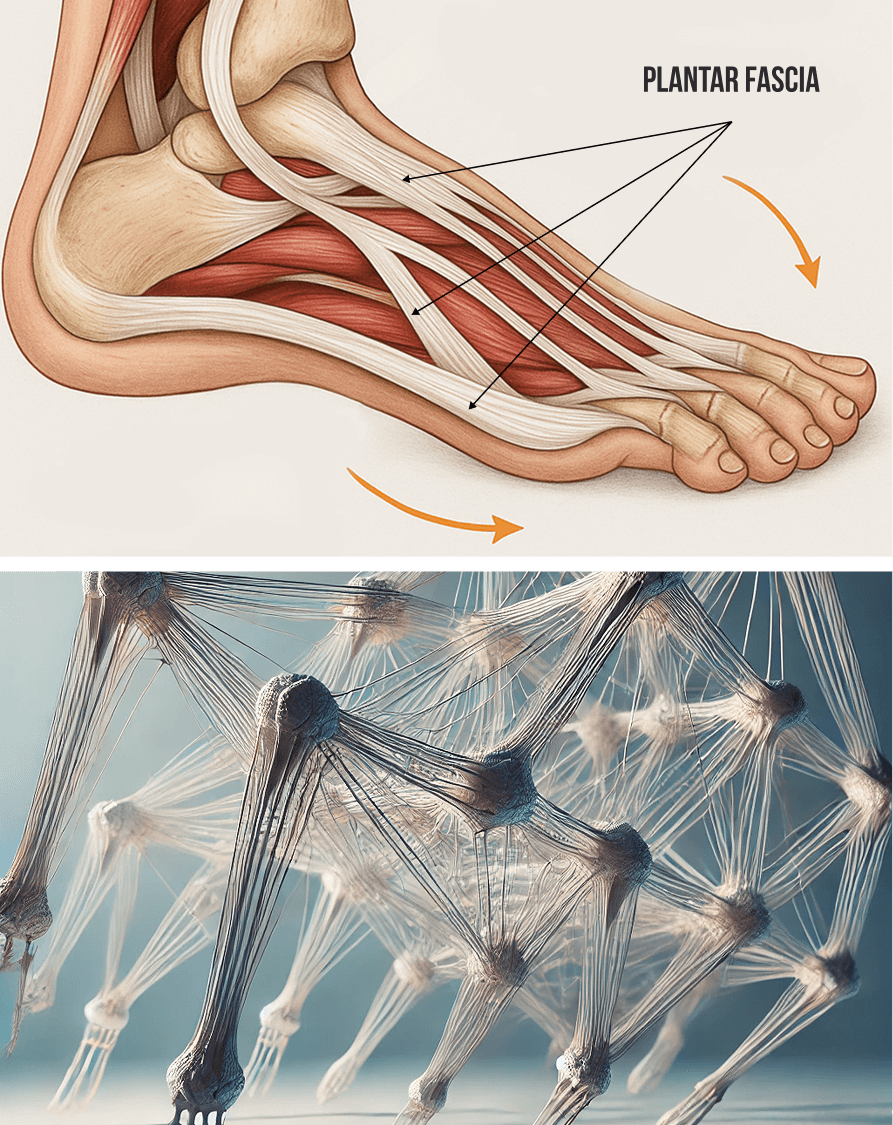
The plantar fascia is a tough band of connective tissue that spans the bottom of the foot from heel to toe, serving to stabilize the many bones that make up your foot and ankle complex. The plantar fascia has elastic properties that store and release energy as it shortens and lengthens, contributing to force production during walking, running and jumping. Although the suffix “itis” is used to describe an inflamed state, it is now evident that plantar fasciitis is not caused by inflammation, but by micro tears and trigger points in the fascia itself.
At NYDNRehab, we are raising the bar for plantar fasciitis treatment by using new regenerative technologies and orthobiologic solutions that accelerate tissue healing and quickly relieve plantar fasciitis pain.
Dr. Lev Kalika, DC, clinical director of NYDNRehab, is an internationally recognized expert in diagnostic and musculoskeletal ultrasonography, with multiple research papers to his credit. Dr. Kalika has studied with some of the world’s most prestigious experts in diagnostic, fascia, and nerve ultrasonography, and has presented his research at multiple international conferences.
