
Among the physical therapy and rehab community, it is well understood that musculoskeletal pain in one area of the body often has its roots in weakness or dysfunction of another area. For example, knee pain can arise from foot or ankle dysfunction, or shoulder pain may occur due to imbalanced muscles in the torso. It is not surprising, then, that Achilles tendon pain may have its origins elsewhere.
In a recent study published in the journal Physical Therapy in Sport (Habets et al., 2017), researchers set out to determine if a relationship exists between deficits in hip strength and Achilles tendinitis in middle-aged male runners.
For this study, researchers designed a controlled trial with a study population of 24 middle aged male runners, 12 of whom displayed symptoms of Achilles tendinitis, and 12 who were asymptomatic.
The study results raise the question of why injuries only occurred in one leg of the symptomatic group, when both hips were weakened.
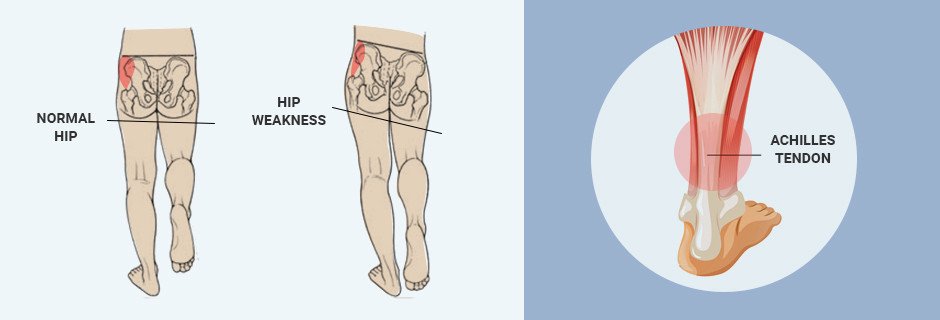
It is often the case that a combination of factors contribute to athletic overuse injuries, and no single factor can be isolated as the underlying cause. In the above-mentioned study, hip weakness appeared to affect Achilles tendon function, but the study only looked at hip strength, and neglected to consider other factors such as knee, foot and ankle strength and function. Moreover, the test results of the study showed isometric strength deficits in the injured group, but found no such deficits in the single leg squat test, a functional test that requires posterior-lateral hip strength.
When attempting to single out a cause of lower extremity overuse injuries, it is important to remember that human movement requires integration of multiple systems in order to complete any task. Dysfunction or strength deficits in any one area can force other areas to take up the slack, and that can lead to overuse and injury.
Consideration of other factors, such as patellar alignment, quadriceps strength, foot posture, and fear-avoidance behaviors should be made as well, to ensure that rehabilitation does not focus on one area to the neglect of other potential causes.
Most PT clinics assess strength by manual muscle testing. This is a key reason why athletes retear their ACLs, re-sprain their ankles and develop multiple consequent injuries that later lead to osteoarthritis.
Muscle strength must be examined under a microscope, and measured in concentric , eccentric and isometric phases. Only then we can establish how much and what type of rehab is necessary, and when the athlete can safely return to sport. This level of accuracy is not possible without modern technology, which many physical therapists are reluctant to use.
STRENGTH IS NOT THE ONLY THING THAT MATTERS
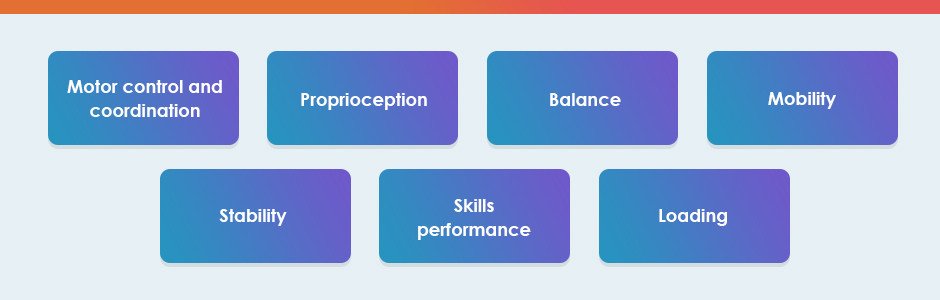
Multiple physical abilities must be restored if we are to help a physically active patient recover:
Runner’s heel
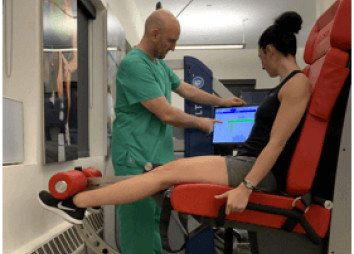


A clinical exam and diagnostic ultrasound imaging can help your therapist pinpoint the exact location and cause of your hip and groin pain. Ultrasound enables both you and your therapist to view the hip and groin region in real time, while in motion. In addition to ultrasound, video gait analysis can help us identify faulty movement mechanics that contribute to hip and groin pain. Once the exact cause is determined, an effective treatment plan can be initiated.
Explore more advanced diagnostic tools available only at NYDNRehab:
Our testing protocol includes:
Combined lumbopelvic hip stability test using DLEST methodology with C.A.R.E.N., our computer assisted rehab environment
Hip joint stability test using DLEST methodology with C.A.R.E.N.
3D star excursion banner test (SEBT) for assessing the involvement of the hip joint and muscles in postural stability
3D gait or running analysis
3D kinematic joint angle analysis during a squat, lunge, drop jump and pelvis on hip rotation
Rehabilitative ultrasonography for viewing intrinsic hip stabilizing muscle activation patterns
Getting at the source of injury and correcting it to restore function is our overriding mission at NYDNRehab. Ignoring overuse injuries and pain can lead to more serious injuries down the road, that can take you out of the game altogether. Physical therapy and chiropractic care can help you eliminate pain and restore full functional movement.
Sometimes, it is impossible to make a trip to the clinic. Whether you’re confined at home or on the go, NYDNRehab TeleHealth services provide a convenient way to receive ongoing professional physical therapy and chiropractic treatment at home, in the office or while traveling. With TeleHealth, you never need to miss a therapy session or lose hard-earned gains in treatment.
If you intend to maintain a physically active lifestyle, the sports medicine pros at NYDNRehab can help. Our unique high-tech gait lab is designed to identify and quantify motor deficits and correct them before injuries occur. Contact us today, and achieve your peak performance potential while reducing your risk of injury. At NYDNRehab, movement is life!
Source
Habets, B, et al. (2017). Hip muscle strength is decreased in middle-aged recreational male athletes with midportion Achilles tendinopathy: a cross-sectional study. Physical Therapy in Sport, 25, 55-61.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: