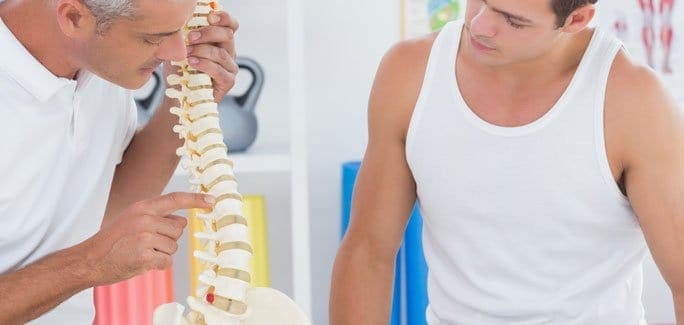
Low back pain is a common complaint of middle aged adults, and a herniated disc is frequently the cause. Spinal discs and spongy fluid-filled sacs located between your vertebra that serve to absorb shock during physical activity. When the outer tissue of a disc becomes torn, fluid can leak out, causing a ruptured or herniated disc.
Repetitive overuse, excessive sitting, poor posture and weak core muscles are often to blame for disc herniation. A ruptured disc can irritate nerves, causing pain and weakness in your low back, buttocks and legs.
When pain and irritation from a herniated disc begin to interfere with your daily life, surgery may seem promising as a quick solution. However, mounting clinical evidence favors non-invasive conservative treatment over surgery for resolving ruptured disc pain.
A recent Meta-Analysis of eleven separate studies by Zhong et al. (2017) found that herniated discs resolve themselves at least 66 percent of the time with conservative care. Even more surprising is that the worst herniated discs are the most likely to recover spontaneously. The research team concluded that conservative therapy promises to become the first line of treatment for herniated discs in the future.
The back pain specialists at NYDNR take a holistic approach to resolving herniated discs. We understand that there are multiple mechanism at play that lead to disc herniation, and we are dedicated to getting to the source of pain and correcting the root cause. Avoid drugs and surgery, and get back to feeling your best with NYDNR.
Source:
Ming Zhong, M. D., and Jin Tao Liu. “Incidence of spontaneous resorption of lumbar disc herniation: a meta-analysis.” Pain physician 20 (2017): E45-E52.