Dr. Kalika specializes in the treatment of tendons and fascia, and has pioneered some of the most advanced solutions for dramatically accelerating plantar fasciitis healing. With 20+ years of functional podiatry experience and an impressive track record of success, Dr. Kalika has dedicated his life’s work to advancing holistic therapies that get to the bottom of myofascial pain, without drugs or surgery.
Dr. Kalika is an active member of the American Institute of Ultrasound in Medicine (AIUM), and has developed his own unique approach to Dynamic Functional and Fascial Ultrasonography. He is trained and certified in the Stecco Method of myofascial release.

Orthobiologic, Sports Medicine and Regenerative Medicine Specialist
The plantar fascia is part of a complex network of fascia – tough elastic connective tissue that supports the structure and function of the human body. Fascia works together with muscles, forming the myofascial system that guides and controls movement, and mediates outside forces. Biotensegrity describes the myofascial system’s state of perpetual elastic tension that enables pain-free mobility.
Fascia encases and separates muscles, lines the walls of body cavities, and suspends and supports the internal organs, holding them in place during movement. Healthy fascia is slippery, smooth and elastic, made up of collagenous layers and lubricated by hyaluronan – a fluid composed of hyaluronic acid, able to hold 100X its volume in water. Fascia’s slippery properties enable muscles, tendons, nerves and blood vessels to glide among other structures without friction.
Fascia is densely innervated with mechanoreceptors – sensory nerves that inform your brain of the body’s position in space, and capable of generating pain 5X greater than muscle tissue. When fascia is injured, its layers become dense and sticky, often entrapping nerves and blood vessels, and preventing them from gliding. Proprioception is impaired and biotensegrity is disrupted, causing pain, reducing movement efficiency, and increasing your risk of injury.
Plantar fasciitis is caused by microtears and densified fascial layers that have lost their elastic properties and become sticky. Not only does it cause debilitating heel and foot pain, but a damaged plantar fascia loses its ability to store and release energy – a phenomenon known as the Windlass Mechanism – thus impairing gait and causing mechanical deficiencies throughout the lower kinetic chain.
Most people first see a medical doctor for foot and heel pain, which is frequently misdiagnosed as plantar fasciitis based on the patient’s symptoms. But plantar fasciitis is one of the most commonly misdiagnosed disorders, and multiple other conditions share the same symptoms.
Conditions that mimic plantar fasciitis symptoms include:

At NYDNRehab, we use high-resolution diagnostic ultrasound to visualize the structures and tissues of the foot and ankle in real time, on your very first visit. Dr. Kalka’s expertise in diagnostic ultrasonography is based on years of training and experience, and an in-depth knowledge of human anatomy. Your in-office ultrasound exam lets us accurately differentiate plantar fasciitis from imposters, so we can quickly proceed with treatment.
Ultrasound imaging gives us a clear picture of what is going on beneath the skin, eliminating guesswork based on symptoms alone, to ensure you get the most effective treatment available. We never take a one-size-fits-all approach to patient care. Our personalized, one-on-one treatment plans are custom-designed to accelerate healing, based on your unique patient profile.
The clinic at NYDNRehab features some of the most advanced technologies and methodologies available in rehabilitative medicine, providing fast and effective pain relief for plantar fasciitis. Patients often report a dramatic reduction in pain after their first treatment session, and complete recovery from plantar fasciitis after just a few sessions.
