Joint pain can be debilitating, interfering with your ability to perform everyday tasks, and keeping you from doing your favorite physical activities. Inflammation of the soft tissues surrounding the joint is often the primary driver of joint pain and stiffness. To alleviate pain and restore mobility, injections of local anesthetics, corticosteroids, or a combination of the two are routinely performed. But new research suggests that the short-term relief of pain and inflammation may carry the high price tag of long-term joint damage.
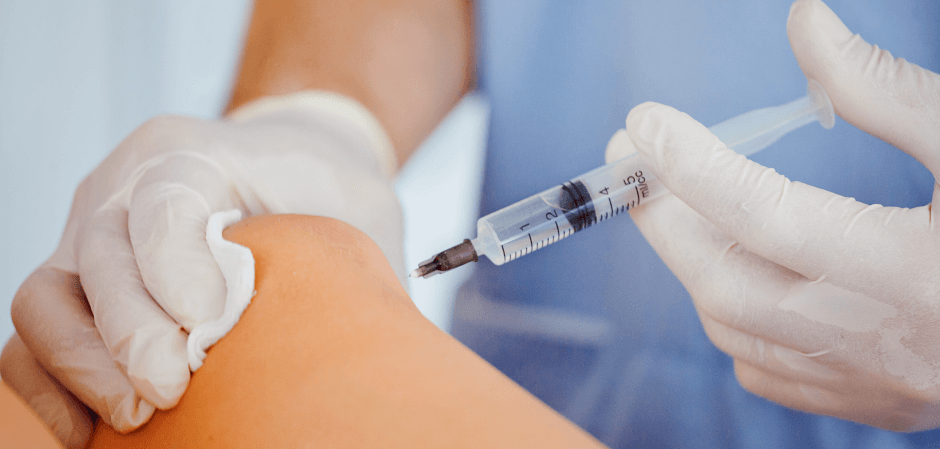
When patients complain about joint pain, the first line of treatment recommended by conventional practitioners is injection of corticosteroids, commonly called steroids. Deemed safe by the FDA, steroid injections, sometimes combined with pain-numbing medicines like lidocaine, are often used to treat pain symptoms in the spine, hip, knee and shoulder.
Conditions commonly treated with steroid injections include:
- Osteoarthritis
- Athletic injuries
- Overuse injuries
- Tendonitis
- Degenerative arthritis
- Low back pain
- Neck pain
Joint injections are also used for diagnostic purposes, to differentiate the locus of pain. For example, a pain-numbing solution may be injected into the hip, to see if regional pain stems from the joint itself, or from other lumbopelvic structures.
But while steroid and analgesic injections provide short-term pain relief, they fail to correct the underlying cause of pain. Moreover, a growing body of evidence suggests that injections of unnatural substances may contribute to significant degeneration of the joint over time.
The most compelling argument given for steroid injections is that they may delay or eliminate the need for surgery. But in truth, many joint surgeries are not only unnecessary, but they often fail to resolve the problem.
Consider these findings:
- Multiple high-quality studies confirm that spinal fusion surgery provides no long-term benefits for patients.
- A study of the benefits of arthroscopic knee surgery found that patients who had actual surgery fared no better after a year than patients given a placebo, or sham surgery.
The argument that steroids delay surgery appears to hold little water in light of research. But even more disturbing is evidence that joint injections do more harm than good to patients’ joints.
- A 2017 study published in the Journal of the American Medical Association, or JAMA, used a study population of 119 male and female patients with osteoarthritic knees. Subjects were assigned to either a treatment group who received steroid injections, or a control group who received saline injections. Injections were administered every 12 weeks for a period of two years. This was a controlled double-blind trial, meaning study participants did not know which group they had been assigned to. At the end of the trial, the research team reported that the cortisone group had a significantly greater loss of knee cartilage thickness, with no significant difference in knee pain. Cartilage cushions and protects the knee joint, and cartilage loss is associated with chronic knee pain and dysfunction.
- A 2018 study used adult dogs to investigate the effects of steroids and pain-numbing injections on shoulder tissues. Subjects were divided into four groups, and each dog was given a single injection. The control group was injected with normal saline, and the three remaining groups were injected with different steroid/analgesic combinations. Researchers took full-thickness samples of the supraspinatus tendon on days 1 and 7, and examined them for cell viability and tissue metabolism. They reported that a single injection of steroid/analgesic solution had significant toxic effects on shoulder tendon tissues, compared to the saline control group.
While steroid and pain-numbing joint injections may provide short-term pain relief, research indicates they have no long-term benefits for patients, and may in fact be harmful. Moreover, eliminating joint pain does not address its underlying cause. Masking pain symptoms with injections may cause additional harm when patients continue to challenge their joints without addressing the source of pain.
Certain injections, including placental injections, hyaluronic acid injections and platelet-rich plasma injections, are free of steroids and contain substances that occur naturally in the human body, such as blood platelets, stem cells, and hyaluronic acid, a naturally occurring component of joint synovial fluid. Prolotherapy injections use harmless natural irritants like sugar or sodium morrhuate, a purified derivative of cod liver oil, to stimulate tissue production and heal ligaments and tendons.
The joint pain specialists at NYDNRehab know that painful joints do not arise out of nowhere. Joint pain is often caused by biomechanical issues in areas of your body located far away from the locus of pain. We use advanced technologies and innovative treatment approaches to get to the bottom of pain and eliminate it at its source.
Our injection therapies are guided by high resolution ultrasonography, to ensure accuracy and eliminate possible harm to nearby nerves and tissues. Don’t just mask your pain. Visit NYDNRehab and resolve joint pain, so you can get back to doing the things you love.
Resources
McAlindon, Timothy E., et al. “Effect of intra-articular triamcinolone vs saline on knee cartilage volume and pain in patients with knee osteoarthritis: a randomized clinical trial.” Jama 317.19 (2017): 1967-1975.
Nuelle, Clayton W., et al. “In Vivo Toxicity of Local Anesthetics and Corticosteroids on Supraspinatus Tenocyte Cell Viability and Metabolism.” The Iowa orthopaedic journal 38 (2018): 107.
Sihvonen, Raine, et al. “Arthroscopic partial meniscectomy versus placebo surgery for a degenerative meniscus tear: a 2-year follow-up of the randomised controlled trial.” Annals of the rheumatic diseases 77.2 (2018): 188-195.