The Achilles tendon is the toughest and largest tendon in the human body, capable of handling loads in excess of 3500 N (~800 pounds). The Achilles extends from the confluence of the gastrocnemius and soleus muscles, and attaches to the calcaneus (heel bone). The tendon has elastic properties that enable it to store and release energy while jumping, and during the gait cycle when walking or running, to propel you forward and upward. Injuries to the Achilles tendon can alter and diminish its elastic properties, reducing overall performance.
Achilles tendon injuries are common in runners, and in athletes who play sports like soccer and basketball that require jumping, landing, cutting and pivoting. They also occur in dancers and gymnasts. Injuries are often the result of repetitive overuse during intense activity, but acute injuries like tendon ruptures can occur from a single incident. Achilles injuries account for as much as 50% of all sports-related injuries.
A growing body of evidence supports the use of extracorporeal shockwave therapy for Achilles tendon treatment. ESWT is a non-invasive regenerative therapy that reduces inflammation, numbs pain and stimulates tissue healing.
or
Dr. Lev Kalika has devoted his life’s work to revolutionizing the way musculoskeletal pain syndromes and disorders are diagnosed and treated. As a world-renowned expert in diagnostic musculoskeletal ultrasonography, Dr. Kalika has published multiple scientific papers on its use in rehabilitative medicine.
Dr. Kalika leverages ultrasound capabilities to target injured tendon tissue using extracorporeal shockwave therapy (ESWT). Ultrasound imaging ensures that the shockwaves hit their mark, for optimal results. Our high resolution ultrasound equipment gives us capabilities for sonoelastography, an important tool for evaluating tendon density during the healing process. Superior microvascular imaging (SMI) enables us to detect early signs of tendon fiber healing at the cellular level.
Dr. Kalika’s 20+ years of experience and expertise in ultrasound imaging, ESWT, and tendon rehabilitation make NYDNRehab the clinic of choice for Achilles tendon rehabilitation in NYC.
While tendons have elastic properties, they are made up mostly of collagen fibers with limited vascularity, making them slow to heal. Conventional treatment for tendon injuries involves classic first aid, such as rest, ice and compression, along with physical therapy and NSAIDs for pain and inflammation. But physical therapy alone may not be sufficient to fully rehabilitate your injured Achilles tendon.
Tendons are an extension of muscles, made up mostly of tough dense collagen fibers, arranged in parallel. Without appropriate treatment after an injury, tendon tears and ruptures can cause collagen fiber disorientation and thinning. Over time, the tendon begins to degenerate, losing its elastic properties and reducing overall performance. ESWT modulates inflammation in the tendon remodeling phase, to initiate tissue repair and encourage optimal fiber remodeling.
Many physical therapy clinics advertise shockwave therapy when what they actually often offer is extracorporeal pulse activation technology (EPAT), which is an acoustic pressure wave and not a true shockwave. ESWT produces high frequency sound waves that stimulate the body’s own reparative mechanisms. ESWT is especially effective for treating chronic degenerative tendon disorders. Ultrasound guidance enhances the accuracy and effectiveness of ESWT.
The clinic at NYDNRehab features some of the most advanced technologies in the world for accurate diagnosis and fast and effective treatment. Our personalized one-on-one approach to patient care ensures that you get a customized treatment plan based on your unique condition and diagnostic results.
Our unique approach to tendon rehab has helped hundreds of athletes and physically active people to safely return to their favorite sports and activities.
Tendon conditions are often misdiagnosed, leading to inferior treatment approaches that waste time and money. Meanwhile, the tendon continues to deteriorate. At NYDNRehab, we know that tendon rehabilitation takes time, and we believe that time should not be wasted.
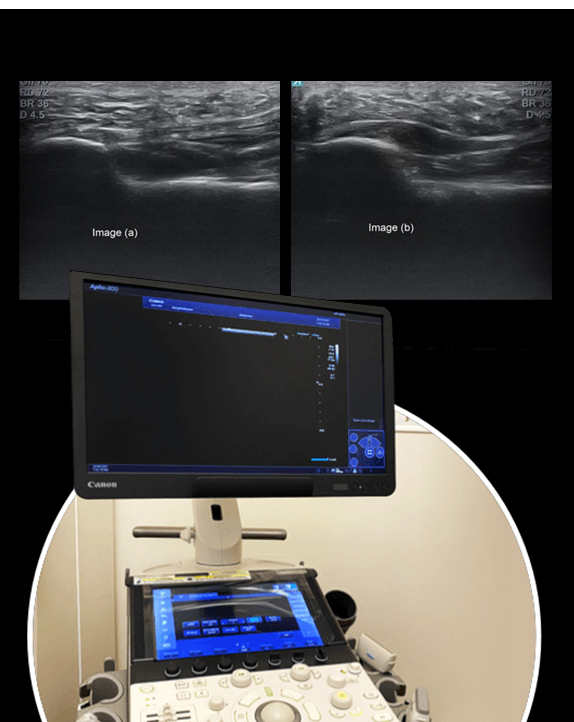
We use the highest resolution diagnostic ultrasonography to visualize dynamic images of your injured tendon in real time. Ultrasound lets us zero in on the injured tissues to identify their nature, severity, and scope. It also equips us with sonoelastography and superb microvascular imaging capabilities, to help distinguish tendonitis from tendinosis, rupture or avulsion.
Ultrasound or MRI alone do not give us a full picture of tendinopathy. Sonoelastography allows us to test tissue stiffness, so that shockwaves can be directed to tissues that appear normal or only moderately damaged on ultrasound or MRI, but have lost their tensile properties. Such tissues are not only pain generators, but they are likely to degenerate over time and become dysfunctional if not properly rehabilitated.
Sometimes Achilles pain comes from surrounding structures, and not from the tendon itself. Pain may arise due to irritation of the Achilles paratenon – a sheath of tissue that covers the Achilles tendon – or from the pre-Achilles (Kager’s) fat pad, a fatty structure located in the ankle joint, in front of the Achilles tendon. Superb microvascular imaging (SMI) gives us a tool to visualize which tissues are actually inflamed, to ensure appropriate treatment.
Dr. Kalika’s expertise as a tendon doctor has helped hundreds of runners and athletes to quickly recover from tendon injuries and return to play.
Low vascularity in tendons means limited access to nutrients necessary for tissue repair. Regenerative therapies leverage innovative new technologies that jump-start the healing process in damaged tendon cells. Your treatment protocol may include a combination of physical therapy and regenerative therapy to restore tendon strength, density and elasticity.