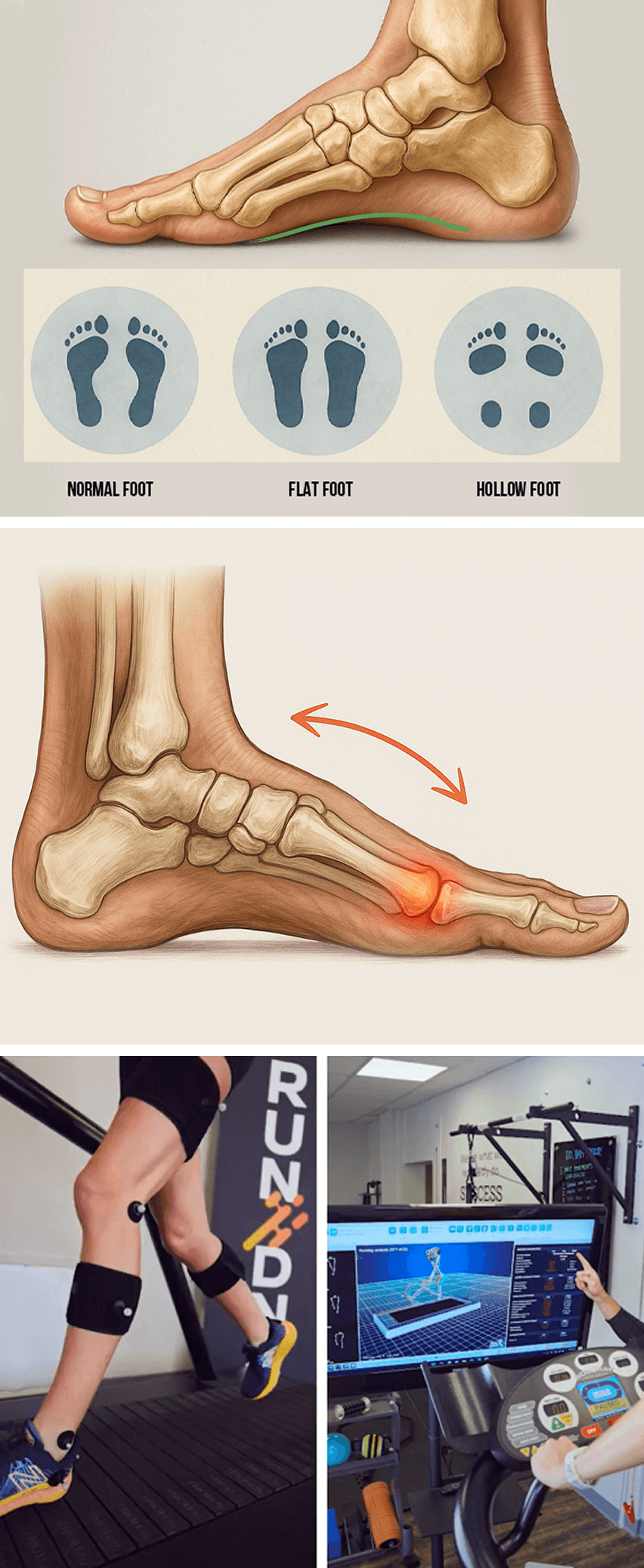
In addition to stress and overuse, plantar fasciitis can arise from biomechanical issues that place excessive stress on the plantar fascia. Conventional treatment zeros in on treating the locus of pain, without addressing other factors that overwork the plantar fascia.
At NYDNRehab, we treat the whole patient, not just your symptoms. Our high-tech motion analysis lab equips us with advanced technologies to quantify movement quality and identify deficiencies that contribute to plantar fascia pain and dysfunction.
Common biomechanical issues that contribute to plantar fasciitis include:
Despite being densely populated with mechanoreceptors, the plantar fascia has minimal vascularity. Its limited blood supply is provided primarily via small capillaries that deliver a minimal amount of nutrients and oxygen. Consequently, damaged fascia can be slow to heal, a factor that prolongs plantar fasciitis pain.
In addition to microtears and fascial layer densification, collagen fibers can become disarrayed, and myofascial trigger points can form, interfering with functional foot mechanics. Addressing these issues is the first step toward eliminating pain and restoring function.
At NYDNRehab, our personalized approach means you get a treatment plan tailored to your unique needs. We treat the whole patient, not just your symptoms – our holistic approach focuses on healing and rehabilitation, not just pain management. Our goal is to restore pain-free foot function using cutting-edge technologies and orthobiologic procedures that accelerate the healing process.
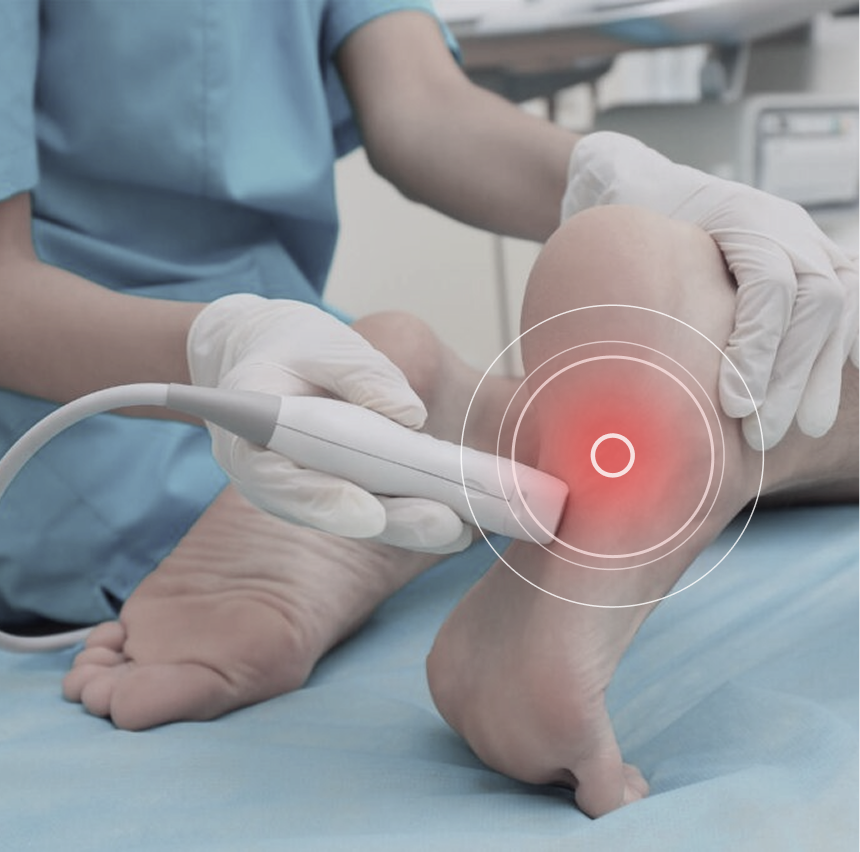
At NYDNRehab, we leverage the most recent evidence-based therapies to quickly eliminate plantar fasciitis pain and restore functional mobility. Our multifaceted approach dramatically accelerates the healing process, and patients often enjoy complete recovery after just a few therapy sessions.
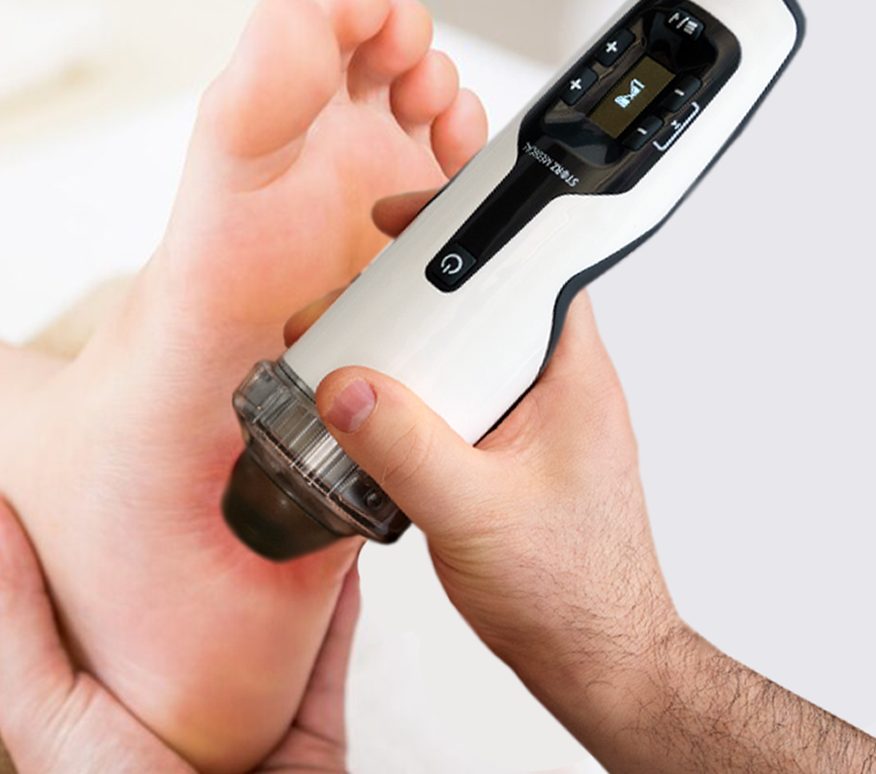
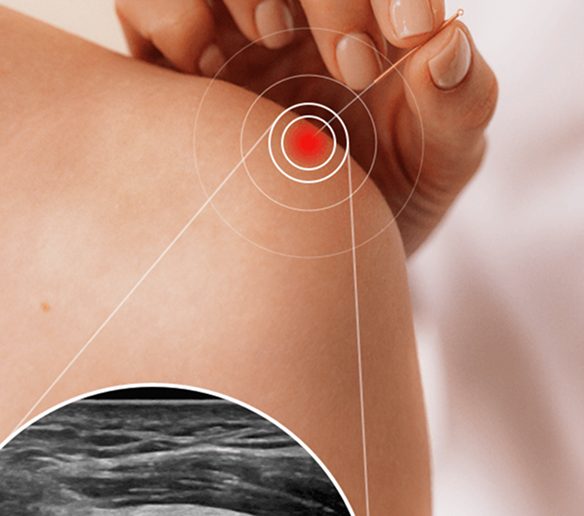
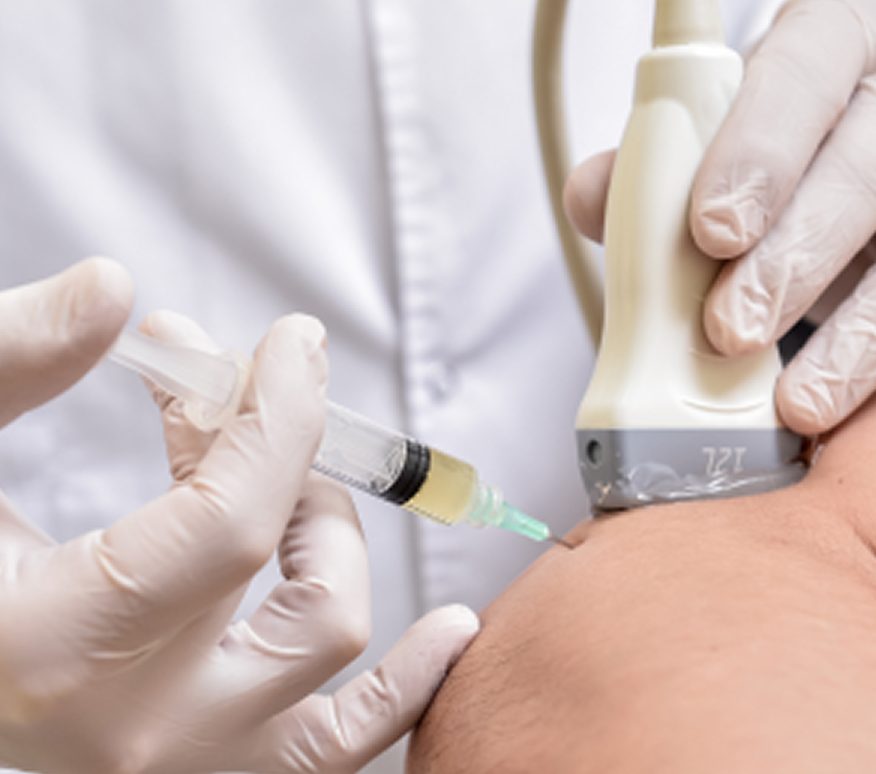

At NYDNRehab, we always begin with a conservative approach to plantar fasciitis treatment, but the secret to our success is precision. We have a 100% track record of success in treating plantar fasciitis, thanks to the combination of extracorporeal shockwave therapy (ESWT) and ultrasound guided dry needling (USDN).
A recent research publication in Nature cites Dr. Kalika’s own research, highlighting USDN as a top-tier evidence-based solution for plantar fasciopathy, and ranking it alongside ESWT and PRP as a primary intervention. To quote the article:
“Current therapeutic approaches for plantar fasciopathy include targeted mechanotherapy, optimized ESWT protocols, ultrasound-guided delivery of orthobiologics (e.g. leukocyte-rich PRP), and precision physical therapies. Furthermore, studies demonstrate the diagnostic and therapeutic value of ultrasound elastography and US-guided interventions for pain modulation. Ultrasound-guided dry needling of myofascial trigger points has been established as a primary intervention option for plantar fasciopathy.”
For patients, our multimodal approach to plantar fasciitis means quick pain relief, fast recovery, and longer-lasting outcomes. In our experience, combining modalities with precision guidance creates the best results.

Plantar fasciitis is a common complaint, especially among people who spend a lot of time on their feet. But you can avoid plantar fasciitis by adopting these preventative strategies:

Independent peer-reviewed research relevant to this treatment approach.