Focused Shockwave Therapy (ESWT)
Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders.
EMTT transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues to target difficult-to-reach tendons..

Electromagnetic Transduction Therapy (EMTT)

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate tendon healing.

HIGH ENERGY INDUCTIVE THERAPY (HEIT)
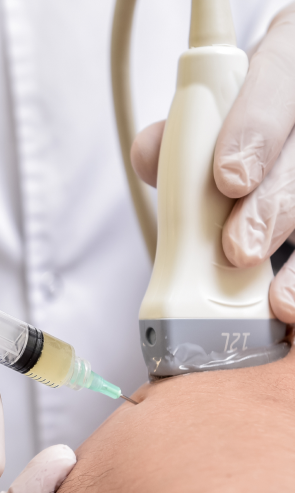
Injection therapies use natural/neutral solutions that stimulate the repair of tendon fibers by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
PRP therapy uses a sample of the patient’s own whole blood, spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tendons, PRP releases biologically active factors to stimulate the synthesis of new connective tissues and blood vessels.
Prolotherapy uses a biologically neutral solution to irritate the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage the growth of new normal tendon fibers.
In addition to regenerative therapies, we use the latest evidence-based approaches for restoring your tendon’s tensile strength and elasticity. Our cutting-edge technologies incorporate artificial intelligence, virtual reality feedback and quantitative data analysis to retrain your motor responses and accurately measure your progress.
Your physical therapy protocol may include some or all of the following:

Tendon injuries are common, yet they are often misdiagnosed and therefore mistreated. At NYDNRehab, our state-of-the-art diagnostic ultrasound equipment ensures accurate diagnosis, to help us design a personalized treatment plan. Microvascular imaging and sonoelastography give us innovative diagnostic tools for measuring your progress, to ensure your treatment is working.
Once we understand the nature of your tendon injury, we use regenerative technologies that are rarely found in run-of-the-mill physical therapy clinics. Our advanced approaches dramatically reduce your chance of needing surgery, while accelerating the healing process.
If you are looking for a muscle and tendon doctor in NYC, contact NYDNRehab today. Our tendon specialists will jump-start your tendon healing so you can get back in the game in the shortest time possible.
Shockwave therapy is most effective during the collagen remodeling phase, which begins about 6 weeks after the initial injury.
ESWT is not painful, but you may experience some discomfort. ESWT is generally more uncomfortable when delivered closer to a bone,
A minimum of three shockwave sessions approximately one week apart is generally recommended. Depending on how well you respond to your initial treatment, you may need more than three sessions.
No, there are plenty of studies showing that shockwave therapy can be effective in treating chronic degenerative tendon conditions and providing long-term pain relief.
Yes, ESWT’s regenerative effects help to restore Achilles tendon architecture at the cellular level, increasing your chances of regaining full function and safely returning to sports.